Last update 19 Sep 2024
Tufts Health Public Plans, Inc.
Last update 19 Sep 2024
Overview
Related
100 Clinical Results associated with Tufts Health Public Plans, Inc.
Login to view more data
0 Patents (Medical) associated with Tufts Health Public Plans, Inc.
Login to view more data
10
News (Medical) associated with Tufts Health Public Plans, Inc.25 Jul 2024
None
Below is a roundup of payer-centric news headlines you may have missed during the month of July 2024.
Legislation
ACA insurance brokers
Led by Senate Finance Committee Chair Ron Wyden, D-Oregon, five senators have introduced a bill that would institute criminal penalties against insurance brokers that change Affordable Care Act plans.
In certain cases, these brokers switch plans without the individuals’ consent, as Wyden has commented on before.
“Predatory health insurance brokers are stealing money out of families’ pockets by leaving them with uncovered medical expenses, unexpected tax liabilities and more by fraudulently changing or enrolling Americans in health insurance plans in the federal marketplace,” said Wyden. “My bill will crack down on fraudulent tactics that cheat hard working Americans out of getting the health care they need.”
The bill, called the Insurance Fraud Accountability Act, is supported by Sherrod Brown, D-Ohio; Tammy Duckworth, D-Illinois; Patty Murray, D-Washington; Brian Schatz, D-Hawaii; and Chris Van Hollen, D-Maryland. It is endorsed by AHIP, the Blue Cross Blue Shield Association and Centene.
Warren leads Chevron Doctrine codification charge
Another group of Democratic lawmakers wants to codify the federal agency protections that were once available under Chevron deference.
A recent Supreme Court ruling overrules Chevron, meaning courts agencies will have less power to fill in legislative gaps for ambiguous law. Liberal lawmakers and judges have worried this will ruling will have serious consequences for healthcare and environmental protections.
Led by Elizabeth Warren, D-Massachusetts, the Stop Corporate Capture Act intends to codify Chevron protections while ensuring lobbyists don’t have outsized influence on rulemaking procedures that go against the interest of the public.
The bill would create an Office of the Public Advocate to help individuals participate in regulatory proceedings, better inform the public of rulemaking, require agencies to respond to petitions with more than 100,000 signatures and make it easier for the public to hold agencies accountable for long delays in completing rules, Warren’s office said in a news release.
Lobbyists would be required to disclose industry-funded research and conflicts of interest and establishes financial penalties for corporate lobbyists that submit false information during rulemaking.
“Many Americans are taught in civics classes that Congress passes a law and that’s it, but the reality is that any major legislation enacted must also be implemented and enforced by the dedicated, nonpartisan experts at our public agencies to become a reality,” said Rep. Pramila Jayapal, D-Washington, in a statement. “Too often, this process is driven by corporate lobbyists and special interests who know exactly how to make these processes benefit their bottom lines at the cost of public interest.”
Illinois signs law banning step therapy
Gov. J.B. Pritzker, D-Illinois, signed a law (PDF) this month banning step therapy, prior authorization for mental health crises and junk insurance, the AP reported.
Junk insurance is when plans offer only limited coverage, but, now, plans will need to meet the Affordable Care Act requirements. It will take effect Jan. 1.
Mental health parity has been a priority in the Biden administration, often drawing criticism from insurers.
Louisiana to soon require menopause treatment coverage
Starting Aug. 1, Louisiana will require insurers and Medicaid to cover menopause and perimenopause treatment, reports the Louisiana Illuminator.
Under House Bill 392, the legislation will make it easier for residents to obtain hormone replacement therapy.
Transactions
Molina Healthcare buys ConnectiCare in $350M deal
EmblemHealth will sell ConnectiCare, Connecticut’s health plan serving 140,000 members, for $350 million to Molina Healthcare.
The purchase signifies 25% of expected 2024 premium revenue, Molina said in a news release. The purchase will be made with cash on hand.
