Request Demo
Last update 11 Nov 2025
Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)
Last update 11 Nov 2025
Overview
Basic Info
Drug Type Therapeutic vaccine, Dendritic cell vaccine |
Synonyms- |
Target- |
Action stimulants |
Mechanism Immunostimulants |
Therapeutic Areas |
Active Indication |
Inactive Indication- |
Originator Organization |
Active Organization |
Inactive Organization- |
License Organization- |
Drug Highest PhasePhase 2 |
First Approval Date- |
Regulation- |
Login to view timeline
Related
7
Clinical Trials associated with Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)NCT06522919
Sequential Immunochemotherapy Treatment with Pembrolizumab Plus Dendritic Cell (DC) Vaccine Followed by Trifluridine/Tipiracil (FTD/TPI) Plus Bevacizumab in Refractory Mismatch-repair-proficient (pMMR) or Microsatellite-stable (MSS) Metastatic Colorectal Cancer (CombiCoR-Vax)
Single-arm, open-label, multicenter phase 2 clinical trial evaluating the clinical and the immunological activity of an innovative strategy with an induction combo immunotherapy (Pembrolizumab plus DC Vaccine) followed by a maintenance chemotherapy (FTD/TPI plus Bevacizumab) in patients with refractory MSS/pMMR metastatic colorectal cancer.
Start Date07 Jan 2025 |
Sponsor / Collaborator- |
NCT04523688
Vaccination With Autologous Dendritic Cells Loaded With Autologous Tumour Homogenate in Glioblastoma: a Phase II Study
Single arm, monocentric trial to assess the safety and the progression-free survival related to the combined treatment of dendritic cell vaccine loaded with autologous tumor homogenate and temozolomide in patients operated for glioblastoma and then treated with standard radiochemotherapy (according to Stupp regimen).
Start Date25 Mar 2021 |
Sponsor / Collaborator |
NCT03546426
Pembrolizumab Plus Autologous Dendritic Cell Vaccine in Patients with PD-L1 Negative Advanced Mesothelioma Who Have Failed Prior Therapies
Pembrolizumab plus autologous dendritic cell vaccine in patients with PD-L1 negative advanced mesothelioma who have failed prior therapies.This is an exploratory, single-arm, open-label, phase 1b clinical trial.
Patients will receive pembrolizumab 200 mg and autologous dendritic cell vaccine every 3 weeks for the first 6 cycles, followed by pembrolizumab 200 mg every 3 weeks until confirmed progression or for a maximum of 2 years (see Figure 1 Study Schema).
After each vaccine administration patients will receive IL-2 3 MU s.c. for 5 days, from day +2 to day +6.
Patients will receive pembrolizumab 200 mg and autologous dendritic cell vaccine every 3 weeks for the first 6 cycles, followed by pembrolizumab 200 mg every 3 weeks until confirmed progression or for a maximum of 2 years (see Figure 1 Study Schema).
After each vaccine administration patients will receive IL-2 3 MU s.c. for 5 days, from day +2 to day +6.
