Request Demo
What is Ublituximab used for?
14 June 2024
In recent years, the landscape of biopharmaceuticals has seen the emergence of various monoclonal antibodies designed to target specific components of the immune system in order to treat a host of autoimmune and malignancy conditions. Ublituximab is one such promising monoclonal antibody, with potential applications in the treatment of multiple sclerosis (MS) and certain types of cancer, particularly B-cell malignancies like chronic lymphocytic leukemia (CLL) and non-Hodgkin's lymphoma (NHL).
Ublituximab is currently being developed by TG Therapeutics, a biopharmaceutical company specializing in the development of treatments for B-cell diseases. It operates under the trade name "Ublituximab" itself, without any additional trade names at this stage. The drug is classified as an anti-CD20 monoclonal antibody, aiming to deplete B-cells by targeting the CD20 antigen found on the surface of these cells. This mechanism is shared by other anti-CD20 monoclonal antibodies like rituximab and ocrelizumab, but ublituximab offers unique advantages, including potential higher potency and lower infusion times.
Clinical trials have demonstrated encouraging results. For instance, in the treatment of relapsing-remitting multiple sclerosis (RRMS), ublituximab has shown significant reductions in annualized relapse rates and MRI brain lesions. In oncology, it has exhibited promising efficacy in combination therapy regimens for CLL and NHL. As of now, ublituximab is in late-stage clinical trials for these indications, and its approval by regulatory bodies like the FDA is anticipated in the near future.
The mechanism of action of ublituximab primarily revolves around its ability to target the CD20 antigen, a specific protein expressed on the surface of B-cells. By binding to CD20, ublituximab flags these cells for destruction through multiple pathways. One major pathway is antibody-dependent cellular cytotoxicity (ADCC), where immune cells like natural killer (NK) cells recognize the bound antibody and destroy the B-cell. Another pathway is complement-dependent cytotoxicity (CDC), wherein the binding of ublituximab activates the complement system, a part of the immune system that leads to the lysis or bursting of the B-cell. Additionally, ublituximab can induce direct apoptosis or programmed cell death in B-cells, contributing to its efficacy in depleting these cells.
Understanding how to use ublituximab is crucial for both healthcare providers and patients. The drug is administered through intravenous (IV) infusion, typically in a clinical setting under medical supervision. The dosing regimen can vary depending on the indication and patient-specific factors. For example, in the treatment of multiple sclerosis, initial doses are followed by maintenance doses at regular intervals, which can be every six months. The onset of action may vary, but patients often experience therapeutic effects within days to weeks of the first infusion. Premedication with corticosteroids, antihistamines, and antipyretics is common practice to minimize infusion-related reactions, which can occur with monoclonal antibody therapies.
Like any medication, ublituximab is associated with potential side effects and contraindications. Common side effects include infusion-related reactions such as fever, chills, rash, headache, and nausea. These reactions are generally mild to moderate in severity and can be managed with premedication and supportive care. More serious but less common side effects may include infections, as the depletion of B-cells can weaken the immune system. Patients may be at increased risk for upper respiratory infections, urinary tract infections, and even opportunistic infections like progressive multifocal leukoencephalopathy (PML), a rare but serious brain infection.
Contraindications for the use of ublituximab include known hypersensitivity to the drug or any of its components. Additionally, patients with active infections should not receive ublituximab until the infection is resolved. Caution is also warranted in patients with a history of hepatitis B, as reactivation of the virus can occur. Patients should undergo screening for hepatitis B virus (HBV) before starting treatment and be monitored during and after treatment for signs of reactivation.
It is also important to consider potential drug interactions with ublituximab. While comprehensive interaction studies are ongoing, it is known that immunosuppressive therapies and biologics can interact with ublituximab. Concomitant use of other immunosuppressants may increase the risk of infections and other immune-related adverse effects. Patients should inform their healthcare providers about all medications they are taking, including over-the-counter drugs, supplements, and herbal products. Vaccinations, particularly live vaccines, should generally be avoided during and after treatment with ublituximab due to the risk of reduced vaccine efficacy and increased risk of infection.