“The addition of ConnectiCare to Molina brings a well-rounded government sponsored healthcare plan, and a new state, to our portfolio,” said Joe Zubretsky, president and CEO of Molina, in a statement. “Today’s announcement demonstrates the continuing success of our strategy of acquiring stable revenue streams, deploying capital efficiently and delivering value through the application of the standard Molina playbook.”
“We believe Molina's commitment to delivering on the promise of the Affordable Care Act, bringing coverage to so many Americans through the federal and state exchanges, makes it the ideal partner to take on ConnectiCare's mission,” said Karen Ignagni, EmblemHealth CEO, in a news release.
Molina Healthcare recorded earnings per share of $5.17 and premium revenue of $9.4 billion during its second-quarter earnings. Its consolidated medical cost ratio was 88.6%.
Centene sells Florida subsidiary
Astrana Health is buying Centene’s Collaborative Health Systems (CHS), a management services organizations across 17 states, for an undisclosed fee.
The transaction will close at the end of the year. Astrana is a provider-centric health tech company helping providers participate in value-based care arrangements.
"With this acquisition, we believe Astrana will be even better positioned to deliver accessible, high-quality, and high-value care to more patients across the nation," said president and CEO of Astrana Health Brandon Sim in a news release. "CHS has built a scaled and impactful value-based care ecosystem in markets spanning the South and East Coast.”
State Medicaid contracts
Florida’s big Medicaid losers are no longer big losers
In April, UnitedHealthcare, Aetna and Molina Healthcare were not awarded Medicaid contracts from the state of Florida. Instead, just Humana, Centene and Elevance Health were selected to administer the program.
This month, the three insurers left out of the initial awards agreed to contracts with the state after all. All three insurers expressed desire to challenge the initial losses.
The insurers were given HIV/AIDS and serious mental illness specialty awards. Aetna and UnitedHealthcare will help manage three regions, while Molina will manage just one region. Florida Community Care and Community Care Plan were also given additional contracts.
Tufts Public Health Plan loses out on Rhode Island Medicaid contract
Rhode Island will have just two health plans manage its Medicaid program: UnitedHealthcare and Neighborhood Health Plan.
Tufts Public Health Plans, the state’s other managed care plan currently contracted, did not earn an award for the next five year cycle, starting next year.
UnitedHealthcare has enjoyed an ongoing contract with Rhode Island since 1993, the company said in a news release.
Aetna fails in Kansas Medicaid complaints
Kansas is denying the attempts of Aetna Better Health and CareSource Kansas to administer the state’s Medicaid program, reports the Kansas Reflector.
This means Healthy Blue, a Blue Cross Blue Shield member will likely retain its contract with the state, in addition to UnitedHealthcare and Centene. Fierce Healthcare previously reported on the KanCare contract award announcement.
BCBSNC losing 700,000 members to Aetna in North Carolina
Blue Cross Blue Shield of North Carolina has opted not to appeal a loss in court that will see the health plan lose more than 700,000 state workers switch to Aetna in January 2025, WRAL reported.
The state determined Aetna scored better on certain questions. Blue Cross subsequently sued, but the court said the insurer did not have enough evidence it was scored unfairly.
Medicaid Section 1115 waivers
Illinois, New Hampshire launching incarceration support program
Under a Section 1115 Medicaid extension (PDF), Illinois is creating a new program to give services to eligible incarcerated individuals.
Services covered, as approved by CMS, include: case management to address behavioral health needs, medication-assisted treatment for substance use disorder, a 30-day supply for prescription medications, diagnostic and treatment services and medical equipment.
“The pre-release benefit package is designed to improve care transitions of such individuals back to the community, including by promoting continuity of coverage, service receipt, and quality of care, as well as the proactive identification of both physical and behavioral health needs and HRSN,” the waiver reads.