Start Date12 Dec 2019 |
Sponsor / Collaborator |
100 Clinical Results associated with Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)
Login to view more data
100 Translational Medicine associated with Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)
Login to view more data
100 Patents (Medical) associated with Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)
Login to view more data
3
Literatures (Medical) associated with Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)01 Jan 2019·Cancer immunology, immunotherapy : CIIQ2 · MEDICINE
An autologous dendritic cell vaccine polarizes a Th-1 response which is tumoricidal to patient-derived breast cancer cells
Q2 · MEDICINE
Article
Author: Dheda, Keertan ; Davids, Malika ; Cairncross, Lydia ; Anderson, David ; Malherbe, Francois ; Panieri, Eugenio ; Meldau, Richard ; Naiker, Thurandrie ; Oelofse, Suzette ; Downs, Jennifer ; Tomasicchio, Michele ; Novitzky, Nicolas ; Londt, Rolanda ; Pooran, Anil ; Esmail, Aliasgar ; Randall, Philippa ; Semple, Lynn
Breast cancer remains one of the leading causes of cancer-associated death worldwide. Conventional treatment is associated with substantial toxicity and suboptimal efficacy. We, therefore, developed and evaluated the in vitro efficacy of an autologous dendritic cell (DC) vaccine to treat breast cancer. We recruited 12 female patients with stage 1, 2, or 3 breast cancer and matured their DCs with autologous tumour-specific lysate, a toll-like receptor (TLR)-3 and 7/8 agonist, and an interferon-containing cocktail. The efficacy of the vaccine was evaluated by its ability to elicit a cytotoxic T-lymphocyte response to autologous breast cancer cells in vitro. Matured DCs (≥ 60% upregulation of CD80, CD86, CD83, and CCR7) produced high levels of the Th1 effector cytokine, IL12-p70 (1.2 ng/ml; p < 0.0001), compared to DCs pulsed with tumour lysate, or matured with an interferon-containing cocktail alone. We further showed that matured DCs enhance antigen-specific CD8 + T-cell responses to HER-2 (4.5%; p < 0.005) and MUC-1 (19%; p < 0.05) tetramers. The mature DCs could elicit a robust and dose-dependent antigen-specific cytotoxic T-lymphocyte response (65%) which was tumoricidal to autologous breast cancer cells in vitro compared to T-lymphocytes that were primed with autologous lysate loaded-DCs (p < 0.005). Lastly, we showed that the mature DCs post-cryopreservation maintained high viability, maintained their mature phenotype, and remained free of endotoxins or mycoplasma. We have developed a DC vaccine that is cytotoxic to autologous breast cancer cells in vitro. The tools and technology generated here will now be applied to a phase I/IIa clinical trial.
01 Jul 2011·Immunotherapy
Combinatorial Strategies for Alleviation of Tumor-Associated Immune Suppression and Therapeutic Vaccination Against Ovarian Cancer
Author: Stone, Pamela JB ; Cannon, Martin J ; Goyne, Hannah
The prospects for development of therapeutic cancer vaccines have enjoyed a renaissance in recent years, with further encouragement accruing from the US FDA’s approval in 2010 of Provenge® (Dendreon Corporation, Seattle, WA, USA), an autologous dendritic cell (DC) vaccine for prostate cancer. Provenge was the first active cellular therapy to reach the market, breaking through what was widely perceived to be a glass ceiling for cellular therapeutics and cancer vaccines. This renewed optimism has also been fuelled by advances in our knowledge of the mechanisms of immune regulation in the tumor microenvironment. This is particularly true for ovarian cancer, which represents a paradigm for self-defense against immunological attack. Although ovarian cancer recruits multiple mechanisms of immune suppression, thus presenting a formidable barrier to effective tumor vaccination, an understanding of these mechanisms may yield opportunities for adjuvant treatments that counterbalance immune suppression and promote vaccine-induced antitumor immunity.
The various mechanisms of immune suppression employed by ovarian cancer are of more than academic interest to tumor immunologists, since many parameters of immune function have a direct impact on the course of disease. A groundbreaking study from Curiel and colleagues showed that ovarian tumors recruit immuno suppressive Tregs, thus conferring immune privilege, and that Treg infiltration was associated with poor prognosis and increased mortality [1]. These observations demonstrated that immune regulation has a direct and profound relationship with the pathogenesis of disease. Other parameters of immune regulation in ovarian cancer also influence patient outcomes, including expression of B7-H1 (PD-L1) by ovarian tumor cells and infiltrating macrophages or DCs, resulting in T-cell anergy and apoptosis through the engagement of PD-1 expressed by effector T cells [2,3]. Expression of B7-H1 has been associated with differentiation and recruitment of Treg [4], and clinical studies have shown that B7-H1 expression correlates with increased morbidity and mortality in ovarian cancer patients [5]. Expression of B7-H4 (a related member of the family of immunomodulatory accessory receptors) by ovarian tumor-associated macrophages has also been correlated with Treg infiltration and adverse patient outcomes [6]. Two independent studies have further shown that ovarian tumor expression of indoleamine 2,3-dioxygenase (IDO) is associated with poor prognosis [7,8]. IDO first came to prominence for its role in immune suppression and fetal protection at the maternal–fetal interface, and is now widely acknowledged to be an important mediator of T-cell anergy through tryptophan catabolism. IDO is known to be expressed by ovarian tumor cells, and most probably by infiltrating myeloid-derived suppressor cells, including DC and macrophages. Of particular note, IDO expression drives the differentiation and recruitment of Treg by DCs [9], and blocks the conversion of Treg to p roinflammatory Th17 cells [10,11].
