Request Demo
Last update 23 May 2026
Talquetamab
Last update 23 May 2026
Overview
Basic Info
Drug Type Bispecific T-cell Engager (BiTE) |
Synonyms DuoBody, TALQUETAMAB-TGVS, 替吉妥单抗 + [7] |
Target |
Action stimulants, inhibitors |
Mechanism CD3 stimulants(T cell surface glycoprotein CD3 stimulants), GPRC5D inhibitors(G-protein coupled receptor family C group 5member D inhibitors), ADCC(Antibody-dependent cell-mediated cytotoxicity (ADCC) effects) |
Therapeutic Areas |
Active Indication |
Inactive Indication- |
Originator Organization |
Inactive Organization- |
License Organization- |
Drug Highest PhaseApproved |
First Approval Date United States (09 Aug 2023), |
RegulationBreakthrough Therapy (United States), Accelerated Approval (United States), Orphan Drug (United States), Orphan Drug (European Union), PRIME (European Union), Priority Review (China), Breakthrough Therapy (China), Conditional marketing approval (China), Orphan Drug (Japan), Orphan Drug (South Korea), Conditional marketing approval (European Union) |
Login to view timeline
Structure/Sequence
Sequence Code 10086313H

Source: *****
Sequence Code 10086327L

Source: *****
Sequence Code 453116282H

Source: *****
Sequence Code 525754800L

Source: *****
Related
40
Clinical Trials associated with TalquetamabNCT07474961
A Multicentre, Adaptive, Randomised, Multidomain, Platform Trial for Dose Optimization in the Treatment of Adult Patients With Haematological Diseases (BLOOD-dose): Core Protocol
BLOOD-dose is a multicentre, adaptive, randomized, multidomain platform trial designed to optimize treatment dosing strategies in adult patients with haematological diseases.
The BLOOD-dose core protocol outlines the overall clinical trial design that applies to all included interventions, while domain-specific appendices (DSA) detail the unique characteristics of each domain and specify domain-specific interventions.
New domains will be incorporated over time to address distinct dose-optimization research questions across different haematological conditions and interventions.
The BLOOD-dose core protocol outlines the overall clinical trial design that applies to all included interventions, while domain-specific appendices (DSA) detail the unique characteristics of each domain and specify domain-specific interventions.
New domains will be incorporated over time to address distinct dose-optimization research questions across different haematological conditions and interventions.
Start Date01 Mar 2027 |
Sponsor / Collaborator |
NCT07029776
A Phase 2 Study Exploring the Use of Bispecific Antibodies to Improve Progression Free Survival in Patients With High-Risk Newly Diagnosed Multiple Myeloma (MMulti-Immune HR)
The purpose of this research is to learn whether using teclistamab and talquetamab at different time points will improve survival in participants with high-risk Multiple Myeloma (MM).
The treatment on this study will consist of Induction chemotherapy and stem cell collection, Immunotherapy 1 chemotherapy and Immunotherapy 2 chemotherapy. For participants whose testing show they are Minimal Residual Disease (MRD) positive (still have myeloma cells present in the bone marrow testing), a Melphalan-based stem cell transplant will be performed. For participants whose testing show they are MRD negative, the stem cell transplant will not be performed. All participants will go on to receive Immunotherapy 3 chemotherapy, Immunotherapy 4 chemotherapy, and Maintenance therapy.
The treatment on this study will consist of Induction chemotherapy and stem cell collection, Immunotherapy 1 chemotherapy and Immunotherapy 2 chemotherapy. For participants whose testing show they are Minimal Residual Disease (MRD) positive (still have myeloma cells present in the bone marrow testing), a Melphalan-based stem cell transplant will be performed. For participants whose testing show they are MRD negative, the stem cell transplant will not be performed. All participants will go on to receive Immunotherapy 3 chemotherapy, Immunotherapy 4 chemotherapy, and Maintenance therapy.
Start Date01 Jul 2026 |
Sponsor / Collaborator |
NCT07581704
Impact of Sirolimus Pre-conditioning on T Cell Activity and T-cell Engaging Bispecific Antibody Efficacy in Multiple Myeloma
This is a single center, single arm Phase Ib study with expansion cohort designed to establish the safety and physiologic effects of sirolimus pre-conditioning followed by T-cell engaging bispecific antibody therapy.
Start Date30 Jun 2026 |
Sponsor / Collaborator |
100 Clinical Results associated with Talquetamab
Login to view more data
100 Translational Medicine associated with Talquetamab
Login to view more data
100 Patents (Medical) associated with Talquetamab
Login to view more data
129
Literatures (Medical) associated with Talquetamab31 Dec 2026·JOURNAL OF MEDICAL ECONOMICS
Costs per responder for patients with relapsed or refractory multiple myeloma treated with Talquetamab compared with usual care
Article
Author: Mu, Fan ; Patel, Neel ; Yang, Chelsey ; Jiao, Tianze ; Liu, Yi-Hsuan ; Grajales-Cruz, Ariel F. ; Lee, Hans C. ; Zhang, Xinke ; Wang, Jiamin ; Goble, Joseph
AIMS:
To evaluate costs per responder for patients with triple-class exposed (TCE) relapsed or refractory multiple myeloma (RRMM) receiving talquetamab (Tal) on weekly (QW) and biweekly (Q2W) dosing schedules, compared with usual care from a United States commercial payer's perspective.
METHODS:
A cost per responder model was developed over a 6-month time horizon, incorporating pre-progression and post-progression costs. For Tal QW and Tal Q2W, pre-progression costs included costs of drug acquisition, inpatient step-up doses (hospitalization, pre-medication, and tocilizumab), outpatient visits, and monitoring. Pre-progression costs for usual care were estimated based on a weighted average of the 10 most used regimens in a real-world LocoMMotion/MoMMent study, including costs of acquisition, administration, co-medication, and monitoring. Post-progression costs included subsequent treatment for a subset of patients and terminal care costs prior to death. All costs were reported in 2025 United States Dollars. Clinical data of overall response rate (ORR), progression-free survival, and overall survival were obtained from an indirect treatment comparison using MonumenTAL-1 (September 2024 data cut) and LocoMMotion/MoMMent (October 2022 and August 2023 data cuts) as data sources. Deterministic sensitivity analyses and scenario analyses were conducted to assess the robustness of model results.
RESULTS:
Over the 6-month period, the total cost of care was $179,556 for usual care, $295,993 for Tal QW, and $315,135 for Tal Q2W. Despite higher costs, Tal demonstrated superior ORR, resulting in lower cost per responder: $575,962 for usual care, $405,470 for Tal QW, and $443,165 for Tal Q2W, representing a 23-30% reduction in cost per responder with Tal. Sensitivity and scenario analyses showed consistent findings.
CONCLUSION:
Although Tal QW and Q2W are associated with higher total per-patient costs compared with usual care, they offer improved clinical effectiveness, resulting in lower cost per responder. These findings suggest greater economic value for Tal in the treatment of TCE RRMM.
29 Apr 2026·Blood Cancer Journal
Efficacy and safety of talquetamab in relapsed/refractory multiple myeloma and renal impairment: a quaternary cancer center cohort.
Letter
Author: Anwer, Faiz ; McDonald, Alexandra ; Roy, Tara ; Rudoni, Joslyn ; Raza, Shahzad ; Pasquini, Marcelo C ; Basali, Diana ; Kissam, Jonathan ; Khouri, Jack ; Hamilton, Kimberly ; Goel, Utkarsh ; Samaras, Christy J ; Valent, Jason ; Mazzoni, Sandra ; Mathur, Saveta ; Bevacqua, Julie ; Ali, Hossam M ; Faiman, Beth M ; Rice, Mikhaila ; Scott, Cynthia ; Van Heeckeren, Willem ; Williams, Louis S
28 Apr 2026·Blood Advances
Vestibular symptoms after talquetamab therapy in heavily pretreated multiple myeloma
Article
Author: Vesole, David ; Phull, Pooja ; Biran, Noa ; Parmar, Harsh ; Di Palma-Grisi, James ; Siegel, David
145
News (Medical) associated with Talquetamab12 May 2026
SPRING HOUSE, Pa., (May 12, 2026) – Johnson & Johnson (NYSE: JNJ) announced today more than 30 hematology abstracts featuring data in multiple myeloma and leukemia, as well as in warm autoimmune hemolytic anemia (wAIHA), will be shared at the European Hematology Association (EHA) 2026 Congress from June 11-14 in Stockholm, Sweden. Among the results to be presented in a plenary session is the Phase 3 MonumenTAL-3 study investigating TALVEY® (talquetamab-tgvs), a GPRC5D bispecific antibody, in combination with DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) with or without pomalidomide in relapsed/refractory multiple myeloma. New pivotal data from the Phase 2/3 ENERGY study evaluating IMAAVY® (nipocalimab-aahu)a in wAIHA, a rare autoantibody-driven disease in which autoantibodies attach to and destroy red blood cells, will also be presented in an oral session.1 The U.S. Food and Drug Administration (FDA) recently granted Priority Review to IMAAVY ® in wAIHA.
Perspectives on key data readouts at EHA“The data we are sharing at EHA 2026 reflect the depth and breadth of our clinical innovations in blood cancer, led by the Phase 3 MonumenTAL-3 results, which are an exciting next step in exploring how we can continue to expand our portfolio of differentiated and combinable therapies in multiple myeloma,” said Yusri Elsayed, M.D., M.H.Sc., Ph.D., Global Therapeutic Area Head, Oncology, Johnson & Johnson. “Together with additional data in leukemia, these findings underscore our leadership in hematology and our continued commitment to advancing meaningful innovation for patients living with complex blood cancers.”
“wAIHA is marked by debilitating fatigue and serious complications of severe anemia. There is an unmet need for an approved treatment for wAIHA that may provide rapid control and sustained relief from symptoms while preserving critical immune functions,” said David Lee, M.D., Ph.D., Global Immunology Therapeutic Area Head, Johnson & Johnson. “The first presentation of Phase 2/3 results from the ENERGY study highlights the potential of an immunoselective treatment approach for wAIHA, which is a rare disease with no U.S. FDA-approved treatments.”
Updated data in multiple myelomaData at EHA will highlight advances in multiple myeloma treatment, including combination regimens and emerging therapies for patients with newly diagnosed and relapsed/refractory multiple myeloma.
New results from the Phase 3 MonumenTAL-3 study evaluating TALVEY® in combination with DARZALEX FASPRO® with or without pomalidomide versus DARZALEX FASPRO®, pomalidomide, and dexamethasone in relapsed/refractory multiple myeloma (Presented as “One of the six best abstracts” during the Plenary Abstracts Session #S100) Subgroup analysis based on cytogenetic and functional risk from the MajesTEC-3 study evaluating TECVAYLI® (teclistamab-cqyv) in combination with DARZALEX FASPRO® in relapsed/refractory multiple myeloma (Oral Abstract #S198) Cytogenetic subgroup analysis from the Phase 3 CARTITUDE-4 study evaluating CARVYKTI® (ciltacabtagene autoleucel; cilta-cel) in patients with lenalidomide-refractory multiple myeloma responding to bridging therapy (Poster Abstract #PF767) [Encore of ASCO 2026] Subgroup analysis from the Phase 3 PERSEUS study evaluating the benefit of DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) in transplant-eligible patients with high- and standard-risk multiple myeloma (Poster Abstract #PS1869) [Encore of ASCO 2026] Final subgroup analysis from the Phase 3 CEPHEUS study evaluating DARZALEX FASPRO® in combination with bortezomib, lenalidomide, and dexamethasone in transplant-ineligible newly diagnosed multiple myeloma (Oral Abstract #S196) [Encore of ASCO 2026] Results from the Phase 3 MajesTEC-9 study of TECVAYLI® versus standard of care therapies as early as second line in patients with multiple myeloma (Oral Abstract #S195) [Encore of ASCO 2026]
New research in warm autoimmune hemolytic anemia (wAIHA)Pivotal study assessed hemoglobin response and fatigue improvement compared to placebo in patients with warm autoimmune hemolytic anemia.
Results from the pivotal ENERGY Phase 2/3 study evaluating the efficacy and safety of IMAAVY®in patients with wAIHA compared with placebo (Oral Abstract #S300) Assessment of the effects of IMAAVY®on fatigue in patients with wAIHA, measured using the Functional Assessment of Chronic Illness Therapy-Fatigue (FACIT-Fatigue) scale (Oral Abstract #S325) Confirmatory evidence on the pharmacodynamic effect of IMAAVY®and the correlation with clinical improvement in patients with wAIHA (Poster Abstract #PF1297)
Key data presentations in leukemiaNew and updated data highlight clinical advances in leukemia, including acute myeloid leukemia (AML) and chronic lymphocytic leukemia (CLL), across targeted therapies and fixed-duration treatment approaches.
Safety analyses from the cAMelot-1 and ALE1002 clinical trials of bleximenib (JNJ-75276617), an investigational oral menin inhibitor, evaluating the presence of QTc interval prolongation when given as monotherapy or in combination with AML-directed therapies for KMT2A or NPM1 Altered AML (Poster Abstract #PF555) Primary analysis from the Phase 2 TAILOR study evaluating the safety and efficacy of dose-modified fixed-duration IMBRUVICA®(ibrutinib) plus venetoclax in previously untreated CLL (Poster Abstract #PF606) Real-world analysis from the prospective REALITY-WW study evaluating first-line fixed-duration IMBRUVICA® in combination with venetoclax in patients with CLL (Poster Abstract #PF613)
Information on Johnson & Johnson sponsored abstracts is available on JNJ.com.
Editor’s Notesa. IMAAVY® is not approved by the U.S. FDA for the treatment of wAIHAABOUT MULTIPLE MYELOMA Multiple myeloma is a complex blood cancer that affects a type of white blood cell called plasma cells, which are found in the bone marrow.2 In multiple myeloma, these plasma cells proliferate and spread rapidly and replace normal cells in the bone marrow with tumors.3 Multiple myeloma is the third most common blood cancer worldwide.4 More than 180,000 new cases of multiple myeloma are diagnosed globally each year.5 People living with multiple myeloma have a 5-year survival rate of 59.8 percent.6 While some people diagnosed with multiple myeloma initially have no symptoms, most patients are diagnosed due to symptoms that can include bone fracture or pain, low red blood cell counts, tiredness, high calcium levels and kidney problems or infections.7,8 In recent years, overall survival has improved from years to decades, with effective treatment options now available across every stage and line of therapy.9
ABOUT WARM AUTOIMMUNE HEMOLYTIC ANEMIAWarm autoimmune hemolytic anemia (wAIHA) is a rare, life-threatening condition where autoantibodies attach to and destroy red blood cells (RBCs), resulting in anemia. Approximately 1-3 new people per 100,000 are affected by wAIHA per year, and about 1 in 8,000 individuals are living with the condition.10,11 This condition affects both women and men, and can affect people at any age with incidence increasing over the age of 50.12,13 Additionally, people with wAIHA are at increased risk of other serious complications such as venous thrombotic events, acute renal failure, and infection.14 There are no U.S. FDA-approved drugs indicated for wAIHA, and treatment typically consists of unapproved corticosteroids, broad immunosuppressants, and B-cell directed therapies.11 With an unmet need for treatment in wAIHA, novel therapies like nipocalimab are being developed to potentially address this need.13
ABOUT ACUTE MYELOID LEUKEMIA Acute myeloid leukemia (AML) is an aggressive, fast-growing blood cancer that originates in the bone marrow and is marked by the uncontrolled proliferation of immature white blood cells known as myeloblasts.15,16 These malignant cells crowd out healthy blood-forming cells, leading to complications such as anemia, infections and bleeding.17 Acute myeloid leukemia progresses rapidly, often requiring immediate treatment after diagnosis.16 It is the most common type of acute leukemia in adults, with a median age of diagnosis around 70 years.15 Despite treatment advances, acute myeloid leukemia remains associated with poor patient outcomes, particularly in older adults or those with high-risk genetic profiles.18 The five-year survival rate remains the lowest among leukemias, with outcomes especially poor in patients with KMT2Ar or NPM1m where relapse/refractory disease survival can be as short as 2 to 3 months after a second relapse – highlighting a significant unmet medical need.18
ABOUT TALVEY® TALVEY® (talquetamab-tgvs) received approval from the U.S. FDA in August 2023 as a first-in-class GPRC5D-targeting bispecific antibody for the treatment of adult patients with relapsed or refractory multiple myeloma who have received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 antibody.19 Since U.S. FDA approval, 7,700 patients were treated with TALVEY®. The European Commission (EC) granted conditional marketing authorization (CMA) of TALVEY®(talquetamab-tgvs) in August 2023 as monotherapy for the treatment of adult patients with relapsed and refractory multiple myeloma (RRMM) who have received at least three prior therapies, including an immunomodulatory agent, a proteasome inhibitor, and an anti-CD38 antibody and have demonstrated disease progression on the last therapy.20
TALVEY® is a bispecific T-cell engaging antibody that binds to the CD3 receptor expressed on the surface of T-cells and G protein-coupled receptor class C group 5 member D (GPRC5D), a novel multiple myeloma target which is highly expressed on the surface of multiple myeloma cells and non-malignant plasma cells, as well as some healthy tissues such as epithelial cells of the skin and tongue.
ABOUT DARZALEX FASPRO® AND DARZALEX® DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) received U.S. FDA approval in May 2020 and is approved for 11 indications in multiple myeloma, four of which are for frontline treatment in newly diagnosed patients who are transplant eligible or ineligible.21 It is the only subcutaneous CD38-directed antibody approved to treat patients with multiple myeloma. DARZALEX FASPRO® is co-formulated with recombinant human hyaluronidase PH20 (rHuPH20), Halozyme’s ENHANZE® drug delivery technology.
DARZALEX® (daratumumab) received U.S. FDA approval in November 2015 and is approved in eight indications, three of which are in the frontline setting, including newly diagnosed patients who are transplant-eligible and ineligible.22 In 2025, DARZALEX FASPRO® was approved by the U.S. FDA and EMA as the first and only treatment for patients with high-risk smoldering multiple myeloma.
DARZALEX® is the first CD38-directed antibody approved to treat multiple myeloma.22 DARZALEX®-based regimens have been used in the treatment of more than 748,000 patients worldwide and more than 68,000 patients in the U.S. alone.
In August 2012, Janssen Biotech, Inc. and Genmab A/S entered a worldwide agreement, which granted Janssen an exclusive license to develop, manufacture and commercialize daratumumab. For more information, visit www.DARZALEX.com. ABOUT IMAAVY®IMAAVY® (nipocalimab-aahu) is an immunoselective treatment designed to target, bind with high affinity, and block FcRn, reducing circulating immunoglobulin G (IgG) antibodies that drive disease while also preserving key immune functions. IMAAVY® is currently approved for the treatment of generalized Myasthenia Gravis (gMG) in adults and pediatric patients 12 years of age and older who are anti-acetylcholine receptor (AChR) or anti-muscle-specific tyrosine kinase (MuSK) antibody positive.23
Nipocalimab is being investigated across three key segments in the autoantibody space including Rheumatologic diseases, Rare Autoantibody diseases, and Maternal Fetal diseases mediated by maternal alloantibodies, in which blockade of IgG binding to FcRn in the placenta is believed to limit transplacental transfer of maternal alloantibodies to the fetus.24,25,26,27,28,29,30,31,32,33
The U.S. FDA and European Medicines Agency (EMA) have granted several key designations to nipocalimab including:
EU EMA Orphan medicinal product designation for HDFN in October 2019 and fetal and neonatal alloimmune thrombocytopenia (FNAIT in April 2025 U.S. FDA Fast Track designation in hemolytic disease of the fetus and newborn (HDFN) and warm autoimmune hemolytic anemia (wAIHA) in July 2019, gMG in December 2021, fetal and neonatal alloimmune thrombocytopenia (FNAIT) in March 2024, Sjögren’s disease (SjD) in March 2025, and systemic lupus erythematosus (SLE) in January 2026 U.S. FDA Orphan drug status for wAIHA in December 2019, HDFN in June 2020, gMG in February 2021, chronic inflammatory demyelinating polyneuropathy (CIDP) in October 2021 and FNAIT in December 2023 U.S. FDA Breakthrough Therapy designation for HDFN in February 2024 and for SjD in November 2024 U.S. FDA granted Priority Review in gMG in Q4 2024 and wAIHA in Q2 2026
The legal manufacturer for IMAAVY ® is Janssen Biotech, Inc.
ABOUT TECVAYLI®TECVAYLI® (teclistamab-cqyv) is a first-in-class, bispecific T-cell engager antibody therapy that uses innovative science to activate the immune system by binding to the CD3 receptor expressed on the surface of T-cells and to the B-cell maturation antigen (BCMA) expressed on the surface of multiple myeloma cells and some healthy B-lineage cells.34 TECVAYLI® received accelerated approval from the U.S. FDA in October 2022 as an off-the-shelf (or ready-to-use) antibody that is administered as a subcutaneous treatment for adult patients with relapsed or refractory multiple myeloma (RRMM) who received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 antibody.
In February 2024, the U.S. FDA approved the supplemental Biologics License Application (sBLA) for TECVAYLI® for a reduced dosing frequency of 1.5 mg/kg every two weeks in patients with RRMM who achieved and maintained a complete response (CR) or better for a minimum of six months.
In March 2026, the U.S. FDA approved TECVAYLI® in combination with DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) for the treatment of adult patients with relapsed or refractory multiple myeloma who have received at least one prior line of therapy, including a proteasome inhibitor and an immunomodulatory agent. The supplemental Biologics License Application was proactively selected for the Commissioner’s National Priority Voucher Pilot Program and also granted the application Breakthrough Therapy Designation and Real-Time Oncology Review. This approval expanded the use of TECVAYLI® into earlier lines of therapy and is the first bispecific antibody-based combination regimen in this setting, offering a potential new standard of care as early as second line.
To date, more than 26,000 patients have been treated worldwide with TECVAYLI®.
The European Commission (EC) granted TECVAYLI® conditional marketing authorization in August 2022 as monotherapy for the treatment of adult patients with RRMM who have received at least three prior therapies, including a proteasome inhibitor, an immunomodulatory agent and an anti-CD38 antibody, and have demonstrated disease progression since the last therapy. In August 2023, the EC approved a Type II variation application for TECVAYLI®, providing the option for a reduced dosing frequency of 1.5 mg/kg every two weeks (Q2W) in patients who have achieved a complete response or better for a minimum of six months.
For more information, visit www.TECVAYLI.com.
ABOUT CARVYKTI® CARVYKTI® (cilta-cel) received U.S. Food and Drug Administration approval in February 2022 for the treatment of adults with relapsed or refractory multiple myeloma after four or more prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 monoclonal antibody.35
In April 2024, CARVYKTI® was approved in the U.S. for treatment of adult patients with relapsed or refractory multiple myeloma who have received at least one prior line of therapy including a proteasome inhibitor, an immunomodulatory agent, and who are refractory to lenalidomide, following a unanimous (11 to 0) U.S. FDA Oncologic Drugs Advisory Committee (ODAC) recommendation in support of this new indication. In April 2024, the European Medicines Agency (EMA) approved a Type II variation for CARVYKTI® for the treatment of adults with relapsed and refractory multiple myeloma who have received at least one prior therapy, including an immunomodulatory agent and a proteasome inhibitor, have demonstrated disease progression on the last therapy, and are refractory to lenalidomide. In September 2022, Japan’s Ministry of Health, Labour and Welfare (MHLW) approved CARVYKTI® for the treatment of adults with relapsed or refractory multiple myeloma in patients that have no history of CAR-positive T cell infusion therapy targeting BCMA and who have received three or more lines of therapies, including an immunomodulatory agent, a proteasome inhibitor and an anti-CD38 monoclonal antibody, and in whom multiple myeloma has not responded to or has relapsed following the most recent therapy.
CARVYKTI® is a BCMA-directed, autologous T-cell immunotherapy, which involves reprogramming a patient’s own T-cells with a transgene encoding chimeric antigen receptor (CAR) that directs the CAR-positive T cells to eliminate cells that express BCMA. BCMA is primarily expressed on the surface of malignant multiple myeloma B-lineage cells, as well as late-stage B cells and plasma cells. The CARVYKTI® CAR protein features two BCMA-targeting single domains designed to confer high avidity against human BCMA. Upon binding to BCMA-expressing cells, the CAR promotes T-cell activation, expansion, and elimination of target cells. CARVYKTI® is available in 17 markets worldwide and has been used to treat more than 11,000 patients globally.
In December 2017, Janssen Biotech, Inc., a Johnson & Johnson company, entered into an exclusive worldwide license and collaboration agreement with Legend Biotech USA, Inc. to develop and commercialize CARVYKTI®. For more information, visit www.CARVYKTI.com.
ABOUT IMBRUVICA®IMBRUVICA® (ibrutinib) is a once-daily oral medication that is jointly developed and commercialized by Janssen Biotech, Inc., and Pharmacyclics LLC, an AbbVie company. IMBRUVICA® blocks the BTK protein, which is needed by normal and abnormal B cells, including specific cancer cells, to multiply and spread. By blocking BTK, IMBRUVICA® may help move abnormal B cells out of their nourishing environments and inhibit their proliferation.36,37,38
IMBRUVICA® has been used to treat more than 325,000 patients worldwide over the last decade. There are more 70 company-sponsored clinical trials, including 18 Phase 3 studies, spanning more than 13 years evaluating the efficacy and safety of IMBRUVICA®.
IMBRUVICA® was first approved by the U.S. FDA in November 2013, and today is indicated for adult patients in four disease areas. To date, IMBRUVICA® has been approved in more than 100 countries/territories for one or more of the following indications: the treatment of adult patients with chronic lymphocytic leukemia (CLL)/small lymphocytic lymphoma (SLL) with or without 17p deletion (del17p); adults with Waldenström’s macroglobulinemia (WM); adults with mantle cell lymphoma (MCL); adults with marginal zone lymphoma (MZL) who require systemic therapy and have received at least one prior anti-CD20-based therapy; and adult and pediatric patients aged one year and older with previously treated chronic graft versus host disease (cGVHD) after failure of one or more lines of systemic therapy.39
TALVEY® IMPORTANT SAFETY INFORMATION
INDICATION AND USAGE
TALVEY® (talquetamab-tgvs) is indicated for the treatment of adult patients with relapsed or refractory multiple myeloma who have received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 monoclonal antibody.
This indication is approved under accelerated approval based on response rate and durability of response. Continued approval for this indication may be contingent upon verification and description of clinical benefit in a confirmatory trial(s).
IMPORTANT SAFETY INFORMATION
WARNING: CYTOKINE RELEASE SYNDROME and NEUROLOGIC TOXICITY, including IMMUNE EFFECTOR CELL-ASSOCIATED NEUROTOXICITY SYNDROME
Cytokine release syndrome (CRS), including life-threatening or fatal reactions, can occur in patients receiving TALVEY®. Initiate TALVEY® treatment with step-up dosing to reduce the risk of CRS. Withhold TALVEY® until CRS resolves or permanently discontinue based on severity.
