Request Demo
Last update 03 Mar 2026

Nelson Laboratories LLC
Last update 03 Mar 2026
Overview
Related
100 Clinical Results associated with Nelson Laboratories LLC
Login to view more data
0 Patents (Medical) associated with Nelson Laboratories LLC
Login to view more data
11
Literatures (Medical) associated with Nelson Laboratories LLC01 Nov 2022·Computational toxicology (Amsterdam, Netherlands)
Principles and procedures for assessment of acute toxicity incorporating in silico methods
Article
Author: Paulino, Alexandre ; Amberg, Alexander ; Patlewicz, Grace ; Vardakou, Ioanna ; Ahlberg, Ernst ; McAtee, Britt ; Martin, Matthew ; Burleigh-Flayers, Heather ; Milchak, Lawrence ; Brigo, Alessandro ; Kemper, Ray ; Gromek, Kamila ; Mumtaz, Moiz ; Glowienke, Susanne ; Suarez, Diana ; Bassan, Arianna ; Jolly, Robert ; Woolley, David ; Madia, Federica ; Cronin, Mark T D ; Graham, Jessica ; Moudgal, Chandrika ; Zwickl, Craig M ; Ruiz, Patricia ; Jones, David ; Masuda-Herrera, Melisa ; Piparo, Elena Lo ; Karmaus, Agnes ; Barton-Maclaren, Tara ; Bellion, Phillip ; Devlin, Amy ; Neilson, Louise ; Valentin, Jean-Pierre ; Muster, Wolfgang ; Mestre, Jordi ; Anger, Lennart T ; Fish, Trevor ; Glover, Kyle ; Myatt, Glenn ; Roncaglioni, Alessandra ; Szabo, David T ; Custer, Laura ; Beilke, Lisa
Acute toxicity in silico models are being used to support an increasing number of application areas including (1) product research and development, (2) product approval and registration as well as (3) the transport, storage and handling of chemicals. The adoption of such models is being hindered, in part, because of a lack of guidance describing how to perform and document an in silico analysis. To address this issue, a framework for an acute toxicity hazard assessment is proposed. This framework combines results from different sources including in silico methods and in vitro or in vivo experiments. In silico methods that can assist the prediction of in vivo outcomes (i.e., LD50) are analyzed concluding that predictions obtained using in silico approaches are now well-suited for reliably supporting assessment of LD50-based acute toxicity for the purpose of GHS classification. A general overview is provided of the endpoints from in vitro studies commonly evaluated for predicting acute toxicity (e.g., cytotoxicity/cytolethality as well as assays targeting specific mechanisms). The increased understanding of pathways and key triggering mechanisms underlying toxicity and the increased availability of in vitro data allow for a shift away from assessments solely based on endpoints such as LD50, to mechanism-based endpoints that can be accurately assessed in vitro or by using in silico prediction models. This paper also highlights the importance of an expert review of all available information using weight-of-evidence considerations and illustrates, using a series of diverse practical use cases, how in silico approaches support the assessment of acute toxicity.
01 Jul 2022·Infection control and hospital epidemiologyQ4 · MEDICINE
Addressing personal protective equipment (PPE) decontamination: Methylene blue and light inactivates severe acute respiratory coronavirus virus 2 (SARS-CoV-2) on N95 respirators and medical masks with maintenance of integrity and fit
Q4 · MEDICINE
Article
Author: Patel, Alpa N ; Faris, Peter ; Mayo, Mark ; Wielick, Constance ; Lin, Yi-Chan ; Cui, Yi ; Nauwynck, Hans ; Chu, Larry F ; Timm, Emily ; Scholte, Florine E M ; De Jaeger, Simon ; Chu, May C ; Kabra, Kareem B ; Laperre, Jan ; Parker, Rod ; Evans, David ; Mores, Christopher N ; Liao, Lei ; Homdayjanakul, Kamonthip ; Lin, Ying Ling ; Clark, Tanner ; Davies, Jan M ; Kilinc-Balci, F Selcen ; Thiry, Etienne ; Haubruge, Eric ; Conly, John M ; Sahni, Jaya ; Molloy-Simard, Vanessa ; Mackie, Cyrus J ; Wagner, Thor ; Jolois, Olivier ; Dams, Lorène ; Gallagher, Thomas ; Chen, James ; Lemyre, Jean-Luc ; Ludwig-Begall, Louisa F ; Lendvay, Thomas Sean ; Zhao, Mervin ; Tritsch, Sarah R ; Lamb, Molly M ; Malott, Rebecca ; Willaert, Jean-Francois ; Price, Amy ; Hope, Karen ; Heyne, Belinda ; Simmons, Sarah M ; Macia, Nicolas ; Reader, Susan ; Chu, Steven ; Smit, Sarah J ; Harcourt, Brian H ; Page, Ken
Abstract:
Objective::
The coronavirus disease 2019 (COVID-19) pandemic has resulted in shortages of personal protective equipment (PPE), underscoring the urgent need for simple, efficient, and inexpensive methods to decontaminate masks and respirators exposed to severe acute respiratory coronavirus virus 2 (SARS-CoV-2). We hypothesized that methylene blue (MB) photochemical treatment, which has various clinical applications, could decontaminate PPE contaminated with coronavirus.