In contrast to the evidence that Treg infiltration is associated with poor outcomes in ovarian cancer, a counterpoint is furnished by the recent observation that Th17 cell infiltration correlates with more favorable clinical outcomes [12]. Tumor-infiltrating Th17 cells were positively associated with effector cells and negatively associated with Treg infiltration, leading to the question of whether Th17 cells could be induced or expanded to therapeutic advantage, either by tumor vaccines or adoptive immunotherapy [13]. There is a substantial body of evidence suggesting that Th17 responses can be induced in vitro with proinflammatory cytokines, notably IL-1β. Such an approach may be viable for adoptive T-cell immunotherapy of ovarian cancer, but the adjuvant use of cytokines in support of tumor vaccination is likely to carry a significant risk of off-target toxicities. Of the alternatives, DC vaccination designed to drive ovarian tumor antigen-specific Th17 responses appears to be the strongest option [14]. In comparison with other approaches to tumor vaccination, the plasticity of DC function allows greater scope for fine-tuning T-cell responses, and currently available evidence suggests that modulation of MAPK signaling in DCs may provide the cornerstone for stimulation of Th17 immunity [14].
If we accept the premise that tumor antigen-specific Th17 responses will be of therapeutic benefit for ovarian cancer patients, either through DC vaccination or alternative approaches to tumor vaccination, we still have to confront the myriad mechanisms of immune suppression in the ovarian tumor microenvironment, which remain the greatest barrier to effective antitumor immunity. The history of tumor vaccination has shown that stimulation of tumor antigen-specific T-cell responses is relatively facile, yet translation to clinical efficacy has remained stubbornly elusive. The judicious use of adjuvants designed to alleviate tumor-associated immunosuppression may furnish the key to successful therapeutic vaccination. Several chemotherapeutic agents have shown evidence of activity against Treg, including fludarabine, imatinib mesylate (Gleevec®, Novartis, Basel, Switzerland) and, most notably, cyclophosphamide, which has long been known for its ability to inhibit Treg suppression and potentiate cellular immune responses against tumors [15]. Cyclophosphamide is gaining popularity as an adjuvant in clinical trials of tumor vaccines, and has the advantages of being cheap, well tolerated and easy to administer orally. In a remarkable twist to the story, a recent report has shown that cyclophosphamide may also promote Th17 cell differentiation in cancer patients [16], further adding to its appeal as an adjuvant for clinical trials of ovarian tumor vaccines.
We should also consider the root causes of Treg recruitment in the ovarian tumor microenvironment. Treg infiltration is driven by expression of CCL22 [1], of which the most prominent sources are likely to be tumor-associated macrophages and DCs. Treg differentiation and expansion may be promoted by multiple mechanisms, including local expression B7-H1 and B7-4, both of which correlate with Treg infiltration in ovarian tumors, and expression of IDO, which may also antagonize Th17 differentiation. A notable feature is that all of these mechanisms are independent prognostic indicators of poor outcomes, and all may be mediated by tumor-associated macrophages or DCs. Accordingly, adjuvant treatments that modify the function of tumor-infiltrating myeloid suppressor cells may have a profound impact on Treg recruitment, local immunity and clinical responses to vaccination. There is some evidence from animal studies that gemcitabine, used as a single agent [17] or in combination with a cyclooxygenase inhibitor [18] has activity against myeloid suppressor cells, preferentially depleting this population in tumor-bearing mice. However, absolute depletion of myeloid cells may not be the most favorable course of action, since tumor-associated macrophages and, to a lesser extent, myeloid DCs also have the ability to stimulate Th17 responses [12]. An alternative course of action may reside with the use of agents that modulate myeloid suppressor cell activity, a function that could be fulfilled by adjuvant chemotherapy with aminobisphosphonates. This class of drugs, which includes zoledronate and pamidronate, inhibits metastatic spread to the bone, and can also impair angiogenesis by blocking VEGF signaling and MMP-9 expression by tumor-associated macrophages. Zoledronate can block myeloid-derived suppressor cell expansion and proangiogenic activity [19], and recent evidence points to a proinflammatory shift in myeloid cell function, favoring polarization from a protumor M2 phenotype to an antitumor M1 phenotype with reduced expression of VEGF and IL-10 and increased production of type I cytokines such as IFN-γ [20,21].
