Last update 02 Oct 2024

Avatar Group
Last update 02 Oct 2024
Overview
Related
100 Clinical Results associated with Avatar Group
Login to view more data
0 Patents (Medical) associated with Avatar Group
Login to view more data
10
Literatures (Medical) associated with Avatar Group01 Mar 2021·Supportive care in cancer : official journal of the Multinational Association of Supportive Care in CancerQ2 · MEDICINE
Inherent and modifiable risk factors for peripheral venous catheter failure during cancer treatment: a prospective cohort study
Q2 · MEDICINE
Article
Author: Marsh, Nicole ; O'Brien, Catherine ; Friese, Christopher ; Rickard, Claire M ; Larsen, Emily N ; Monteagle, Emily
PURPOSE:
To identify modifiable and non-modifiable risk factors for peripheral intravenous catheter (PIV) failure among patients requiring intravenous treatment for oncology and haematology conditions.
METHODS:
A single-centre prospective cohort study was conducted between October 2017 and February 2019. Adult in-patients requiring a PIV for therapy were prospectively recruited from two cancer units at a tertiary hospital in Queensland, Australia. The primary outcome was a composite of complications leading to PIV failure (local and bloodstream infection; occlusion; infiltration/extravasation; leakage; dislodgement; and/or phlebitis). Secondary outcomes were (i) PIV dwell time; (ii) insertion and (iii) failure of a CVAD; (iv) adverse events; (v) length of hospital stay. Outcomes were investigated using Bayesian multivariable linear regression modelling and survival analysis.
RESULTS:
Of 200 participants, 396 PIVs were included. PIV failure incidence was 34.9%; the most common failure type was occlusion/infiltration (n = 74, 18.7%), then dislodgement (n = 33, 8.3%), and phlebitis (n = 30, 7.6%). While several patient and treatment risk factors were significant in univariable modelling, in the final multivariable model, only the use of non-sterile tape (external to the primary dressing) was significantly associated with decreased PIV dislodgement (hazard ratio 0.06, 95% confidence interval 0.01, 0.48; p = 0.008).
CONCLUSION:
PIV failure rates among patients receiving cancer treatment are high, the sequelae of which may include delayed treatment and infection. Larger studies on risk factors and interventions to prevent PIV failure in this population are needed; however, the use of secondary securements (such as non-sterile tape) to provide further securement to the primary PIV dressing is particularly important.
TRIAL REGISTRATION:
Study methods were registered prospectively with the Australian New Zealand Clinical Trials Registry on the 27th March 2017 (ACTRN12617000438358); https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?id=372191&isReview=true.
01 Jun 2020·PediatricsQ2 · MEDICINE
Developing Pediatric Appropriateness Criteria for Intravenous Catheters
Q2 · MEDICINE
Review
Author: Chopra, Vineet ; Ullman, Amanda
* Abbreviations:
IV — : intravenous
MAGIC — : Michigan Appropriateness Guide for Intravenous Catheters
miniMAGIC — : mini Michigan Appropriateness Guide for Intravenous Catheters
Consider this scenario: an 8-month-old infant with osteomyelitis needs intravenous (IV) access for 3 weeks of antibiotics; what device will best ensure successful therapy and low risk of complications? Or consider this: a teenager with cystic fibrosis is hospitalized for the third time this year with an acute exacerbation. Despite multiple efforts by experienced clinicians, an IV catheter cannot be successfully placed in a peripheral vein. Frustrated, the nurse says, “Let’s just put in a peripherally inserted central catheter.” Is this the best choice for the patient?
These scenarios, and many more like them, occur for hundreds of pediatric patients in hospitals every day. Yet, the approach to these decisions is far from consistent.1 Ask a provider why they choose a specific device or consult a certain specialist for an IV access procedure, and you may hear, “That’s how I have always done it,” or “This is how I was trained.” In part, these monocentric styles have evolved as a result of evidence gaps in pediatric vascular access. Compared with adult populations, the evidence base for risk, benefits, and alternatives of IV …
Address correspondence to Amanda Ullman, PhD, RN, Menzies Health Institute Queensland, Griffith University, Kessels Rd, Nathan, QLD4111, Australia. E-mail: a.ullman@griffith.edu.au
01 Jan 2020·Journal of paediatrics and child healthQ4 · MEDICINE
Flushing of peripheral intravenous catheters: A pilot, factorial, randomised controlled trial of high versus low frequency and volume in paediatrics
Q4 · MEDICINE
Article
Author: Mihala, Gabor ; Schults, Jessica ; Kleidon, Tricia M ; Rickard, Claire M ; Flynn, Julie ; Keogh, Samantha
Aim:
To test the feasibility of an efficacy trial comparing different flushing frequencies and volumes to reduce peripheral intravenous cannula (PIVC) failure in paediatric inpatients.