A similar program (PDF) has been approved in New Hampshire, providing pre-release services for eligible individuals that include substance use disorder or other behavioral health conditions.
Colorado adds doula services under Medicaid
Colorado has added coverage for doula services for pregnant members in Medicaid, the state announced this month.
The state’s Medicaid program covers 40% of births in Colorado, a news release said.
“There is a wealth of research that shows doula support can help reduce epidural use, labor duration, low-birthweight and premature deliveries, and postpartum depression rates,” said Adela Flores-Brennan in a statement. “There’s also evidence doula support leads to reduced c-section rates, which is higher in the BIPOC population and contributes to morbidity and mortality.”
Doulas are professionals that provide guidance before, during and after childbirth.
Miscellaneous
Insurer customer experience crashes to five-year low
A recent analysis from consulting firm Forrester Research found that health insurers’ customer experience has declined significantly.
Ten brands scored their lowest ratings in five years, while five brands had their first statistically significant declines. Nearly one-third of the industry earned poor ratings.
Insurers that had rating decreases included Kaiser Permanente, Humana, Florida Blue, Blue Cross and Blue Shield of Texas, Anthem Blue Cross and Blue Shield.
Optum, Caron Treatment Centers team up on substance use disorder
A substance use disorder residential program for teenagers is now in-network with Optum in Pennsylvania.
The agreement covers various lengths of stay. Programming also includes gender-affirming care and other gender-specific programming.
“As a mission-driven organization, we strive to help as many individuals as possible who struggle with addiction—and their families—thrive in recovery,” said John Driscoll, CEO of Caron Treatment Centers. in a news release. “However, access to quality addiction treatment remains a barrier for many, which is why we’re committed to expanding access to treatment and recovery services across our continuum.

Acquisition
02 Nov 2023
Healthcare mergers and acquisitions are in no short supply as providers, retailers, health tech companies and other industry players look to expand their businesses and gain a competitive edge.
Healthcare mergers and acquisitions are in no short supply as providers, health tech companies, retailers and other industry players look to expand their businesses and gain a competitive edge. Here’s a roundup of new deals that were revealed, closed, rumored or called off during the month of October.
Providers
UnityPoint Health and Presbyterian Healthcare Services called off plans for a cross-market merger. The entity would have spanned 48 hospitals with $11 billion in annual revenue. The systems did not share why they called off the deal, only noting to reporters that regulatory approvals didn’t play a role. However, the news came alongside word that UnityPoint President and CEO Clay Holderman would be leaving the organization.
Henry Ford Health came together with several of Ascension Michigan’s hospitals and other facilities to form a joint venture with over $10.5 billion in annual operating revenue. The deal is expected to close in summer 2024 and create an entity with about 50,000 employees, 13 acute care hospitals and over 550 sites of care under the Henry Ford Health branding. The organizations stressed that their pending deal is “neither a merger nor an acquisition” with no cash transaction taking place.
Aspirus Health and St. Luke’s Duluth took their merger plans a step forward with the signing of a definitive agreement. The tentative deal that was first announced back in July would yield a 19-hospital nonprofit. The agreement targets spring 2024 for a close, pending regulatory approvals, and outlines hundreds of millions of investments into St. Luke’s strategic projects. Minnesota Attorney General Keith Ellison said he is reviewing the deal.
Prospect Medical Holdings agreed to sell off the struggling four-hospital Crozer Health in order to fend off litigation from the Pennsylvania attorney general’s office and a local nonprofit. The private equity firm had acquired Crozer in 2016 and sought to close a failing hospital, which the groups said it was required to operate until at least 2026. Prospect said it hired Morgan Stanley to advise on a sale that it expects to move forward within 60 days.
UPMC (PDF) entered into a definitive integration and affiliation agreement with Washington Health Care Services. Per a notice, UPMC would appoint a third of the two-hospital system’s board once the deal is closed. The deal is still pending regulatory signoffs.