Although the available clinical evidence provides a strong rationale for the design of tumor vaccines that promote Th17 immunity in ovarian cancer patients [12,13], this is likely to be a contentious issue, since the various studies that show therapeutic benefit from Th17 immunity are counterbalanced by reports that indicate a role for IL-17 in tumor progression [14]. We believe that Th17-based therapeutic vaccines for ovarian cancer should be tested in clinical trials, but there remains the question of whether vaccination alone would be sufficient to provide clinical benefit in the face of continuing local immune suppression in the tumor microenvironment. The long history of clinical disappointment from tumor vaccination has clearly shown that stimulation of antitumor immunity is not in itself sufficient, and that there is a clear need for adjuvant treatments that create a more favorable environment for vaccine efficacy. Cyclophosphamide has obvious appeal, since it may help to support vaccine-driven Th17 responses in addition to abrogating Treg activity. We also feel that there is a strong case for targeting tumor-associated macrophages/myeloid suppressor cells, since these populations are likely the drivers that fuel Treg infiltration, differentiation and expansion in ovarian tumors.
15 Nov 2010·Clinical cancer research : an official journal of the American Association for Cancer ResearchQ1 · MEDICINE
A Randomized Trial ofEx vivoCD40L Activation of a Dendritic Cell Vaccine in Colorectal Cancer Patients: Tumor-Specific Immune Responses Are Associated with Improved Survival
Q1 · MEDICINE
Article
Author: Fisher, Dawn A. ; Wallace, Paul K. ; Noelle, Randolph J. ; Ernstoff, Marc S. ; Channon, Jacqueline Y. ; Barth, Richard J. ; Gui, Jiang
Abstract:
Purpose: To determine whether an autologous dendritic cell (DC) vaccine could induce antitumor immune responses in patients after resection of colorectal cancer metastases and whether these responses could be enhanced by activating DCs with CD40L.Experimental Design: Twenty-six patients who had undergone resection of colorectal metastases were treated with intranodal injections of an autologous tumor lysate– and control protein [keyhole limpet hemocyanin (KLH)]–pulsed DC vaccine. Patients were randomized to receive DCs that had been either activated or not activated with CD40L. All patients were followed for a minimum of 5.5 years.Results: Immunization induced an autologous tumor-specific T-cell proliferative or IFNγ enzyme-linked immunospot response in 15 of 24 assessable patients (63%) and a tumor-specific DTH response in 61%. Patients with evidence of a vaccine-induced, tumor-specific T-cell proliferative or IFNγ response 1 week after vaccination had a markedly better recurrence-free survival (RFS) at 5 years (63% versus 18%, P = 0.037) than nonresponders. In contrast, no association was observed between induction of KLH-specific immune responses and RFS. CD40L maturation induced CD86 and CD83 expression on DCs but had no effect on immune responses or RFS.Conclusion: Adjuvant treatment of patients after resection of colorectal metastases with an autologous tumor lysate–pulsed, DC vaccine–induced, tumor-specific immune responses in a high proportion of patients. There was an association between induction of tumor-specific immune responses and RFS. Activation of this DC vaccine with CD40L did not lead to increased immune responses. Clin Cancer Res; 16(22); 5548–56. ©2010 AACR.