Design::
The 2 arms of the study included (1) PPE inoculation with coronaviruses followed by MB with light (MBL) decontamination treatment and (2) PPE treatment with MBL for 5 cycles of decontamination to determine maintenance of PPE performance.
Methods::
MBL treatment was used to inactivate coronaviruses on 3 N95 filtering facepiece respirator (FFR) and 2 medical mask models. We inoculated FFR and medical mask materials with 3 coronaviruses, including SARS-CoV-2, and we treated them with 10 µM MB and exposed them to 50,000 lux of white light or 12,500 lux of red light for 30 minutes. In parallel, integrity was assessed after 5 cycles of decontamination using multiple US and international test methods, and the process was compared with the FDA-authorized vaporized hydrogen peroxide plus ozone (VHP+O3) decontamination method.
Results::
Overall, MBL robustly and consistently inactivated all 3 coronaviruses with 99.8% to >99.9% virus inactivation across all FFRs and medical masks tested. FFR and medical mask integrity was maintained after 5 cycles of MBL treatment, whereas 1 FFR model failed after 5 cycles of VHP+O3.
Conclusions::
MBL treatment decontaminated respirators and masks by inactivating 3 tested coronaviruses without compromising integrity through 5 cycles of decontamination. MBL decontamination is effective, is low cost, and does not require specialized equipment, making it applicable in low- to high-resource settings.
04 Oct 2021·The Journal of cell biologyQ1 · BIOLOGY
Anisotropic expansion of hepatocyte lumina enforced by apical bulkheads
Q1 · BIOLOGY
Article
Author: Kalaidzidis, Yannis L. ; Gralinska, Elzbieta ; Franke, Christian ; Valenzuela, José Ignacio ; Delpierre, Julien ; Prikazchikova, Tatiana ; Zatsepin, Timofei ; Seifert, Sarah ; Shcherbinina, Evgeniya ; Koteliansky, Victor ; Repnik, Urska ; Morales-Navarrete, Hernán Andrés ; Vingron, Martin ; Belicova, Lenka ; Räägel, Helin ; Zerial, Marino
Lumen morphogenesis results from the interplay between molecular pathways and mechanical forces. In several organs, epithelial cells share their apical surfaces to form a tubular lumen. In the liver, however, hepatocytes share the apical surface only between adjacent cells and form narrow lumina that grow anisotropically, generating a 3D network of bile canaliculi (BC). Here, by studying lumenogenesis in differentiating mouse hepatoblasts in vitro, we discovered that adjacent hepatocytes assemble a pattern of specific extensions of the apical membrane traversing the lumen and ensuring its anisotropic expansion. These previously unrecognized structures form a pattern, reminiscent of the bulkheads of boats, also present in the developing and adult liver. Silencing of Rab35 resulted in loss of apical bulkheads and lumen anisotropy, leading to cyst formation. Strikingly, we could reengineer hepatocyte polarity in embryonic liver tissue, converting BC into epithelial tubes. Our results suggest that apical bulkheads are cell-intrinsic anisotropic mechanical elements that determine the elongation of BC during liver tissue morphogenesis.
29
News (Medical) associated with Nelson Laboratories LLC25 Feb 2026
Nelson Labs’
Thor Rollins
, RM RDC, has been selected as Convenor of WG1 within TC 194, the working group responsible for the ISO 10993-1 standard.
Rollins spoke with
MD+DI
about this role and to peel back the layers of ISO 10993-1.
Can you give an overview of ISO 10993-1?