Mountain Health Network, Marshall Health, Marshall University and an 80-member multispecialty physician group came together in a four-hospital academic health system dubbed Marshall Health Network, based in West Virginia.
UC San Diego Health is purchasing Alvarado Hospital Medical Center from Prime Healthcare for $200 million. The organizations are aiming to close their deal before the end of the year.
Parkview Health picked up two Ohio hospitals and an outpatient center in an affiliation deal that closed in early October.
USA Health, the academic health system of the University of South Alabama, added the 349-bed Ascension Providence Hospital and its associated clinics. The system had purchased the facilities for $85 million.
Yale New Haven Health acquired PhysicianOne Urgent Care, which operates 27 locations across Connecticut, Rhode Island, Massachusetts and New York.
Payers
Blue Cross and Blue Shield of North Carolina will acquire 55 FastMed locations in North Carolina for an undisclosed sum. Blue Cross NC, which has been a minority investor in FastMed since 2012, said it plans to invest in the locations to build on patient experience and access to critical services. The pending deal is expected to close in early 2024 pending approvals.
Blue Cross Blue Shield of Vermont received an all-clear from its state’s regulators to become a subsidiary of Blue Cross Blue Shield of Michigan. The deal, unveiled back in May, is said to generate savings for the former company through shared contracts and vendors. The arrangement will also leave both organizations in charge of their respective governance, operations and policies.
Froedtert Health is buying out Ascension’s 50% stake in Network Health, a Wisconsin health plan jointly run by the nonprofit health systems. The plan offers commercial and Medicare health insurance plans across 23 of the state’s counties and currently serves more than 117,000 members. Financial terms and a target closing window were not disclosed.
Tech
IKS Health, a company that provides administrative, clinical, operational and revenue tech solutions, acquired AQuity Solutions for $200 million to broaden its services from ambulatory care providers to hospitals. The resulting entity will have annual revenues of more than $330 million and an expanded workforce of more than 14,000 employees serving over 150,000 clinicians in many of the largest hospitals, health systems and specialty groups in the U.S.
Olive AI, a healthcare automation unicorn, announced the sale of its remaining assets amid a shutdown of operations. Its clearinghouse and patient access business units were acquired by Waystar, while the prior authorization business unit has gone to Humata Health.
MDLIVE, the telehealth arm of healthcare payer Cigna’s Evernorth, is acquiring Bright.md for an undisclosed sum. The deal will help MDLIVE launch asynchronous options for virtual urgent care in the coming year.
Commure, which sells tech tools to health systems, unveiled a deal to merge with healthcare workflow automation software maker Athelas by the end of October. The combined company will have about 800 employees with plans to scale up thanks to a $70 million investment from General Catalyst that puts the combined entity at a reported valuation of $6 billion. Other financial terms of the deal were not disclosed.
Access Healthcare, a tech-enabled revenue cycle management and healthcare services firm, acquired patient engagement services company Envera Health to broaden its portfolio of capabilities. Terms were not disclosed.
WellSky, a software and services vendor, picked up post-acute care tech services firm Corridor from HealthEdge Investment Partners. The deal, for which financial details were not disclosed, will help WellSky expand its medical coding and revenue cycle management offerings.
Vizient acquired PrefTech OR, a preference card management software maker serving providers, for an undisclosed sum.
The American Health Information Management Association acquired HCPro, which offers educational and compliance-related revenue cycle management products and services, from its parent company Simplify Compliance. The nonprofit association will be operating HCPro as a for-profit, wholly owned subsidiary.

Acquisition
05 Oct 2023
The deal, which is pending review, would give Froedtert Health full ownership of a commercial and Medicare payer with 117,000 members.
Froedtert Health is buying out Ascension’s 50% stake in a Wisconsin health plan jointly run by the nonprofit health systems, the former announced this week.