100 Deals associated with Dendritic cells vaccine(Istituto Scientifico Romagnolo per lo Studio e la cura dei Tumori)
Login to view more data
R&D Status
10 top R&D records. to view more data
Login
| Indication | Highest Phase | Country/Location | Organization | Date |
|---|---|---|---|---|
| Advanced Head and Neck Squamous Cell Carcinoma | Phase 2 | Italy | - | 12 Dec 2019 |
| Soft Tissue Sarcoma | Phase 2 | Italy | - | 12 Dec 2019 |
| Colorectal Cancer | Phase 2 | Italy | - | 02 Dec 2016 |
| Melanoma, Cutaneous Malignant | Phase 2 | Italy | - | 08 Oct 2013 |
| Metastatic melanoma | Phase 2 | Italy | - | 08 Oct 2013 |
| Advanced cancer | Phase 1 | Italy | 12 Dec 2019 | |
| Mesothelioma, Malignant | Phase 1 | Italy | 12 Dec 2019 |
Login to view more data
Clinical Result
Clinical Result
Indication
Phase
Evaluation
View All Results
| Study | Phase | Population | Analyzed Enrollment | Group | Results | Evaluation | Publication Date |
|---|
No Data | |||||||
Login to view more data
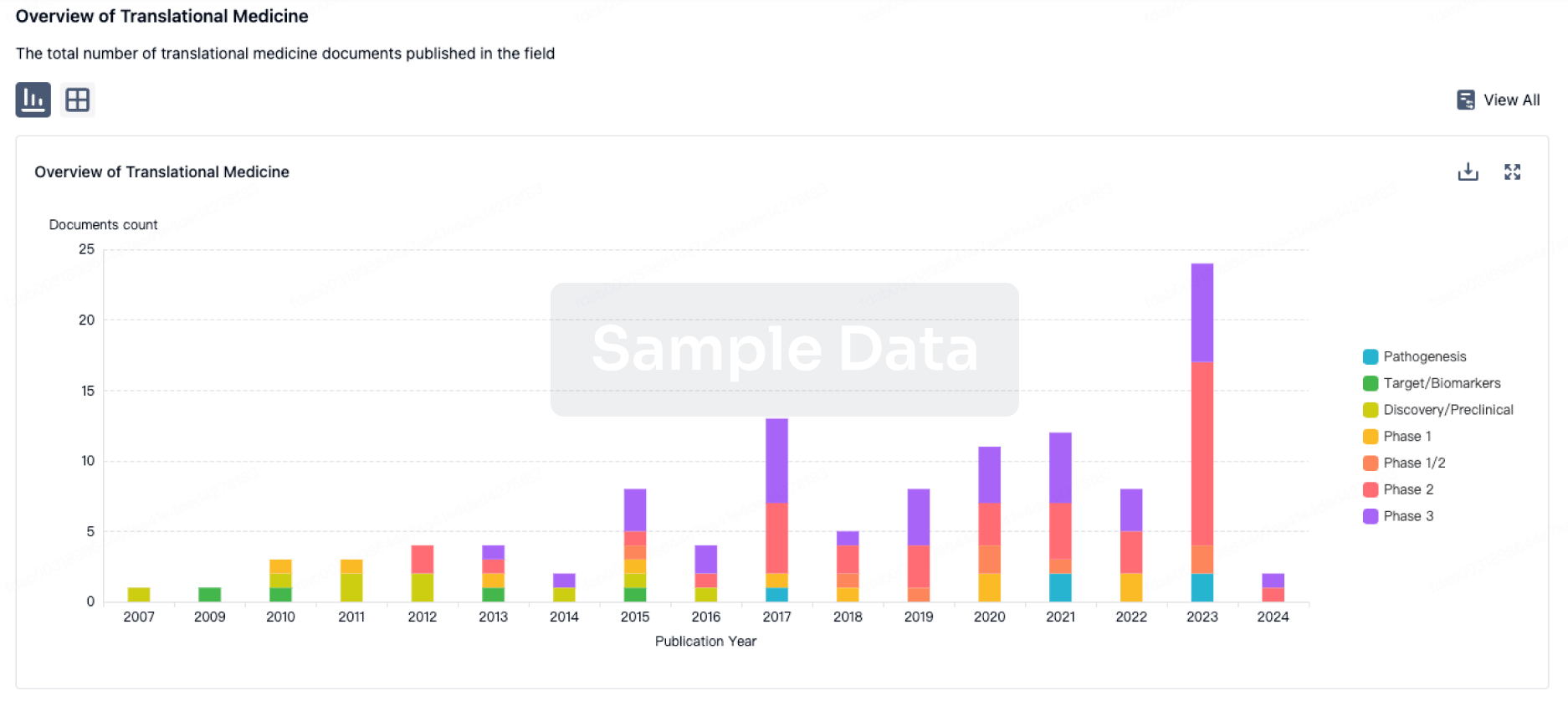
Translational Medicine
Boost your research with our translational medicine data.