In summary, ublituximab represents a significant advancement in the treatment of autoimmune diseases like multiple sclerosis and B-cell malignancies. Its mechanism of action allows for targeted depletion of B-cells, providing therapeutic benefits while minimizing off-target effects. Understanding the proper administration, potential side effects, and drug interactions is essential for optimizing treatment outcomes. As research progresses, ublituximab holds promise for improving the quality of life for patients suffering from these challenging conditions.
Ublituximab is currently being developed by TG Therapeutics, a biopharmaceutical company specializing in the development of treatments for B-cell diseases. It operates under the trade name "Ublituximab" itself, without any additional trade names at this stage. The drug is classified as an anti-CD20 monoclonal antibody, aiming to deplete B-cells by targeting the CD20 antigen found on the surface of these cells. This mechanism is shared by other anti-CD20 monoclonal antibodies like rituximab and ocrelizumab, but ublituximab offers unique advantages, including potential higher potency and lower infusion times.
Clinical trials have demonstrated encouraging results. For instance, in the treatment of relapsing-remitting multiple sclerosis (RRMS), ublituximab has shown significant reductions in annualized relapse rates and MRI brain lesions. In oncology, it has exhibited promising efficacy in combination therapy regimens for CLL and NHL. As of now, ublituximab is in late-stage clinical trials for these indications, and its approval by regulatory bodies like the FDA is anticipated in the near future.
The mechanism of action of ublituximab primarily revolves around its ability to target the CD20 antigen, a specific protein expressed on the surface of B-cells. By binding to CD20, ublituximab flags these cells for destruction through multiple pathways. One major pathway is antibody-dependent cellular cytotoxicity (ADCC), where immune cells like natural killer (NK) cells recognize the bound antibody and destroy the B-cell. Another pathway is complement-dependent cytotoxicity (CDC), wherein the binding of ublituximab activates the complement system, a part of the immune system that leads to the lysis or bursting of the B-cell. Additionally, ublituximab can induce direct apoptosis or programmed cell death in B-cells, contributing to its efficacy in depleting these cells.
Understanding how to use ublituximab is crucial for both healthcare providers and patients. The drug is administered through intravenous (IV) infusion, typically in a clinical setting under medical supervision. The dosing regimen can vary depending on the indication and patient-specific factors. For example, in the treatment of multiple sclerosis, initial doses are followed by maintenance doses at regular intervals, which can be every six months. The onset of action may vary, but patients often experience therapeutic effects within days to weeks of the first infusion. Premedication with corticosteroids, antihistamines, and antipyretics is common practice to minimize infusion-related reactions, which can occur with monoclonal antibody therapies.
Like any medication, ublituximab is associated with potential side effects and contraindications. Common side effects include infusion-related reactions such as fever, chills, rash, headache, and nausea. These reactions are generally mild to moderate in severity and can be managed with premedication and supportive care. More serious but less common side effects may include infections, as the depletion of B-cells can weaken the immune system. Patients may be at increased risk for upper respiratory infections, urinary tract infections, and even opportunistic infections like progressive multifocal leukoencephalopathy (PML), a rare but serious brain infection.
Contraindications for the use of ublituximab include known hypersensitivity to the drug or any of its components. Additionally, patients with active infections should not receive ublituximab until the infection is resolved. Caution is also warranted in patients with a history of hepatitis B, as reactivation of the virus can occur. Patients should undergo screening for hepatitis B virus (HBV) before starting treatment and be monitored during and after treatment for signs of reactivation.
It is also important to consider potential drug interactions with ublituximab. While comprehensive interaction studies are ongoing, it is known that immunosuppressive therapies and biologics can interact with ublituximab. Concomitant use of other immunosuppressants may increase the risk of infections and other immune-related adverse effects. Patients should inform their healthcare providers about all medications they are taking, including over-the-counter drugs, supplements, and herbal products. Vaccinations, particularly live vaccines, should generally be avoided during and after treatment with ublituximab due to the risk of reduced vaccine efficacy and increased risk of infection.
In summary, ublituximab represents a significant advancement in the treatment of autoimmune diseases like multiple sclerosis and B-cell malignancies. Its mechanism of action allows for targeted depletion of B-cells, providing therapeutic benefits while minimizing off-target effects. Understanding the proper administration, potential side effects, and drug interactions is essential for optimizing treatment outcomes. As research progresses, ublituximab holds promise for improving the quality of life for patients suffering from these challenging conditions.