The plan, Network Health, offers commercial and Medicare health insurance plans across 23 of the state’s counties. It currently serves more than 117,000 members, which the systems said will not see any disruptions in coverage as a result of the deal.
“The opportunity to acquire 100% ownership of Network Health is consistent with our mission to advance the health of the people of the diverse communities we serve through exceptional care enhanced by innovation and discovery,” Cathy Jacobson, president and CEO of Milwaukee-based Froedtert Health, said in a statement. “As a proven health insurance plan that consistently receives top ratings from the Centers for Medicare and Medicaid Services, we’re confident this investment will complement our robust population health strategy, allowing us to care for more people at the right place and at the right time.”
Financial terms of the deal were not disclosed. The organizations also held off on setting a specific window for the sale’s close, which they said would be contingent on regulatory review and approval.
Ascension Wisconsin—the 17-hospital subsidiary system of St. Louis-based Ascension that controlled the stake in Network Health—plans to extend its provider agreement and remain in-network for members following the deal’s close, according to the announcement.
Network Health was founded in 1982, though Froedtert didn’t buy in until 2014 when it spent almost $108 million for its stake.
Word of the remaining half’s purchase comes just a month after Froedtert announced it was all-in on a potential merger with fellow nonprofit system ThedaCare, a deal that would yield an 18-hospital, multibillion-dollar organization.
Ascension, meanwhile, can likely use the money it would receive from the sale. The Catholic juggernaut recently reported a nearly $2.7 billion net loss for the fiscal year ended June 30, which it said was driven by a combination of high expenses, “sustained revenue challenges” and a one-time noncash impairment loss of almost $1.5 billion.

Acquisition
100 Deals associated with Tufts Health Public Plans, Inc.
Login to view more data
100 Translational Medicine associated with Tufts Health Public Plans, Inc.
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 05 Oct 2024
No data posted
Login to keep update
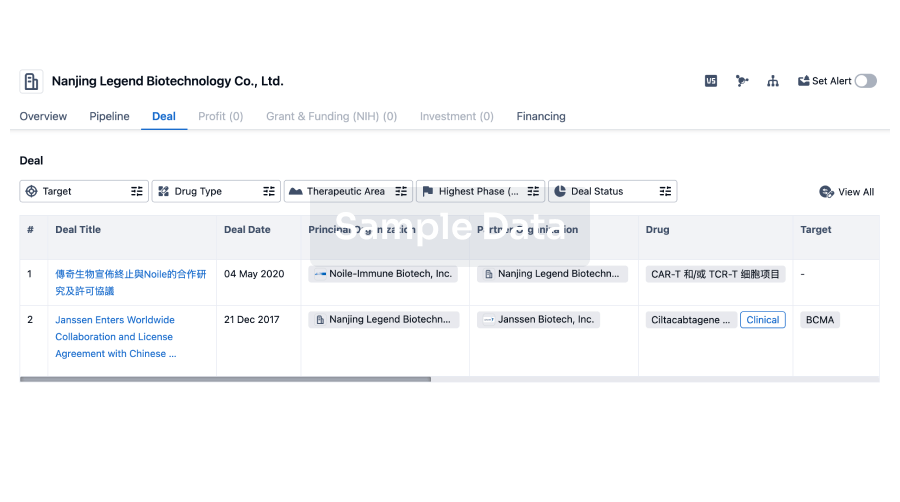
Deal
Boost your decision using our deal data.