login
or
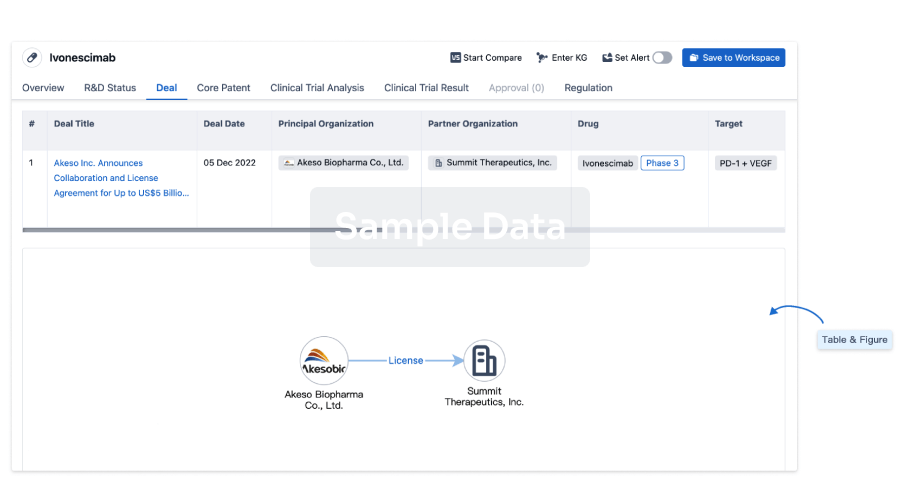
Deal
Boost your decision using our deal data.
login
or
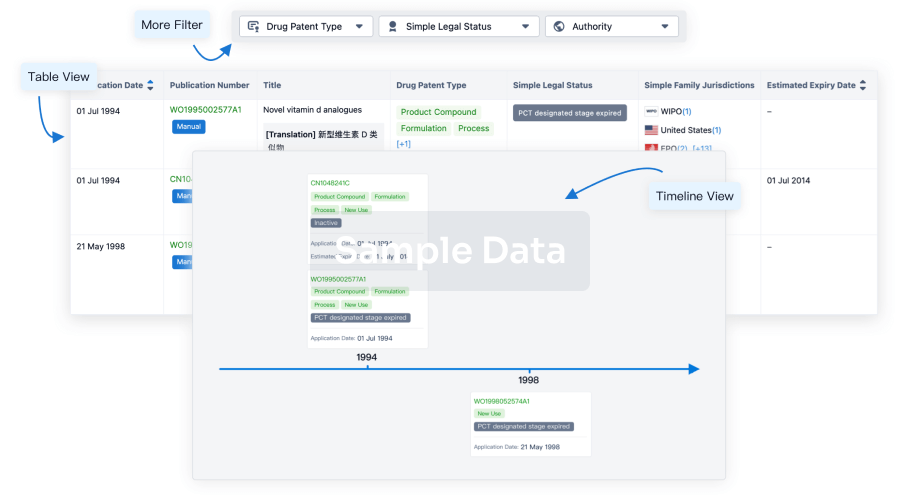
Core Patent
Boost your research with our Core Patent data.
login
or
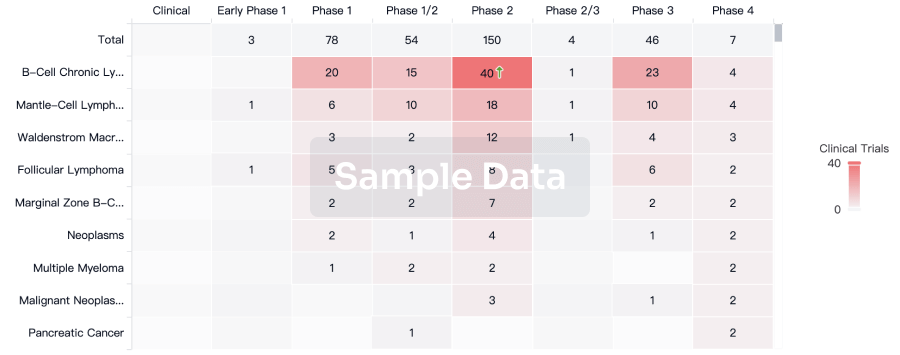
Clinical Trial
Identify the latest clinical trials across global registries.
login
or
Approval
Accelerate your research with the latest regulatory approval information.
login
or
Regulation
Understand key drug designations in just a few clicks with Synapse.
login
or
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free