Methods:
Pilot, 2 × 2 factorial, randomised controlled trial comparing PIVC flushing techniques in intervention pairs: (i) low volume (3 mL) versus high volume (10 mL); and (ii) low frequency (24 hourly) versus high frequency (6 hourly). Patients were excluded if: fluids were restricted, weight < 5 kg, PIVC already in situ for >24 h or continuous infusion. The primary end‐point was feasibility (eligibility, recruitment, retention, protocol adherence, missing data and sample size estimates) of a large trial. Secondary end‐points were PIVC failure (composite and individual), bloodstream infection and mortality.
Results:
A total of 919 children were screened from April to November 2015, with 55 enrolled. Screening feasibility criteria were not met, mainly due to continuous infusions and PIVCs in situ >24 h or planned for imminent removal. However, 80% of eligible participants consented, 2% withdrew, protocol adherence was 100%, and there was no missing primary end‐point data. PIVC failure was significantly higher (hazard ratio = 2.90, 95% confidence interval: 1.11–7.54) in the 3 mL compared to the 10 mL group. There was no difference in failure between frequency groups (hazard ratio = 0.91, 95% confidence interval: 0.36–2.33). There was no interaction effect (P = 0.22).
Conclusion:
Trial feasibility proved challenging due to eligibility criteria, which could be improved with additional recruiting staff. Firm conclusions cannot be made based on this small sample, but flush volume may impact PIVC failure.
2
News (Medical) associated with Avatar Group01 Apr 2024
Longstanding partnership deepens with new financing, beta access to clinical manufacturing instruments, and AACR data presentations
SAN FRANCISCO--(BUSINESS WIRE)-- Xcell Biosciences Inc. (Xcellbio), an instrumentation company focused on cell and gene therapy applications, today announced it has added new elements to its research collaboration agreement with LabCorp, a global leader of innovative and comprehensive laboratory services. Through the expanded collaboration, Labcorp will participate in the beta program for Xcellbio’s clinical manufacturing line of AVATAR™ instruments and has been given an observer seat on the company’s board of directors. In exchange, Labcorp has increased its strategic investment in Xcellbio. Financial details of the investment were not disclosed. The companies will be jointly presenting results from their existing cell and gene therapy collaboration at the upcoming annual meeting of the American Association for Cancer Research (AACR).
Xcellbio has developed the AVATAR incubator system for cell therapy research and development. Its latest platform, the AVATAR Foundry system, is a cGMP cell therapy manufacturing platform that delivers novel capabilities for improving the potency of cell therapies. These capabilities are especially important for cell therapies targeting solid tumors, which are frequently met with challenges in overcoming the harsh immunosuppressive tumor microenvironment (TME) to achieve durable potency at the target tumor site. The AVATAR and AVATAR Foundry systems offer small-scale research and process development as well as scale-up manufacturing platforms for metabolically reprogramming therapeutic cells to improve their potency and persistence in the TME.
“We have worked closely with the Xcellbio team for years and have been continually impressed by their dedication to improving the development and manufacture of cell and gene therapies,” said Maryland Franklin, Ph.D., vice president and enterprise head of cell and gene therapy at Labcorp, who has now joined Xcellbio’s board of directors as an observer. “Incorporating AVATAR technology into Labcorp’s robust cell and gene therapy development program will allow us to deliver decision-enabling results to our clients around the world and, ultimately, will help us drive precision healthcare for a broad range of patients.”
Through the expanded collaboration, Labcorp’s preclinical oncology site in Ann Arbor, Mich., will become a beta site for the AVATAR Foundry system. More information about the beta access program is available at .
“We are proud to be a trusted partner for Labcorp, who recognizes that key partnerships will help unlock what’s possible in the development of cell and gene therapies,” said Brian Feth, co-founder and CEO at Xcellbio. “We look forward to deepening our ties as we continue on our shared mission of developing safer, more effective treatments for more patients and a wide array of diseases.”
Poster Presentations at AACR
Along with scientific collaborators at Labcorp, Xcell team members will be presenting two posters at the upcoming AACR annual meeting, taking place April 5-10 in San Diego.
