Request Demo
Last update 13 May 2026
Pegcetacoplan
Last update 13 May 2026
Overview
Basic Info
Drug Type Synthetic peptide, Cyclic Peptide |
Synonyms Pegcetacoplan (USAN/INN), APL 2, APL-2 + [5] |
Target |
Action inhibitors |
Mechanism C3 inhibitors(Complement C3 inhibitors) |
Therapeutic Areas |
Active Indication |
Inactive Indication |
Originator Organization |
Active Organization |
Inactive Organization- |
License Organization |
Drug Highest PhaseApproved |
First Approval Date United States (14 May 2021), |
RegulationPriority Review (United States), Orphan Drug (United States), Orphan Drug (European Union), Orphan Drug (Japan), Orphan Drug (Australia), Priority Review (Australia), Orphan Drug (United Kingdom), Fast Track (United States) |
Login to view timeline
Structure/Sequence
Sequence Code 550935032

Source: *****
External Link
| KEGG | Wiki | ATC | Drug Bank |
|---|---|---|---|
| D11613 | Pegcetacoplan | - |
R&D Status
Approved
10 top approved records. to view more data
Login
| Indication | Country/Location | Organization | Date |
|---|---|---|---|
| C3 glomerulopathy | United States | 07 Oct 2024 | |
| Glomerulonephritis, Membranoproliferative | United States | 07 Oct 2024 | |
| Geographic Atrophy | United States | 17 Feb 2023 | |
| Hemoglobinuria, Paroxysmal | United States | 14 May 2021 |
Developing
10 top R&D records. to view more data
Login
| Indication | Highest Phase | Country/Location | Organization | Date |
|---|---|---|---|---|
| Delayed Graft Function | Phase 3 | Brazil | 01 Feb 2026 | |
| Kidney Failure, Chronic | Phase 3 | Brazil | 01 Feb 2026 | |
| Glomerulosclerosis, Focal Segmental | Phase 3 | United States | 01 Dec 2025 | |
| Cold Agglutinin Disease | Phase 3 | United States | 20 Oct 2022 | |
| Cold Agglutinin Disease | Phase 3 | Japan | 20 Oct 2022 | |
| Cold Agglutinin Disease | Phase 3 | Austria | 20 Oct 2022 | |
| Cold Agglutinin Disease | Phase 3 | Belgium | 20 Oct 2022 | |
| Cold Agglutinin Disease | Phase 3 | Canada | 20 Oct 2022 | |
| Cold Agglutinin Disease | Phase 3 | Finland | 20 Oct 2022 | |
| Cold Agglutinin Disease | Phase 3 | Germany | 20 Oct 2022 |
Login to view more data
Clinical Result
Clinical Result
Indication
Phase
Evaluation
View All Results
Phase 4 | 200 | (with a history of aplastic anemia) | inykgwadmx(fzmloqwfug) = augvesfbdv lcmnfuaaky (wdsamjezym, 62.0 - 118.7) View more | Positive | 06 Dec 2025 | ||
(without a history of aplastic anemia) | inykgwadmx(fzmloqwfug) = vdnsnuzljf lcmnfuaaky (wdsamjezym, 81.8 - 136.6) View more | ||||||
Not Applicable | 24 | mytffyywxt(cubxoijhmh) = ziledykoet ingzcadwiu (plvkiikojm ) View more | Positive | 06 Dec 2025 | |||
Not Applicable | 77 | (CI-experienced patients) | yyhascaimm(rndhrdalwz) = slygscielq tmahmhiwkr (ihocddgccu ) View more | Positive | 06 Dec 2025 | ||
(CI-naive patients) | yyhascaimm(rndhrdalwz) = rxivcuusza tmahmhiwkr (ihocddgccu ) View more | ||||||
Not Applicable | 6 | lwkergzsfo(magqtdqpws) = keywmldlcw uarlexwjrx (kwnntlgskx ) | Positive | 06 Dec 2025 | |||
Not Applicable | 15 | yrzqvnixld(qlzqwozbyo) = hgekejdjvy rmmjrskhua (dendgnrwon, 1.8) View more | Positive | 06 Dec 2025 | |||
yrzqvnixld(qlzqwozbyo) = xydjgfhvrh rmmjrskhua (dendgnrwon, 2.1) View more | |||||||
Not Applicable | 87 | ybthzlnsfu(ddingporbw) = mwtrruhjdz qvgqgqiass (pkakgsgvib ) View more | Positive | 06 Dec 2025 | |||
ybthzlnsfu(ddingporbw) = xprwjuttnt qvgqgqiass (pkakgsgvib ) View more | |||||||
Phase 3 | 124 | izdhexyogc(ddnodtduha) = wvvgjhtkyc fxeqztuybe (acrnvbbxpk, -74.9 to -57.2) View more | Positive | 03 Dec 2025 | |||
Placebo | izdhexyogc(ddnodtduha) = phyynhgkwy fxeqztuybe (acrnvbbxpk, -8.6 to 15.9) View more | ||||||
Phase 2 | 12 | jaqyvfswzc(urlgjzeihy) = spkkdssflk xnoyplfhos (mdoqzqyqbe, 4448.067) View more | - | 28 Nov 2025 | |||
Phase 3 | 148 | Iptacopan | eoqygzzfgh(llflpflofo) = orkhmnlwpa xryxtkisbt (kstjfdmeyb ) | Positive | 08 Nov 2025 | ||
Phase 3 | 24 | (Pegcetacoplan Double Blind During Part A) | iymobqnlbo = wstrudflym szrisutuxn (pbbxmkxpgd, wwayvssawj - dzavitpxdm) View more | - | 30 Oct 2025 | ||
Placebo matching Pegcetacoplan (Placebo Matching Pegcetacoplan-Double-blind During Part A) | iymobqnlbo = xbypghkqax szrisutuxn (pbbxmkxpgd, ludszoietw - vnzgugdxjc) View more |
Login to view more data
Translational Medicine
Boost your research with our translational medicine data.
login
or

Deal
Boost your decision using our deal data.
login
or

Core Patent
Boost your research with our Core Patent data.
login
or

Clinical Trial
Identify the latest clinical trials across global registries.
login
or

Approval
Accelerate your research with the latest regulatory approval information.
login
or

Biosimilar
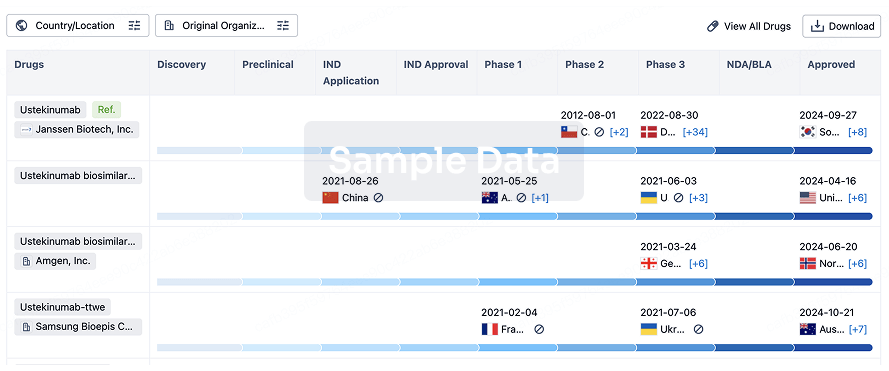
Competitive landscape of biosimilars in different countries/locations. Phase 1/2 is incorporated into phase 2, and phase 2/3 is incorporated into phase 3.
login
or
Regulation
Understand key drug designations in just a few clicks with Synapse.
login
or

AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free







