Request Demo
What is the mechanism of Cefmenoxime Hydrochloride?
17 July 2024
Cefmenoxime Hydrochloride is a third-generation cephalosporin antibiotic, which is utilized primarily to combat a variety of bacterial infections. This antibiotic operates by inhibiting bacterial cell wall synthesis, thereby leading to cell death and alleviation of the infection. Understanding the mechanism of Cefmenoxime Hydrochloride requires an exploration of both its biochemical interactions and its pharmacodynamics.
Cefmenoxime Hydrochloride works by targeting the penicillin-binding proteins (PBPs) found within the bacterial cell wall. PBPs play a crucial role in the synthesis and maintenance of the peptidoglycan layer, which is essential for bacterial cell wall integrity. Specifically, PBPs are responsible for the final stages of assembling the peptidoglycan lattice, which involves cross-linking peptide chains. By binding to these PBPs, Cefmenoxime Hydrochloride disrupts this process, leading to the formation of a defective cell wall.
The binding of Cefmenoxime Hydrochloride to PBPs is facilitated by its beta-lactam ring, a common structural feature of cephalosporins. This beta-lactam ring mimics the D-alanyl-D-alanine portion of the peptidoglycan substrate, allowing the antibiotic to interfere with the transpeptidation reaction catalyzed by PBPs. As a result, the peptidoglycan synthesis is halted, rendering the bacterial cell wall weak and prone to lysis. The osmotic pressure within the bacterial cell becomes unmanageable without a robust cell wall, leading to cell death.
Additionally, Cefmenoxime Hydrochloride exhibits a broad spectrum of activity against both Gram-positive and Gram-negative bacteria. This broad-spectrum efficacy is primarily due to its ability to penetrate the outer membrane of Gram-negative bacteria, which is often a significant barrier to many antibiotics. The presence of a syn-methoxyimino group in Cefmenoxime Hydrochloride helps in resisting beta-lactamase enzymes produced by certain bacteria, which would normally degrade the antibiotic and render it ineffective.
Pharmacodynamically, Cefmenoxime Hydrochloride is characterized by its ability to achieve high concentrations in various body tissues and fluids, including cerebrospinal fluid, making it effective against infections in different anatomical locations. Furthermore, it exhibits a relatively long half-life, allowing for sustained antimicrobial activity and convenient dosing regimens.
In clinical practice, Cefmenoxime Hydrochloride is administered via intravenous or intramuscular injections. Its pharmacokinetic properties ensure rapid absorption and distribution, leading to prompt therapeutic effects. It is efficiently excreted by the kidneys, which necessitates dose adjustments in patients with renal impairment to avoid potential toxicity.
Despite its efficacy, the use of Cefmenoxime Hydrochloride, like other antibiotics, must be judicious to prevent the development of antibiotic resistance. Overuse and misuse of antibiotics can lead to the emergence of resistant strains of bacteria, which can significantly reduce the effectiveness of these critical drugs.
In conclusion, Cefmenoxime Hydrochloride operates through a well-defined mechanism involving the inhibition of bacterial cell wall synthesis via binding to penicillin-binding proteins. Its broad-spectrum activity and resistance to beta-lactamase enzymes make it a potent antibiotic for treating a range of bacterial infections. However, careful management and appropriate usage are essential to maintain its effectiveness and mitigate the risk of resistance. Understanding the detailed mechanism of Cefmenoxime Hydrochloride not only enhances its clinical application but also underscores the importance of ongoing research and stewardship in antibiotic use.
Cefmenoxime Hydrochloride works by targeting the penicillin-binding proteins (PBPs) found within the bacterial cell wall. PBPs play a crucial role in the synthesis and maintenance of the peptidoglycan layer, which is essential for bacterial cell wall integrity. Specifically, PBPs are responsible for the final stages of assembling the peptidoglycan lattice, which involves cross-linking peptide chains. By binding to these PBPs, Cefmenoxime Hydrochloride disrupts this process, leading to the formation of a defective cell wall.
The binding of Cefmenoxime Hydrochloride to PBPs is facilitated by its beta-lactam ring, a common structural feature of cephalosporins. This beta-lactam ring mimics the D-alanyl-D-alanine portion of the peptidoglycan substrate, allowing the antibiotic to interfere with the transpeptidation reaction catalyzed by PBPs. As a result, the peptidoglycan synthesis is halted, rendering the bacterial cell wall weak and prone to lysis. The osmotic pressure within the bacterial cell becomes unmanageable without a robust cell wall, leading to cell death.
Additionally, Cefmenoxime Hydrochloride exhibits a broad spectrum of activity against both Gram-positive and Gram-negative bacteria. This broad-spectrum efficacy is primarily due to its ability to penetrate the outer membrane of Gram-negative bacteria, which is often a significant barrier to many antibiotics. The presence of a syn-methoxyimino group in Cefmenoxime Hydrochloride helps in resisting beta-lactamase enzymes produced by certain bacteria, which would normally degrade the antibiotic and render it ineffective.
Pharmacodynamically, Cefmenoxime Hydrochloride is characterized by its ability to achieve high concentrations in various body tissues and fluids, including cerebrospinal fluid, making it effective against infections in different anatomical locations. Furthermore, it exhibits a relatively long half-life, allowing for sustained antimicrobial activity and convenient dosing regimens.