Poster #3908: Generation of new oncology cell models through long-term acclimation under hypoxic and hyperbaric culture conditions
Presenter: Yewei Xing, Labcorp
Summary: In this poster, scientists will show that long-term acclimation of conventional tumor cell lines to conditions reflective of the TME alters their phenotype and gene expression pro
Poster #6334: Metabolic reprogramming enhances expansion and potency of CAR-T cells
Presenter: Candy Garcia and James Lim, Xcellbio
Summary: This presentation will illustrate how manufacturing CD19 CAR T cells in optimized environmental conditions can enhance their expansion potential and potency, as measured with an in vitro tumor killing assay.
About Xcell Biosciences
Xcellbio is driven by its mission to enhance the performance and safety of cell and gene-based therapies through the design and development of revolutionary technology platforms. The company’s commercial instruments and AI-driven software allow researchers to discover novel insights into immune and tumor biology and enable the translation of these insights at patient scale through the development of its pioneering cGMP cell therapy manufacturing platform. Based in San Francisco, Xcellbio can also be found online at .
About Labcorp
Labcorp (NYSE: LH) is a global leader of innovative and comprehensive laboratory services that helps doctors, hospitals, pharmaceutical companies, researchers and patients make clear and confident decisions. We provide insights and advance science to improve health and improve lives through our unparalleled diagnostics and drug development laboratory capabilities. The company's more than 67,000 employees serve clients in over 100 countries, worked on over 84% of the new drugs approved by the FDA in 2023 and performed more than 600 million tests for patients around the world. Learn more about us at .
Cell TherapyAACRGene Therapy
29 Aug 2023
VANCOUVER, Wash., Aug. 28, 2023 /PRNewswire/ -- Prominently featured in The Inner Circle, Lauren Roles is acknowledged as a Top Pinnacle Healthcare Professional for her contributions to the field of Internal Medicine.
Continue Reading
Lauren Roles
Dr. Roles pursued higher education at the University of Puget Sound in Tacoma, Washington where she earned a Bachelor of Science degree in Molecular and Cellular Biology. She received a medical degree from the University of Colorado School of Medicine in Denver; completed a residency in internal medicine at Eisenhower Medical Center in Rancho Mirage California; and finished a fellowship in geriatric medicine at Oregon Health & Science University in Portland.
Dual board-certified as an internist and in geriatric medicine by the American Board of Internal Medicine (ABIM), the doctor explained that the ABIM is a physician-led non-profit independent evaluation organization driven by doctors who want to achieve higher standards for better care in a rapidly changing world. The doctor explained that internal medicine is the medical specialty dealing with the prevention, diagnosis, and treatment of adult diseases. Physicians specializing in internal medicine are called internists and manage and prevent common and complex diseases by providing comprehensive care and promoting overall well-being.
Focused on enabling people to identify and reach their health goals, Dr. Roles works at Vancouver Clinic in Vancouver Washington, and is trained to help older adults with complicated health problems. She asserts that she enjoys making tailored plans for each individual considering their unique conditions, concerns, and hopes to reach their health goals so that they can do everything they want to do.
The doctor believes that the key to practicing medicine well is to listen to the needs of patients. She is dedicated to providing the latest advancements in her practice and is associated with the American College of Physicians; The American Geriatric Society; and the Oregon Geriatric Society.
In her spare time, Dr. Roles enjoys reading a good science fiction or fantasy novel and spending time with her golden doodle, Samwise, named after The Lord of the Rings character, and her cat, Na'Vi, who is named for the blue people from Avatar. The doctor said that she is fascinated by evolutionary biology, is building her own tiny collection of dinosaur fossils; and hopes to one day participate in a real dig.
The doctor would like to thank her parents, Royal and Diane Roles, for all of their support and dedicate this honor to her mentor and high school biology teacher, Mr. Deopke.
For more information, please visit her website at .