Neurologic toxicity, including immune effector cell-associated neurotoxicity syndrome (ICANS), and serious and life-threatening or fatal reactions, can occur with TALVEY®. Monitor patients for signs and symptoms of neurologic toxicity including ICANS during treatment and treat promptly. Withhold or permanently discontinue TALVEY® based on severity.
Because of the risk of CRS and neurologic toxicity, including ICANS, TALVEY® is available only through a restricted program called the TECVAYLI® and TALVEY® Risk Evaluation and Mitigation Strategy (REMS).
CONTRAINDICATIONS: None.
WARNINGS AND PRECAUTIONS Cytokine Release Syndrome (CRS): TALVEY® can cause cytokine release syndrome, including life-threatening or fatal reactions. In the clinical trial, CRS occurred in 76% of patients who received TALVEY® at the recommended dosages, with Grade 1 CRS occurring in 57% of patients, Grade 2 in 17%, and Grade 3 in 1.5%. Recurrent CRS occurred in 30% of patients. Most events occurred following step-up dose 1 (29%) or step-up dose 2(44%) at the recommended dosages. CRS occurred in 33% of patients with step-up dose 3 in the biweekly dosing schedule (N=153). CRS occurred in 30% of patients with the first 0.4 mg/kg treatment dose and in 12% of patients treated with the first 0.8 mg/kg treatment dose. The CRS rate for both dosing schedules combined was less than 3% for each of the remaining doses in Cycle 1 and less than 3% cumulatively from Cycle 2 onward. The median time to onset of CRS was 27 (range: 0.1 to 167) hours from the last dose, and the median duration was 17 (range: 0 to 622) hours. Clinical signs and symptoms of CRS include but are not limited to pyrexia, hypotension, chills, hypoxia, headache, and tachycardia. Potentially life-threatening complications of CRS may include cardiac dysfunction, acute respiratory distress syndrome, neurologic toxicity, renal and/or hepatic failure, and disseminated intravascular coagulation (DIC). Initiate therapy with step-up dosing and administer pre-treatment medications (corticosteroids, antihistamine, and antipyretics) prior to each dose of TALVEY® in the step-up dosing schedule to reduce the risk of CRS. Monitor patients following administration accordingly. In patients who experience CRS, pre-treatment medications should be administered prior to the next TALVEY® dose.
Counsel patients to seek medical attention should signs or symptoms of CRS occur. At the first sign of CRS, immediately evaluate patient for hospitalization and institute treatment with supportive care based on severity, and consider further management per current practice guidelines. Withhold TALVEY® until CRS resolves or permanently discontinue based on severity.
Neurologic Toxicity including ICANS: TALVEY® can cause serious, or life-threatening neurologic toxicity or fatal neurologic toxicity including immune effector cell-associated neurotoxicity syndrome (ICANS), including fatal reactions. In the clinical trial, neurologic toxicity, including ICANS, occurred in 55% of patients who received the recommended dosages, with Grade 3 or 4 neurologic toxicity occurring in 6% of patients. The most frequent neurologic toxicities were headache (20%), encephalopathy (15%), sensory neuropathy (14%), and motor dysfunction (10%).
ICANS was reported in 9% of 265 patients where ICANS was collected and who received the recommended dosages. Recurrent ICANS occurred in 3% of patients. Most patients experienced ICANS following step-up dose 1 (3%), step-up dose 2 (3%), step-up dose 3 of the biweekly dosing schedule (1.8%), or the initial treatment dose of the weekly dosing schedule (2.6%) (N=156) or the biweekly dosing schedule (3.7%) (N=109). The median time to onset of ICANS was 2.5 (range: 1 to 16) days after the most recent dose with a median duration of 2 (range: 1 to 22) days. The onset of ICANS can be concurrent with CRS, following resolution of CRS, or in the absence of CRS. Clinical signs and symptoms of ICANS may include but are not limited to confusional state, depressed level of consciousness, disorientation, somnolence, lethargy, and bradyphrenia.
Monitor patients for signs and symptoms of neurologic toxicity during treatment and treat promptly. At the first sign of neurologic toxicity, including ICANS, immediately evaluate the patient and provide supportive care based on severity. Withhold or permanently discontinue TALVEY® based on severity and consider further management per current practice guidelines [see Dosage and Administration (2.5)].
Due to the potential for neurologic toxicity, patients receiving TALVEY® are at risk of depressed level of consciousness. Advise patients to refrain from driving or operating heavy or potentially dangerous machinery during the step-up dosing schedule and for 48 hours after completion of the step-up dosing schedule, and in the event of new onset of any neurological symptoms, until symptoms resolve.
TECVAYLI® and TALVEY® REMS: TALVEY® is available only through a restricted program under a REMS, called the TECVAYLI® and TALVEY® REMS because of the risks of CRS and neurologic toxicity, including ICANS. Further information about the TECVAYLI® and TALVEY® REMS program is available at www.TEC-TALREMS.com or by telephone at 1-855-810-8064.
Oral Toxicity and Weight Loss: TALVEY® can cause oral toxicities, including dysgeusia, dry mouth, dysphagia, and stomatitis. In the clinical trial, 80% of patients had oral toxicity, with Grade 3 occurring in 2.1% of patients who received the recommended dosages. The most frequent oral toxicities were dysgeusia (49%), dry mouth (34%), dysphagia (23%), and ageusia (18%). The median time to onset of oral toxicity was 15 (range: 1 to 634) days, and the median time to resolution to baseline was 43 (1 to 530) days. Oral toxicity did not resolve to baseline in 65% of patients.
TALVEY® can cause weight loss. In the clinical trial, 62% of patients experienced weight loss, regardless of having an oral toxicity, including 29% of patients with Grade 2 (10% or greater) weight loss and 2.7% of patients with Grade 3 (20% or greater) weight loss. The median time to onset of Grade 2 or higher weight loss was 67 (range: 6 to 407) days, and the median time to resolution was 50 (range: 1 to 403) days. Weight loss did not resolve in 57% of patients who reported weight loss.
Monitor patients for signs and symptoms of oral toxicity. Counsel patients to seek medical attention should signs or symptoms of oral toxicity occur and provide supportive care as per current clinical practice, including consultation with a nutritionist. Monitor weight regularly during therapy. Evaluate clinically significant weight loss further. Withhold TALVEY® or permanently discontinue based on severity.
Infections: TALVEY® can cause infections, including life-threatening or fatal infections. Serious infections occurred in 16% of patients, with fatal infections in 1.5% of patients. Grade 3 or 4 infections occurred in 17% of patients. The most common serious infections reported were bacterial infection (8%), which included sepsis and COVID-19 (2.7%). Monitor patients for signs and symptoms of infection prior to and during treatment with TALVEY® and treat appropriately. Administer prophylactic antimicrobials according to local guidelines. Withhold or consider permanent discontinuation of TALVEY® as recommended, based on severity.
Cytopenias: TALVEY® can cause cytopenias, including neutropenia and thrombocytopenia. In the clinical trial, Grade 3 or 4 decreased neutrophils occurred in 35% of patients, and Grade 3 or 4 decreased platelets occurred in 22% of patients who received TALVEY®. The median time to onset for Grade 3 or 4 neutropenia was 22 (range: 1 to 312) days, and the median time to resolution to Grade 2 or lower was 8 (range: 1 to 79) days. The median time to onset for Grade 3 or 4 thrombocytopenia was 12 (range: 2 to 183) days, and the median time to resolution to Grade 2 or lower was 10 (range: 1 to 64) days. Monitor complete blood counts during treatment and withhold TALVEY® as recommended, based on severity.
Skin Toxicity: TALVEY® can cause serious skin reactions, including rash, maculo-papular rash, erythema, and erythematous rash. In the clinical trial, skin reactions occurred in 62% of patients, with Grade 3 skin reactions in 0.3%. The median time to onset was 25 (range: 1 to 630) days. The median time to improvement to Grade 1 or less was 33 days.
Monitor for skin toxicity, including rash progression. Consider early intervention and treatment to manage skin toxicity. Withhold TALVEY® as recommended based on severity.
Hepatotoxicity: TALVEY® can cause hepatotoxicity. Elevated ALT occurred in 33% of patients, with Grade 3 or 4 ALT elevation occurring in 2.7%; elevated AST occurred in 31% of patients, with Grade 3 or 4 AST elevation occurring in 3.3%. Grade 3 or 4 elevations of total bilirubin occurred in 0.3% of patients. Liver enzyme elevation can occur with or without concurrent CRS.
Monitor liver enzymes and bilirubin at baseline and during treatment as clinically indicated. Withhold TALVEY® or consider permanent discontinuation of TALVEY®, based on severity [see Dosage and Administration (2.5)].
Embryo-Fetal Toxicity: Based on its mechanism of action, TALVEY® may cause fetal harm when administered to a pregnant woman. Advise pregnant women of the potential risk to the fetus. Advise females of reproductive potential to use effective contraception during treatment with TALVEY® and for 3 months after the last dose.
Adverse Reactions: The most common adverse reactions (≥20%) are pyrexia, CRS, dysgeusia, nail disorder, musculoskeletal pain, skin disorder, rash, fatigue, weight decreased, dry mouth, xerosis, dysphagia, upper respiratory tract infection, diarrhea, hypotension, and headache.
The most common Grade 3 or 4 laboratory abnormalities (≥30%) are lymphocyte count decreased, neutrophil count decreased, white blood cell decreased, and hemoglobin decreased.
Please read full Prescribing Information, including Boxed WARNING, for TALVEY®.
DARZALEX FASPRO® INDICATIONS AND IMPORTANT SAFETY INFORMATION INDICATIONS DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) is indicated for the treatment of adult patients with multiple myeloma: · In combination with bortezomib, lenalidomide, and dexamethasone for induction and consolidation in newly diagnosed patients who are eligible for autologous stem cell transplant · In combination with bortezomib, melphalan, and prednisone in newly diagnosed patients who are ineligible for autologous stem cell transplant · In combination with lenalidomide and dexamethasone in newly diagnosed patients who are ineligible for autologous stem cell transplant and in patients with relapsed or refractory multiple myeloma who have received at least one prior therapy · In combination with bortezomib, thalidomide, and dexamethasone in newly diagnosed patients who are eligible for autologous stem cell transplant · In combination with pomalidomide and dexamethasone in patients who have received at least one prior line of therapy including lenalidomide and a proteasome inhibitor (PI) · In combination with carfilzomib and dexamethasone in patients with relapsed or refractory multiple myeloma who have received one to three prior lines of therapy · In combination with bortezomib and dexamethasone in patients who have received at least one prior therapy · As monotherapy in patients who have received at least three prior lines of therapy including a PI and an immunomodulatory agent or who are double refractory to a PI and an immunomodulatory agent
DARZALEX FASPRO® as monotherapy is indicated for the treatment of adult patients with high-risk smoldering multiple myeloma.
IMPORTANT SAFETY INFORMATION
CONTRAINDICATIONS DARZALEX FASPRO® is contraindicated in patients with a history of severe hypersensitivity to daratumumab, hyaluronidase, or any of the components of the formulation.
WARNINGS AND PRECAUTIONS
Hypersensitivity and Other Administration Reactions Both systemic administration-related reactions, including severe or life-threatening reactions, and local injection-site reactions can occur with DARZALEX FASPRO®. Fatal reactions have been reported with daratumumab-containing products, including DARZALEX FASPRO®.
Systemic Reactions
In a pooled safety population of 1446 patients with multiple myeloma (N=1235) or light chain (AL) amyloidosis (N=193) who received DARZALEX FASPRO® as monotherapy or in combination, 7% of patients experienced a systemic administration-related reaction (Grade 2: 3%, Grade 3: 0.8%, Grade 4: 0.1%). In patients with high-risk smoldering multiple myeloma (N=193), systemic administration-related reactions occurred in 17% of patients in AQUILA (Grade 2: 7%, Grade 3: 1%).
In all patients (N=1639), systemic administration-related reactions occurred in 7% of patients with the first injection, 0.5% with the second injection, and cumulatively 1% with subsequent injections. The median time to onset was 3.2 hours (range: 4 minutes to 3.5 days). Of the 283 systemic administration-related reactions that occurred in 135 patients, 240 (85%) occurred on the day of DARZALEX FASPRO® administration. Delayed systemic administration-related reactions have occurred in 1% of the patients.
Severe reactions included hypoxia, dyspnea, hypertension, tachycardia, and ocular adverse reactions, including choroidal effusion, acute myopia, and acute angle closure glaucoma. Other signs and symptoms of systemic administration-related reactions may include respiratory symptoms, such as bronchospasm, nasal congestion, cough, throat irritation, allergic rhinitis, and wheezing, as well as anaphylactic reaction, pyrexia, chest pain, pruritus, chills, vomiting, nausea, hypotension, and blurred vision. Pre-medicate patients with histamine-1 receptor antagonist, acetaminophen, and corticosteroids. Monitor patients for systemic administration-related reactions, especially following the first and second injections. For anaphylactic reaction or life-threatening (Grade 4) administration-related reactions, immediately and permanently discontinue DARZALEX FASPRO®. Consider administering corticosteroids and other medications after the administration of DARZALEX FASPRO® depending on dosing regimen and medical history to minimize the risk of delayed (defined as occurring the day after administration) systemic administration-related reactions.
Ocular adverse reactions, including acute myopia and narrowing of the anterior chamber angle due to ciliochoroidal effusions with potential for increased intraocular pressure or glaucoma, have occurred with daratumumab-containing products. If ocular symptoms occur, interrupt DARZALEX FASPRO® and seek immediate ophthalmologic evaluation prior to restarting DARZALEX FASPRO®.
Local Reactions
In this pooled safety population of 1446 patients with multiple myeloma (N=1253) or light chain amyloidosis (N=193), injection-site reactions occurred in 8% of patients, including Grade 2 reactions in 1.1%. The most frequent (>1%) injection-site reaction were injection site erythema and injection site rash. In patients with high-risk smoldering multiple myeloma (N=193), injection-site reactions occurred in 28% of patients, including Grade 2 reactions in 3%. These local reactions occurred a median of 6 minutes (range: 0 minutes to 6.5 days) after starting administration of DARZALEX FASPRO®. Monitor for local reactions and consider symptomatic management.
Infections DARZALEX FASPRO® can cause serious, life-threatening, or fatal infections. In patients who received DARZALEX FASPRO® in a pooled safety population including patients with smoldering multiple myeloma and light chain (AL) amyloidosis (N=1639), serious infections, including opportunistic infections, occurred in 24% of patients, Grade 3 or 4 infections occurred in 22%, and fatal infections occurred in 2.5%. The most common type of serious infection reported was pneumonia (8.5%).
Monitor patients for signs and symptoms of infection prior to and during treatment with DARZALEX FASPRO® and treat appropriately. Administer prophylactic antimicrobials according to guidelines.
Neutropenia Daratumumab may increase neutropenia induced by background therapy. Monitor complete blood cell counts periodically during treatment according to manufacturer’s prescribing information for background therapies. Monitor patients with neutropenia for signs of infection. Consider withholding DARZALEX FASPRO® until recovery of neutrophils. In lower body weight patients receiving DARZALEX FASPRO®, higher rates of Grade 3-4 neutropenia were observed.
Thrombocytopenia Daratumumab may increase thrombocytopenia induced by background therapy. Monitor complete blood cell counts periodically during treatment according to manufacturer’s prescribing information for background therapies. Consider withholding DARZALEX FASPRO® until recovery of platelets.
Embryo-Fetal Toxicity Based on the mechanism of action, DARZALEX FASPRO® can cause fetal harm when administered to a pregnant woman. DARZALEX FASPRO® may cause depletion of fetal immune cells and decreased bone density. Advise pregnant women of the potential risk to a fetus. Advise females with reproductive potential to use effective contraception during treatment with DARZALEX FASPRO® and for 3 months after the last dose.
The combination of DARZALEX FASPRO® with lenalidomide, thalidomide, or pomalidomide is contraindicated in pregnant women because lenalidomide, thalidomide, and pomalidomide may cause birth defects and death of the unborn child. Refer to the lenalidomide, thalidomide, or pomalidomide prescribing information on use during pregnancy.
Interference With Serological Testing Daratumumab binds to CD38 on red blood cells (RBCs) and results in a positive indirect antiglobulin test (indirect Coombs test). Daratumumab-mediated positive indirect antiglobulin test may persist for up to 6 months after the last daratumumab administration. Daratumumab bound to RBCs masks detection of antibodies to minor antigens in the patient’s serum. The determination of a patient’s ABO and Rh blood type are not impacted.
Notify blood transfusion centers of this interference with serological testing and inform blood banks that a patient has received DARZALEX FASPRO®. Type and screen patients prior to starting DARZALEX FASPRO®.
Interference With Determination of Complete Response Daratumumab is a human immunoglobulin G (IgG) kappa monoclonal antibody that can be detected on both the serum protein electrophoresis (SPE) and immunofixation (IFE) assays used for the clinical monitoring of endogenous M-protein. This interference can impact the determination of complete response and of disease progression in some DARZALEX FASPRO®-treated patients with IgG kappa myeloma protein.
ADVERSE REACTIONS
In multiple myeloma, the most common adverse reaction (≥20%) with DARZALEX FASPRO® monotherapy is upper respiratory tract infection. The most common adverse reactions with combination therapy (≥20% for any combination) include fatigue, nausea, diarrhea, dyspnea, insomnia, headache, rash, pyrexia, cough, muscle spasms, back pain, vomiting, hypertension, musculoskeletal pain, upper respiratory tract infection, , peripheral neuropathy, peripheral sensory neuropathy, constipation, pneumonia, edema, peripheral edema, and anemia.
The most common adverse reactions (≥20%) in patients with high-risk smoldering multiple myeloma who received DARZALEX FASPRO® monotherapy are upper respiratory tract infection, musculoskeletal pain, fatigue, diarrhea, rash, sleep disorder, sensory neuropathy, and injection site reactions.
The most common hematology laboratory abnormalities (≥40%) with DARZALEX FASPRO® are decreased leukocytes, decreased lymphocytes, decreased neutrophils, decreased platelets, and decreased hemoglobin.
Please click here to read the full Prescribing Information for DARZALEX FASPRO®.
DARZALEX® INDICATIONS AND IMPORTANT SAFETY INFORMATION INDICATIONS DARZALEX® (daratumumab) is indicated for the treatment of adult patients with multiple myeloma: · In combination with bortezomib, melphalan, and prednisone in newly diagnosed patients who are ineligible for autologous stem cell transplant · In combination with lenalidomide and dexamethasone in newly diagnosed patients who are ineligible for autologous stem cell transplant and in patients with relapsed or refractory multiple myeloma who have received at least one prior therapy · In combination with bortezomib, thalidomide, and dexamethasone in newly diagnosed patients who are eligible for autologous stem cell transplant · In combination with pomalidomide and dexamethasone in patients who have received at least one prior line of therapy including lenalidomide and a proteasome inhibitor · In combination with carfilzomib and dexamethasone in patients with relapsed or refractory multiple myeloma who have received one to three prior lines of therapy · In combination with bortezomib and dexamethasone in patients who have received at least one prior therapy · As monotherapy in patients who have received at least three prior lines of therapy including a proteasome inhibitor (PI) and an immunomodulatory agent or who are double-refractory to a PI and an immunomodulatory agent
CONTRAINDICATIONS DARZALEX® is contraindicated in patients with a history of severe hypersensitivity (eg, anaphylactic reactions) to daratumumab or any of the components of the formulation.
WARNINGS AND PRECAUTIONS
Infusion-Related Reactions DARZALEX® can cause severe and/or serious infusion-related reactions including anaphylactic reactions. These reactions can be life threatening, and fatal outcomes have been reported. In clinical trials (monotherapy and combination: N=2066), infusion-related reactions occurred in 37% of patients with the Week 1 (16 mg/kg) infusion, 2% with the Week 2 infusion, and cumulatively 6% with subsequent infusions. Less than 1% of patients had a Grade 3/4 infusion-related reaction at Week 2 or subsequent infusions. The median time to onset was 1.5 hours (range: 0 to 73 hours). Nearly all reactions occurred during infusion or within 4 hours of completing DARZALEX®. Severe reactions have occurred, including bronchospasm, hypoxia, dyspnea, hypertension, tachycardia, headache, laryngeal edema, pulmonary edema, and ocular adverse reactions, including choroidal effusion, acute myopia, and acute angle closure glaucoma. Signs and symptoms may include respiratory symptoms, such as nasal congestion, cough, throat irritation, as well as chills, vomiting, and nausea. Less common signs and symptoms were wheezing, allergic rhinitis, pyrexia, chest discomfort, pruritus, hypotension and blurred vision.
When DARZALEX® dosing was interrupted in the setting of ASCT (CASSIOPEIA) for a median of 3.75 months (range: 2.4 to 6.9 months), upon re-initiation of DARZALEX®, the incidence of infusion-related reactions was 11% for the first infusion following ASCT. Infusion-related reactions occurring at re-initiation of DARZALEX® following ASCT were consistent in terms of symptoms and severity (Grade 3 or 4: <1%) with those reported in previous studies at Week 2 or subsequent infusions. In EQUULEUS, patients receiving combination treatment (n=97) were administered the first 16 mg/kg dose at Week 1 split over two days, ie, 8 mg/kg on Day 1 and Day 2, respectively. The incidence of any grade infusion-related reactions was 42%, with 36% of patients experiencing infusion-related reactions on Day 1 of Week 1, 4% on Day 2 of Week 1, and 8% with subsequent infusions.
Pre-medicate patients with antihistamines, antipyretics, and corticosteroids. Frequently monitor patients during the entire infusion. Interrupt DARZALEX® infusion for reactions of any severity and institute medical management as needed. Permanently discontinue DARZALEX® therapy if an anaphylactic reaction or life-threatening (Grade 4) reaction occurs and institute appropriate emergency care. For patients with Grade 1, 2, or 3 reactions, reduce the infusion rate when re-starting the infusion.
To reduce the risk of delayed infusion-related reactions, administer oral corticosteroids to all patients following DARZALEX® infusions. Patients with a history of chronic obstructive pulmonary disease may require additional post-infusion medications to manage respiratory complications. Consider prescribing short- and long-acting bronchodilators and inhaled corticosteroids for patients with chronic obstructive pulmonary disease.
Ocular adverse reactions, including acute myopia and narrowing of the anterior chamber angle due to ciliochoroidal effusions with potential for increased intraocular pressure or glaucoma, have occurred with DARZALEX® infusion. If ocular symptoms occur, interrupt DARZALEX® infusion and seek immediate ophthalmologic evaluation prior to restarting DARZALEX®.
Interference With Serological Testing
Daratumumab binds to CD38 on red blood cells (RBCs) and results in a positive indirect antiglobulin test (indirect Coombs test). Daratumumab-mediated positive indirect antiglobulin test may persist for up to 6 months after the last daratumumab infusion. Daratumumab bound to RBCs masks detection of antibodies to minor antigens in the patient’s serum. The determination of a patient’s ABO and Rh blood type is not impacted. Notify blood transfusion centers of this interference with serological testing and inform blood banks that a patient has received DARZALEX®. Type and screen patients prior to starting DARZALEX®.
Neutropenia and Thrombocytopenia
DARZALEX® may increase neutropenia and thrombocytopenia induced by background therapy. Monitor complete blood cell counts periodically during treatment according to manufacturer’s prescribing information for background therapies. Monitor patients with neutropenia for signs of infection. Consider withholding DARZALEX® until recovery of neutrophils or for recovery of platelets.
Interference With Determination of Complete Response
Daratumumab is a human immunoglobulin G (IgG) kappa monoclonal antibody that can be detected on both the serum protein electrophoresis (SPE) and immunofixation (IFE) assays used for the clinical monitoring of endogenous M-protein. This interference can impact the determination of complete response and of disease progression in some patients with IgG kappa myeloma protein.
Embryo-Fetal Toxicity
Based on the mechanism of action, DARZALEX® can cause fetal harm when administered to a pregnant woman. DARZALEX® may cause depletion of fetal immune cells and decreased bone density. Advise pregnant women of the potential risk to a fetus. Advise females with reproductive potential to use effective contraception during treatment with DARZALEX® and for 3 months after the last dose
The combination of DARZALEX® with lenalidomide, pomalidomide, or thalidomide is contraindicated in pregnant women because lenalidomide, pomalidomide, and thalidomide may cause birth defects and death of the unborn child. Refer to the lenalidomide, pomalidomide, or thalidomide prescribing information on use during pregnancy.
ADVERSE REACTIONS The most frequently reported adverse reactions (incidence ≥20%) were: upper respiratory infection, neutropenia, infusion related reactions, thrombocytopenia, diarrhea, constipation, anemia, peripheral sensory neuropathy, fatigue, peripheral edema, nausea, cough, pyrexia, dyspnea, and asthenia. The most common hematologic laboratory abnormalities (≥40%) with DARZALEX® are: neutropenia, lymphopenia, thrombocytopenia, leukopenia, and anemia.
Please click here to read the full Prescribing Information for DARZALEX®.
WHAT IS IMAAVY® (nipocalimab-aahu)?
IMAAVY® is a prescription medicine used to treat adults and children 12 years of age and older with a disease called generalized myasthenia gravis (gMG) who are anti-acetylcholine receptor (AChR) or anti-muscle-specific tyrosine kinase (MuSK) antibody positive.
It is not known if IMAAVY® is safe and effective in children under 12 years of age.
IMPORTANT SAFETY INFORMATION
What is the most important information I should know about IMAAVY®?
IMAAVY® is a prescription medicine that may cause serious side effects, including:· Infections are a common side effect of IMAAVY® that can be serious. Receiving IMAAVY® may increase your risk of infection. Tell your healthcare provider right away if you have any of the following infection symptoms:
· Allergic (hypersensitivity) reactions may happen during or up to a few weeks after your IMAAVY® infusion. Get emergency medical help right away if you get any of these symptoms during or after your IMAAVY® infusion:
· Infusion-related reactions are possible. Tell your healthcare provider right away if you get any of these symptoms during or a few days after your IMAAVY® infusion:
Do not receive IMAAVY® if you have a severe allergic reaction to nipocalimab-aahu or any of the ingredients in IMAAVY®. Reactions have included angioedema and anaphylaxis.
Before using IMAAVY®, tell your healthcare provider about all of your medical conditions, including if you:
· ever had an allergic reaction to IMAAVY®.· have or had any recent infections or symptoms of infection.· have recently received or are scheduled to receive an immunization (vaccine). People who take IMAAVY® should not receive live vaccines.· are pregnant, plan to become pregnant, or are breastfeeding. It is not known whether IMAAVY® will harm your baby.Pregnancy Safety Study. There is a pregnancy safety study for IMAAVY® if IMAAVY® is given during pregnancy or you become pregnant while receiving IMAAVY®. Your healthcare provider should report IMAAVY exposure by contacting Janssen at 1-800-526-7736 or www.IMAAVY®.com.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
What are the possible side effects of IMAAVY ®?IMAAVY® may cause serious side effects. See “What is the most important information I should know about IMAAVY®?”
The most common side effects of IMAAVY® include: respiratory tract infection, peripheral edema (swelling in your hands, ankles, or feet), and muscle spasms.