Rollins:
ISO 10993, the whole suite of standards, focuses on the biocompatibility or biological risk of medical devices in patients. It’s been around for decades in various forms. The concept behind the series is to evaluate medical devices as they come into contact with patients and assess the inherent risks of those devices based on their materials, processes, and usage. The goal is to mitigate risks through specific tests or evaluations to ensure the device is safe.
Part one of ISO 10993 serves as the umbrella standard for the entire series. It outlines the overall concepts of risk assessment for biological evaluation. While the other sections focus on specific endpoints or types of testing, part one acts as the foundation, connecting all the other standards into a cohesive framework for assessment. I often call it the "bible of biocompatibility" because it provides the guidance needed to unify the standards and conduct initial evaluations. When regulatory bodies want to ensure a device is safe, they refer to the ISO 10993 series, with part one being the key document for understanding how to start the evaluation process.
The latest news is that you’ve been named convener for the standard. Can you talk about that role and what it entails?
Rollins:
Absolutely. Each standard has an organizational structure to manage its development. The convener is essentially the lead responsible for organizing the standard and overseeing the work being done. Each member body, representing different countries, assigns experts to the ISO group. For the US, our member body is AAMI, and we currently have about six ISO experts, including me.
As the new convener, my role is to direct the work of the group. This involves setting the direction for the standard, breaking the work into manageable sessions, publishing drafts, collecting comments, resolving those comments, and ultimately releasing a finalized document that can be used. Previously, Jim Anderson, another US member, served as the convener for part one for decades. He retired, and I was asked to take his place. Starting in January of this year, I’ve been leading the group and shaping the future of part one.
Let’s discuss the US and its ambivalence toward adopting the standard. Why was that the case?
Rollins:
I was part of the working group at the time, though I wasn’t the convener then. There was a significant effort led by the Australian delegation to radically progress the standard. The original standard was developed during a time when countries wanted to standardize tests they were already using, creating a uniform global approach. Over the years, part one became synonymous with a table format—Annex A, Table 1—which listed tests based on device use. Unfortunately, this led to a "checkbox" mentality, where people simply ticked off tests without considering the broader risk-based approach we intended.
For the past 15 years, we’ve been working to evolve the standard away from checkboxing and toward a more risk-based approach. The Australian delegation decided to push this forward aggressively, revolutionizing the standard to focus solely on risk-based evaluation and minimize checkboxing.
As a US group, we weren’t against the concept. In fact, we supported the idea. However, we voted no because the new standard introduced many new elements without providing sufficient guidance on how to implement them. The document required certain actions but didn’t offer enough instructions to help users understand how to carry them out. That’s why the US voted no — not because the standard was inherently bad, but because we felt it wasn’t mature enough for day-to-day use. We wanted more time to refine it.
Ultimately, the standard was approved despite the US voting no on every draft. However, we were just one vote in the process.
So the standard got approved, and now, as convener, my job is to address areas that we believe are not yet mature or fully developed. Currently, there are six specific areas where we need to provide more guidance. My focus is on working with six different projects to release documents that offer clearer instructions for these areas. The goal is to make the standard more practical and user-friendly because, to be honest, some aspects of the document are difficult for people to use in its current form.
Why is this standard so important for medical device companies?
Rollins:
Biocompatibility is a critical consideration for any device that comes into contact with the body, whether directly or indirectly. Unlike other endpoints that may only apply to certain devices—such as sterility, packaging in sterile barriers, or reprocessing—biocompatibility applies to almost all devices because nearly every medical device interacts with the body in some way.
ISO 10993 is the standard universally used to evaluate biocompatibility for regulatory submissions. Even Class I devices, which may not require 510(k) submissions to FDA, still need to assess the safety of their materials and processes. While you may not submit this data to FDA, it’s essential to evaluate biocompatibility according to ISO 10993 to address biological risks and ensure patient safety.
This standard is vital because it provides the framework that regulators use to determine whether a device is safe for market approval. It ensures that medical devices meet safety requirements, protecting patients and guiding manufacturers in their regulatory processes.
04 Nov 2025
FDA and members of the U.S. medical device industry are not on board with the International Organization for Standardization’s (ISO’s)
ISO 10993-1: 2026
, which replaces ISO 10933-1:2018 and is expected to be published in January. The global document governs how medical device manufacturers seek biological evaluation of their devices within a risk management process.
We asked the U.S. Cochair for that standard,
Thor S. Rollins, B.S., RM (NRCM), a biocompatibility expert with Nelson Labs
, to explain why the U.S. remains the global holdout and what medical device manufacturers need to do now to prepare.