login
or
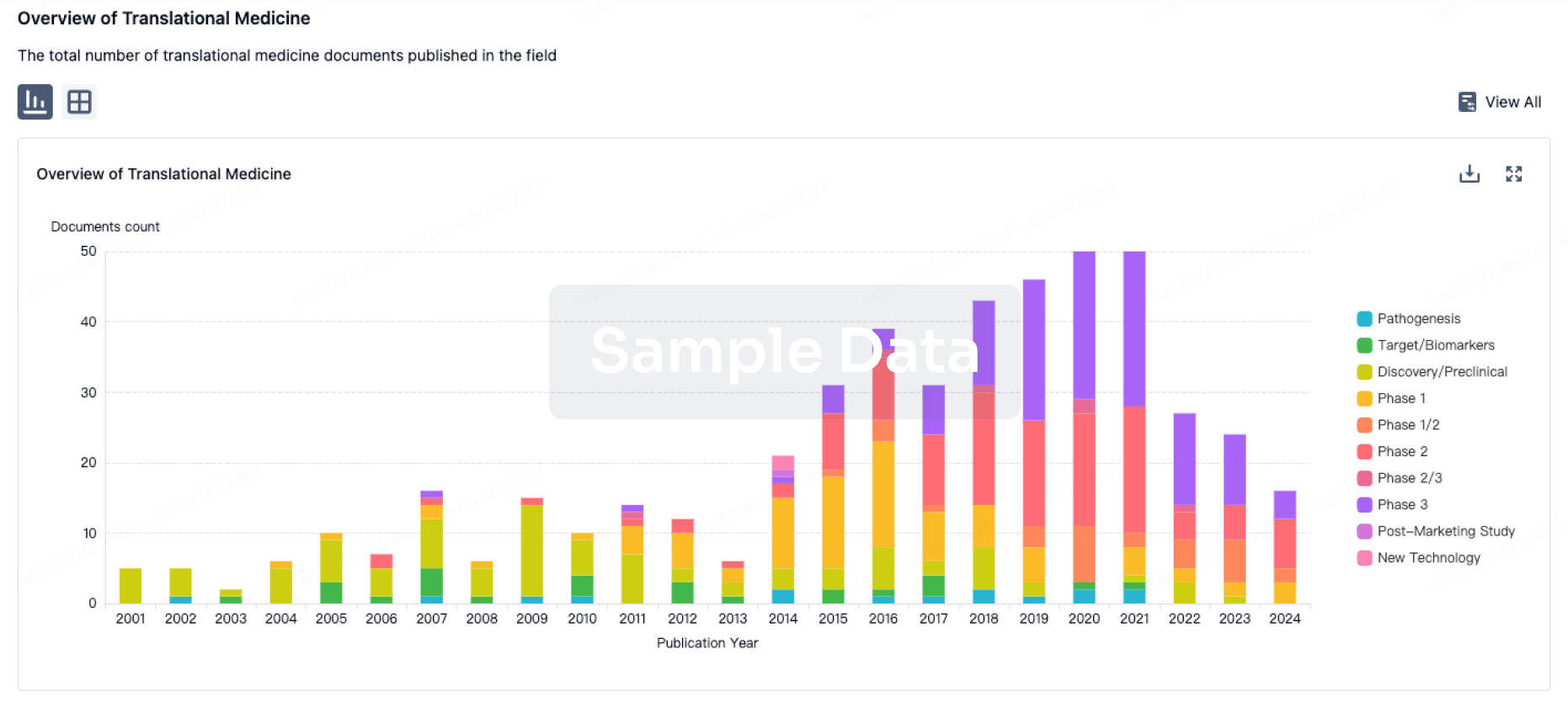
Translational Medicine
Boost your research with our translational medicine data.