These are not all the possible side effects of IMAAVY®. Call your doctor for medical advice about side effects. You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch, or call 1-800-FDA-1088.
Please see the full Prescribing Information and Medication Guide for IMAAVY® and discuss any questions you have with your doctor.
Dosage Form and Strengths: IMAAVY® is supplied as a 300 mg/1.62 mL and a 1,200 mg/6.5 mL (185 mg/mL) single-dose vial per carton for intravenous injection.
TECVAYLI® IMPORTANT SAFETY INFORMATION
INDICATION AND USAGE
TECVAYLI® (teclistamab-cqyv) is a bispecific B-cell maturation antigen (BCMA)-directed CD3 T-cell engager indicated for the treatment of adult patients with relapsed or refractory multiple myeloma:
· in combination with daratumumab and hyaluronidase-fihj in patients who have received at least one prior line of therapy, including a proteasome inhibitor and an immunomodulatory agent.· as monotherapy, in patients who have received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent and an anti-CD38 monoclonal antibody.
IMPORTANT SAFETY INFORMATION
WARNING: CYTOKINE RELEASE SYNDROME and NEUROLOGIC TOXICITY including IMMUNE EFFECTOR CELL-ASSOCIATED NEUROTOXICITY SYNDROME
Cytokine release syndrome (CRS), including life-threatening or fatal reactions, can occur in patients receiving TECVAYLI. Initiate treatment with TECVAYLI step-up dosing schedule to reduce risk of CRS. Withhold TECVAYLI until CRS resolves or permanently discontinue based on severity.
Neurologic toxicity, including Immune Effector Cell-Associated Neurotoxicity Syndrome (ICANS) and serious, life-threatening, or fatal reactions, can occur in patients receiving TECVAYLI. Monitor patients for signs or symptoms of neurologic toxicity, including ICANS, during treatment. Withhold TECVAYLI until neurologic toxicity resolves or permanently discontinue based on severity.
TECVAYLI is available only through a restricted program called the TECVAYLI and TALVEY® Risk Evaluation and Mitigation Strategy (REMS).
WARNINGS AND PRECAUTIONS
Cytokine Release Syndrome - TECVAYLIcan cause cytokine release syndrome (CRS), including life-threatening or fatal reactions.
In the clinical trials (monotherapy and combination therapy; N=448), CRS occurred in 64% of patients who received TECVAYLI at the recommended dose, with Grade 1 CRS occurring in 46% of patients, Grade 2 in 18%, and Grade 3 in 0.2%. Recurrent CRS occurred in 27% of patients. Most patients experienced CRS during the initial step-up dosing schedule (step-up dose 1 [37%], step-up dose 2 [32%], or the initial treatment dose [20%]). CRS first occurred following subsequent doses of TECVAYLI in 2.5% of patients. The median time to onset of CRS was 2 (range: 1 to 9) days after the most recent dose and the median duration of CRS was 2 (range: 1 to 22) days.
Clinical signs and symptoms of CRS included, but were not limited to, fever, hypoxia, chills, hypotension, sinus tachycardia, headache, and elevated liver enzymes (aspartate aminotransferase and alanine aminotransferase elevation).
Initiate therapy according to TECVAYLI step-up dosing schedule to reduce risk of CRS. Administer pretreatment medications to reduce risk of CRS and monitor patients following administration of TECVAYLI accordingly.
At the first sign of CRS, immediately evaluate patient for hospitalization. Administer supportive care based on severity and consider further management per current practice guidelines. Withhold until CRS resolves or permanently discontinue TECVAYLI based on severity.
TECVAYLI is available only through a restricted program under a REMS.
Neurologic Toxicity including Immune Effector Cell-Associated Neurotoxicity Syndrome - TECVAYLI can cause serious, life-threatening, or fatal neurologic toxicity, including immune effector cell-associated neurotoxicity syndrome (ICANS).
In the clinical trials (monotherapy and combination therapy trials; N=448), neurologic toxicity occurred in 60% of patients who received TECVAYLI at the recommended dosage, with Grade 3 or 4 neurologic toxicity in 6%. Neurologic toxicities reported in ≥5% of patients included headache (27%), sensory neuropathy (16%), motor dysfunction (15%), insomnia (12%), encephalopathy (11%), and dizziness (8%). Fatal neurologic toxicity occurred in 0.4% of patients, including Guillain-Barré syndrome and status epilepticus (one patient each).
In MajesTEC-1, ICANS was reported in 6% of patients who received TECVAYLI as monotherapy at the recommended dosage. Recurrent ICANS occurred in 1.8% of patients. Most patients experienced ICANS following step-up dose 1 (1.2%), step-up dose 2 (0.6%), or the initial treatment dose (1.8%). Less than 3% of patients developed first occurrence of ICANS following subsequent TECVAYLI doses. The median time to onset of ICANS was 4 (range: 2 to 8) days after the most recent dose with a median duration of 3 (range: 1 to 20) days. The most frequent clinical manifestations of ICANS reported were confusional state and dysgraphia.
In MajesTEC-3, ICANS was reported in 1.1% of patients who received the recommended TECVAYLI dosage in combination with daratumumab and hyaluronidase-fihj, including Grade 4 ICANS in 1 patient. All events of ICANS occurred during the step-up dosing schedule. The median time to onset of ICANS was 2 (range: 1 to 3) days after the most recent dose and the median duration of ICANS was 2 (range: 1 to 2) days. The clinical manifestations of ICANS reported were amnesia, encephalopathy and delirium.
The onset of ICANS can be concurrent with CRS, following resolution of CRS, or in the absence of CRS.
Monitor patients for signs and symptoms of neurologic toxicity, including ICANS during TECVAYLI treatment. At the first sign of neurologic toxicity, including ICANS, immediately evaluate patient and provide supportive therapy based on severity. Withhold until neurologic toxicity resolves or permanently discontinue TECVAYLI based on severity per recommendations and consider further management per current practice guidelines.
Due to the potential for neurologic toxicity, patients receiving TECVAYLI are at risk of depressed level of consciousness. Advise patients to refrain from driving or operating heavy or potentially dangerous machinery during and for 48 hours after completion of TECVAYLI step-up dosing schedule and in the event of new onset of any neurologic toxicity symptoms until neurologic toxicity resolves.
TECVAYLI is available only through a restricted program under a REMS.
TECVAYLI and TALVEY REMS - TECVAYLI is available only through a restricted program under a REMS called the TECVAYLI and TALVEY REMS because of the risks of CRS and neurologic toxicity, including ICANS.
Hepatotoxicity - TECVAYLI can cause hepatotoxicity, including fatalities. There was one fatal case of hepatic failure in MajesTEC-1. In patients who received TECVAYLI at the recommended dose in the clinical trials (monotherapy and combination therapy trials; N=448) elevated aspartate aminotransferase (AST) occurred in 47% of patients, with Grade 3 or 4 elevations in 2.9%. Elevated alanine aminotransferase (ALT) occurred in 48% of patients, with Grade 3 or 4 elevations in 3.8%. Elevated total bilirubin occurred in 10% of patients with Grade 3 or 4 elevations in 0.7%. Liver enzyme elevation can occur with or without concurrent CRS.
Monitor liver enzymes and bilirubin at baseline and during treatment as clinically indicated. Withhold TECVAYLI or consider permanent discontinuation of TECVAYLI based on severity.
Infections - TECVAYLI can cause severe, life-threatening, or fatal infections.
In MajesTEC-1 (N=165), in patients who received the recommended TECVAYLI dosage, serious infections, including opportunistic infections, occurred in 30% of patients, Grade 3 or 4 infections in 35% of patients, and fatal infections in 4.2% of patients.
In MajesTEC-3 (N=283), in patients who received TECVAYLI in combination with daratumumab and hyaluronidase-fihj at the recommended dosage, serious infections, including opportunistic infections, occurred in 54% of patients, Grade 3 or Grade 4 infections in 54% of patients, and fatal infections in 4.6% of patients.
Monitor patients for signs and symptoms of infection prior to and during treatment with TECVAYLI and treat appropriately. Administer prophylactic antimicrobials according to current practice guidelines.
Withhold TECVAYLI or consider permanent discontinuation of TECVAYLI based on severity.
Monitor immunoglobulin levels prior to and during treatment with TECVAYLI and administer subcutaneous or intravenous immunoglobulin (IVIG) to maintain the serum levels >400 mg/dL.
Neutropenia - TECVAYLI can cause neutropenia and febrile neutropenia. In patients who received TECVAYLI at the recommended dose in the clinical trials (monotherapy and combination therapy trials; N=448), decreased neutrophils occurred in 88% of patients, with Grade 3 or 4 decreased neutrophils in 70%. Febrile neutropenia occurred in 6% of patients.
Monitor complete blood cell counts at baseline and periodically during treatment and provide supportive care per local institutional guidelines.
Monitor patients with neutropenia for signs of infection.
Withhold TECVAYLI based on severity.
Hypersensitivity and Other Administration Reactions - TECVAYLI can cause both systemic administration-related and local injection-site reactions.
Systemic Reactions - In patients who received the recommended TECVAYLI dosage in the clinical trials (monotherapy and combination therapy trials; N=448), 2.5% of patients experienced systemic-administration reactions, which included recurrent pyrexia and rash.
Local Reactions - In patients who received TECVAYLI at the recommended dosage in the clinical trials (monotherapy and combination therapy trials; N=448), injection-site reactions occurred in 37% of patients, with Grade 1 injection-site reactions in 29% and Grade 2 in 9%.
Withhold TECVAYLI or consider permanent discontinuation of TECVAYLI based on severity.
Embryo-Fetal Toxicity - Based on its mechanism of action, TECVAYLI may cause fetal harm when administered to a pregnant patient. Advise pregnant patients of the potential risk to the fetus. Advise females of reproductive potential to use effective contraception during treatment with TECVAYLI and for 5 months after the last dose.
ADVERSE REACTIONSThe most common adverse reactions (≥20%) in patients who received TECVAYLI monotherapy were pyrexia, CRS, musculoskeletal pain, injection site reaction, fatigue, upper respiratory tract infection, nausea, headache, pneumonia, and diarrhea. The most common adverse reactions (≥20%) in patients who received TECVAYLI in combination with daratumumab and hyaluronidase-fihj were hypogammaglobulinemia, upper respiratory tract infection, CRS, cough, diarrhea, musculoskeletal pain, COVID-19, pneumonia, injection site reaction, fatigue, pyrexia, headache, nausea, gastroenteritis, and weight decreased.
The most common Grade 3 to 4 laboratory abnormalities (≥20%) with TECVAYLI (as monotherapy or in combination with daratumumab and hyaluronidase-fihj) were decreased lymphocytes, decreased neutrophils, decreased white blood cells, decreased hemoglobin, and decreased platelets.
Please read full Prescribing Information, including Boxed WARNING, for TECVAYLI.
CARVYKTI® IMPORTANT SAFETY INFORMATION
WARNING: CYTOKINE RELEASE SYNDROME, NEUROLOGIC TOXICITIES, HLH/MAS, PROLONGED and RECURRENT CYTOPENIA, and SECONDARY HEMATOLOGICAL MALIGNANCIES
Cytokine Release Syndrome (CRS), including fatal or life-threatening reactions, occurred in patients following treatment with CARVYKTI®. Do not administer CARVYKTI® to patients with active infection or inflammatory disorders. Treat severe or life-threatening CRS with tocilizumab or tocilizumab and corticosteroids.
Immune Effector Cell-associated Neurotoxicity Syndrome (ICANS), which may be fatal or life-threatening, occurred following treatment with CARVYKTI®, including before CRS onset, concurrently with CRS, after CRS resolution, or in the absence of CRS. Monitor for neurologic events after treatment with CARVYKTI®. Provide supportive care and/or corticosteroids as needed.
Parkinsonism and Guillain-Barré syndrome (GBS) and their associated complications resulting in fatal or life-threatening reactions have occurred following treatment with CARVYKTI®.
Hemophagocytic Lymphohistiocytosis/Macrophage Activation Syndrome (HLH/MAS), including fatal and life-threatening reactions, occurred in patients following treatment with CARVYKTI®. HLH/MAS can occur with CRS or neurologic toxicities.
Prolonged and/or recurrent cytopenias with bleeding and infection and requirement for stem cell transplantation for hematopoietic recovery occurred following treatment with CARVYKTI®.
Immune Effector Cell-associated Enterocolitis (IEC-EC), including fatal or life-threatening reactions, occurred following treatment with CARVYKTI®.
Secondary hematological malignancies, including myelodysplastic syndrome and acute myeloid leukemia, have occurred in patients following treatment with CARVYKTI®. T-cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T-cell immunotherapies, including CARVYKTI®.
WARNINGS AND PRECAUTIONS
INCREASED EARLY MORTALITY - In CARTITUDE-4, a (1:1) randomized controlled trial, there was a numerically higher percentage of early deaths in patients randomized to the CARVYKTI® treatment arm compared to the control arm. Among patients with deaths occurring within the first 10 months from randomization, a greater proportion (29/208; 14%) occurred in the CARVYKTI® arm compared to (25/211; 12%) in the control arm. Of the 29 deaths that occurred in the CARVYKTI® arm within the first 10 months of randomization, 10 deaths occurred prior to CARVYKTI® infusion, and 19 deaths occurred after CARVYKTI® infusion. Of the 10 deaths that occurred prior to CARVYKTI® infusion, all occurred due to disease progression, and none occurred due to adverse events. Of the 19 deaths that occurred after CARVYKTI® infusion, 3 occurred due to disease progression, and 16 occurred due to adverse events. The most common adverse events were due to infection (n=12).
CYTOKINE RELEASE SYNDROME (CRS),including fatal or life-threatening reactions, occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® for RRMM in the CARTITUDE-1 & -4 studies (N=285), CRS occurred in 84% (238/285), including ≥ Grade 3 CRS (ASTCT 2019) in 4% (11/285) of patients. Median time to onset of CRS, any grade, was 7 days (range: 1 to 23 days). CRS resolved in 82% with a median duration of 4 days (range: 1 to 97 days). The most common manifestations of CRS in all patients combined (≥10%) included fever (84%), hypotension (29%) and aspartate aminotransferase increased (11%). Serious events that may be associated with CRS include pyrexia, hemophagocytic lymphohistiocytosis, respiratory failure, disseminated intravascular coagulation, capillary leak syndrome, and supraventricular and ventricular tachycardia. CRS occurred in 78% of patients in CARTITUDE-4 (3% Grade 3 to 4) and in 95% of patients in CARTITUDE-1 (4% Grade 3 to 4).
Identify CRS based on clinical presentation. Evaluate for and treat other causes of fever, hypoxia, and hypotension. CRS has been reported to be associated with findings of HLH/MAS, and the physiology of the syndromes may overlap. HLH/MAS is a potentially life-threatening condition. In patients with progressive symptoms of CRS or refractory CRS despite treatment, evaluate for evidence of HLH/MAS.
Confirm that a minimum of 2 doses of tocilizumab are available prior to infusion of CARVYKTI®.
Of the 285 patients who received CARVYKTI® in clinical trials, 53% (150/285) patients received tocilizumab; 35% (100/285) received a single dose, while 18% (50/285) received more than 1 dose of tocilizumab. Overall, 14% (39/285) of patients received at least 1 dose of corticosteroids for treatment of CRS.
Monitor patients at least daily for 7 days following CARVYKTI® infusion for signs and symptoms of CRS. Monitor patients for signs or symptoms of CRS for at least 2 weeks after infusion. At the first sign of CRS, immediately institute treatment with supportive care, tocilizumab, or tocilizumab and corticosteroids.
Counsel patients to seek immediate medical attention should signs or symptoms of CRS occur at any time.
NEUROLOGIC TOXICITIES, which may be severe, life-threatening, or fatal, occurred following treatment with CARVYKTI®. Neurologic toxicities included ICANS, neurologic toxicity with signs and symptoms of Parkinsonism, GBS, immune mediated myelitis, peripheral neuropathies, and cranial nerve palsies. Counsel patients on the signs and symptoms of these neurologic toxicities, and on the delayed nature of onset of some of these toxicities. Instruct patients to seek immediate medical attention for further assessment and management if signs or symptoms of any of these neurologic toxicities occur at any time.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & 4 studies for RRMM, one or more neurologic toxicities occurred in 24% (69/285), including ≥ Grade 3 cases in 7% (19/285) of patients. Median time to onset was 10 days (range: 1 to 101) with 63/69 (91%) of cases developing by 30 days. Neurologic toxicities resolved in 72% (50/69) of patients with a median duration to resolution of 23 days (range: 1 to 544). Of patients developing neurotoxicity, 96% (66/69) also developed CRS. Subtypes of neurologic toxicities included ICANS in 13%, peripheral neuropathy in 7%, cranial nerve palsy in 7%, parkinsonism in 3%, and immune mediated myelitis in 0.4% of the patients.
Immune Effector Cell-Associated Neurotoxicity Syndrome (ICANS): Patients receiving CARVYKTI® may experience fatal or life-threatening ICANS following treatment with CARVYKTI®, including before CRS onset, concurrently with CRS, after CRS resolution, or in the absence of CRS.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, ICANS occurred in 13% (36/285), including Grade ≥3 in 2% (6/285) of the patients. Median time to onset of ICANS was 8 days (range: 1 to 28 days). ICANS resolved in 30 of 36 (83%) of patients, with a median time to resolution of 3 days (range: 1 to 143 days). Median duration of ICANS was 6 days (range: 1 to 1229 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff. Of patients with ICANS, 97% (35/36) had CRS. The onset of ICANS occurred during CRS in 69% of patients, before and after the onset of CRS in 14% of patients, respectively.
Immune Effector Cell-associated Neurotoxicity Syndrome occurred in 7% of patients in CARTITUDE-4 (0.5% Grade 3) and in 23% of patients in CARTITUDE-1 (3% Grade 3). The most frequent (≥2%) manifestations of ICANS included encephalopathy (12%), aphasia (4%), headache (3%), motor dysfunction (3%), ataxia (2%), and sleep disorder (2%).
Monitor patients at least daily for 7 days following CARVYKTI® infusion for signs and symptoms of ICANS. Rule out other causes of ICANS symptoms. Monitor patients for signs or symptoms of ICANS for at least 2 weeks after infusion and treat promptly. Neurologic toxicity should be managed with supportive care and/or corticosteroids as needed. Advise patients to avoid driving for at least 2 weeks following infusion.
Parkinsonism: Neurologic toxicity with parkinsonism has been reported in clinical trials of CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, parkinsonism occurred in 3% (8/285), including Grade ≥3 in 2% (5/285) of the patients. Median time to onset of parkinsonism was 56 days (range: 14 to 914 days). Parkinsonism resolved in 1 of 8 (13%) of patients with a median time to resolution of 523 days. Median duration of parkinsonism was 243.5 days (range: 62 to 720 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff. The onset of parkinsonism occurred after CRS for all patients and after ICANS for 6 patients.
Parkinsonism occurred in 1% of patients in CARTITUDE-4 (no Grade 3 to 4) and in 6% of patients in CARTITUDE-1 (4% Grade 3 to 4).
Manifestations of parkinsonism included movement disorders, cognitive impairment, and personality changes. Monitor patients for signs and symptoms of parkinsonism that may be delayed in onset and managed with supportive care measures. There is limited efficacy information with medications used for the treatment of Parkinson’s disease for the improvement or resolution of parkinsonism symptoms following CARVYKTI® treatment.
Guillain-Barré Syndrome: A fatal outcome following GBS occurred following treatment with CARVYKTI® despite treatment with intravenous immunoglobulins. Symptoms reported include those consistent with Miller-Fisher variant of GBS, encephalopathy, motor weakness, speech disturbances, and polyradiculoneuritis.
Monitor for GBS. Evaluate patients presenting with peripheral neuropathy for GBS. Consider treatment of GBS with supportive care measures and in conjunction with immunoglobulins and plasma exchange, depending on severity of GBS.
Immune Mediated Myelitis: Grade 3 myelitis occurred 25 days following treatment with CARVYKTI® in CARTITUDE-4 in a patient who received CARVYKTI® as subsequent therapy. Symptoms reported included hypoesthesia of the lower extremities and the lower abdomen with impaired sphincter control. Symptoms improved with the use of corticosteroids and intravenous immune globulin. Myelitis was ongoing at the time of death from other cause.
Peripheral Neuropathy occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, peripheral neuropathy occurred in 7% (21/285), including Grade ≥3 in 1% (3/285) of the patients. Median time to onset of peripheral neuropathy was 57 days (range: 1 to 914 days). Peripheral neuropathy resolved in 11 of 21 (52%) of patients with a median time to resolution of 58 days (range: 1 to 215 days). Median duration of peripheral neuropathy was 149.5 days (range: 1 to 692 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff.
Peripheral neuropathies occurred in 7% of patients in CARTITUDE-4 (0.5% Grade 3 to 4) and in 7% of patients in CARTITUDE-1 (2% Grade 3 to 4). Monitor patients for signs and symptoms of peripheral neuropathies. Patients who experience peripheral neuropathy may also experience cranial nerve palsies or GBS.
Cranial Nerve Palsies occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, cranial nerve palsies occurred in 7% (19/285), including Grade ≥3 in 1% (1/285) of the patients. Median time to onset of cranial nerve palsies was 21 days (range: 17 to 101 days). Cranial nerve palsies resolved in 17 of 19 (89%) of patients with a median time to resolution of 66 days (range: 1 to 209 days). Median duration of cranial nerve palsies was 70 days (range: 1 to 262 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff. Cranial nerve palsies occurred in 9% of patients in CARTITUDE-4 (1% Grade 3 to 4) and in 3% of patients in CARTITUDE-1 (1% Grade 3 to 4).
The most frequent cranial nerve affected was the 7th cranial nerve. Additionally, cranial nerves III, V, and VI have been reported to be affected.
Monitor patients for signs and symptoms of cranial nerve palsies. Consider management with systemic corticosteroids, depending on the severity and progression of signs and symptoms.
HEMOPHAGOCYTIC LYMPHOHISTIOCYTOSIS (HLH)/MACROPHAGE ACTIVATION SYNDROME (MAS): Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, HLH/MAS occurred in 1% (3/285) of patients. All events of HLH/MAS had onset within 99 days of receiving CARVYKTI®, with a median onset of 10 days (range: 8 to 99 days), and all occurred in the setting of ongoing or worsening CRS. The manifestations of HLH/MAS included hyperferritinemia, hypotension, hypoxia with diffuse alveolar damage, coagulopathy and hemorrhage, cytopenia, and multi-organ dysfunction, including renal dysfunction and respiratory failure.
Patients who develop HLH/MAS have an increased risk of severe bleeding. Monitor hematologic parameters in patients with HLH/MAS and transfuse per institutional guidelines. Fatal cases of HLH/MAS occurred following treatment with CARVYKTI®.
HLH is a life-threatening condition with a high mortality rate if not recognized and treated early. Treatment of HLH/MAS should be administered per institutional standards.
PROLONGED AND RECURRENT CYTOPENIAS: Patients may exhibit prolonged and recurrent cytopenias following lymphodepleting chemotherapy and CARVYKTI® infusion.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, Grade 3 or higher cytopenias not resolved by Day 30 following CARVYKTI® infusion occurred in 62% (176/285) of the patients and included thrombocytopenia 33% (94/285), neutropenia 27% (76/285), lymphopenia 24% (67/285), and anemia 2% (6/285). After Day 60 following CARVYKTI® infusion, 22%, 20%, 5%, and 6% of patients had a recurrence of Grade 3 or 4 lymphopenia, neutropenia, thrombocytopenia, and anemia, respectively, after initial recovery of their Grade 3 or 4 cytopenia. Seventy-seven percent (219/285) of patients had one, two, or three or more recurrences of Grade 3 or 4 cytopenias after initial recovery of Grade 3 or 4 cytopenia. Sixteen and 25 patients had Grade 3 or 4 neutropenia and thrombocytopenia, respectively, at the time of death.
Monitor blood counts prior to and after CARVYKTI® infusion. Manage cytopenias with growth factors and blood product transfusion support according to local institutional guidelines.
INFECTIONS: CARVYKTI® should not be administered to patients with active infection or inflammatory disorders. Severe, life-threatening, or fatal infections occurred in patients after CARVYKTI® infusion.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, infections occurred in 57% (163/285), including Grade ≥3 in 24% (69/285) of patients. Grade 3 or 4 infections with an unspecified pathogen occurred in 12%, viral infections in 6%, bacterial infections in 5%, and fungal infections in 1% of patients. Overall, 5% (13/285) of patients had Grade 5 infections, 2.5% of which were due to COVID-19. Patients treated with CARVYKTI® had an increased rate of fatal COVID-19 infections compared to the standard therapy arm.
Monitor patients for signs and symptoms of infection before and after CARVYKTI® infusion and treat patients appropriately. Administer prophylactic, pre-emptive, and/or therapeutic antimicrobials according to the standard institutional guidelines. Febrile neutropenia was observed in 5% of patients after CARVYKTI® infusion and may be concurrent with CRS. In the event of febrile neutropenia, evaluate for infection and manage with broad-spectrum antibiotics, fluids, and other supportive care, as medically indicated. Counsel patients on the importance of prevention measures. Follow institutional guidelines for the vaccination and management of immunocompromised patients with COVID-19.
Viral Reactivation: Hepatitis B virus (HBV) reactivation, in some cases resulting in fulminant hepatitis, hepatic failure, and death, can occur in patients with hypogammaglobulinemia. Perform screening for Cytomegalovirus (CMV), HBV, hepatitis C virus (HCV), and human immunodeficiency virus (HIV) or any other infectious agents if clinically indicated in accordance with clinical guidelines before collection of cells for manufacturing. Consider antiviral therapy to prevent viral reactivation per local institutional guidelines/clinical practice.
Reactivation of John Cunningham (JC) virus, leading to progressive multifocal leukoencephalopathy (PML), including cases with fatal outcomes, have been reported following treatment. Perform appropriate diagnostic evaluations in patients with neurological adverse events.
HYPOGAMMAGLOBULINEMIA: can occur in patients receiving treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, hypogammaglobulinemia adverse event was reported in 36% (102/285) of patients; laboratory IgG levels fell below 500 mg/dL after infusion in 93% (265/285) of patients. Hypogammaglobulinemia either as an adverse reaction or laboratory IgG level below 500 mg/dL after infusion occurred in 94% (267/285) of patients treated. Fifty-six percent (161/285) of patients received intravenous immunoglobulin (IVIG) post CARVYKTI® for either an adverse reaction or prophylaxis.
Monitor immunoglobulin levels after treatment with CARVYKTI® and administer IVIG for IgG <400 mg/dL. Manage per local institutional guidelines, including infection precautions and antibiotic or antiviral prophylaxis.
Use of Live Vaccines: The safety of immunization with live viral vaccines during or following CARVYKTI® treatment has not been studied. Vaccination with live virus vaccines is not recommended for at least 6 weeks prior to the start of lymphodepleting chemotherapy, during CARVYKTI® treatment, and until immune recovery following treatment with CARVYKTI®.