What is ISO 10993-1:2026, and why haven’t U.S. manufacturers embraced the standard?
Rollins:
ISO 10993-1 is the biocompatibility standard for the world. While 10993 is the standard series that represents biocompatibility for the medical device industry, Part 1 is the introduction that outlines the general principles of a risk assessment for biocompatibility.
It has been that way for decades. We’ve been working for about the last two years on updating it, and it’s a radical change. There are lot of moving parts. A lot of different things have been added to it. It’s a complete overhaul.
With that, there are a lot of controversial items. Among the main impacts:
Additions to risk estimation, including how do you estimate and mitigate any risks, and have some kind of program in place to be able to do that? There’s potential to have more genotoxicity evaluations for cardiovascular devices, and concern about devices leaving behind materials in the blood flow that could cause genotoxicity concerns. There’s that risk estimation I talked about.
There are concerns about something called foreseeable misuse. How do we look at risks that might not only occur with how the device is intended to be used, but also if it is misused? How might biological risks be associated with that?
And regarding end-of-life testing, how does biocompatibility change over the lifecycle of the medical device? This means having to look at biocompatibility not just at the start of a medical device’s life, but also at the end of its life, which could be the end of a shelf life (when it’s expired) or when hospitals stop reprocessing a device.
All of these sound like they make sense, and they do. The contexts aren’t controversial. What’s controversial is how do you give guidance on how to do these things?
Rollins:
Let me be frank, the standard dictates that you should do these things, but we really don’t give guidance on how.
So, the U.S. has pretty much said that we should stop or pause this standard and go back and work on it so that we can give guidance on how to meet new requirements.
The rest of the world doesn’t feel that way.
Those of us in the standards committee are writing technical specifications on the topic, but it’s still years away before we get those published.
What does this mean for the industry?
Rollins:
This means that FDA is likely going to partially recognize this new part one and will come up with its own guidance on how to look at these things.
The worry there is that we might have a guidance by FDA that says one thing and eventually a 10993 that says some other thing. And we’ll have two different ways to approach biocompatibility, depending on whether you’re going to the U.S. or the rest of the world.
Who is on the U.S. committee, and how does voting work?
Rollins:
FDA is part of the vote. The committee also includes U.S. manufacturers’ representatives to the Association for the Advancement of Medical Instrumentation (
AAMI
).
There are multiple votes throughout this process. The first votes are in the ISO committee, in which there are about six of us from the U.S., including from FDA, who represent the U.S. With each vote, the U.S. has voted no.
The last vote includes all U.S. AAMI representatives. Again, the U.S. representatives voted no.
What do medical device manufacturers need to know now about the use of this standard if they’re developing devices for use in the U.S. and abroad?
Rollins:
Like I said, there are a lot of changes.
This standard should be put out any day now. We’re waiting for it to be published. Then, any new device that gets submitted globally will have to follow all these new standards.
Manufacturers should probably find out what’s in the new standard. There are lots of people—not just us—who have done white papers and
webinars
on what the new 10993 is going to have in it.
I would try to get hold of the draft, if you can find it.
The truth is, once it gets published, that will be considered state of the art by Europe, so regulatory bodies are going to start enforcing the standard. All those changes that I talked about are going to be required of new medical devices.
I think FDA is still trying to figure out what they’re going to do with this new one.
Isn’t that a problem?
Rollins:
It is. We have a new standard that’s coming out that’s fundamentally changing how people need to look at biocompatibility, and I don’t know if industry is ready.
I think that if you are making a device in 2026 or are going to be submitting a device in 2026, you should do your due diligence today to really find out how your device might change with the new standard. Look into how to meet the standards.
These tests can be three months long. If you’re starting testing today, you should probably do it according to the requirements of the new standards (not the old one) because by the time you get results, the new standard will be out.
That’s a big story.
Rollins:
It’s huge. I don’t think people realize what kind of impact it will have. That’s why a lot of the American medical device manufacturers voted no, including Nelson Labs. We just don’t feel like it has been given enough time based on the potential impact to devices.
04 Sep 2025
There are a host of questions surrounding updates to ISO 10993-1, an international standard that sets the general principles for the biological evaluation of medical devices. Last month, representatives from Nelson Laboratories sponsored
a 3-day webinar
to discuss what these updates might mean for the medical device industry going forward.