login
or
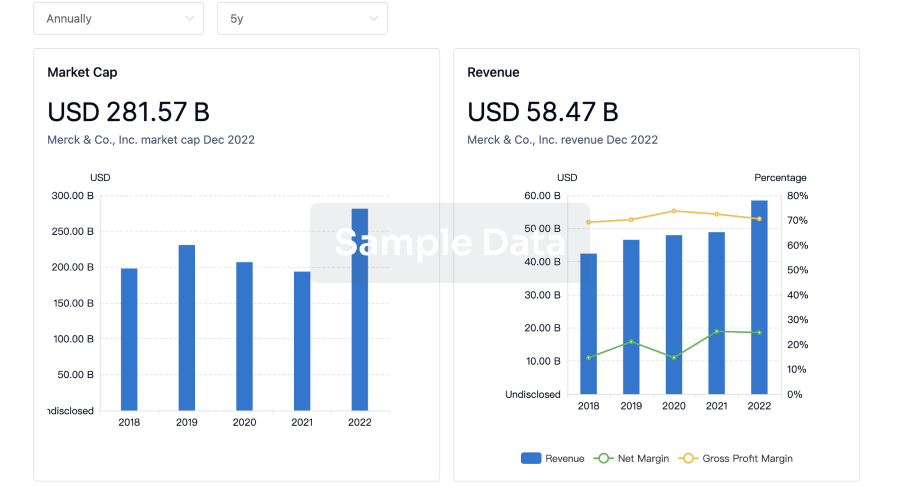
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
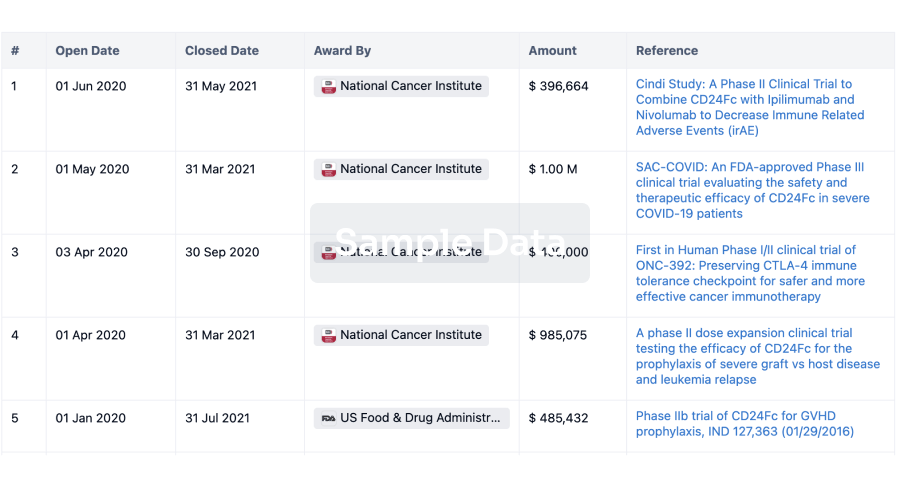
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
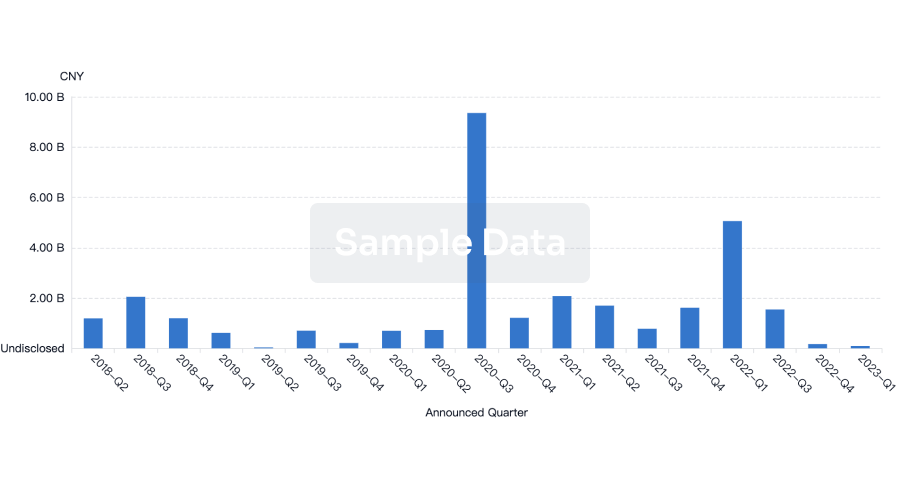
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free