HYPERSENSITIVITY REACTIONS occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, hypersensitivity reactions occurred in 5% (13/285), all of which were ≤2 Grade. Manifestations of hypersensitivity reactions included flushing, chest discomfort, tachycardia, wheezing, tremor, burning sensation, non-cardiac chest pain, and pyrexia. Serious hypersensitivity reactions, including anaphylaxis, may be due to the dimethyl sulfoxide (DMSO) in CARVYKTI®. Patients should be carefully monitored for 2 hours after infusion for signs and symptoms of severe reaction. Treat promptly and manage patients appropriately according to the severity of the hypersensitivity reaction.
IMMUNE EFFECTOR CELL-ASSOCIATED ENTERCOLITIS (IEC-EC) has occurred in patients treated with CARVYKTI®. Manifestations include severe or prolonged diarrhea, abdominal pain, and weight loss requiring parenteral nutrition. IEC-EC has been associated with fatal outcome from perforation or sepsis. Manage according to institutional guidelines, including referral to gastroenterology and infectious disease specialists. In cases of refractory IEC-EC, consider additional workup to exclude alternative etiologies, including T-cell lymphoma of the GI tract, which has been reported in the post marketing setting.
SECONDARY MALIGNANCIES: Patients treated with CARVYKTI® may develop secondary malignancies. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, myeloid neoplasms occurred in 5% (13/285) of patients (9 cases of myelodysplastic syndrome, 3 cases of acute myeloid leukemia, and 1 case of myelodysplastic syndrome followed by acute myeloid leukemia). The median time to onset of myeloid neoplasms was 447 days (range: 56 to 870 days) after treatment with CARVYKTI®. Ten of these 13 patients died following the development of myeloid neoplasms; 2 of the 13 cases of myeloid neoplasm occurred after initiation of subsequent antimyeloma therapy. Cases of myelodysplastic syndrome and acute myeloid leukemia have also been reported in the post marketing setting. T-cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T-cell immunotherapies, including CARVYKTI®. Mature T-cell malignancies, including CAR-positive tumors, may present as soon as weeks following infusions, and may include fatal outcomes.
Monitor lifelong for secondary malignancies. In the event that a secondary malignancy occurs, contact Janssen Biotech, Inc., at 1-800-526-7736 for reporting and to obtain instructions on collection of patient samples.
ADVERSE REACTIONS The most common nonlaboratory adverse reactions (incidence greater than 20%) are pyrexia, cytokine release syndrome, hypogammaglobulinemia, hypotension, musculoskeletal pain, fatigue, infections-pathogen unspecified, cough, chills, diarrhea, nausea, encephalopathy, decreased appetite, upper respiratory tract infection, headache, tachycardia, dizziness, dyspnea, edema, viral infections, coagulopathy, constipation, and vomiting. The most common Grade 3 or 4 laboratory adverse reactions (incidence greater than or equal to 50%) include lymphopenia, neutropenia, white blood cell decreased, thrombocytopenia, and anemia.
Please read full Prescribing Information, including Boxed Warning, for CARVYKTI®.
IMBRUVICA® IMPORTANT SAFETY INFORMATION
INDICATIONS
IMBRUVICA® is a kinase inhibitor indicated for the treatment of:
Adult patients with chronic lymphocytic leukemia (CLL)/Small lymphocytic lymphoma (SLL). Adult patients with chronic lymphocytic leukemia (CLL)/Small lymphocytic lymphoma (SLL) with 17p deletion. Adult patients with Waldenström’s macroglobulinemia (WM). Adult and pediatric patients age 1 year and older with chronic graft versus host disease (cGVHD) after failure of one or more lines of systemic therapy.
For more information, visit www.IMBRUVICA.com.
WARNINGS AND PRECAUTIONS
Hemorrhage: Fatal bleeding events have occurred in patients who received IMBRUVICA®. Major hemorrhage (≥ Grade 3, serious, or any central nervous system events; e.g., intracranial hemorrhage [including subdural hematoma], gastrointestinal bleeding, hematuria, and post procedural hemorrhage) occurred in 4.2% of patients, with fatalities occurring in 0.4% of 2,838 patients who received IMBRUVICA® in 27 clinical trials. Bleeding events of any grade including bruising and petechiae occurred in 39%, and excluding bruising and petechiae occurred in 23% of patients who received IMBRUVICA®, respectively.
The mechanism for the bleeding events is not well understood.
Use of either anticoagulant or antiplatelet agents concomitantly with IMBRUVICA® increases the risk of major hemorrhage. Across clinical trials, 3.1% of 2,838 patients who received IMBRUVICA® without antiplatelet or anticoagulant therapy experienced major hemorrhage. The addition of antiplatelet therapy with or without anticoagulant therapy increased this percentage to 4.4%, and the addition of anticoagulant therapy with or without antiplatelet therapy increased this percentage to 6.1%. Consider the risks and benefits of anticoagulant or antiplatelet therapy when co-administered with IMBRUVICA®. Monitor for signs and symptoms of bleeding.
Consider the benefit-risk of withholding IMBRUVICA® for at least 3 to 7 days pre- and post-surgery depending upon the type of surgery and the risk of bleeding.
Infections: Fatal and non-fatal infections (including bacterial, viral, or fungal) have occurred with IMBRUVICA® therapy. Grade 3 or greater infections occurred in 21% of 1,476 patients with B-cell malignancies who received IMBRUVICA® in clinical trials. Cases of progressive multifocal leukoencephalopathy (PML) and Pneumocystis jirovecii pneumonia (PJP) have occurred in patients treated with IMBRUVICA®. Consider prophylaxis according to standard of care in patients who are at increased risk for opportunistic infections. Monitor and evaluate patients for fever and infections and treat appropriately.
Cardiac Arrhythmias, Cardiac Failure, and Sudden Death: Fatal and serious cardiac arrhythmias and cardiac failure have occurred with IMBRUVICA®. Deaths due to cardiac causes or sudden deaths occurred in 1% of 4,896 patients who received IMBRUVICA® in clinical trials, including in patients who received IMBRUVICA® in unapproved monotherapy or combination regimens. These adverse reactions occurred in patients with and without preexisting hypertension or cardiac comorbidities. Patients with cardiac comorbidities may be at greater risk of these events. Grade 3 or greater ventricular tachyarrhythmias were reported in 0.2%, Grade 3 or greater atrial fibrillation and atrial flutter were reported in 3.7%, and Grade 3 or greater cardiac failure was reported in 1.3% of 4,896 patients who received IMBRUVICA® in clinical trials, including in patients who received IMBRUVICA® in unapproved monotherapy or combination regimens. These events have occurred particularly in patients with cardiac risk factors including hypertension and diabetes mellitus, a previous history of cardiac arrhythmias, and in patients with acute infections. Evaluate cardiac history and function at baseline, and monitor patients for cardiac arrhythmias and cardiac function. Obtain further evaluation (e.g., ECG, echocardiogram) as indicated for patients who develop symptoms of arrhythmia (e.g., palpitations, lightheadedness, syncope, chest pain), new onset dyspnea, or other cardiovascular concerns. Manage cardiac arrhythmias and cardiac failure appropriately, follow dose modification guidelines, and consider the risks and benefits of continued IMBRUVICA® treatment.
Hypertension: Hypertension occurred in 19% of 1,476 patients with B-cell malignancies who received IMBRUVICA® in clinical trials. Grade 3 or greater hypertension occurred in 8% of patients. Based on data from a subset of these patients, (N=1,124), the median time to onset was 5.9 months (range, 0 to 24 months). In a long-term safety analysis over 5 years of 1,284 patients with B-cell malignancies treated for a median of 36 months (range, 0 to 98 months), the cumulative rate of hypertension increased over time. The prevalence for Grade 3 or greater hypertension was 4% (year 0-1), 7% (year 1-2), 9% (year 2-3), 9% (year 3-4), and 9% (year 4-5); the overall incidence for the 5-year period was 11%. Monitor blood pressure in patients treated with IMBRUVICA®, initiate or adjust anti-hypertensive medication throughout treatment with IMBRUVICA® as appropriate, and follow dosage modification guidelines for Grade 3 or higher hypertension.
Cytopenias: In 645 patients with B-cell malignancies who received IMBRUVICA® as a single agent, grade 3 or 4 neutropenia occurred in 23% of patients, grade 3 or 4 thrombocytopenia in 8% and grade 3 or 4 anemia in 2.8%, based on laboratory measurements. Monitor complete blood counts monthly.
Second Primary Malignancies: Other malignancies (10%), including non-skin carcinomas (3.9%), occurred among the 1,476 patients with B-cell malignancies who received IMBRUVICA® in clinical trials. The most frequent second primary malignancy was non-melanoma skin cancer (6%).
Tumor Lysis Syndrome: Tumor lysis syndrome has been infrequently reported with IMBRUVICA®. Assess the baseline risk (e.g., high tumor burden) and take appropriate precautions. Monitor patients closely and treat as appropriate.
Embryo-Fetal Toxicity: Based on findings in animals, IMBRUVICA® can cause fetal harm when administered to a pregnant woman. Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with IMBRUVICA® and for 1 month after the last dose. Advise males with female partners of reproductive potential to use effective contraception during the same time period.
ADVERSE REACTIONS
B-cell malignancies: The most common adverse reactions (≥30%) in adult patients with B-cell malignancies were thrombocytopenia (55%)*, diarrhea (44%), fatigue (39%), musculoskeletal pain (39%), neutropenia (39%)*, rash (36%), anemia (35%)*, bruising (32%), and nausea (30%).
The most common Grade ≥ 3 adverse reactions (≥5%) in adult patients with B-cell malignancies were neutropenia (21%)*, thrombocytopenia (14%)*, pneumonia (8%), and hypertension (8%).
Approximately 9% (CLL/SLL), and 14% (WM) of adult patients had a dose reduction due to adverse reactions.Approximately 4-10% (CLL/SLL) and 5% (WM) of adult patients discontinued due to adverse reactions.cGVHD: The most common adverse reactions (≥20%) in adult or pediatric patients with cGVHD were fatigue (57%), anemia (49%)*, bruising (40%), diarrhea (36%), thrombocytopenia (33%)*, musculoskeletal pain (30%), pyrexia (30%), muscle spasms (29%), stomatitis (29%), hemorrhage (26%), nausea (26%), abdominal pain (23%), pneumonia (23%), and headache (21%).
The most common Grade 3 or higher adverse reactions (≥5%) reported in adult or pediatric patients with cGVHD were pneumonia (14%), anemia (13%)*, fatigue (12%), pyrexia (11%), diarrhea (10%), neutropenia (10%)*, sepsis (10%), osteonecrosis (9%), stomatitis (9%), hypokalemia (7%), headache (5%), and musculoskeletal pain (5%).
Discontinuation of IMBRUVICA® treatment due to an adverse reaction occurred in 24% of adult patients and 23% of pediatric patients. Adverse reactions leading to dose reduction occurred in 26% of adult patients and 19% of pediatric patients.
*Treatment-emergent decreases (all grades) were based on laboratory measurements.
DRUG INTERACTIONS
CYP3A Inhibitors: Co-administration of IMBRUVICA® with strong or moderate CYP3A inhibitors may increase ibrutinib plasma concentrations. Increased ibrutinib concentrations may increase the risk of drug-related toxicity. Dose modifications of IMBRUVICA® are recommended when used concomitantly with posaconazole, voriconazole, and moderate CYP3A inhibitors. Avoid concomitant use of other strong CYP3A inhibitors. Interrupt IMBRUVICA® if strong inhibitors are used short-term (e.g., for ≤ 7 days). Avoid grapefruit and Seville oranges during IMBRUVICA® treatment, as these contain strong or moderate inhibitors of CYP3A. See dose modification guidelines in USPI sections 2.3 and 7.1.
CYP3A Inducers: Avoid coadministration with strong CYP3A inducers.
SPECIFIC POPULATIONS
Pediatric Use: The safety and effectiveness of IMBRUVICA® have not been established for the treatment of cGVHD after failure of one or more lines of therapy in pediatric patients less than 1 year of age. The safety and effectiveness of IMBRUVICA® in pediatric patients have not been established in CLL/SLL, CLL/SLL with 17p deletion, WM, or in patients with mature B-cell non-Hodgkin lymphoma.
In the randomized population from a study that included 35 patients (26 pediatric patients age 5 to less than 17 years) with previously treated mature B-cell non-Hodgkin lymphoma, major hemorrhage and discontinuation of chemoimmunotherapy due to adverse reactions occurred more frequently in the ibrutinib plus chemoimmunotherapy arm compared to the chemoimmunotherapy alone arm.
Hepatic Impairment:Adult Patients with B-cell Malignancies: Hepatic Impairment (based on Child-Pugh criteria): Avoid use of IMBRUVICA® in patients with severe hepatic impairment. In patients with mild or moderate impairment, reduce recommended IMBRUVICA® dose and monitor more frequently for adverse reactions of IMBRUVICA®.
Patients with cGVHD: Avoid use of IMBRUVICA® in patients with total bilirubin level > 3x upper limit of normal (ULN) (unless of non-hepatic origin or due to Gilbert’s syndrome). Reduce recommended dose when administering IMBRUVICA® to patients with total bilirubin level > 1.5 to 3x ULN (unless of non-hepatic origin or due to Gilbert’s syndrome).
Please click here to see the full Prescribing Information.
ABOUT JOHNSON & JOHNSONAt Johnson & Johnson, we believe health is everything. Our strength in healthcare innovation empowers us to build a world where complex diseases are prevented, treated, and cured, where treatments are smarter and less invasive, and solutions are personal. Through our expertise in Innovative Medicine and MedTech, we are uniquely positioned to innovate across the full spectrum of healthcare solutions today to deliver the breakthroughs of tomorrow and profoundly impact health for humanity.
Learn more at https://www.jnj.com/ or at www.innovativemedicine.jnj.com.
Follow us at @JNJInnovMed.
Janssen Biotech, Inc., is a Johnson & Johnson company.
Cautions Concerning Forward-Looking StatementsThis press release contains “forward-looking statements” as defined in the Private Securities Litigation Reform Act of 1995 related to TALVEY ® (talquetamab), DARZALEX FASPRO® (daratumumab), IMAAVY ® (nipocalimab-aahu), TECVAYLI ® (teclistamab), CARVYKTI ® (ciltacabtagene autoleucel; cilta-cel), bleximenib (JNJ-75276617) and IMBRUVICA® (ibrutinib). The reader is cautioned not to rely on these forward-looking statements. These statements are based on current expectations of future events. If underlying assumptions prove inaccurate or known or unknown risks or uncertainties materialize, actual results could vary materially from the expectations and projections of Johnson & Johnson. Risks and uncertainties include, but are not limited to: challenges and uncertainties inherent in product research and development, including the uncertainty of clinical success and of obtaining regulatory approvals; uncertainty of commercial success; manufacturing difficulties and delays; competition, including technological advances, new products and patents attained by competitors; challenges to patents; product efficacy or safety concerns resulting in product recalls or regulatory action; changes in behavior and spending patterns of purchasers of health care products and services; changes to applicable laws and regulations, including global health care reforms; and trends toward health care cost containment. A further list and descriptions of these risks, uncertainties and other factors can be found in Johnson & Johnson’s most recent Annual Report on Form 10-K, including in the sections captioned “Cautionary Note Regarding Forward-Looking Statements” and “Item 1A. Risk Factors,” and in Johnson & Johnson’s subsequent Quarterly Reports on Form 10-Q and other filings with the Securities and Exchange Commission. Copies of these filings are available online at www.sec.gov, www.jnj.com, www.investor.jnj.com or on request from Johnson & Johnson. Johnson & Johnson does not undertake to update any forward-looking statement as a result of new information or future events or developments.
# # #
1 Rarediseases.org. Warm Autoimmune Hemolytic Anemia. Available at https://rarediseases.org/rare-diseases/warm-autoimmune-hemolytic-anemia/. Last accessed: May 2026.
2 Rajkumar SV. Multiple Myeloma: 2020 Update on Diagnosis, Risk-Stratification and Management. Am J Hematol. 2020;95(5):548-567.
3 National Cancer Institute. Plasma cell neoplasms. Avaliable at https://www.cancer.gov/types/myeloma/patient/myeloma-treatment-pdq. Last accessed May 2026.
4 City of Hope (2022) Multiple myeloma: Causes, symptoms & treatments. Avaliable at https://www.cancercenter.com/cancer-types/multiple-myeloma. Last accessed: May 2026.
5 International Agency for Research on Cancer (World Health Organization). (2024). Multiple myeloma fact sheet. Avaliable at https://gco.iarc.who.int/media/globocan/factsheets/cancers/35-multiple-myeloma-fact-sheet.pdf. Last accessed: May 2026.
6 SEER Explorer: An interactive website for SEER cancer statistics. Surveillance Research Program, National Cancer Institute. Avaliable at https://seer.cancer.gov/explorer/. Last accessed May 2026.
7 American Cancer Society. What is multiple myeloma? Avaliable at https://www.cancer.org/cancer/multiple-myeloma/about/what-is-multiple-myeloma.html. Last accessed: May 2026.
8 American Cancer Society. Multiple myeloma early detection, diagnosis, and staging. Avaliable at https://www.cancer.org/cancer/types/multiple-myeloma/detection-diagnosis-staging/detection.html. Last accessed May 2026.
9 Kazandjian D. Multiple myeloma epidemiology and survival: a unique malignancy. J Clin Oncol. 2018;36(15):1479–1487. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC6119139/
10 Tranekær S, et al. Epidemiology of secondary warm autoimmune haemolytic anaemia-A systematic review and meta-analysis. J Clin Med. 2021 Mar 17;10(6):1244.
11 Sudulagunta SR, et al. Warm Autoimmune Hemolytic Anemia: Clinical Profile and Management. J Hematol. 2017 Mar; 6(1): 12–20. Published online 2017 Mar 21. doi: 10.14740/jh303w.
12 National Organization for Rare Disorders, Warm autoimmune Hemolytic Anemia. Available at: https://rarediseases.org/rare-diseases/warm-autoimmune-hemolytic-anemia/. Last accessed: May 2026.
13 Cherif H, Cai Q, Crivera C, Leon A, Rahman I, Leval A, Noel W, Kjellander C. Overall survival and treatment patterns among patients with warm autoimmune hemolytic anemia in Sweden: A nationwide population-based study. Eur J Haematol, 2025 Jan;114(1):129-138.
14 Fattizzo B, Barcellini W. New therapies for the treatment of warm autoimmune hemolytic anemia. Transfusion Medical Reviews. 2022;36(4).
15 The Leukemia & Lymphoma Society. Facts 2022–2023: Updated data on blood cancers. Avaliable athttps://www.lls.org/sites/default/files/2023-08/PS80_Facts_2022_2023.pdf. Last accessed: May 2026.
16 MD Anderson Cancer Center. Acute myeloid leukemia. Avaliable at https://www.mdanderson.org/cancer-types/acute-myeloid-leukemia.html. Last accessed: May 2026.
17 American Cancer Society. Signs and symptoms of acute myeloid leukemia (AML). Avaliable at https://www.cancer.org/cancer/types/acute-myeloid-leukemia/detection-diagnosis-staging/signs-symptoms.html. Last accessed: May 2026.
18 Shimony S, Stahl M, Stone RM. Acute myeloid leukemia: 2023 update on diagnosis, risk‑stratification, and management. Am J Hematol. 2023;98(3):502–526.https://doi.org/10.1002/ajh.26822. Accessed June 2026.
19 TALVEY® U.S. Prescribing Information. Horsham, PA: Janssen Biotech, Inc. August 2023.
20 European Medicines Agency. TALVEY Summary of Product Characteristics. August 2023.
21 DARZALEX FASPRO® U.S. Prescribing Information. 2025. Horsham, PA: Janssen Biotech, Inc.
22 DARZALEX® U.S. Prescribing Information. 2022. Horsham, PA: Janssen Biotech, Inc.
23 IMAAVY® U.S. Prescribing Information. 2025. Horsham, PA: Janssen Biotech, Inc.
24 ClinicalTrials.gov Identifier: NCT04951622. Available at: https://clinicaltrials.gov/ct2/show/NCT04951622. Last accessed: May 2026.
25 ClinicalTrials.gov Identifier: NCT03842189. Available at: https://clinicaltrials.gov/ct2/show/NCT03842189. Last accessed: May 2026.
26 ClinicalTrials.gov Identifier: NCT05327114. Available at: https://www.clinicaltrials.gov/study/NCT05327114. Last accessed: May 2026.
27 ClinicalTrials.gov Identifier: NCT04119050. Available at: https://clinicaltrials.gov/study/NCT04119050. Last accessed: May 2026.
28 ClinicalTrials.gov Identifier: NCT05379634. Available at: https://clinicaltrials.gov/study/NCT05379634. Last accessed: May 2026.
29 ClinicalTrials.gov Identifier: NCT05912517. Available at: https://www.clinicaltrials.gov/study/NCT05912517. Last accessed: May 2026.
30 ClinicalTrials.gov Identifier: NCT04968912. Available at: https://clinicaltrials.gov/study/NCT04968912. Last accessed: May 2026.
31 ClinicalTrials.gov Identifier: NCT04882878. Available at: https://clinicaltrials.gov/study/NCT04882878. Last accessed: May 2026.
32 ClinicalTrials.gov Identifier: NCT06449651. Available at: https://clinicaltrials.gov/study/NCT06449651. Last accessed: May 2026.
33 ClinicalTrials.gov Identifier: NCT06533098 Available at: https://clinicaltrials.gov/study/NCT06533098. Last accessed: May 2026.
34 U.S. FDA Approves TECVAYLI® (teclistamab-cqyv), the First Bispecific T-cell Engager Antibody for the Treatment of Patients with Relapsed or Refractory Multiple Myeloma. Avaliable at https://www.jnj.com/u-s-fda-approves-tecvayli-teclistamab-cqyv-the-first-bispecific-t-cell-engager-antibody-for-the-treatment-of-patients-with-relapsed-or-refractory-multiple-myeloma. Last accessed: May 2025.
35 CARVYKTI® U.S. Prescribing Information. 2025. Horsham, PA: Janssen Biotech, Inc.
36 Genetics Home Reference. Isolated growth hormone deficiency. Avaliable at http://ghr.nlm.nih.gov/condition/isolated-growth-hormone-deficiency. Last accessed: May 2026.
37 Turetsky A, et al. Single cell imaging of Bruton’s tyrosine kinase using an irreversible inhibitor. Scientific Reports. 2014;6:4782.
38 de Rooij MF, et al. The clinically active BTK inhibitor PCI-32765 targets B-cell receptor- and chemokine-controlled adhesion and migration in chronic lymphocytic leukemia. Blood. 2012;119(11):2590-2594.
39 IMBRUVICA® U.S. Prescribing Information, February 2024. Horsham, PA: Janssen Biotech, Inc.
Media contact:Bridget Kimmelbkimmel@its.jnj.com
Oncology Media Relationsoncology_media_relations@its.jnj.com
Investor contact:Jess Margevichinvestor-relations@its.jnj.com
Phase 3Clinical ResultPhase 2Drug ApprovalOrphan Drug
29 Apr 2026
RARITAN, N.J., April 29, 2026 – Johnson & Johnson (NYSE:JNJ) will present more than 20 abstracts at the 2026 American Society of Clinical Oncology (ASCO) Annual Meeting, highlighting the breadth of the Company’s leadership in oncology research across solid tumors and hematologic malignancies. The data include late-breaking Phase 3 PROTEUS results for ERLEADA® (apalutamide) in curative-intent treatment of high-risk localized or locally advanced prostate cancer, to be featured in a plenary session, along with additional studies across multiple myeloma and prostate, head and neck, lung, colorectal, and bladder cancers.
Perspectives on Key Data Readouts at ASCO
“Our pivotal, practice‑defining data at ASCO reflect the momentum of our oncology strategy and the depth of our scientific investment across solid tumors and hematologic malignancies,” said Yusri Elsayed, M.D., M.H.Sc., Ph.D., Global Therapeutic Area Head, Oncology, Johnson & Johnson. “With a portfolio built to intervene earlier, target smarter, and deliver more durable outcomes, we are advancing potential new standards of care for patients with high-risk localized prostate cancer, multiple myeloma, and recurrent head and neck cancer, and remain steadfast in our mission to one day eliminate cancer.”
Key Data Presentations
Prostate Cancer
Final analysis from the Phase 3 PROTEUS study evaluating the safety and efficacy of perioperative ERLEADA® plus hormone therapy (androgen deprivation therapy) before and after prostate surgery in high-risk localized or locally advanced prostate cancer (Plenary Session – Oral Abstract LBA#1) Trial-in-progress update from the Phase 3 KLK2-comPAS study of pasritamig (JNJ-78278343) in combination with best supportive care in metastatic castration-resistant prostate cancer (Poster Abstract #TPS5136) Trial-in-progress update from the Phase 3 KLK2-PASenger study of pasritamig in combination with docetaxel compared with docetaxel alone in metastatic castration-resistant prostate cancer (Poster Abstract #TPS5139)
Multiple Myeloma
Results from the Phase 3 MajesTEC-9 study of TECVAYLI® (teclistamab-cqyv) versus standard of care therapies as early as second line in patients with multiple myeloma (Oral Abstract #7507) Subgroup analysis from the Phase 3 PERSEUS study evaluating the benefit of DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) in transplant-eligible patients with high- and standard-risk multiple myeloma (Oral Abstract #7505) Final subgroup analysis from the Phase 3 CEPHEUS study evaluating DARZALEX FASPRO® in combination with bortezomib, lenalidomide, and dexamethasone in transplant-ineligible newly diagnosed multiple myeloma (Rapid Oral Abstract #7513) Results from the Phase 2 OPTec/OPTal study evaluating outpatient, step-up administration of TECVAYLI® or TALVEY® (talquetamab-tgvs) with prophylactic tocilizumab in patients with relapsed or refractory multiple myeloma (RRMM) (Rapid Oral Abstract #7510) Cytogenetic subgroup analysis from the Phase 3 CARTITUDE-4 study evaluating CARVYKTI® (ciltacabtagene autoleucel; cilta-cel)in patients with lenalidomide-refractory multiple myeloma responding to bridging therapy (Poster Abstract #7536) Results from the CARTITUDE clinical studies of CARVYKTI® evaluating incidence and characterization of Immune Effector Cell-Associated Enterocolitis (IEC-EC) in RRMM (Poster Abstract #7533)
Head and Neck Cancer
Pivotal Phase 1b/2 OrigAMI-4 results evaluating RYBREVANT FASPRO™ (amivantamab and hyaluronidase-lpuj) in patients with recurrent or metastatic head and neck cancer following prior immunotherapy and chemotherapy (Oral Abstract #6008) Trial-in-progress update from the Phase 3 OrigAMI-5 study of RYBREVANT FASPRO™ in combination with immunotherapy and chemotherapy in the first-line recurrent or metastatic head and neck setting (Abstract #TPS6127)
Lung Cancer
Updated results from the CHRYSALIS-2 study, including overall survival, for RYBREVANT® (amivantamab-vmjw) and LAZCLUZE®(lazertinib) in the first-line treatment of patients with atypical EGFR-mutated non-small cell lung cancers (Oral Abstract #8501) Early safety results from the Phase 2b COPERNICUS study evaluating a pragmatic approach to RYBREVANT FASPRO™ plus LAZCLUZE® with proactive therapy management in the first-line treatment of patients with advanced EGFR-mutated non-small cell lung cancer (Poster Abstract #8613) Interim efficacy and safety results from the Phase 2b COPERNICUS study of RYBREVANT FASPRO™ plus chemotherapy with enhanced proactive management of potential dermatological effects in patients with previously treated advanced EGFR-mutated non-small cell lung cancer (Poster Abstract #8614)
Colorectal Cancer
· Biomarker analyses from the Phase 1b/2 OrigAMI-1 study of RYBREVANT® across different tumor subtypes in RAS/BRAF wild-type metastatic colorectal cancer (Poster Abstract #3548)
Bladder Cancer
· A real-world market research study exploring decision-making and regret after radical cystectomy (Online Publication #e16605)
Information on abstracts sponsored by Johnson & Johnson is available on JNJ.com.