Contact: Katherine Green, 516-825-5634, editorial@continentalwhoswho.com
SOURCE The Inner Circle

Executive Change
100 Deals associated with Avatar Group
Login to view more data
100 Translational Medicine associated with Avatar Group
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 06 Oct 2024
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or
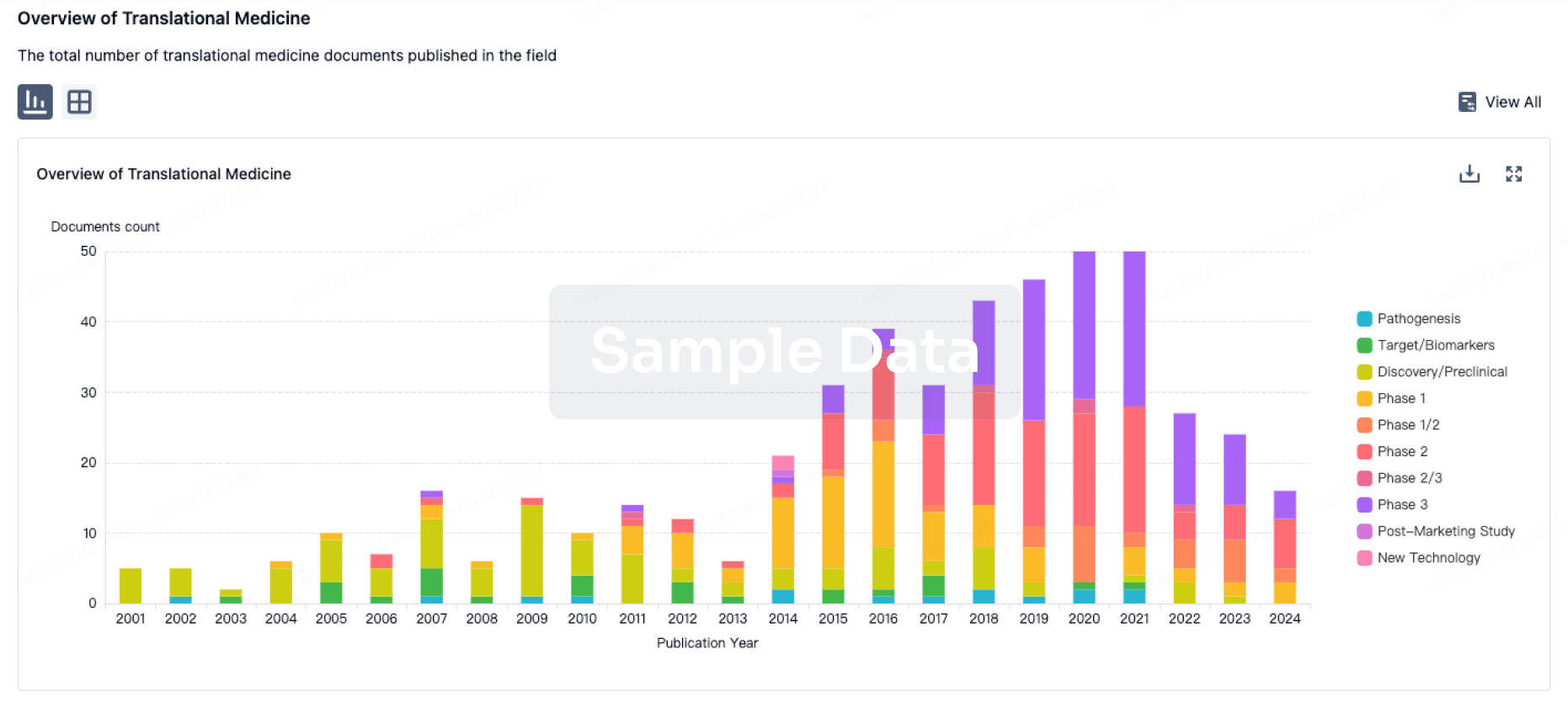
Translational Medicine