How to obtain the latest development progress of all drugs?
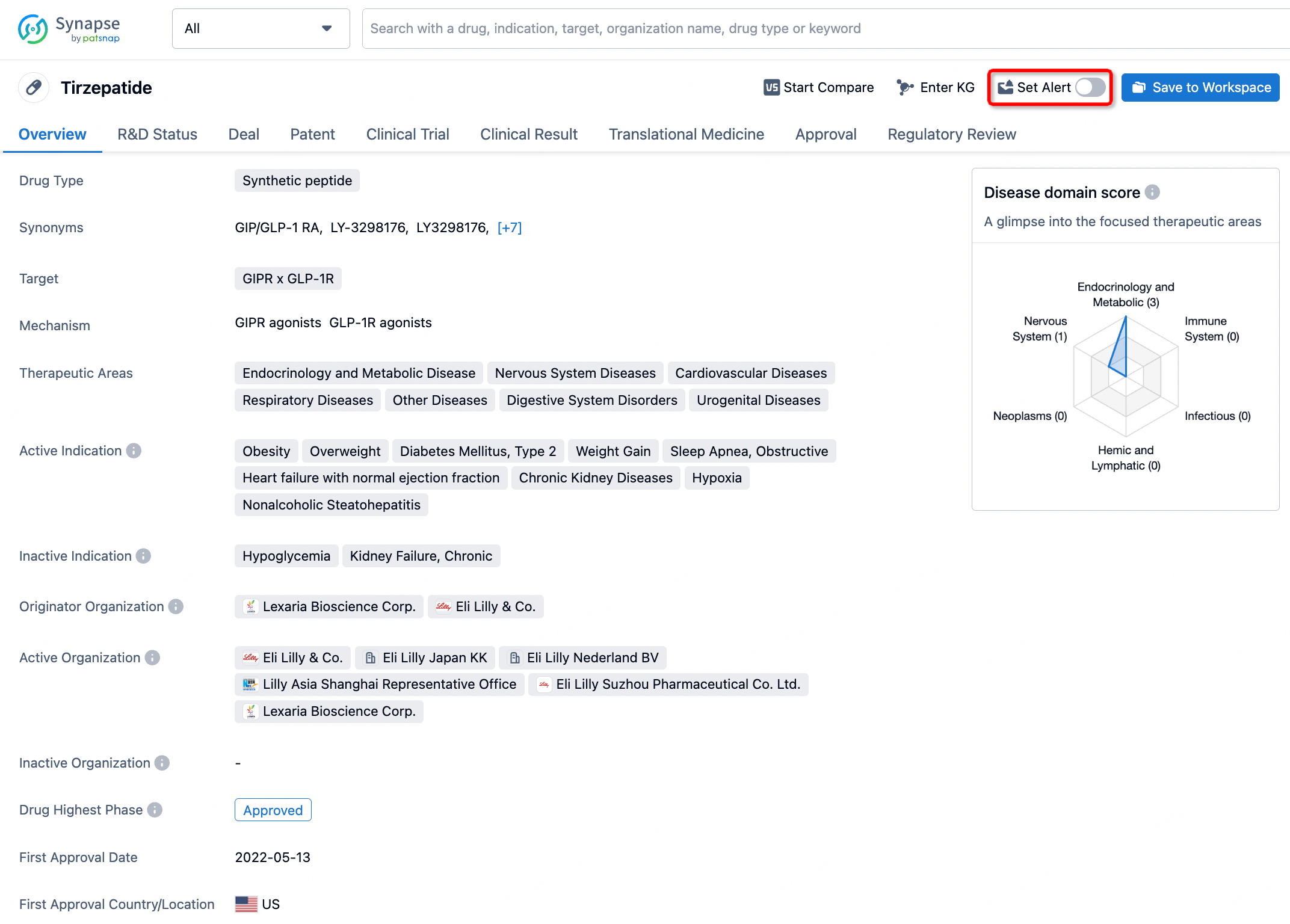
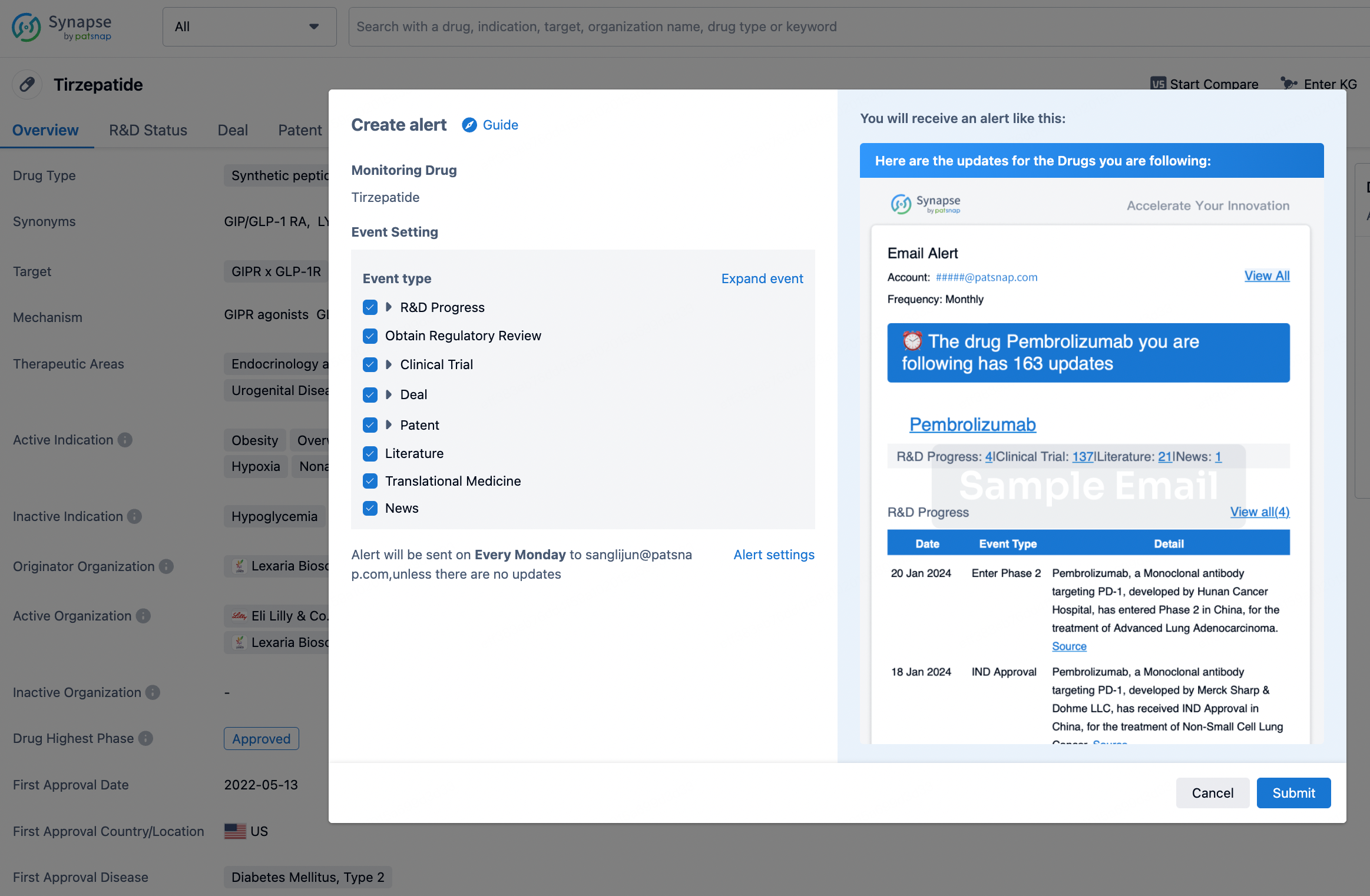
In the Synapse database, you can stay updated on the latest research and development advances of all drugs. This service is accessible anytime and anywhere, with updates available daily or weekly. Use the "Set Alert" function to stay informed. Click on the image below to embark on a brand new journey of drug discovery!
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.