About ERLEADA®ERLEADA® (apalutamide) is an androgen receptor inhibitor indicated for the treatment of patients with non-metastatic castration-resistant prostate cancer (nmCRPC) and for the treatment of patients with metastatic castration-sensitive prostate cancer (mCSPC). ERLEADA® received U.S. Food and Administration (FDA) approval for nmCRPC in February 2018 and received U.S. FDA approval for mCSPC in September 2019.ERLEADA® is the first and only next-generation androgen receptor inhibitor offering a once-daily, single-tablet treatment option for patients. To date, more than 340,000 patients worldwide have been treated with ERLEADA®. Additional studies are ongoing to evaluate ERLEADA® in earlier stages of prostate cancer, including high-risk localized and locally advanced disease.1
The legal manufacturer for ERLEADA® is Janssen Biotech, Inc. For more information, visit www.ERLEADA.com.
About Pasritamig (JNJ-78278343)Pasritamig (JNJ-78278343) is an investigational bispecific T-cell-engager antibody (bsAb) targeting human kallikrein 2 (KLK2), a novel and highly specific prostate cancer target, and CD3 receptor complexes on T cells, leveraging the body’s immune system to selectively target and eliminate cancer cells. This innovative approach is being evaluated in patients with metastatic castration-resistant prostate cancer (mCRPC), who have limited treatment options.
About TECVAYLI®TECVAYLI® (teclistamab-cqyv) is a first-in-class, bispecific T-cell engager antibody therapy that uses innovative science to activate the immune system by binding to the CD3 receptor expressed on the surface of T-cells and to the B-cell maturation antigen (BCMA) expressed on the surface of multiple myeloma cells and some healthy B-lineage cells. TECVAYLI® received accelerated approval from the U.S. Food and Drug Administration (FDA) in October 2022 as an off-the-shelf (or ready-to-use) antibody that is administered as a subcutaneous treatment for adult patients with relapsed or refractory multiple myeloma (RRMM) who received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 antibody.2
In February 2024, the U.S. FDA approved the supplemental Biologics License Application (sBLA) for TECVAYLI® for a reduced dosing frequency of 1.5 mg/kg every two weeks in patients with RRMM who achieved and maintained a complete response (CR) or better for a minimum of six months. In March 2026, the U.S. FDA approved TECVAYLI® in combination with DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) for the treatment of adult patients with relapsed or refractory multiple myeloma who have received at least one prior line of therapy, including a proteasome inhibitor and an immunomodulatory agent. The supplemental Biologics License Application was proactively selected for the Commissioner’s National Priority Voucher Pilot Program and also granted the application Breakthrough Therapy Designation and Real-Time Oncology Review. This approval expanded the use of TECVAYLI® into earlier lines of therapy and is the first bispecific antibody-based combination regimen in this setting, offering a potential new standard of care as early as second line.
To date, more than 26,000 patients have been treated worldwide with TECVAYLI®.
The European Commission (EC) granted TECVAYLI® conditional marketing authorization in August 2022 as monotherapy for the treatment of adult patients with RRMM who have received at least three prior therapies, including a proteasome inhibitor, an immunomodulatory agent and an anti-CD38 antibody, and have demonstrated disease progression since the last therapy. In August 2023, the EC approved a Type II variation application for TECVAYLI®, providing the option for a reduced dosing frequency of 1.5 mg/kg every two weeks (Q2W) in patients who have achieved a complete response or better for a minimum of six months.For more information, visit www.TECVAYLI.com.
About DARZALEX FASPRO® and DARZALEX®DARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) received U.S. FDA approval in May 2020 and is approved for 11 indications in multiple myeloma, four of which are for frontline treatment in newly diagnosed patients who are transplant eligible or ineligible.3 It is the only subcutaneous CD38-directed antibody approved to treat patients with multiple myeloma. DARZALEX FASPRO® is co-formulated with recombinant human hyaluronidase PH20 (rHuPH20), Halozyme’s ENHANZE® drug delivery technology.
DARZALEX® (daratumumab) received U.S. FDA approval in November 2015 and is approved in eight indications, three of which are in the frontline setting, including newly diagnosed patients who are transplant-eligible and ineligible.4 In 2025, DARZALEX FASPRO® was approved by the U.S. FDA and EMA as the first and only treatment for patients with high-risk smoldering multiple myeloma.
DARZALEX® is the first CD38-directed antibody approved to treat multiple myeloma.2 DARZALEX®-based regimens have been used in the treatment of more than 748,000 patients worldwide and more than 68,000 patients in the U.S. alone.
In August 2012, Janssen Biotech, Inc. and Genmab A/S entered a worldwide agreement, which granted Janssen an exclusive license to develop, manufacture and commercialize daratumumab.
For more information, visit www.DARZALEX.com.
ABOUT TALVEY® TALVEY® (talquetamab-tgvs) received approval from the U.S. FDA in August 2023 as a first-in-class GPRC5D-targeting bispecific antibody for the treatment of adult patients with relapsed or refractory multiple myeloma who have received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 antibody.5 Since FDA approval, 7,700 patients were treated with TALVEY®. The European Commission (EC) granted conditional marketing authorization (CMA) of TALVEY®(talquetamab-tgvs) in August 2023 as monotherapy for the treatment of adult patients with relapsed and refractory multiple myeloma (RRMM) who have received at least three prior therapies, including an immunomodulatory agent, a proteasome inhibitor, and an anti-CD38 antibody and have demonstrated disease progression on the last therapy.6
TALVEY® is a bispecific T-cell engaging antibody that binds to the CD3 receptor expressed on the surface of T-cells and G protein-coupled receptor class C group 5 member D (GPRC5D), a novel multiple myeloma target which is highly expressed on the surface of multiple myeloma cells and non-malignant plasma cells, as well as some healthy tissues such as epithelial cells of the skin and tongue.
About CARVYKTI®CARVYKTI® (cilta-cel) received U.S. Food and Drug Administration approval in February 2022 for the treatment of adults with relapsed or refractory multiple myeloma after four or more prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 monoclonal antibody.7
In April 2024, CARVYKTI® was approved in the U.S. for treatment of adult patients with relapsed or refractory multiple myeloma who have received at least one prior line of therapy including a proteasome inhibitor, an immunomodulatory agent, and who are refractory to lenalidomide, following a unanimous (11 to 0) FDA Oncologic Drugs Advisory Committee (ODAC) recommendation in support of this new indication. In April 2024, the European Medicines Agency (EMA) approved a Type II variation for CARVYKTI® for the treatment of adults with relapsed and refractory multiple myeloma who have received at least one prior therapy, including an immunomodulatory agent and a proteasome inhibitor, have demonstrated disease progression on the last therapy, and are refractory to lenalidomide. In September 2022, Japan’s Ministry of Health, Labour and Welfare (MHLW) approved CARVYKTI® for the treatment of adults with relapsed or refractory multiple myeloma in patients that have no history of CAR-positive T cell infusion therapy targeting BCMA and who have received three or more lines of therapies, including an immunomodulatory agent, a proteasome inhibitor and an anti-CD38 monoclonal antibody, and in whom multiple myeloma has not responded to or has relapsed following the most recent therapy.
CARVYKTI® is a BCMA-directed, autologous T-cell immunotherapy, which involves reprogramming a patient’s own T-cells with a transgene encoding chimeric antigen receptor (CAR) that directs the CAR-positive T cells to eliminate cells that express BCMA. BCMA is primarily expressed on the surface of malignant multiple myeloma B-lineage cells, as well as late-stage B cells and plasma cells. The CARVYKTI® CAR protein features two BCMA-targeting single domains designed to confer high avidity against human BCMA. Upon binding to BCMA-expressing cells, the CAR promotes T-cell activation, expansion, and elimination of target cells. CARVYKTI® is available in 17 markets worldwide and has been used to treat more than 11,000 patients globally.
In December 2017, Janssen Biotech, Inc., a Johnson & Johnson company, entered into an exclusive worldwide license and collaboration agreement with Legend Biotech USA, Inc. to develop and commercialize CARVYKTI®.
For more information, visit www.CARVYKTI.com.
About RYBREVANT FASPRO™ and RYBREVANT®In December 2025, the U.S. FDA approved RYBREVANT FASPRO™ (amivantamab and hyaluronidase-lpuj) across all indications of intravenous RYBREVANT® (amivantamab-vmjw).This subcutaneously administered therapy is also approved in Europe, Japan, China, and other markets.8,9
RYBREVANT FASPRO™ is co-formulated with recombinant human hyaluronidase PH20 (rHuPH20), Halozyme’s ENHANZE® drug delivery technology.
The effectiveness of RYBREVANT FASPRO™ has been established based on adequate and well controlled studies of RYBREVANT®. Data across multiple Phase 3 studies, including MARIPOSA, have demonstrated the clinical benefit of RYBREVANT® in improving progression-free survival (PFS) and overall survival (OS) in advanced EGFR-mutated non-small cell lung cancer (NSCLC).
RYBREVANT® is approved in the U.S., Europe and other markets across four indications in EGFR-mutated NSCLC, including two in the first-line setting and two in the second-line, for patients with either exon 19 deletions, exon 21 L858R mutations, or exon 20 insertion mutations, as monotherapy or in combination with LAZCLUZE® (lazertinib) or chemotherapy.
RYBREVANT® is a first-in-class, fully-human bispecific antibody targeting EGFR and MET with immune cell-directing activity.
The legal manufacturer for RYBREVANT® is Janssen Biotech, Inc. For more information, visit: https://www.RYBREVANT.com.
About LAZCLUZE®
In 2018, Janssen Biotech, Inc., entered into a license and collaboration agreement with Yuhan Corporation for the development of LAZCLUZE® (marketed as LECLAZA in South Korea). LAZCLUZE® is an oral, third-generation, brain-penetrant EGFR TKI that targets both the T790M mutation and activating EGFR mutations while sparing wild-type EGFR. An analysis of the efficacy and safety of LAZCLUZE® from the Phase 3 LASER301 study was published in The Journal of Clinical Oncology in 2023.10,11
ERLEADA® INDICATIONS AND IMPORTANT SAFETY INFORMATION
INDICATIONS
ERLEADA® (apalutamide) is an androgen receptor inhibitor indicated for the treatment of patients with:
· Metastatic castration-sensitive prostate cancer (mCSPC)· Non-metastatic castration-resistant prostate cancer (nmCRPC)
IMPORTANT SAFETY INFORMATION
WARNINGS AND PRECAUTIONS
Cerebrovascular and Ischemic Cardiovascular Events,including events leading to death, occurred in patients receiving ERLEADA. Monitor for signs and symptoms of ischemic heart disease and cerebrovascular disorders. Optimize management of cardiovascular risk factors, such as hypertension, diabetes, or dyslipidemia. Consider discontinuation of ERLEADA for Grade 3 and 4 events.
In a randomized study (SPARTAN) of patients with nmCRPC, ischemic cardiovascular events occurred in 3.7% of patients treated with ERLEADA and 2% of patients treated with placebo. In a randomized study (TITAN) in patients with mCSPC, ischemic cardiovascular events occurred in 4.4% of patients treated with ERLEADA and 1.5% of patients treated with placebo. Across the SPARTAN and TITAN studies, 4 patients (0.3%) treated with ERLEADA and 2 patients (0.2%) treated with placebo died from an ischemic cardiovascular event. Patients with history of unstable angina, myocardial infarction, congestive heart failure, stroke, or transient ischemic attack within 6 months of randomization were excluded from the SPARTAN and TITAN studies.
In the SPARTAN study, cerebrovascular events occurred in 2.5% of patients treated with ERLEADA and 1% of patients treated with placebo. In the TITAN study, cerebrovascular events occurred in 1.9% of patients treated with ERLEADA and 2.1% of patients treated with placebo. Across the SPARTAN and TITAN studies, 3 patients (0.2%) treated with ERLEADA and 2 patients (0.2%) treated with placebo died from a cerebrovascular event.
Fractures occurred in patients receiving ERLEADA. Evaluate patients for fracture risk. Monitor and manage patients at risk for fractures according to established treatment guidelines and consider use of bone-targeted agents.
In a randomized study (SPARTAN) of patients with nmCRPC, fractures occurred in 12% of patients treated with ERLEADA and in 7% of patients treated with placebo. In a randomized study (TITAN) of patients with mCSPC, fractures occurred in 9% of patients treated with ERLEADA and in 6% of patients treated with placebo.
Falls occurred in patients receiving ERLEADA with increased frequency in the elderly. Evaluate patients for fall risk.
In a randomized study (SPARTAN), falls occurred in 16% of patients treated with ERLEADA compared with 9% of patients treated with placebo. Falls were not associated with loss of consciousness or seizure.
Seizure occurred in patients receiving ERLEADA. Permanently discontinue ERLEADA in patients who develop a seizure during treatment. It is unknown whether anti-epileptic medications will prevent seizures with ERLEADA. Advise patients of the risk of developing a seizure while receiving ERLEADA and of engaging in any activity where sudden loss of consciousness could cause harm to themselves or others.
In two randomized studies (SPARTAN and TITAN), five patients (0.4%) treated with ERLEADA and one patient treated with placebo (0.1%) experienced a seizure. Seizure occurred from 159 to 650 days after initiation of ERLEADA. Patients with a history of seizure or, predisposing factors for seizure, or receiving drugs known to decrease the seizure threshold or to induce seizure were excluded. There is no clinical experience in re-administering ERLEADA to patients who experienced a seizure.
Severe Cutaneous Adverse Reactions — Fatal and life-threatening cases of severe cutaneous adverse reactions (SCARs), including Stevens‑Johnson syndrome/toxic epidermal necrolysis (SJS/TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS) occurred in patients receiving ERLEADA.
Monitor patients for the development of SCARs. Advise patients of the signs and symptoms of SCARs (eg, a prodrome of fever, flu-like symptoms, mucosal lesions, progressive skin rash, or lymphadenopathy). If a SCAR is suspected, interrupt ERLEADA until the etiology of the reaction has been determined. Consultation with a dermatologist is recommended. If a SCAR is confirmed, or for other Grade 4 skin reactions, permanently discontinue ERLEADA [see Dosage and Administration (2.2)].
Interstitial Lung Disease (ILD)/Pneumonitis — Fatal and life-threatening interstitial lung disease (ILD) or pneumonitis can occur in patients treated with ERLEADA.
Post-marketing cases of ILD/pneumonitis, including fatal cases, occurred in patients treated with ERLEADA. Across clinical trials (TITAN and SPARTAN, n=1327), 0.8% of patients treated with ERLEADA experienced ILD/pneumonitis, including 0.2% who experienced Grade 3 events [see Adverse Reactions (6.1, 6.2)].
Monitor patients for new or worsening symptoms indicative of ILD/pneumonitis (eg, dyspnea, cough, fever). Immediately withhold ERLEADA if ILD/pneumonitis is suspected.
Permanently discontinue ERLEADA in patients with severe ILD/pneumonitis or if no other potential causes of ILD/pneumonitis are identified [see Dosage and Administration (2.2)].
Embryo-Fetal Toxicity — The safety and efficacy of ERLEADA have not been established in females. Based on findings from animals and its mechanism of action, ERLEADA can cause fetal harm and loss of pregnancy when administered to a pregnant female. Advise males with female partners of reproductive potential to use effective contraception during treatment and for 3 months after the last dose of ERLEADA [see Use in Specific Populations (8.1, 8.3)].
ADVERSE REACTIONS
The most common adverse reactions (≥10%) that occurred more frequently in the ERLEADA-treated patients (≥2% over placebo) from the randomized placebo-controlled clinical trials (TITAN and SPARTAN) were fatigue, arthralgia, rash, decreased appetite, fall, weight decreased, hypertension, hot flush, diarrhea, and fracture.
Laboratory Abnormalities — All Grades (Grade 3-4)
Hematology — In the TITAN study: white blood cell decreased ERLEADA 27% (0.4%), placebo 19% (0.6%). In the SPARTAN study: anemia ERLEADA 70% (0.4%), placebo 64% (0.5%); leukopenia ERLEADA 47% (0.3%), placebo 29% (0%); lymphopenia ERLEADA 41% (1.8%), placebo 21% (1.6%) Chemistry — In the TITAN study: hypertriglyceridemia ERLEADA 17% (2.5%), placebo 12% (2.3%). In the SPARTAN study: hypercholesterolemia ERLEADA 76% (0.1%), placebo 46% (0%); hyperglycemia ERLEADA 70% (2%), placebo 59% (1.0%); hypertriglyceridemia ERLEADA 67% (1.6%), placebo 49% (0.8%); hyperkalemia ERLEADA 32% (1.9%), placebo 22% (0.5%)
Rash — In 2 randomized studies (SPARTAN and TITAN), rash was most commonly described as macular or maculopapular. Adverse reactions of rash were 26% with ERLEADA vs 8% with placebo. Grade 3 rashes (defined as covering >30% body surface area [BSA]) were reported with ERLEADA treatment (6%) vs placebo (0.5%).
The onset of rash occurred at a median of 83 days. Rash resolved in 78% of patients within a median of 78 days from onset of rash. Rash was commonly managed with oral antihistamines and topical corticosteroids, and 19% of patients received systemic corticosteroids. Dose reduction or dose interruption occurred in 14% and 28% of patients, respectively. Of the patients who had dose interruption, 59% experienced recurrence of rash upon reintroduction of ERLEADA.
Hypothyroidism — In 2 randomized studies (SPARTAN and TITAN), hypothyroidismwas reported for 8% of patients treated with ERLEADA and 1.5% of patients treated with placebo based on assessments of thyroid-stimulating hormone (TSH) every 4 months. Elevated TSH occurred in 25% of patients treated with ERLEADA and 7% of patients treated with placebo. The median onset was at the first scheduled assessment. There were no Grade 3 or 4 adverse reactions. Thyroid replacement therapy, when clinically indicated, should be initiated or dose adjusted.
DRUG INTERACTIONS
Effect of Other Drugs on ERLEADA
ERLEADA Strong CYP2C8 or CYP3A4 Inhibitors
Reduce the ERLEADA dose as recommended for adverse reactions [see Dosage and Administration (2.2)]. Co-administration of a strong CYP2C8 or CYP3A4 inhibitor is predicted to increase the steady‑state exposure of the active moieties (sum of unbound apalutamide plus the potency‑adjusted unbound N-desmethyl-apalutamide).
Effect of ERLEADA on Other Drugs
Substrates of CYP3A4, CYP2C9, CYP2C19, P-gp, BCRP, or OATP1B1
Refer to the Prescribing Information for these substrates. Consider alternative agents when possible or evaluate for loss of activity of the substrate if concomitant use cannot be avoided.
Apalutamide is a strong inducer of CYP3A4 and CYP2C19, a weak inducer of CYP2C9, and an inducer of P-gp, BCRP, and OATP1B1. Apalutamide decreases exposure of substrates of CYP3A4, CYP2C19, CYP2C9, P-gp, BCRP, or OATP1B [see Clinical Pharmacology (12.3)], which may decrease the effectiveness of these substrates.
USE IN SPECIFIC POPULATIONS
The recommended ERLEADA dosage in patients with (Child-Pugh C) is lower than the recommended dosage in patients with normal hepatic function. No dosage modification is recommended for patients with mild (Child-Pugh A) or moderate (Child-Pugh B) hepatic impairment.
Please see full Prescribing Information for ERLEADA.
TECVAYLI® INDICATIONS AND IMPORTANT SAFETY INFORMATION
INDICATIONS AND USAGE
TECVAYLI® (teclistamab-cqyv) is a bispecific B-cell maturation antigen (BCMA)-directed CD3 T-cell engager indicated for the treatment of adult patients with relapsed or refractory multiple myeloma:
· in combination with daratumumab and hyaluronidase-fihj in patients who have received at least one prior line of therapy, including a proteasome inhibitor and an immunomodulatory agent.· as monotherapy, in patients who have received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent and an anti-CD38 monoclonal antibody.
IMPORTANT SAFETY INFORMATION
WARNINGS AND PRECAUTIONS
Cytokine Release Syndrome - TECVAYLIcan cause cytokine release syndrome (CRS), including life-threatening or fatal reactions.
In the clinical trials (monotherapy and combination therapy; N=448), CRS occurred in 64% of patients who received TECVAYLI at the recommended dose, with Grade 1 CRS occurring in 46% of patients, Grade 2 in 18%, and Grade 3 in 0.2%. Recurrent CRS occurred in 27% of patients. Most patients experienced CRS during the initial step-up dosing schedule (step-up dose 1 [37%], step-up dose 2 [32%], or the initial treatment dose [20%]). CRS first occurred following subsequent doses of TECVAYLI in 2.5% of patients. The median time to onset of CRS was 2 (range: 1 to 9) days after the most recent dose and the median duration of CRS was 2 (range: 1 to 22) days.
Clinical signs and symptoms of CRS included, but were not limited to, fever, hypoxia, chills, hypotension, sinus tachycardia, headache, and elevated liver enzymes (aspartate aminotransferase and alanine aminotransferase elevation).
Initiate therapy according to TECVAYLI step-up dosing schedule to reduce risk of CRS. Administer pretreatment medications to reduce risk of CRS and monitor patients following administration of TECVAYLI accordingly.
At the first sign of CRS, immediately evaluate patient for hospitalization. Administer supportive care based on severity and consider further management per current practice guidelines. Withhold until CRS resolves or permanently discontinue TECVAYLI based on severity.
TECVAYLI is available only through a restricted program under a REMS.
Neurologic Toxicity including Immune Effector Cell-Associated Neurotoxicity Syndrome - TECVAYLI can cause serious, life-threatening, or fatal neurologic toxicity, including immune effector cell-associated neurotoxicity syndrome (ICANS).
In the clinical trials (monotherapy and combination therapy trials; N=448), neurologic toxicity occurred in 60% of patients who received TECVAYLI at the recommended dosage, with Grade 3 or 4 neurologic toxicity in 6%. Neurologic toxicities reported in ≥5% of patients included headache (27%), sensory neuropathy (16%), motor dysfunction (15%), insomnia (12%), encephalopathy (11%), and dizziness (8%). Fatal neurologic toxicity occurred in 0.4% of patients, including Guillain-Barré syndrome and status epilepticus (one patient each).
In MajesTEC-1, ICANS was reported in 6% of patients who received TECVAYLI as monotherapy at the recommended dosage. Recurrent ICANS occurred in 1.8% of patients. Most patients experienced ICANS following step-up dose 1 (1.2%), step-up dose 2 (0.6%), or the initial treatment dose (1.8%). Less than 3% of patients developed first occurrence of ICANS following subsequent TECVAYLI doses. The median time to onset of ICANS was 4 (range: 2 to 8) days after the most recent dose with a median duration of 3 (range: 1 to 20) days. The most frequent clinical manifestations of ICANS reported were confusional state and dysgraphia.
In MajesTEC-3, ICANS was reported in 1.1% of patients who received the recommended TECVAYLI dosage in combination with daratumumab and hyaluronidase-fihj, including Grade 4 ICANS in 1 patient. All events of ICANS occurred during the step-up dosing schedule. The median time to onset of ICANS was 2 (range: 1 to 3) days after the most recent dose and the median duration of ICANS was 2 (range: 1 to 2) days. The clinical manifestations of ICANS reported were amnesia, encephalopathy and delirium.
The onset of ICANS can be concurrent with CRS, following resolution of CRS, or in the absence of CRS.
Monitor patients for signs and symptoms of neurologic toxicity, including ICANS during TECVAYLI treatment. At the first sign of neurologic toxicity, including ICANS, immediately evaluate patient and provide supportive therapy based on severity. Withhold until neurologic toxicity resolves or permanently discontinue TECVAYLI based on severity per recommendations and consider further management per current practice guidelines.
Due to the potential for neurologic toxicity, patients receiving TECVAYLI are at risk of depressed level of consciousness. Advise patients to refrain from driving or operating heavy or potentially dangerous machinery during and for 48 hours after completion of TECVAYLI step-up dosing schedule and in the event of new onset of any neurologic toxicity symptoms until neurologic toxicity resolves.
TECVAYLI is available only through a restricted program under a REMS.
TECVAYLI and TALVEY REMS - TECVAYLI is available only through a restricted program under a REMS called the TECVAYLI and TALVEY REMS because of the risks of CRS and neurologic toxicity, including ICANS.
Hepatotoxicity - TECVAYLI can cause hepatotoxicity, including fatalities. There was one fatal case of hepatic failure in MajesTEC-1. In patients who received TECVAYLI at the recommended dose in the clinical trials (monotherapy and combination therapy trials; N=448) elevated aspartate aminotransferase (AST) occurred in 47% of patients, with Grade 3 or 4 elevations in 2.9%. Elevated alanine aminotransferase (ALT) occurred in 48% of patients, with Grade 3 or 4 elevations in 3.8%. Elevated total bilirubin occurred in 10% of patients with Grade 3 or 4 elevations in 0.7%. Liver enzyme elevation can occur with or without concurrent CRS.
Monitor liver enzymes and bilirubin at baseline and during treatment as clinically indicated. Withhold TECVAYLI or consider permanent discontinuation of TECVAYLI based on severity.
Infections - TECVAYLI can cause severe, life-threatening, or fatal infections.
In MajesTEC-1 (N=165), in patients who received the recommended TECVAYLI dosage, serious infections, including opportunistic infections, occurred in 30% of patients, Grade 3 or 4 infections in 35% of patients, and fatal infections in 4.2% of patients.
In MajesTEC-3 (N=283), in patients who received TECVAYLI in combination with daratumumab and hyaluronidase-fihj at the recommended dosage, serious infections, including opportunistic infections, occurred in 54% of patients, Grade 3 or Grade 4 infections in 54% of patients, and fatal infections in 4.6% of patients.
Monitor patients for signs and symptoms of infection prior to and during treatment with TECVAYLI and treat appropriately. Administer prophylactic antimicrobials according to current practice guidelines.
Withhold TECVAYLI or consider permanent discontinuation of TECVAYLI based on severity.