Audrey Turley, director of Lab Operations, Biosafety for Nelson Labs, tackled several questions on
day one
.
Here are some of the most pressing questions that came up during day one of the webinar.
What were the underlying reasons for changes regarding foreseeable misuse?
Turley:
The end goal is to ensure patient safety by covering how devices are actually used. Device manufacturers are often aware that their devices get used differently than intended. The change ensures evaluation of these scenarios upfront rather than after market release.
This addition is logical because we should consider potential misuse during the design and manufacturing process. If we already know doctors might use a device differently than intended, we should assess those scenarios to protect that patient population.
For bioaccumulation, is the contact duration increased in general or just for the specific chemical?
Turley:
If you can separate the chemical from the device, you can assess it just for the chemical. However, if the chemical is an intrinsic part of the device that will bioaccumulate and have exposure to the patient, then it impacts your entire patient contact duration.
Will there still be limited or brief patient-contacting devices/components if there is a stated reasonably foreseeable misuse where a device is being used longer than indicated?
Turley:
There are times when it's not reasonable to say a device would be left in a patient longer than intended, especially for brief contact devices. The key is having the conversation up front rather than waiting for regulatory agencies to raise concerns.
You can still classify something as brief contact if you can justify it based on:
The typical clinical use
What could go wrong
The chances of it being left in longer
Whether the device can function with components left in
The actual risk to the patient
For absorbable devices that take longer than 30 days to be completely excreted based on ADME data, should they be classified as long-term devices?
Turley:
This is a case where contact duration may change. If a device is absorbed but takes more than 30 days to be fully excreted, the patient remains exposed during that time. This might require assessing long-term exposure, such as sub-chronic exposure, for those compounds.
This doesn't necessarily mean reclassifying the device as permanent, but it does mean addressing how those categories apply to your device and how you'll address the biological effects.
How do you know if a compound will bioaccumulate?
Turley:
This determination is based on publicly available information. First, identify the compounds through chemistry testing appropriate for the exposure duration. Toxicologists can then identify if compounds bioaccumulate.
For new materials, this requires significant work upfront to ensure product safety. The challenge becomes greater when chemistry data isn't available, especially for limited-contact devices. Manufacturers need to:
Conduct in-depth research on all contacting materials
Consider bioaccumulation potential for all devices, regardless of contact duration
Evaluate processing materials that might be eliminated if problematic
Will FDA recognize and adopt the new version of the ISO rule?
Turley:
The US voted against this standard for several reasons. While we can't predict with certainty, we would expect FDA to provide guidance on which parts of the standard they recognize. Manufacturers can check the FDA website for this information.
100 Deals associated with Nelson Laboratories LLC
Login to view more data
100 Translational Medicine associated with Nelson Laboratories LLC
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 04 Mar 2026
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or

Translational Medicine
Boost your research with our translational medicine data.
login
or

Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or

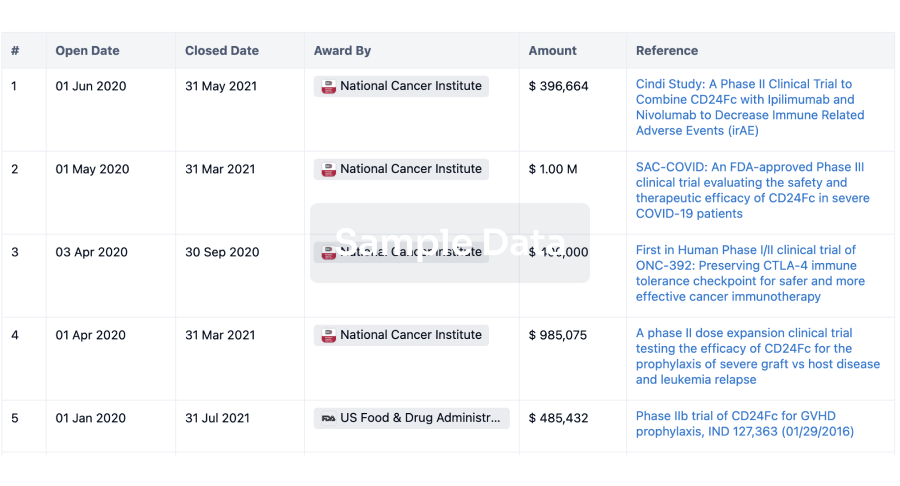
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or

Financing
Unearth financing trends to validate and advance investment opportunities.
login
or

AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free