Boost your research with our translational medicine data.
login
or
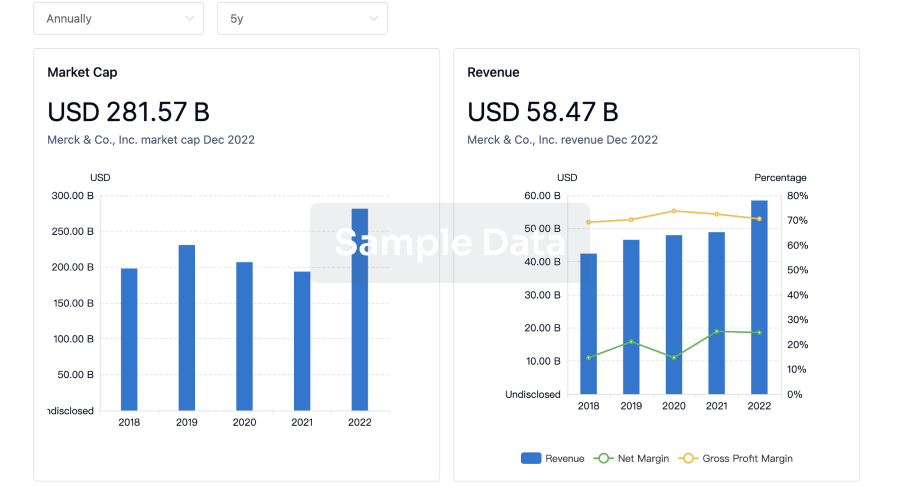
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
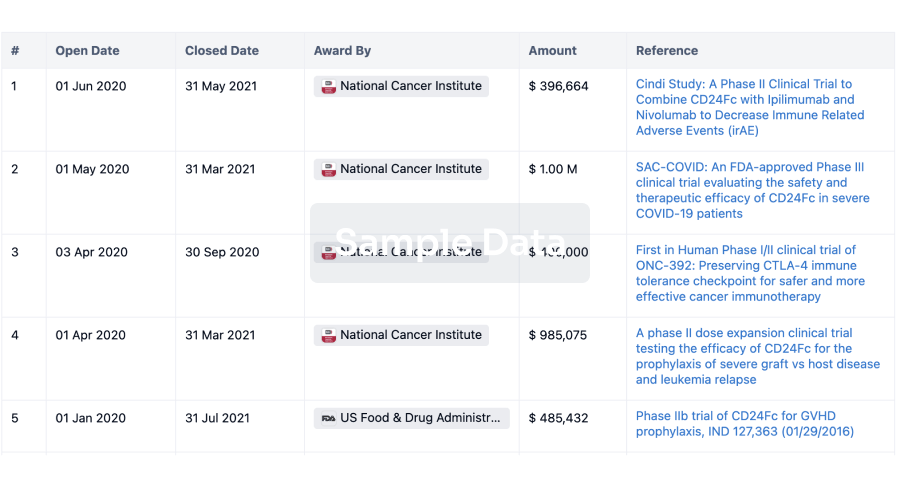
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
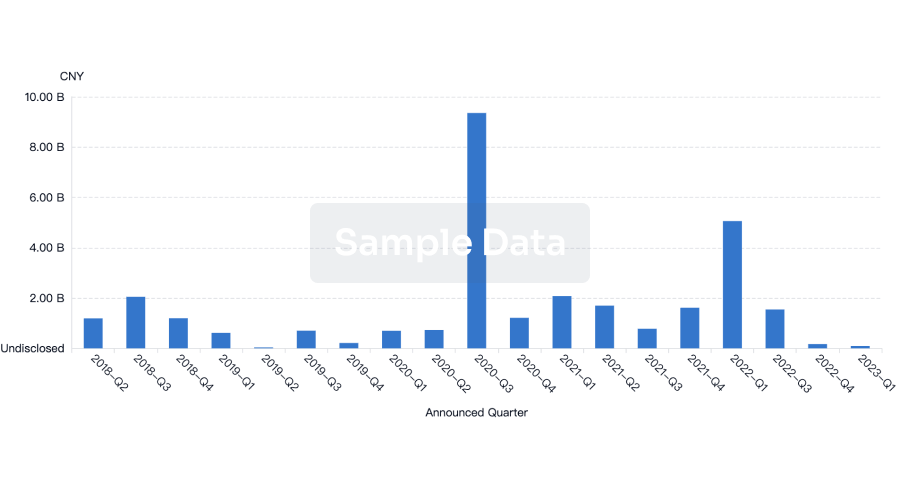
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
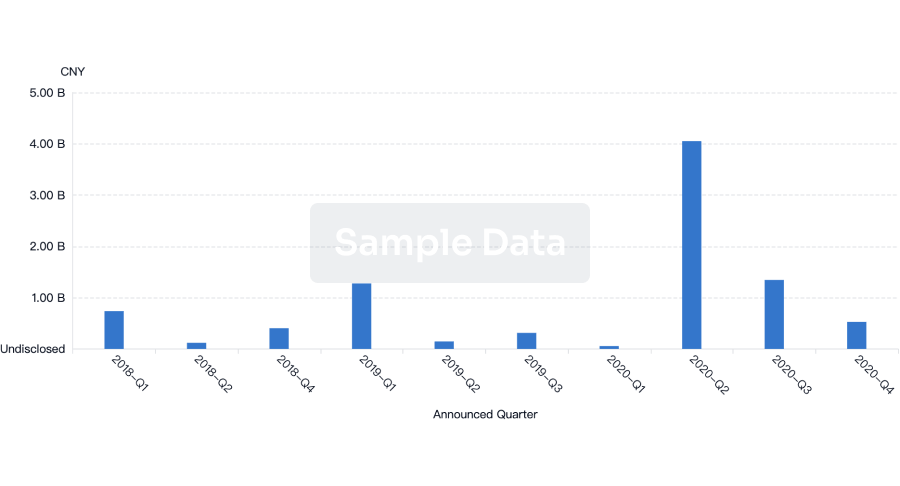
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free