Monitor immunoglobulin levels prior to and during treatment with TECVAYLI and administer subcutaneous or intravenous immunoglobulin (IVIG) to maintain the serum levels >400 mg/dL.
Neutropenia - TECVAYLI can cause neutropenia and febrile neutropenia. In patients who received TECVAYLI at the recommended dose in the clinical trials (monotherapy and combination therapy trials; N=448), decreased neutrophils occurred in 88% of patients, with Grade 3 or 4 decreased neutrophils in 70%. Febrile neutropenia occurred in 6% of patients.
Monitor complete blood cell counts at baseline and periodically during treatment and provide supportive care per local institutional guidelines.
Monitor patients with neutropenia for signs of infection.
Withhold TECVAYLI based on severity.
Hypersensitivity and Other Administration Reactions - TECVAYLI can cause both systemic administration-related and local injection-site reactions.
Systemic Reactions - In patients who received the recommended TECVAYLI dosage in the clinical trials (monotherapy and combination therapy trials; N=448), 2.5% of patients experienced systemic-administration reactions, which included recurrent pyrexia and rash.
Local Reactions - In patients who received TECVAYLI at the recommended dosage in the clinical trials (monotherapy and combination therapy trials; N=448), injection-site reactions occurred in 37% of patients, with Grade 1 injection-site reactions in 29% and Grade 2 in 9%.
Withhold TECVAYLI or consider permanent discontinuation of TECVAYLI based on severity.
Embryo-Fetal Toxicity - Based on its mechanism of action, TECVAYLI may cause fetal harm when administered to a pregnant patient. Advise pregnant patients of the potential risk to the fetus. Advise females of reproductive potential to use effective contraception during treatment with TECVAYLI and for 5 months after the last dose.
ADVERSE REACTIONSThe most common adverse reactions (≥20%) in patients who received TECVAYLI monotherapy were pyrexia, CRS, musculoskeletal pain, injection site reaction, fatigue, upper respiratory tract infection, nausea, headache, pneumonia, and diarrhea. The most common adverse reactions (≥20%) in patients who received TECVAYLI in combination with daratumumab and hyaluronidase-fihj were hypogammaglobulinemia, upper respiratory tract infection, CRS, cough, diarrhea, musculoskeletal pain, COVID-19, pneumonia, injection site reaction, fatigue, pyrexia, headache, nausea, gastroenteritis, and weight decreased.
The most common Grade 3 to 4 laboratory abnormalities (≥20%) with TECVAYLI (as monotherapy or in combination with daratumumab and hyaluronidase-fihj) were decreased lymphocytes, decreased neutrophils, decreased white blood cells, decreased hemoglobin, and decreased platelets.
Please read full Prescribing Information, including Boxed WARNING, for TECVAYLI.
DARZALEX FASPRO® INDICATIONS AND IMPORTANT SAFETY INFORMATION
INDICATIONSDARZALEX FASPRO® (daratumumab and hyaluronidase-fihj) is indicated for the treatment of adult patients with multiple myeloma:· In combination with bortezomib, lenalidomide, and dexamethasone for induction and consolidation in newly diagnosed patients who are eligible for autologous stem cell transplant· In combination with bortezomib, melphalan, and prednisone in newly diagnosed patients who are ineligible for autologous stem cell transplant· In combination with lenalidomide and dexamethasone in newly diagnosed patients who are ineligible for autologous stem cell transplant and in patients with relapsed or refractory multiple myeloma who have received at least one prior therapy· In combination with bortezomib, thalidomide, and dexamethasone in newly diagnosed patients who are eligible for autologous stem cell transplant· In combination with pomalidomide and dexamethasone in patients who have received at least one prior line of therapy including lenalidomide and a proteasome inhibitor (PI)· In combination with carfilzomib and dexamethasone in patients with relapsed or refractory multiple myeloma who have received one to three prior lines of therapy· In combination with bortezomib and dexamethasone in patients who have received at least one prior therapy· As monotherapy in patients who have received at least three prior lines of therapy including a PI and an immunomodulatory agent or who are double refractory to a PI and an immunomodulatory agent
DARZALEX FASPRO® as monotherapy is indicated for the treatment of adult patients with high-risk smoldering multiple myeloma.
IMPORTANT SAFETY INFORMATION
CONTRAINDICATIONS
DARZALEX FASPRO® is contraindicated in patients with a history of severe hypersensitivity to daratumumab, hyaluronidase, or any of the components of the formulation.
WARNINGS AND PRECAUTIONS
Hypersensitivity and Other Administration Reactions
Both systemic administration-related reactions, including severe or life-threatening reactions, and local injection-site reactions can occur with DARZALEX FASPRO®. Fatal reactions have been reported with daratumumab-containing products, including DARZALEX FASPRO®.
Systemic Reactions
In a pooled safety population of 1446 patients with multiple myeloma (N=1235) or light chain (AL) amyloidosis (N=193) who received DARZALEX FASPRO® as monotherapy or in combination, 7% of patients experienced a systemic administration-related reaction (Grade 2: 3%, Grade 3: 0.8%, Grade 4: 0.1%). In patients with high-risk smoldering multiple myeloma (N=193), systemic administration-related reactions occurred in 17% of patients in AQUILA (Grade 2: 7%, Grade 3: 1%).
In all patients (N=1639), systemic administration-related reactions occurred in 7% of patients with the first injection, 0.5% with the second injection, and cumulatively 1% with subsequent injections. The median time to onset was 3.2 hours (range: 4 minutes to 3.5 days). Of the 283 systemic administration-related reactions that occurred in 135 patients, 240 (85%) occurred on the day of DARZALEX FASPRO® administration. Delayed systemic administration-related reactions have occurred in 1% of the patients.
Severe reactions included hypoxia, dyspnea, hypertension, tachycardia, and ocular adverse reactions, including choroidal effusion, acute myopia, and acute angle closure glaucoma. Other signs and symptoms of systemic administration-related reactions may include respiratory symptoms, such as bronchospasm, nasal congestion, cough, throat irritation, allergic rhinitis, and wheezing, as well as anaphylactic reaction, pyrexia, chest pain, pruritus, chills, vomiting, nausea, hypotension, and blurred vision.
Pre-medicate patients with histamine-1 receptor antagonist, acetaminophen, and corticosteroids. Monitor patients for systemic administration-related reactions, especially following the first and second injections. For anaphylactic reaction or life-threatening (Grade 4) administration-related reactions, immediately and permanently discontinue DARZALEX FASPRO®. Consider administering corticosteroids and other medications after the administration of DARZALEX FASPRO® depending on dosing regimen and medical history to minimize the risk of delayed (defined as occurring the day after administration) systemic administration-related reactions.
Ocular adverse reactions, including acute myopia and narrowing of the anterior chamber angle due to ciliochoroidal effusions with potential for increased intraocular pressure or glaucoma, have occurred with daratumumab-containing products. If ocular symptoms occur, interrupt DARZALEX FASPRO® and seek immediate ophthalmologic evaluation prior to restarting DARZALEX FASPRO®.
Local Reactions
In this pooled safety population of 1446 patients with multiple myeloma (N=1253) or light chain amyloidosis (N=193), injection-site reactions occurred in 8% of patients, including Grade 2 reactions in 1.1%. The most frequent (>1%) injection-site reaction were injection site erythema and injection site rash. In patients with high-risk smoldering multiple myeloma (N=193), injection-site reactions occurred in 28% of patients, including Grade 2 reactions in 3%. These local reactions occurred a median of 6 minutes (range: 0 minutes to 6.5 days) after starting administration of DARZALEX FASPRO®. Monitor for local reactions and consider symptomatic management.
Infections
DARZALEX FASPRO® can cause serious, life-threatening, or fatal infections. In patients who received DARZALEX FASPRO® in a pooled safety population including patients with smoldering multiple myeloma and light chain (AL) amyloidosis (N=1639), serious infections, including opportunistic infections, occurred in 24% of patients, Grade 3 or 4 infections occurred in 22%, and fatal infections occurred in 2.5%. The most common type of serious infection reported was pneumonia (8.5%).
Monitor patients for signs and symptoms of infection prior to and during treatment with DARZALEX FASPRO® and treat appropriately. Administer prophylactic antimicrobials according to guidelines.
Neutropenia
Daratumumab may increase neutropenia induced by background therapy. Monitor complete blood cell counts periodically during treatment according to manufacturer’s prescribing information for background therapies. Monitor patients with neutropenia for signs of infection. Consider withholding DARZALEX FASPRO® until recovery of neutrophils. In lower body weight patients receiving DARZALEX FASPRO®, higher rates of Grade 3-4 neutropenia were observed.
Thrombocytopenia
Daratumumab may increase thrombocytopenia induced by background therapy. Monitor complete blood cell counts periodically during treatment according to manufacturer’s prescribing information for background therapies. Consider withholding DARZALEX FASPRO® until recovery of platelets.
Embryo-Fetal ToxicityBased on the mechanism of action, DARZALEX FASPRO® can cause fetal harm when administered to a pregnant woman. DARZALEX FASPRO® may cause depletion of fetal immune cells and decreased bone density. Advise pregnant women of the potential risk to a fetus. Advise females with reproductive potential to use effective contraception during treatment with DARZALEX FASPRO® and for 3 months after the last dose.
The combination of DARZALEX FASPRO® with lenalidomide, thalidomide, or pomalidomide is contraindicated in pregnant women because lenalidomide, thalidomide, and pomalidomide may cause birth defects and death of the unborn child. Refer to the lenalidomide, thalidomide, or pomalidomide prescribing information on use during pregnancy.
Interference With Serological Testing
Daratumumab binds to CD38 on red blood cells (RBCs) and results in a positive indirect antiglobulin test (indirect Coombs test). Daratumumab-mediated positive indirect antiglobulin test may persist for up to 6 months after the last daratumumab administration. Daratumumab bound to RBCs masks detection of antibodies to minor antigens in the patient’s serum. The determination of a patient’s ABO and Rh blood type are not impacted.
Notify blood transfusion centers of this interference with serological testing and inform blood banks that a patient has received DARZALEX FASPRO®. Type and screen patients prior to starting DARZALEX FASPRO®.
Interference With Determination of Complete Response
Daratumumab is a human immunoglobulin G (IgG) kappa monoclonal antibody that can be detected on both the serum protein electrophoresis (SPE) and immunofixation (IFE) assays used for the clinical monitoring of endogenous M-protein. This interference can impact the determination of complete response and of disease progression in some DARZALEX FASPRO®-treated patients with IgG kappa myeloma protein.
ADVERSE REACTIONS
In multiple myeloma, the most common adverse reaction (≥20%) with DARZALEX FASPRO® monotherapy is upper respiratory tract infection. The most common adverse reactions with combination therapy (≥20% for any combination) include fatigue, nausea, diarrhea, dyspnea, insomnia, headache, rash, pyrexia, cough, muscle spasms, back pain, vomiting, hypertension, musculoskeletal pain, upper respiratory tract infection, , peripheral neuropathy, peripheral sensory neuropathy, constipation, pneumonia, edema, peripheral edema, and anemia.
The most common adverse reactions (≥20%) in patients with high-risk smoldering multiple myeloma who received DARZALEX FASPRO® monotherapy are upper respiratory tract infection, musculoskeletal pain, fatigue, diarrhea, rash, sleep disorder, sensory neuropathy, and injection site reactions.
The most common hematology laboratory abnormalities (≥40%) with DARZALEX FASPRO® are decreased leukocytes, decreased lymphocytes, decreased neutrophils, decreased platelets, and decreased hemoglobin.
Please click here to read the full Prescribing Information for DARZALEX FASPRO®.
DARZALEX® INDICATIONS AND IMPORTANT SAFETY INFORMATION
INDICATIONS
DARZALEX® (daratumumab) is indicated for the treatment of adult patients with multiple myeloma:· In combination with bortezomib, melphalan, and prednisone in newly diagnosed patients who are ineligible for autologous stem cell transplant· In combination with lenalidomide and dexamethasone in newly diagnosed patients who are ineligible for autologous stem cell transplant and in patients with relapsed or refractory multiple myeloma who have received at least one prior therapy· In combination with bortezomib, thalidomide, and dexamethasone in newly diagnosed patients who are eligible for autologous stem cell transplant· In combination with pomalidomide and dexamethasone in patients who have received at least one prior line of therapy including lenalidomide and a proteasome inhibitor· In combination with carfilzomib and dexamethasone in patients with relapsed or refractory multiple myeloma who have received one to three prior lines of therapy· In combination with bortezomib and dexamethasone in patients who have received at least one prior therapy· As monotherapy in patients who have received at least three prior lines of therapy including a proteasome inhibitor (PI) and an immunomodulatory agent or who are double-refractory to a PI and an immunomodulatory agent
CONTRAINDICATIONS
DARZALEX® is contraindicated in patients with a history of severe hypersensitivity (eg, anaphylactic reactions) to daratumumab or any of the components of the formulation.
WARNINGS AND PRECAUTIONS
Infusion-Related Reactions
DARZALEX® can cause severe and/or serious infusion-related reactions including anaphylactic reactions. These reactions can be life threatening, and fatal outcomes have been reported. In clinical trials (monotherapy and combination: N=2066), infusion-related reactions occurred in 37% of patients with the Week 1 (16 mg/kg) infusion, 2% with the Week 2 infusion, and cumulatively 6% with subsequent infusions. Less than 1% of patients had a Grade 3/4 infusion-related reaction at Week 2 or subsequent infusions. The median time to onset was 1.5 hours (range: 0 to 73 hours). Nearly all reactions occurred during infusion or within 4 hours of completing DARZALEX®. Severe reactions have occurred, including bronchospasm, hypoxia, dyspnea, hypertension, tachycardia, headache, laryngeal edema, pulmonary edema, and ocular adverse reactions, including choroidal effusion, acute myopia, and acute angle closure glaucoma. Signs and symptoms may include respiratory symptoms, such as nasal congestion, cough, throat irritation, as well as chills, vomiting, and nausea. Less common signs and symptoms were wheezing, allergic rhinitis, pyrexia, chest discomfort, pruritus, hypotension and blurred vision.
When DARZALEX® dosing was interrupted in the setting of ASCT (CASSIOPEIA) for a median of 3.75 months (range: 2.4 to 6.9 months), upon re-initiation of DARZALEX®, the incidence of infusion-related reactions was 11% for the first infusion following ASCT. Infusion-related reactions occurring at re-initiation of DARZALEX® following ASCT were consistent in terms of symptoms and severity (Grade 3 or 4: <1%) with those reported in previous studies at Week 2 or subsequent infusions. In EQUULEUS, patients receiving combination treatment (n=97) were administered the first 16 mg/kg dose at Week 1 split over two days, ie, 8 mg/kg on Day 1 and Day 2, respectively. The incidence of any grade infusion-related reactions was 42%, with 36% of patients experiencing infusion-related reactions on Day 1 of Week 1, 4% on Day 2 of Week 1, and 8% with subsequent infusions.
Pre-medicate patients with antihistamines, antipyretics, and corticosteroids. Frequently monitor patients during the entire infusion. Interrupt DARZALEX® infusion for reactions of any severity and institute medical management as needed. Permanently discontinue DARZALEX® therapy if an anaphylactic reaction or life-threatening (Grade 4) reaction occurs and institute appropriate emergency care. For patients with Grade 1, 2, or 3 reactions, reduce the infusion rate when re-starting the infusion.
To reduce the risk of delayed infusion-related reactions, administer oral corticosteroids to all patients following DARZALEX® infusions. Patients with a history of chronic obstructive pulmonary disease may require additional post-infusion medications to manage respiratory complications. Consider prescribing short- and long-acting bronchodilators and inhaled corticosteroids for patients with chronic obstructive pulmonary disease.
Ocular adverse reactions, including acute myopia and narrowing of the anterior chamber angle due to ciliochoroidal effusions with potential for increased intraocular pressure or glaucoma, have occurred with DARZALEX® infusion. If ocular symptoms occur, interrupt DARZALEX® infusion and seek immediate ophthalmologic evaluation prior to restarting DARZALEX®.
Interference With Serological Testing
Daratumumab binds to CD38 on red blood cells (RBCs) and results in a positive indirect antiglobulin test (indirect Coombs test). Daratumumab-mediated positive indirect antiglobulin test may persist for up to 6 months after the last daratumumab infusion. Daratumumab bound to RBCs masks detection of antibodies to minor antigens in the patient’s serum. The determination of a patient’s ABO and Rh blood type is not impacted. Notify blood transfusion centers of this interference with serological testing and inform blood banks that a patient has received DARZALEX®. Type and screen patients prior to starting DARZALEX®.
Neutropenia and Thrombocytopenia
DARZALEX® may increase neutropenia and thrombocytopenia induced by background therapy. Monitor complete blood cell counts periodically during treatment according to manufacturer’s prescribing information for background therapies. Monitor patients with neutropenia for signs of infection. Consider withholding DARZALEX® until recovery of neutrophils or for recovery of platelets.
Interference With Determination of Complete Response
Daratumumab is a human immunoglobulin G (IgG) kappa monoclonal antibody that can be detected on both the serum protein electrophoresis (SPE) and immunofixation (IFE) assays used for the clinical monitoring of endogenous M-protein. This interference can impact the determination of complete response and of disease progression in some patients with IgG kappa myeloma protein.
Embryo-Fetal Toxicity
Based on the mechanism of action, DARZALEX® can cause fetal harm when administered to a pregnant woman. DARZALEX® may cause depletion of fetal immune cells and decreased bone density. Advise pregnant women of the potential risk to a fetus. Advise females with reproductive potential to use effective contraception during treatment with DARZALEX® and for 3 months after the last dose
The combination of DARZALEX® with lenalidomide, pomalidomide, or thalidomide is contraindicated in pregnant women because lenalidomide, pomalidomide, and thalidomide may cause birth defects and death of the unborn child. Refer to the lenalidomide, pomalidomide, or thalidomide prescribing information on use during pregnancy.
ADVERSE REACTIONS
The most frequently reported adverse reactions (incidence ≥20%) were: upper respiratory infection, neutropenia, infusion related reactions, thrombocytopenia, diarrhea, constipation, anemia, peripheral sensory neuropathy, fatigue, peripheral edema, nausea, cough, pyrexia, dyspnea, and asthenia. The most common hematologic laboratory abnormalities (≥40%) with DARZALEX® are: neutropenia, lymphopenia, thrombocytopenia, leukopenia, and anemia.
Please click here to read the full Prescribing Information for DARZALEX®.
TALVEY® IMPORTANT SAFETY INFORMATION
INDICATION AND USAGE
TALVEY® (talquetamab-tgvs) is indicated for the treatment of adult patients with relapsed or refractory multiple myeloma who have received at least four prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 monoclonal antibody.
This indication is approved under accelerated approval based on response rate and durability of response. Continued approval for this indication may be contingent upon verification and description of clinical benefit in a confirmatory trial(s).
IMPORTANT SAFETY INFORMATION
WARNING: CYTOKINE RELEASE SYNDROME and NEUROLOGIC TOXICITY, including IMMUNE EFFECTOR CELL-ASSOCIATED NEUROTOXICITY SYNDROME
Cytokine release syndrome (CRS), including life-threatening or fatal reactions, can occur in patients receiving TALVEY®. Initiate TALVEY® treatment with step-up dosing to reduce the risk of CRS. Withhold TALVEY® until CRS resolves or permanently discontinue based on severity.
Neurologic toxicity, including immune effector cell-associated neurotoxicity syndrome (ICANS), and serious and life-threatening or fatal reactions, can occur with TALVEY®. Monitor patients for signs and symptoms of neurologic toxicity including ICANS during treatment and treat promptly. Withhold or permanently discontinue TALVEY® based on severity.
Because of the risk of CRS and neurologic toxicity, including ICANS, TALVEY® is available only through a restricted program called the TECVAYLI® and TALVEY® Risk Evaluation and Mitigation Strategy (REMS). CONTRAINDICATIONS: None.
WARNINGS AND PRECAUTIONS Cytokine Release Syndrome (CRS): TALVEY® can cause cytokine release syndrome, including life-threatening or fatal reactions. In the clinical trial, CRS occurred in 76% of patients who received TALVEY® at the recommended dosages, with Grade 1 CRS occurring in 57% of patients, Grade 2 in 17%, and Grade 3 in 1.5%. Recurrent CRS occurred in 30% of patients. Most events occurred following step-up dose 1 (29%) or step-up dose 2(44%) at the recommended dosages. CRS occurred in 33% of patients with step-up dose 3 in the biweekly dosing schedule (N=153). CRS occurred in 30% of patients with the first 0.4 mg/kg treatment dose and in 12% of patients treated with the first 0.8 mg/kg treatment dose. The CRS rate for both dosing schedules combined was less than 3% for each of the remaining doses in Cycle 1 and less than 3% cumulatively from Cycle 2 onward. The median time to onset of CRS was 27 (range: 0.1 to 167) hours from the last dose, and the median duration was 17 (range: 0 to 622) hours. Clinical signs and symptoms of CRS include but are not limited to pyrexia, hypotension, chills, hypoxia, headache, and tachycardia. Potentially life-threatening complications of CRS may include cardiac dysfunction, acute respiratory distress syndrome, neurologic toxicity, renal and/or hepatic failure, and disseminated intravascular coagulation (DIC).
Initiate therapy with step-up dosing and administer pre-treatment medications (corticosteroids, antihistamine, and antipyretics) prior to each dose of TALVEY® in the step-up dosing schedule to reduce the risk of CRS. Monitor patients following administration accordingly. In patients who experience CRS, pre-treatment medications should be administered prior to the next TALVEY® dose.
Counsel patients to seek medical attention should signs or symptoms of CRS occur. At the first sign of CRS, immediately evaluate patient for hospitalization and institute treatment with supportive care based on severity, and consider further management per current practice guidelines. Withhold TALVEY® until CRS resolves or permanently discontinue based on severity.
Neurologic Toxicity including ICANS: TALVEY® can cause serious, or life-threatening neurologic toxicity or fatal neurologic toxicity including immune effector cell-associated neurotoxicity syndrome (ICANS), including fatal reactions. In the clinical trial, neurologic toxicity, including ICANS, occurred in 55% of patients who received the recommended dosages, with Grade 3 or 4 neurologic toxicity occurring in 6% of patients. The most frequent neurologic toxicities were headache (20%), encephalopathy (15%), sensory neuropathy (14%), and motor dysfunction (10%).
ICANS was reported in 9% of 265 patients where ICANS was collected and who received the recommended dosages. Recurrent ICANS occurred in 3% of patients. Most patients experienced ICANS following step-up dose 1 (3%), step-up dose 2 (3%), step-up dose 3 of the biweekly dosing schedule (1.8%), or the initial treatment dose of the weekly dosing schedule (2.6%) (N=156) or the biweekly dosing schedule (3.7%) (N=109). The median time to onset of ICANS was 2.5 (range: 1 to 16) days after the most recent dose with a median duration of 2 (range: 1 to 22) days. The onset of ICANS can be concurrent with CRS, following resolution of CRS, or in the absence of CRS. Clinical signs and symptoms of ICANS may include but are not limited to confusional state, depressed level of consciousness, disorientation, somnolence, lethargy, and bradyphrenia.
Monitor patients for signs and symptoms of neurologic toxicity during treatment and treat promptly. At the first sign of neurologic toxicity, including ICANS, immediately evaluate the patient and provide supportive care based on severity. Withhold or permanently discontinue TALVEY® based on severity and consider further management per current practice guidelines [see Dosage and Administration (2.5)].
Due to the potential for neurologic toxicity, patients receiving TALVEY® are at risk of depressed level of consciousness. Advise patients to refrain from driving or operating heavy or potentially dangerous machinery during the step-up dosing schedule and for 48 hours after completion of the step-up dosing schedule, and in the event of new onset of any neurological symptoms, until symptoms resolve.
TECVAYLI® and TALVEY® REMS: TALVEY® is available only through a restricted program under a REMS, called the TECVAYLI® and TALVEY® REMS because of the risks of CRS and neurologic toxicity, including ICANS. Further information about the TECVAYLI® and TALVEY® REMS program is available at www.TEC-TALREMS.com or by telephone at 1-855-810-8064.
Oral Toxicity and Weight Loss: TALVEY® can cause oral toxicities, including dysgeusia, dry mouth, dysphagia, and stomatitis. In the clinical trial, 80% of patients had oral toxicity, with Grade 3 occurring in 2.1% of patients who received the recommended dosages. The most frequent oral toxicities were dysgeusia (49%), dry mouth (34%), dysphagia (23%), and ageusia (18%). The median time to onset of oral toxicity was 15 (range: 1 to 634) days, and the median time to resolution to baseline was 43 (1 to 530) days. Oral toxicity did not resolve to baseline in 65% of patients.
TALVEY® can cause weight loss. In the clinical trial, 62% of patients experienced weight loss, regardless of having an oral toxicity, including 29% of patients with Grade 2 (10% or greater) weight loss and 2.7% of patients with Grade 3 (20% or greater) weight loss. The median time to onset of Grade 2 or higher weight loss was 67 (range: 6 to 407) days, and the median time to resolution was 50 (range: 1 to 403) days. Weight loss did not resolve in 57% of patients who reported weight loss.
Monitor patients for signs and symptoms of oral toxicity. Counsel patients to seek medical attention should signs or symptoms of oral toxicity occur and provide supportive care as per current clinical practice, including consultation with a nutritionist. Monitor weight regularly during therapy. Evaluate clinically significant weight loss further. Withhold TALVEY® or permanently discontinue based on severity.
Infections: TALVEY® can cause infections, including life-threatening or fatal infections. Serious infections occurred in 16% of patients, with fatal infections in 1.5% of patients. Grade 3 or 4 infections occurred in 17% of patients. The most common serious infections reported were bacterial infection (8%), which included sepsis and COVID-19 (2.7%). Monitor patients for signs and symptoms of infection prior to and during treatment with TALVEY® and treat appropriately. Administer prophylactic antimicrobials according to local guidelines. Withhold or consider permanent discontinuation of TALVEY® as recommended, based on severity.
Cytopenias: TALVEY® can cause cytopenias, including neutropenia and thrombocytopenia. In the clinical trial, Grade 3 or 4 decreased neutrophils occurred in 35% of patients, and Grade 3 or 4 decreased platelets occurred in 22% of patients who received TALVEY®. The median time to onset for Grade 3 or 4 neutropenia was 22 (range: 1 to 312) days, and the median time to resolution to Grade 2 or lower was 8 (range: 1 to 79) days. The median time to onset for Grade 3 or 4 thrombocytopenia was 12 (range: 2 to 183) days, and the median time to resolution to Grade 2 or lower was 10 (range: 1 to 64) days. Monitor complete blood counts during treatment and withhold TALVEY® as recommended, based on severity.
Skin Toxicity: TALVEY® can cause serious skin reactions, including rash, maculo-papular rash, erythema, and erythematous rash. In the clinical trial, skin reactions occurred in 62% of patients, with Grade 3 skin reactions in 0.3%. The median time to onset was 25 (range: 1 to 630) days. The median time to improvement to Grade 1 or less was 33 days.