In clinical practice, Cefmenoxime Hydrochloride is administered via intravenous or intramuscular injections. Its pharmacokinetic properties ensure rapid absorption and distribution, leading to prompt therapeutic effects. It is efficiently excreted by the kidneys, which necessitates dose adjustments in patients with renal impairment to avoid potential toxicity.
Despite its efficacy, the use of Cefmenoxime Hydrochloride, like other antibiotics, must be judicious to prevent the development of antibiotic resistance. Overuse and misuse of antibiotics can lead to the emergence of resistant strains of bacteria, which can significantly reduce the effectiveness of these critical drugs.
In conclusion, Cefmenoxime Hydrochloride operates through a well-defined mechanism involving the inhibition of bacterial cell wall synthesis via binding to penicillin-binding proteins. Its broad-spectrum activity and resistance to beta-lactamase enzymes make it a potent antibiotic for treating a range of bacterial infections. However, careful management and appropriate usage are essential to maintain its effectiveness and mitigate the risk of resistance. Understanding the detailed mechanism of Cefmenoxime Hydrochloride not only enhances its clinical application but also underscores the importance of ongoing research and stewardship in antibiotic use.
How to obtain the latest development progress of all drugs?
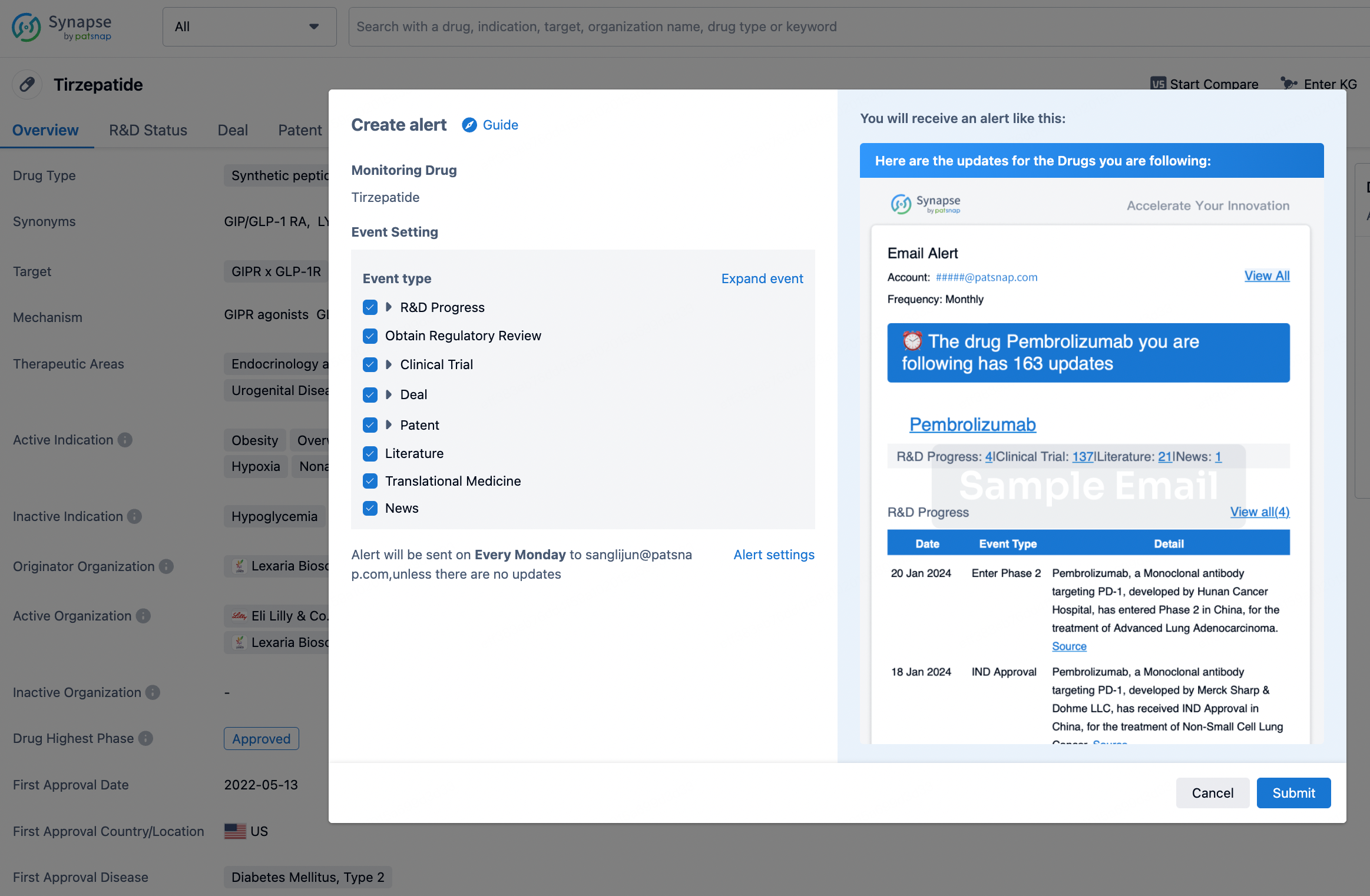
In the Synapse database, you can stay updated on the latest research and development advances of all drugs. This service is accessible anytime and anywhere, with updates available daily or weekly. Use the "Set Alert" function to stay informed. Click on the image below to embark on a brand new journey of drug discovery!
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.