Monitor for skin toxicity, including rash progression. Consider early intervention and treatment to manage skin toxicity. Withhold TALVEY® as recommended based on severity.
Hepatotoxicity: TALVEY® can cause hepatotoxicity. Elevated ALT occurred in 33% of patients, with Grade 3 or 4 ALT elevation occurring in 2.7%; elevated AST occurred in 31% of patients, with Grade 3 or 4 AST elevation occurring in 3.3%. Grade 3 or 4 elevations of total bilirubin occurred in 0.3% of patients. Liver enzyme elevation can occur with or without concurrent CRS.
Monitor liver enzymes and bilirubin at baseline and during treatment as clinically indicated. Withhold TALVEY® or consider permanent discontinuation of TALVEY®, based on severity [see Dosage and Administration (2.5)].
Embryo-Fetal Toxicity: Based on its mechanism of action, TALVEY® may cause fetal harm when administered to a pregnant woman. Advise pregnant women of the potential risk to the fetus. Advise females of reproductive potential to use effective contraception during treatment with TALVEY® and for 3 months after the last dose.
Adverse Reactions: The most common adverse reactions (≥20%) are pyrexia, CRS, dysgeusia, nail disorder, musculoskeletal pain, skin disorder, rash, fatigue, weight decreased, dry mouth, xerosis, dysphagia, upper respiratory tract infection, diarrhea, hypotension, and headache.
The most common Grade 3 or 4 laboratory abnormalities (≥30%) are lymphocyte count decreased, neutrophil count decreased, white blood cell decreased, and hemoglobin decreased.
Please read full Prescribing Information, including Boxed WARNING, for TALVEY®.
CARVYKTI® IMPORTANT SAFETY INFORMATION
WARNING: CYTOKINE RELEASE SYNDROME, NEUROLOGIC TOXICITIES, HLH/MAS, PROLONGED and RECURRENT CYTOPENIA, and SECONDARY HEMATOLOGICAL MALIGNANCIES
Cytokine Release Syndrome (CRS), including fatal or life-threatening reactions, occurred in patients following treatment with CARVYKTI®. Do not administer CARVYKTI® to patients with active infection or inflammatory disorders. Treat severe or life-threatening CRS with tocilizumab or tocilizumab and corticosteroids.
Immune Effector Cell-associated Neurotoxicity Syndrome (ICANS), which may be fatal or life-threatening, occurred following treatment with CARVYKTI®, including before CRS onset, concurrently with CRS, after CRS resolution, or in the absence of CRS. Monitor for neurologic events after treatment with CARVYKTI®. Provide supportive care and/or corticosteroids as needed.
Parkinsonism and Guillain-Barré syndrome (GBS) and their associated complications resulting in fatal or life-threatening reactions have occurred following treatment with CARVYKTI®.
Hemophagocytic Lymphohistiocytosis/Macrophage Activation Syndrome (HLH/MAS), including fatal and life-threatening reactions, occurred in patients following treatment with CARVYKTI®. HLH/MAS can occur with CRS or neurologic toxicities.
Prolonged and/or recurrent cytopenias with bleeding and infection and requirement for stem cell transplantation for hematopoietic recovery occurred following treatment with CARVYKTI®.
Immune Effector Cell-associated Enterocolitis (IEC-EC), including fatal or life-threatening reactions, occurred following treatment with CARVYKTI®.
Secondary hematological malignancies, including myelodysplastic syndrome and acute myeloid leukemia, have occurred in patients following treatment with CARVYKTI®. T-cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T-cell immunotherapies, including CARVYKTI®.
WARNINGS AND PRECAUTIONS
INCREASED EARLY MORTALITY - In CARTITUDE-4, a (1:1) randomized controlled trial, there was a numerically higher percentage of early deaths in patients randomized to the CARVYKTI® treatment arm compared to the control arm. Among patients with deaths occurring within the first 10 months from randomization, a greater proportion (29/208; 14%) occurred in the CARVYKTI® arm compared to (25/211; 12%) in the control arm. Of the 29 deaths that occurred in the CARVYKTI® arm within the first 10 months of randomization, 10 deaths occurred prior to CARVYKTI® infusion, and 19 deaths occurred after CARVYKTI® infusion. Of the 10 deaths that occurred prior to CARVYKTI® infusion, all occurred due to disease progression, and none occurred due to adverse events. Of the 19 deaths that occurred after CARVYKTI® infusion, 3 occurred due to disease progression, and 16 occurred due to adverse events. The most common adverse events were due to infection (n=12).
CYTOKINE RELEASE SYNDROME (CRS),including fatal or life-threatening reactions, occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® for RRMM in the CARTITUDE-1 & -4 studies (N=285), CRS occurred in 84% (238/285), including ≥ Grade 3 CRS (ASTCT 2019) in 4% (11/285) of patients. Median time to onset of CRS, any grade, was 7 days (range: 1 to 23 days). CRS resolved in 82% with a median duration of 4 days (range: 1 to 97 days). The most common manifestations of CRS in all patients combined (≥10%) included fever (84%), hypotension (29%) and aspartate aminotransferase increased (11%). Serious events that may be associated with CRS include pyrexia, hemophagocytic lymphohistiocytosis, respiratory failure, disseminated intravascular coagulation, capillary leak syndrome, and supraventricular and ventricular tachycardia. CRS occurred in 78% of patients in CARTITUDE-4 (3% Grade 3 to 4) and in 95% of patients in CARTITUDE-1 (4% Grade 3 to 4).
Identify CRS based on clinical presentation. Evaluate for and treat other causes of fever, hypoxia, and hypotension. CRS has been reported to be associated with findings of HLH/MAS, and the physiology of the syndromes may overlap. HLH/MAS is a potentially life-threatening condition. In patients with progressive symptoms of CRS or refractory CRS despite treatment, evaluate for evidence of HLH/MAS.
Confirm that a minimum of 2 doses of tocilizumab are available prior to infusion of CARVYKTI®.
Of the 285 patients who received CARVYKTI® in clinical trials, 53% (150/285) patients received tocilizumab; 35% (100/285) received a single dose, while 18% (50/285) received more than 1 dose of tocilizumab. Overall, 14% (39/285) of patients received at least 1 dose of corticosteroids for treatment of CRS.
Monitor patients at least daily for 7 days following CARVYKTI® infusion for signs and symptoms of CRS. Monitor patients for signs or symptoms of CRS for at least 2 weeks after infusion. At the first sign of CRS, immediately institute treatment with supportive care, tocilizumab, or tocilizumab and corticosteroids.
Counsel patients to seek immediate medical attention should signs or symptoms of CRS occur at any time.
NEUROLOGIC TOXICITIES, which may be severe, life-threatening, or fatal, occurred following treatment with CARVYKTI®. Neurologic toxicities included ICANS, neurologic toxicity with signs and symptoms of Parkinsonism, GBS, immune mediated myelitis, peripheral neuropathies, and cranial nerve palsies. Counsel patients on the signs and symptoms of these neurologic toxicities, and on the delayed nature of onset of some of these toxicities. Instruct patients to seek immediate medical attention for further assessment and management if signs or symptoms of any of these neurologic toxicities occur at any time.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & 4 studies for RRMM, one or more neurologic toxicities occurred in 24% (69/285), including ≥ Grade 3 cases in 7% (19/285) of patients. Median time to onset was 10 days (range: 1 to 101) with 63/69 (91%) of cases developing by 30 days. Neurologic toxicities resolved in 72% (50/69) of patients with a median duration to resolution of 23 days (range: 1 to 544). Of patients developing neurotoxicity, 96% (66/69) also developed CRS. Subtypes of neurologic toxicities included ICANS in 13%, peripheral neuropathy in 7%, cranial nerve palsy in 7%, parkinsonism in 3%, and immune mediated myelitis in 0.4% of the patients.
Immune Effector Cell-Associated Neurotoxicity Syndrome (ICANS): Patients receiving CARVYKTI® may experience fatal or life-threatening ICANS following treatment with CARVYKTI®, including before CRS onset, concurrently with CRS, after CRS resolution, or in the absence of CRS.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, ICANS occurred in 13% (36/285), including Grade ≥3 in 2% (6/285) of the patients. Median time to onset of ICANS was 8 days (range: 1 to 28 days). ICANS resolved in 30 of 36 (83%) of patients, with a median time to resolution of 3 days (range: 1 to 143 days). Median duration of ICANS was 6 days (range: 1 to 1229 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff. Of patients with ICANS, 97% (35/36) had CRS. The onset of ICANS occurred during CRS in 69% of patients, before and after the onset of CRS in 14% of patients, respectively.
Immune Effector Cell-associated Neurotoxicity Syndrome occurred in 7% of patients in CARTITUDE-4 (0.5% Grade 3) and in 23% of patients in CARTITUDE-1 (3% Grade 3). The most frequent (≥2%) manifestations of ICANS included encephalopathy (12%), aphasia (4%), headache (3%), motor dysfunction (3%), ataxia (2%), and sleep disorder (2%).
Monitor patients at least daily for 7 days following CARVYKTI® infusion for signs and symptoms of ICANS. Rule out other causes of ICANS symptoms. Monitor patients for signs or symptoms of ICANS for at least 2 weeks after infusion and treat promptly. Neurologic toxicity should be managed with supportive care and/or corticosteroids as needed. Advise patients to avoid driving for at least 2 weeks following infusion.
Parkinsonism: Neurologic toxicity with parkinsonism has been reported in clinical trials of CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, parkinsonism occurred in 3% (8/285), including Grade ≥3 in 2% (5/285) of the patients. Median time to onset of parkinsonism was 56 days (range: 14 to 914 days). Parkinsonism resolved in 1 of 8 (13%) of patients with a median time to resolution of 523 days. Median duration of parkinsonism was 243.5 days (range: 62 to 720 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff. The onset of parkinsonism occurred after CRS for all patients and after ICANS for 6 patients.
Parkinsonism occurred in 1% of patients in CARTITUDE-4 (no Grade 3 to 4) and in 6% of patients in CARTITUDE-1 (4% Grade 3 to 4).
Manifestations of parkinsonism included movement disorders, cognitive impairment, and personality changes. Monitor patients for signs and symptoms of parkinsonism that may be delayed in onset and managed with supportive care measures. There is limited efficacy information with medications used for the treatment of Parkinson’s disease for the improvement or resolution of parkinsonism symptoms following CARVYKTI® treatment.
Guillain-Barré Syndrome: A fatal outcome following GBS occurred following treatment with CARVYKTI® despite treatment with intravenous immunoglobulins. Symptoms reported include those consistent with Miller-Fisher variant of GBS, encephalopathy, motor weakness, speech disturbances, and polyradiculoneuritis.
Monitor for GBS. Evaluate patients presenting with peripheral neuropathy for GBS. Consider treatment of GBS with supportive care measures and in conjunction with immunoglobulins and plasma exchange, depending on severity of GBS.
Immune Mediated Myelitis: Grade 3 myelitis occurred 25 days following treatment with CARVYKTI® in CARTITUDE-4 in a patient who received CARVYKTI® as subsequent therapy. Symptoms reported included hypoesthesia of the lower extremities and the lower abdomen with impaired sphincter control. Symptoms improved with the use of corticosteroids and intravenous immune globulin. Myelitis was ongoing at the time of death from other cause.
Peripheral Neuropathy occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, peripheral neuropathy occurred in 7% (21/285), including Grade ≥3 in 1% (3/285) of the patients. Median time to onset of peripheral neuropathy was 57 days (range: 1 to 914 days). Peripheral neuropathy resolved in 11 of 21 (52%) of patients with a median time to resolution of 58 days (range: 1 to 215 days). Median duration of peripheral neuropathy was 149.5 days (range: 1 to 692 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff.
Peripheral neuropathies occurred in 7% of patients in CARTITUDE-4 (0.5% Grade 3 to 4) and in 7% of patients in CARTITUDE-1 (2% Grade 3 to 4). Monitor patients for signs and symptoms of peripheral neuropathies. Patients who experience peripheral neuropathy may also experience cranial nerve palsies or GBS.
Cranial Nerve Palsies occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, cranial nerve palsies occurred in 7% (19/285), including Grade ≥3 in 1% (1/285) of the patients. Median time to onset of cranial nerve palsies was 21 days (range: 17 to 101 days). Cranial nerve palsies resolved in 17 of 19 (89%) of patients with a median time to resolution of 66 days (range: 1 to 209 days). Median duration of cranial nerve palsies was 70 days (range: 1 to 262 days) in all patients, including those with ongoing neurologic events at the time of death or data cutoff. Cranial nerve palsies occurred in 9% of patients in CARTITUDE-4 (1% Grade 3 to 4) and in 3% of patients in CARTITUDE-1 (1% Grade 3 to 4).
The most frequent cranial nerve affected was the 7th cranial nerve. Additionally, cranial nerves III, V, and VI have been reported to be affected.
Monitor patients for signs and symptoms of cranial nerve palsies. Consider management with systemic corticosteroids, depending on the severity and progression of signs and symptoms.
HEMOPHAGOCYTIC LYMPHOHISTIOCYTOSIS (HLH)/MACROPHAGE ACTIVATION SYNDROME (MAS): Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, HLH/MAS occurred in 1% (3/285) of patients. All events of HLH/MAS had onset within 99 days of receiving CARVYKTI®, with a median onset of 10 days (range: 8 to 99 days), and all occurred in the setting of ongoing or worsening CRS. The manifestations of HLH/MAS included hyperferritinemia, hypotension, hypoxia with diffuse alveolar damage, coagulopathy and hemorrhage, cytopenia, and multi-organ dysfunction, including renal dysfunction and respiratory failure.
Patients who develop HLH/MAS have an increased risk of severe bleeding. Monitor hematologic parameters in patients with HLH/MAS and transfuse per institutional guidelines. Fatal cases of HLH/MAS occurred following treatment with CARVYKTI®.
HLH is a life-threatening condition with a high mortality rate if not recognized and treated early. Treatment of HLH/MAS should be administered per institutional standards.
PROLONGED AND RECURRENT CYTOPENIAS: Patients may exhibit prolonged and recurrent cytopenias following lymphodepleting chemotherapy and CARVYKTI® infusion.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, Grade 3 or higher cytopenias not resolved by Day 30 following CARVYKTI® infusion occurred in 62% (176/285) of the patients and included thrombocytopenia 33% (94/285), neutropenia 27% (76/285), lymphopenia 24% (67/285), and anemia 2% (6/285). After Day 60 following CARVYKTI® infusion, 22%, 20%, 5%, and 6% of patients had a recurrence of Grade 3 or 4 lymphopenia, neutropenia, thrombocytopenia, and anemia, respectively, after initial recovery of their Grade 3 or 4 cytopenia. Seventy-seven percent (219/285) of patients had one, two, or three or more recurrences of Grade 3 or 4 cytopenias after initial recovery of Grade 3 or 4 cytopenia. Sixteen and 25 patients had Grade 3 or 4 neutropenia and thrombocytopenia, respectively, at the time of death.
Monitor blood counts prior to and after CARVYKTI® infusion. Manage cytopenias with growth factors and blood product transfusion support according to local institutional guidelines.
INFECTIONS: CARVYKTI® should not be administered to patients with active infection or inflammatory disorders. Severe, life-threatening, or fatal infections occurred in patients after CARVYKTI® infusion.
Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, infections occurred in 57% (163/285), including Grade ≥3 in 24% (69/285) of patients. Grade 3 or 4 infections with an unspecified pathogen occurred in 12%, viral infections in 6%, bacterial infections in 5%, and fungal infections in 1% of patients. Overall, 5% (13/285) of patients had Grade 5 infections, 2.5% of which were due to COVID-19. Patients treated with CARVYKTI® had an increased rate of fatal COVID-19 infections compared to the standard therapy arm.
Monitor patients for signs and symptoms of infection before and after CARVYKTI® infusion and treat patients appropriately. Administer prophylactic, pre-emptive, and/or therapeutic antimicrobials according to the standard institutional guidelines. Febrile neutropenia was observed in 5% of patients after CARVYKTI® infusion and may be concurrent with CRS. In the event of febrile neutropenia, evaluate for infection and manage with broad-spectrum antibiotics, fluids, and other supportive care, as medically indicated. Counsel patients on the importance of prevention measures. Follow institutional guidelines for the vaccination and management of immunocompromised patients with COVID-19.
Viral Reactivation: Hepatitis B virus (HBV) reactivation, in some cases resulting in fulminant hepatitis, hepatic failure, and death, can occur in patients with hypogammaglobulinemia. Perform screening for Cytomegalovirus (CMV), HBV, hepatitis C virus (HCV), and human immunodeficiency virus (HIV) or any other infectious agents if clinically indicated in accordance with clinical guidelines before collection of cells for manufacturing. Consider antiviral therapy to prevent viral reactivation per local institutional guidelines/clinical practice.
Reactivation of John Cunningham (JC) virus, leading to progressive multifocal leukoencephalopathy (PML), including cases with fatal outcomes, have been reported following treatment. Perform appropriate diagnostic evaluations in patients with neurological adverse events.
HYPOGAMMAGLOBULINEMIA: can occur in patients receiving treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, hypogammaglobulinemia adverse event was reported in 36% (102/285) of patients; laboratory IgG levels fell below 500 mg/dL after infusion in 93% (265/285) of patients. Hypogammaglobulinemia either as an adverse reaction or laboratory IgG level below 500 mg/dL after infusion occurred in 94% (267/285) of patients treated. Fifty-six percent (161/285) of patients received intravenous immunoglobulin (IVIG) post CARVYKTI® for either an adverse reaction or prophylaxis.
Monitor immunoglobulin levels after treatment with CARVYKTI® and administer IVIG for IgG <400 mg/dL. Manage per local institutional guidelines, including infection precautions and antibiotic or antiviral prophylaxis.
Use of Live Vaccines: The safety of immunization with live viral vaccines during or following CARVYKTI® treatment has not been studied. Vaccination with live virus vaccines is not recommended for at least 6 weeks prior to the start of lymphodepleting chemotherapy, during CARVYKTI® treatment, and until immune recovery following treatment with CARVYKTI®.
HYPERSENSITIVITY REACTIONS occurred following treatment with CARVYKTI®. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, hypersensitivity reactions occurred in 5% (13/285), all of which were ≤2 Grade. Manifestations of hypersensitivity reactions included flushing, chest discomfort, tachycardia, wheezing, tremor, burning sensation, non-cardiac chest pain, and pyrexia.
Serious hypersensitivity reactions, including anaphylaxis, may be due to the dimethyl sulfoxide (DMSO) in CARVYKTI®. Patients should be carefully monitored for 2 hours after infusion for signs and symptoms of severe reaction. Treat promptly and manage patients appropriately according to the severity of the hypersensitivity reaction.
IMMUNE EFFECTOR CELL-ASSOCIATED ENTERCOLITIS (IEC-EC) has occurred in patients treated with CARVYKTI®. Manifestations include severe or prolonged diarrhea, abdominal pain, and weight loss requiring parenteral nutrition. IEC-EC has been associated with fatal outcome from perforation or sepsis. Manage according to institutional guidelines, including referral to gastroenterology and infectious disease specialists.
In cases of refractory IEC-EC, consider additional workup to exclude alternative etiologies, including T-cell lymphoma of the GI tract, which has been reported in the post marketing setting.
SECONDARY MALIGNANCIES: Patients treated with CARVYKTI® may develop secondary malignancies. Among patients receiving CARVYKTI® in the CARTITUDE-1 & -4 studies, myeloid neoplasms occurred in 5% (13/285) of patients (9 cases of myelodysplastic syndrome, 3 cases of acute myeloid leukemia, and 1 case of myelodysplastic syndrome followed by acute myeloid leukemia). The median time to onset of myeloid neoplasms was 447 days (range: 56 to 870 days) after treatment with CARVYKTI®. Ten of these 13 patients died following the development of myeloid neoplasms; 2 of the 13 cases of myeloid neoplasm occurred after initiation of subsequent antimyeloma therapy. Cases of myelodysplastic syndrome and acute myeloid leukemia have also been reported in the post marketing setting. T-cell malignancies have occurred following treatment of hematologic malignancies with BCMA- and CD19-directed genetically modified autologous T-cell immunotherapies, including CARVYKTI®. Mature T-cell malignancies, including CAR-positive tumors, may present as soon as weeks following infusions, and may include fatal outcomes.
Monitor lifelong for secondary malignancies. In the event that a secondary malignancy occurs, contact Janssen Biotech, Inc., at 1-800-526-7736 for reporting and to obtain instructions on collection of patient samples.
ADVERSE REACTIONS
The most common nonlaboratory adverse reactions (incidence greater than 20%) are pyrexia, cytokine release syndrome, hypogammaglobulinemia, hypotension, musculoskeletal pain, fatigue, infections-pathogen unspecified, cough, chills, diarrhea, nausea, encephalopathy, decreased appetite, upper respiratory tract infection, headache, tachycardia, dizziness, dyspnea, edema, viral infections, coagulopathy, constipation, and vomiting. The most common Grade 3 or 4 laboratory adverse reactions (incidence greater than or equal to 50%) include lymphopenia, neutropenia, white blood cell decreased, thrombocytopenia, and anemia.
Please read full Prescribing Information, including Boxed Warning, for CARVYKTI®.
RYBREVANT FASPRO™ AND RYBREVANT® INDICATIONS AND IMPORTANT SAFETY INFORMATION
INDICATIONS
RYBREVANT FASPRO™ (amivantamab and hyaluronidase-lpuj) and RYBREVANT® (amivantamab-vmjw) are indicated:· in combination with LAZCLUZE® (lazertinib) for the first-line treatment of adult patients with locally advanced or metastatic NSCLC with EGFR exon 19 deletions or exon 21 L858R substitution mutations, as detected by an FDA-approved test.· in combination with carboplatin and pemetrexed for the treatment of adult patients with locally advanced or metastatic NSCLC with EGFR exon 19 deletions or exon 21 L858R substitution mutations, whose disease has progressed on or after treatment with an EGFR tyrosine kinase inhibitor.· in combination with carboplatin and pemetrexed for the first-line treatment of adult patients with locally advanced or metastatic NSCLC with EGFR exon 20 insertion mutations, as detected by an FDA-approved test.· as a single agent for the treatment of adult patients with locally advanced or metastatic NSCLC with EGFR exon 20 insertion mutations, as detected by an FDA approved test, whose disease has progressed on or after platinum-based chemotherapy.
IMPORTANT SAFETY INFORMATION
CONTRAINDICATIONS
RYBREVANT FASPRO™ is contraindicated in patients with known hypersensitivity to hyaluronidase or to any of its excipients.
WARNINGS AND PRECAUTIONS
Hypersensitivity and Administration-Related Reactions with RYBREVANT FASPRO™
RYBREVANT FASPRO™ can cause hypersensitivity and administration-related reactions (ARRs); signs and symptoms of ARR include dyspnea, flushing, fever, chills, chest discomfort, hypotension, and vomiting. The median time to ARR onset is approximately 2 hours.
RYBREVANT FASPRO™ with LAZCLUZE®
In PALOMA-3 (n=206), all Grade ARRs occurred in 13% of patients, including 0.5% Grade 3. Of the patients who experienced ARRs, 89% occurred with the initial dose (Week 1, Day 1).
Premedicate with antihistamines, antipyretics, and glucocorticoids and administer RYBREVANT FASPRO™ as recommended. Monitor patients for any signs and symptoms of administration-related reactions during injection in a setting where cardiopulmonary resuscitation medication and equipment are available. Interrupt RYBREVANT FASPRO™ injection if ARR is suspected. Resume treatment upon resolution of symptoms or permanently discontinue RYBREVANT FASPRO™ based on severity.
Infusion-Related Reactions with RYBREVANT®
RYBREVANT® can cause infusion-related reactions (IRR) including anaphylaxis; signs and symptoms of IRR include dyspnea, flushing, fever, chills, nausea, chest discomfort, hypotension, and vomiting. The median time to IRR onset is approximately 1 hour.
RYBREVANT® with LAZCLUZE®
In MARIPOSA (n=421), IRRs occurred in 63% of patients, including Grade 3 in 5% and Grade 4 in 1% of patients. IRR-related infusion modifications occurred in 54%, dose reduction in 0.7%, and permanent discontinuation of RYBREVANT® in 4.5% of patients.
RYBREVANT® with Carboplatin and Pemetrexed
Based on the pooled safety population (n=281), IRRs occurred in 50% of patients including Grade 3 (3.2%) adverse reactions. IRR-related infusion modifications occurred in 46%, and permanent discontinuation of RYBREVANT® in 2.8% of patients.
RYBREVANT® as a Single Agent
In CHRYSALIS (n=302), IRRs occurred in 66% of patients. IRRs occurred in 65% of patients on Week 1 Day 1, 3.4% on Day 2 infusion, 0.4% with Week 2 infusion, and were cumulatively 1.1% with subsequent infusions. 97% were Grade 1-2, 2.2% were Grade 3, and 0.4% were Grade 4. The median time to onset was 1 hour (range: 0.1 to 18 hours) after start of infusion. IRR-related infusion modifications occurred in 62%, and permanent discontinuation of RYBREVANT® in 1.3% of patients.
Premedicate with antihistamines, antipyretics, and glucocorticoids and infuse RYBREVANT® as recommended. Administer RYBREVANT® via a peripheral line on Week 1 and Week 2 to reduce the risk of IRRs. Monitor patients for signs and symptoms of IRRs in a setting where cardiopulmonary resuscitation medication and equipment are available. Interrupt infusion if IRR is suspected. Reduce the infusion rate or permanently discontinue RYBREVANT® based on severity. If an anaphylactic reaction occurs, permanently discontinue RYBREVANT®.
Interstitial Lung Disease/Pneumonitis
RYBREVANT FASPRO™ and RYBREVANT® can cause severe and fatal interstitial lung disease (ILD)/pneumonitis.
RYBREVANT FASPRO™ with LAZCLUZE®
In PALOMA-3, ILD/pneumonitis occurred in 6% of patients, including Grade 3 in 1%, Grade 4 in 1.5%, and fatal cases in 1.9% of patients. 5% of patients permanently discontinued RYBREVANT FASPRO™ and LAZCLUZE® due to ILD/pneumonitis.
RYBREVANT® with LAZCLUZE®
In MARIPOSA, ILD/pneumonitis occurred in 3.1% of patients, including Grade 3 in 1.0% and Grade 4 in 0.2% of patients. There was one fatal case of ILD/pneumonitis and 2.9% of patients permanently discontinued RYBREVANT® and LAZCLUZE® due to ILD/pneumonitis.
RYBREVANT® with Carboplatin and Pemetrexed
Based on the pooled safety population, ILD/pneumonitis occurred in 2.1% of patients with 1.8% of patients experiencing Grade 3 ILD/pneumonitis. 2.1% discontinued RYBREVANT® due to ILD/pneumonitis.
RYBREVANT® as a Single Agent
In CHRYSALIS, ILD/pneumonitis occurred in 3.3% of patients, with 0.7% of patients experiencing Grade 3 ILD/pneumonitis. Three patients (1%) permanently discontinued RYBREVANT® due to ILD/pneumonitis.
Monitor patients for new or worsening symptoms indicative of ILD/pneumonitis (e.g., dyspnea, cough, fever). Immediately withhold RYBREVANT FASPRO™ or RYBREVANT® and LAZCLUZE® (when applicable) in patients with suspected ILD/pneumonitis and permanently discontinue if ILD/pneumonitis is confirmed.
Venous Thromboembolic (VTE) Events with Concomitant Use with LAZCLUZE®
RYBREVANT FASPRO™ and RYBREVANT® in combination with LAZCLUZE® can cause serious and fatal venous thromboembolic (VTE) events, including deep vein thrombosis and pulmonary embolism. Without prophylactic anticoagulation, the majority of these events occurred during the first four months of treatment.
RYBREVANT FASPRO™ with LAZCLUZE®
In PALOMA-3 (n=206), all Grade VTE occurred in 11% of patients and 1.5% were Grade 3. 80% (n=164) of patients received prophylactic anticoagulation at study entry, with an all Grade VTE incidence of 7%. In patients who did not receive prophylactic anticoagulation (n=42), all Grade VTE occurred in 17% of patients. In total, 0.5% of patients had VTE leading to dose reductions of RYBREVANT FASPRO™ and no patients required permanent discontinuation. The median time to onset of VTEs was 95 days (range: 17 to 390).
RYBREVANT® with LAZCLUZE®
In MARIPOSA, VTEs occurred in 36% of patients including Grade 3 in 10% and Grade 4 in 0.5% of patients. On-study VTEs occurred in 1.2% of patients (n=5) while receiving anticoagulation therapy. There were two fatal cases of VTE (0.5%), 9% of patients had VTE leading to dose interruptions of RYBREVANT®, and 7% of patients had VTE leading to dose interruptions of LAZCLUZE®; 1% of patients had VTE leading to dose reductions of RYBREVANT®, and 0.5% of patients had VTE leading to dose reductions of LAZCLUZE®; 3.1% of patients had VTE leading to permanent discontinuation of RYBREVANT®, and 1.9% of patients had VTE leading to permanent discontinuation of LAZCLUZE®. The median time to onset of VTEs was 84 days (range: 6 to 777).
Administer prophylactic anticoagulation for the first four months of treatment. The use of Vitamin K antagonists is not recommended.
Monitor for signs and symptoms of VTE events and treat as medically appropriate. Withhold RYBREVANT FASPRO™ or RYBREVANT® and LAZCLUZE® based on severity. Once anticoagulant treatment has been initiated, resume RYBREVANT FASPRO™ or RYBREVANT® and LAZCLUZE® at the same dose level at the discretion of the healthcare provider. In the event of VTE recurrence despite therapeutic anticoagulation, permanently discontinue RYBREVANT FASPRO™ or RYBREVANT®. Treatment can continue with LAZCLUZE® at the same dose level at the discretion of the healthcare provider. Refer to the LAZCLUZE® Prescribing Information for recommended LAZCLUZE® dosage modification.
Dermatologic Adverse Reactions
RYBREVANT FASPRO™ and RYBREVANT® can cause severe rash including toxic epidermal necrolysis (TEN), dermatitis acneiform, pruritus and dry skin.
RYBREVANT FASPRO™ with LAZCLUZE®
In PALOMA-3, rash occurred in 80% of patients, including Grade 3 in 17% and Grade 4 in 0.5% of patients. Rash leading to dose reduction occurred in 11% of patients, and RYBREVANT FASPRO™ was permanently discontinued due to rash in 1.5% of patients.
RYBREVANT® with LAZCLUZE®
In MARIPOSA, rash occurred in 86% of patients, including Grade 3 in 26% of patients. The median time to onset of rash was 14 days (range: 1 to 556 days). Rash leading to dose interruptions occurred in 37% of patients for RYBREVANT® and 30% for LAZCLUZE®, rash leading to dose reductions occurred in 23% of patients for RYBREVANT® and 19% for LAZCLUZE®, and rash leading to permanent discontinuation occurred in 5% of patients for RYBREVANT® and 1.7% for LAZCLUZE®.
RYBREVANT® with Carboplatin and Pemetrexed
Based on the pooled safety population, rash occurred in 82% of patients, including Grade 3 (15%) adverse reactions. Rash leading to dose reductions occurred in 14% of patients, and 2.5% permanently discontinued RYBREVANT® and 3.1% discontinued pemetrexed.
RYBREVANT® as a Single Agent
In CHRYSALIS, rash occurred in 74% of patients, including Grade 3 in 3.3% of patients. The median time to onset of rash was 14 days (range: 1 to 276 days). Rash leading to dose reduction occurred in 5% and permanent discontinuation due to rash occurred in 0.7% of patients. Toxic epidermal necrolysis occurred in one patient (0.3%).
When initiating treatment with RYBREVANT FASPRO™ or RYBREVANT®, prophylactic and concomitant medications are recommended to reduce the risk and severity of dermatologic adverse reactions. Instruct patients to limit sun exposure during and for 2 months after treatment. Advise patients to wear protective clothing and use broad spectrum UVA/UVB sunscreen.
If skin reactions develop, administer supportive care including topical corticosteroids and topical and/or oral antibiotics. For Grade 3 reactions, add oral steroids and consider dermatologic consultation. Promptly refer patients presenting with severe rash, atypical appearance or distribution, or lack of improvement within 2 weeks to a dermatologist. For patients receiving RYBREVANT FASPRO™ or RYBREVANT® in combination with LAZCLUZE®, withhold, reduce the dose, or permanently discontinue both drugs based on severity. For patients receiving RYBREVANT FASPRO™ or RYBREVANT® as a single agent or in combination with carboplatin and pemetrexed, withhold, dose reduce or permanently discontinue RYBREVANT FASPRO™ or RYBREVANT® based on severity.
Ocular Toxicity
RYBREVANT FASPRO™ and RYBREVANT® can cause ocular toxicity including keratitis, blepharitis, dry eye symptoms, conjunctival redness, blurred vision, visual impairment, ocular itching, eye pruritus and uveitis.
RYBREVANT FASPRO™ with LAZCLUZE®
In PALOMA-3, all Grade ocular toxicity occurred in 13% of patients, including 0.5% Grade 3.
RYBREVANT® with LAZCLUZE®
In MARIPOSA, ocular toxicity occurred in 16%, including Grade 3 or 4 ocular toxicity in 0.7% of patients. Withhold, reduce the dose, or permanently discontinue RYBREVANT® and continue LAZCLUZE® based on severity.
RYBREVANT® with Carboplatin and Pemetrexed
Based on the pooled safety population, ocular toxicity occurred in 16% of patients. All events were Grade 1 or 2.
RYBREVANT® as a Single Agent
In CHRYSALIS, keratitis occurred in 0.7% and uveitis occurred in 0.3% of patients. All events were Grade 1-2.
Promptly refer patients presenting with new or worsening eye symptoms to an ophthalmologist. Withhold, dose reduce or permanently discontinue RYBREVANT FASPRO™ or RYBREVANT® based on severity.
Embryo-Fetal Toxicity
Based on animal models, RYBREVANT FASPRO™, RYBREVANT® and LAZCLUZE® can cause fetal harm when administered to a pregnant woman. Verify pregnancy status of females of reproductive potential prior to initiating RYBREVANT FASPRO™ and RYBREVANT®. Advise pregnant women and females of reproductive potential of the potential risk to the fetus. Advise patients of reproductive potential to use effective contraception during treatment and for 3 months after the last dose of RYBREVANT FASPRO™ or RYBREVANT®, and for 3 weeks after the last dose of LAZCLUZE®.
ADVERSE REACTIONS
RYBREVANT FASPRO™ with LAZCLUZE®
In PALOMA-3 (n=206), the most common adverse reactions (≥20%) were rash (80%), nail toxicity (58%), musculoskeletal pain (50%), fatigue (37%), stomatitis (36%), edema (34%), nausea (30%), diarrhea (22%), vomiting (22%), constipation (22%), decreased appetite (22%), and headache (21%). The most common Grade 3 or 4 laboratory abnormalities (≥2%) were decreased lymphocyte count (6%), decreased sodium (5%), decreased potassium (5%), decreased albumin (4.9%), increased alanine aminotransferase (3.4%), decreased platelet count (2.4%), increased aspartate aminotransferase (2%), increased gamma-glutamyl transferase (2%), and decreased hemoglobin (2%).
Serious adverse reactions occurred in 33% of patients, with those occurring in ≥2% of patients including ILD/pneumonitis (6%); and pneumonia, VTE and fatigue (2.4% each). Death due to adverse reactions occurred in 5% of patients treated with RYBREVANT FASPRO™, including ILD/pneumonitis (1.9%), pneumonia (1.5%), and respiratory failure and sudden death (1% each).
RYBREVANT® with LAZCLUZE®
In MARIPOSA (n=421), the most common adverse reactions (ARs) (≥20%) were rash (86%), nail toxicity (71%), infusion-related reactions (IRRs) (RYBREVANT®) (63%), musculoskeletal pain (47%), stomatitis (43%), edema (43%), VTE (36%), paresthesia (35%), fatigue (32%), diarrhea (31%), constipation (29%), COVID-19 (26%), hemorrhage (25%), dry skin (25%), decreased appetite (24%), pruritus (24%), and nausea (21%). The most common Grade 3 or 4 laboratory abnormalities (≥2%) were decreased albumin (8%), decreased sodium (7%), increased ALT (7%), decreased potassium (5%), decreased hemoglobin (3.8%), increased AST (3.8%), increased GGT (2.6%), and increased magnesium (2.6%).
Serious ARs occurred in 49% of patients, with those occurring in ≥2% of patients including VTE (11%), pneumonia (4%), ILD/pneumonitis and rash (2.9% each), COVID-19 (2.4%), and pleural effusion and IRRs (RYBREVANT®) (2.1% each). Fatal ARs occurred in 7% of patients due to death not otherwise specified (1.2%); sepsis and respiratory failure (1% each); pneumonia, myocardial infarction, and sudden death (0.7% each); cerebral infarction, pulmonary embolism (PE), and COVID-19 infection (0.5% each); and ILD/pneumonitis, acute respiratory distress syndrome (ARDS), and cardiopulmonary arrest (0.2% each).
RYBREVANT® with Carboplatin and Pemetrexed
In MARIPOSA-2 (n=130), the most common ARs (≥20%) were rash (72%), IRRs (59%), fatigue (51%), nail toxicity (45%), nausea (45%), constipation (39%), edema (36%), stomatitis (35%), decreased appetite (31%), musculoskeletal pain (30%), vomiting (25%), and COVID-19 (21%). The most common Grade 3 to 4 laboratory abnormalities (≥2%) were decreased neutrophils (49%), decreased white blood cells (42%), decreased lymphocytes (28%), decreased platelets (17%), decreased hemoglobin (12%), decreased potassium (11%), decreased sodium (11%), increased alanine aminotransferase (3.9%), decreased albumin (3.8%), and increased gamma-glutamyl transferase (3.1%).
In MARIPOSA-2, serious ARs occurred in 32% of patients, with those occurring in >2% of patients including dyspnea (3.1%), thrombocytopenia (3.1%), sepsis (2.3%), and PE (2.3%). Fatal ARs occurred in 2.3% of patients; these included respiratory failure, sepsis, and ventricular fibrillation (0.8% each).
In PAPILLON (n=151), the most common ARs (≥20%) were rash (90%), nail toxicity (62%), stomatitis (43%), IRRs (42%), fatigue (42%), edema (40%), constipation (40%), decreased appetite (36%), nausea (36%), COVID-19 (24%), diarrhea (21%), and vomiting (21%). The most common Grade 3 to 4 laboratory abnormalities (≥2%) were decreased albumin (7%), increased alanine aminotransferase (4%), increased gamma-glutamyl transferase (4%), decreased sodium (7%), decreased potassium (11%), decreased magnesium (2%), and decreases in white blood cells (17%), hemoglobin (11%), neutrophils (36%), platelets (10%), and lymphocytes (11%).
In PAPILLON, serious ARs occurred in 37% of patients, with those occurring in ≥2% of patients including rash, pneumonia, ILD, PE, vomiting, and COVID-19. Fatal adverse reactions occurred in 7 patients (4.6%) due to pneumonia, cerebrovascular accident, cardio-respiratory arrest, COVID-19, sepsis, and death not otherwise specified.
RYBREVANT® as a Single Agent
In CHRYSALIS (n=129), the most common ARs (≥20%) were rash (84%), IRR (64%), paronychia (50%), musculoskeletal pain (47%), dyspnea (37%), nausea (36%), fatigue (33%), edema (27%), stomatitis (26%), cough (25%), constipation (23%), and vomiting (22%). The most common Grade 3 to 4 laboratory abnormalities (≥2%) were decreased lymphocytes (8%), decreased albumin (8%), decreased phosphate (8%), decreased potassium (6%), increased alkaline phosphatase (4.8%), increased glucose (4%), increased gamma-glutamyl transferase (4%), and decreased sodium (4%).
Serious ARs occurred in 30% of patients, with those occurring in ≥2% of patients including PE, pneumonitis/ILD, dyspnea, musculoskeletal pain, pneumonia, and muscular weakness. Fatal adverse reactions occurred in 2 patients (1.5%) due to pneumonia and 1 patient (0.8%) due to sudden death.
LAZCLUZE® DRUG INTERACTIONS
Avoid concomitant use of LAZCLUZE® with strong and moderate CYP3A4 inducers. Consider an alternate concomitant medication with no potential to induce CYP3A4.
Monitor for adverse reactions associated with a CYP3A4 or BCRP substrate where minimal concentration changes may lead to serious adverse reactions, as recommended in the approved product labeling for the CYP3A4 or BCRP substrate.
Please see full Prescribing Information for RYBREVANT FASPRO™, RYBREVANT® and LAZCLUZE®.
About Johnson & JohnsonAt Johnson & Johnson, we believe health is everything. Our strength in healthcare innovation empowers us to build a world where complex diseases are prevented, treated, and cured, where treatments are smarter and less invasive, and solutions are personal. Through our expertise in Innovative Medicine and MedTech, we are uniquely positioned to innovate across the full spectrum of healthcare solutions today to deliver the breakthroughs of tomorrow, and profoundly impact health for humanity.
Learn more at https://www.jnj.com/ or at www.innovativemedicine.jnj.com.
Cautions Concerning Forward-Looking StatementsThis press release contains “forward-looking statements” as defined in the Private Securities Litigation Reform Act of 1995 related to ERLEADA® (apalutamide), pasritamig (JNJ-78278343), TECVAYLI® (teclistamab-cqyv), DARZALEX® (daratumumab), TALVEY® (talquetamab-tgvs), CARVYKTI® (cilta-cel), RYBREVANT FASPRO™ (amivantamab and hyaluronidase-lpuj), RYBREVANT® (amivantamab-vmjw) and LAZCLUZE® (lazertinib).The reader is cautioned not to rely on these forward-looking statements. These statements are based on current expectations of future events. If underlying assumptions prove inaccurate or known or unknown risks or uncertainties materialize, actual results could vary materially from the expectations and projections of Johnson & Johnson. Risks and uncertainties include, but are not limited to: challenges and uncertainties inherent in product research and development, including the uncertainty of clinical success and of obtaining regulatory approvals; uncertainty of commercial success; manufacturing difficulties and delays; competition, including technological advances, new products and patents attained by competitors; challenges to patents; product efficacy or safety concerns resulting in product recalls or regulatory action; changes in behavior and spending patterns of purchasers of health care products and services; changes to applicable laws and regulations, including global health care reforms; and trends toward health care cost containment. A further list and descriptions of these risks, uncertainties and other factors can be found in Johnson & Johnson’s most recent Annual Report on Form 10-K, including in the sections captioned “Cautionary Note Regarding Forward-Looking Statements” and “Item 1A. Risk Factors,” and in Johnson & Johnson’s subsequent Quarterly Reports on Form 10-Q and other filings with the Securities and Exchange Commission. Copies of these filings are available online at www.sec.gov, www.jnj.com, www.investor.jnj.com or on request from Johnson & Johnson. Johnson & Johnson does not undertake to update any forward-looking statement as a result of new information or future events or developments.
1 ERLEADA® U.S. Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
2 U.S. FDA Approves TECVAYLI® (teclistamab-cqyv), the First Bispecific T-cell Engager Antibody for the Treatment of Patients with Relapsed or Refractory Multiple Myeloma. https://www.jnj.com/u-s-fda-approves-tecvayli-teclistamab-cqyv-the-first-bispecific-t-cell-engager-antibody-for-the-treatment-of-patients-with-relapsed-or-refractory-multiple-myeloma. Accessed April 2026.
3 DARZALEX FASPRO® U.S. Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
4 DARZALEX® U.S. Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
5 TALVEY® U.S. Prescribing Information, August 2023.
6 European Medicines Agency. TALVEY® Summary of Product Characteristics. August 2023.
7 CARVYKTI® U.S. Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
8 RYBREVANT FASPRO® Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
9 RYBREVANT® Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
10 Cho BC, et al. Lazertinib versus gefitinib as first-line treatment in patients with EGFR-mutated advanced non-small-cell lung cancer: Results From LASER301. J Clin Oncol. 2023;41(26):4208-4217.
11 LAZCLUZE® Prescribing Information. Horsham, PA: Janssen Biotech, Inc.
Phase 3ImmunotherapyClinical ResultPhase 2Drug Approval
14 Apr 2026
Johnson & Johnson said its newly launched oral IL-23 peptide Icotyde (icotrokinra) has already racked up roughly 1500 prescriptions in the first few weeks since its March approval for plaque psoriasis, a pace that has company executives abuzz about the drug's prospects."It's off to a very fast start," said Jennifer Taubert, EVP for Innovative Medicine, at J&J's first-quarter earnings call Tuesday. "We think it's got the potential to become one of our biggest products."The once-daily pill is indicated for moderate-to-severe psoriasis patients as young as 12 years old who are candidates for systemic therapy or phototherapy. In head-to-head superiority studies, Icotyde showed superior skin clearance when put up against Bristol Myers Squibb's oral TYK2 inhibitor Sotyktu (deucravacitinib), while having a safety profile akin to placebo.'One-two punch'"A number of us were out at the AAD (American Academy of Dermatology) meeting as well, and the KOL receptivity to the strength and the simplicity of the label has been really encouraging," Taubert said. "Things like no lab monitoring…no black box or drug interactions really is giving us good confidence that this is going to be really the preferred choice in first choice for systemic therapy." FirstWord is running a poll to gauge early physician expectations for the drug, click here to be notified of the results.Icotyde's role was also highlighted alongside Tremfya (guselkumab), J&J's established injectable biologic for psoriasis, which the company predicts will exceed $10 billion in peak annual sales. Tremfya, which treats psoriasis as well as inflammatory bowel diseases (IBD), generated $1.6 billion in first-quarter sales, up 68% year-over-year, and beat estimates of $1.2 billion."We think that with that one-two punch, we have got the portfolio for psoriatic disease and patients that are really excited about both agents going forward," Taubert said, adding "we're in the middle of very, very positive conversations with [payors] to try to drive…early and very broad access."Data for Icotyde in psoriatic arthritis is expected to read out later this year; the drug is currently being evaluated in the Phase III ICONIC-PsA 1 and ICONIC-PsA 2 studies. Enrollment is also underway in a pair of IBD trials; ICONIC-UC in ulcerative colitis and ICONIC-CD in Crohn's disease.Moving beyond StelaraMeanwhile, the performance of J&J's former blockbuster Stelara – used to treat psoriasis, Crohn’s disease and other autoimmune conditions – continues its downward slide in the face of biosimilar competition, with quarterly sales tumbling nearly 60% during the quarter to $656 million (see – Vital Signs: Fastest falling drugs of 2025).However, instead of switching to biosimilars, Chief Financial Officer Joseph Wolk told CNBC, "We are seeing increased share in Tremfya and we anticipate we'll see something similar in the new oral offering."In other results, J&J reported that sales of its multiple myeloma treatment Darzalex were 22.5% higher in the quarter at $4 billion, compared to the year-ago period, whereas analysts were projecting $3.4 billion. Newer blood cancer therapies Carvykti ($597 million, +62.1%), Tecvayli ($202 million, +33.5%) and Talvey ($152 million, 76.7%) also helped drive growth."[J&J] has emerged as one of the cleaner names in the group as the company moves beyond the Stelara loss of exclusivity and with healthy growth in its core portfolio," said JP Morgan analysts. "We see J&J as capable of generating sustained top-tier growth."The company bumped up its full-year sales forecast to between $100.3 billion and $101.3 billion, nudging both ends of the previous range up by $300 million. Profit is expected to be higher as well, with earnings now estimated to be between $11.45 and $11.65 per share, a two-cent bump at each end of the range.
100 Deals associated with Talquetamab
Login to view more data
R&D Status
Approved
10 top approved records. to view more data
Login
| Indication | Country/Location | Organization | Date |
|---|---|---|---|
| Refractory Multiple Myeloma | Japan | 24 Jun 2025 | |
| Relapse multiple myeloma | Japan | 24 Jun 2025 | |
| Multiple Myeloma | United States | 09 Aug 2023 |
Developing
10 top R&D records. to view more data
Login
| Indication | Highest Phase | Country/Location | Organization | Date |
|---|---|---|---|---|
| Residual Neoplasm | Phase 2 | United States | 21 Aug 2025 | |
| Peripheral Stem Cell Transplantation | Phase 2 | United States | 05 Jun 2025 | |
| Smoldering Multiple Myeloma | Phase 2 | United States | 04 Dec 2023 | |
| Extramedullary Disease in Multiple Myeloma | Phase 2 | Spain | 21 Sep 2023 | |
| Hematologic Neoplasms | Phase 1 | United States | 16 Dec 2017 | |
| Hematologic Neoplasms | Phase 1 | Belgium | 16 Dec 2017 | |
| Hematologic Neoplasms | Phase 1 | Netherlands | 16 Dec 2017 | |
| Hematologic Neoplasms | Phase 1 | Spain | 16 Dec 2017 |
Login to view more data
Clinical Result
Clinical Result
Indication
Phase
Evaluation
View All Results
| Study | Phase | Population | Analyzed Enrollment | Group | Results | Evaluation | Publication Date |
|---|
Not Applicable | 36 | (Renal Impairment) | rjceczaosn(gyuwnfsydg) = Comparable safety profile in RI vs No RI: 66.7% any-grade cytokine release syndrome (CRS) with 8.3% grade ≥3 CRS in each, but more grade 1 CRS in RI 58.3% vs 45.8% (=0.73). Any-grade Immune effector cell-associated neurotoxicity syndrome (ICANS) was 16.7% vs 20.8%, with grade ≥3 ICANS 8.3% vs 12.5%. Infection rate 8.3% vs 16.7% (=0.65), dysgeusia was 83.3% in each, skin-related AEs 75% vs 58.3% (=0.47), and nail-related AEs 83.3% vs 54.2% (=0.14). Median inpatient step-up dosing was 10 vs 9 days (=0.23). grqjwcevfu (fikkzadfng ) View more | Positive | 04 Feb 2026 | ||
(No Renal Impairment) | |||||||
Not Applicable | 25 | ylzuwxtziv(pemiksscil) = xrxotgiojt beaehwhujk (ntjfbkvlyl ) View more | Positive | 04 Feb 2026 | |||
Not Applicable | 43 | qspawhmtbb(vnyumyhfyi) = jkjhjufemc utkwnzsvwo (fknuojhiub ) | Positive | 04 Feb 2026 | |||
qspawhmtbb(vnyumyhfyi) = cnydpwjisp utkwnzsvwo (fknuojhiub ) | |||||||
Not Applicable | 10 | CAR-T | qhbzxoault(zazpvyfcnj) = itwtocyeaj ciruitkoja (nqapaohhwg ) View more | Positive | 04 Feb 2026 | ||
Not Applicable | 465 | lralelpask(otqtntvpwa) = awrcvigcwa ddeiljvozy (lhwdrcrons ) View more | Negative | 04 Feb 2026 | |||
lralelpask(otqtntvpwa) = hrodlnstch ddeiljvozy (lhwdrcrons ) View more | |||||||
Not Applicable | 61 | Bispecific Therapies | tipekrmfbc(zlywkgojmx) = hzxjrgzvuo pdcgmrirfr (cbsoiwyalj ) View more | Positive | 04 Feb 2026 | ||
Phase 2 | 90 | bszxkoyzvn(xlfxhddflp) = eioiuonbln npnwdrejoo (gzwwazbqme, 69 - 87) View more | Positive | 01 Jan 2026 | |||
Phase 2 | 90 | pcheeowwby(yxdsorsfqn) = uxfdudoxzy dkkefnwedd (mfvofbzcqz, 69 - 87) View more | Positive | 07 Dec 2025 | |||
Not Applicable | 417 | (patients with renal impairment (RI)) | lsakhdnniw(uiizgyfhzc) = cmjjwtowrh lrpqrtdgpu (fqjbkyxuzw ) View more | Positive | 06 Dec 2025 | ||
(without renal impairment (RI)) | lsakhdnniw(uiizgyfhzc) = vvxjcajuaw lrpqrtdgpu (fqjbkyxuzw ) View more | ||||||
Not Applicable | 87 | fbqpoinqsp(yuidwiermj) = hjuzmhhkyt avjwnqtjdc (wzscrcbbbh ) View more | Positive | 06 Dec 2025 |
Login to view more data
Translational Medicine
Boost your research with our translational medicine data.
login
or

Deal
Boost your decision using our deal data.
login
or

Core Patent
Boost your research with our Core Patent data.
login
or

Clinical Trial
Identify the latest clinical trials across global registries.
login
or

Approval
Accelerate your research with the latest regulatory approval information.
login
or

Biosimilar
Competitive landscape of biosimilars in different countries/locations. Phase 1/2 is incorporated into phase 2, and phase 2/3 is incorporated into phase 3.
login
or
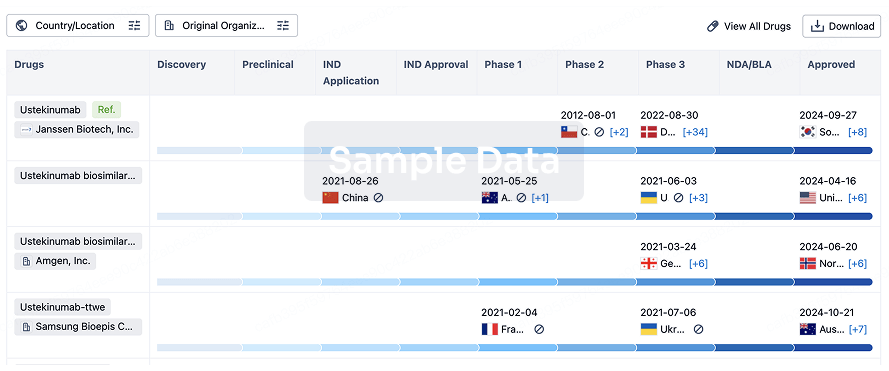
Regulation
Understand key drug designations in just a few clicks with Synapse.
login
or

AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free






