Request Demo
Last update 05 Dec 2025

East Lancashire Hospitals NHS
Last update 05 Dec 2025
Overview
Related
23
Clinical Trials associated with East Lancashire Hospitals NHSNCT06985979
Exploring the Needs of High-intensity User Patients Within the Emergency Department: Informing the Development of a Psychosocial Service
The aim of this qualitative interview study is to explore the unmet needs of patients who frequently attend the emergency department and the challenges of the staff who support them.
The study will interview 10 patients who frequently attend the emergency department and 10 staff members working within the emergency department.
The study will interview 10 patients who frequently attend the emergency department and 10 staff members working within the emergency department.
Start Date01 Jun 2025 |
Sponsor / Collaborator |
NCT07011407
Facial Recognition in Acute Illness - The FACIAL Study
Facial recognition is a non-invasive method for analysing facial characteristics and changes in facial expressions. There is evidence to suggest there may be a link between physiological health and facial expression patterns. Many medical conditions are associated with specific facial characteristics, with some related to inherited genetic conditions and others that have been acquired as a result of medical conditions such as stroke, nerve injuries and dementia. If successful, this technology could prove useful for studies evaluating the monitoring of acute or chronic illness. The proposed study will ask participants to do a maximal exercise test that will challenge the body, as a proof-of-principle, to see how this correlates with facial expressions. Depending on the study outcomes and future work, it could prove to be a useful tool and clinical application in healthcare for evaluating and tracking patient health and well-being. The investigators want to conduct a proof-of-principle study where physically stressed young and healthy participants (in the form of a maximal exercise test), whilst recording facial expressions, will be used to determine the relationship between physiological stress and changes in facial parameters.
Start Date01 Jun 2025 |
Sponsor / Collaborator |
NCT05964140
Should we Use Post-operative Antibiotics Following Surgery for Patients With Mandible Fractures? The MANTRA Trial (MANdibular TRauma and Antibiotic Use)
1. FULL TITLE OF THE PROJECT Should we use post-operative antibiotics following surgery for patients with mandible fractures? The MANTRA trial (MANdibular TRauma and Antibiotic use)
2. SUMMARY OF RESEARCH (ABSTRACT) Research Question: Are post-operative antibiotics required following surgery for patients with mandible fractures? Background: Mandible fractures are the commonest facial fractures needing surgery and account for a significant percentage of the acute workload in Oral & Maxillofacial Surgery (OMFS) units. The UK records over 6000 new cases per year. Patients having surgery for mandible fractures have a theoretical risk of developing surgical site infection, due to the proximity of the fracture lines to the oral cavity microbes and the presence of foreign body (titanium fixation miniplates). For this reason, clinicians often prescribe antibiotics after surgery, to reduce the risk of infection. Previous systematic reviews and a multicentre cohort study performed by this team, revealed significant clinical variation in post-operative antibiotic prescription amongst UK OMFS clinicians and the presence of clinical equipoise. Antibiotic overuse can lead to antibiotic resistance and other antibiotic-related side effects; judicious antibiotic use and stewardship is of paramount importance.
Aim: To determine whether post-operative antibiotics are required at all, following surgery for mandible fractures, and, if so, what is the most clinically- and cost-effective regimen
Objectives:
Primary Objective To conduct a Randomized Controlled Trial (MANTRA) in order to establish the non-inferiority (or not) of not giving post-operative antibiotics versus 2 other post-operative antibiotic regimens. An internal pilot phase will optimise recruitment and retention.
Secondary Objectives
* Measure the cost-effectiveness of the proposed antibiotic pathways
* Assess patient and clinician acceptability to change clinical practice
* Process evaluation to inform dissemination and implementation Methods: The investigators designed and propose the MANTRA RCT to compare 3 post-operative antibiotic approaches to prevent Surgical Site Infections (SSIs) following surgery for mandible fractures. The MANTRA trial is a large open label, multicentre study in NHS OMFS units. The 3 study arms represent the most common clinical pathways in the UK based on previous work; the control group is the approach prescribed by most UK OMFS clinicians. All patients will receive 1 dose of IV antibiotics (co-amoxiclav 1.2g, if no penicillin allergy, which is the most commonly used prophylactic antibiotic currently) on induction of anaesthesia, prior to their surgery.
The participants will be randomised to the following (1:1:1):
Group A: No further antibiotics Group B: 2 further postoperative IV doses of co-amoxiclav 1.2g Group C: 2 further postoperative IV doses (as above), followed by a 5-day course of oral co-amoxiclav 625mg every 8 hours if no penicillin allergy (Control).
Trial processes will be optimised by an internal pilot phase ensuring we recruit, randomise, and retain participants with clear progression criteria. We will also conduct cost-effectiveness analyses and process evaluation for dissemination and implementation
Timeline:
Start of grant: 1st July 2023 Start of RCT / pilot: 1st January 2024 End of pilot: 30th June 2024 End of recruitment: 31st December 2026 End of follow-up: 30th June 2027 Completion: 31st December 2027
Impact and dissemination:
* Practice changing outputs that standardise the use of antibiotics in mandible fractures in the NHS and provide a framework for other surgical prophylaxis research
* A bespoke clinical dissemination plan via an engagement and training legacy
* Cost-effectiveness data to inform policy making
* A research legacy and change of culture in the specialty of OMFS
2. SUMMARY OF RESEARCH (ABSTRACT) Research Question: Are post-operative antibiotics required following surgery for patients with mandible fractures? Background: Mandible fractures are the commonest facial fractures needing surgery and account for a significant percentage of the acute workload in Oral & Maxillofacial Surgery (OMFS) units. The UK records over 6000 new cases per year. Patients having surgery for mandible fractures have a theoretical risk of developing surgical site infection, due to the proximity of the fracture lines to the oral cavity microbes and the presence of foreign body (titanium fixation miniplates). For this reason, clinicians often prescribe antibiotics after surgery, to reduce the risk of infection. Previous systematic reviews and a multicentre cohort study performed by this team, revealed significant clinical variation in post-operative antibiotic prescription amongst UK OMFS clinicians and the presence of clinical equipoise. Antibiotic overuse can lead to antibiotic resistance and other antibiotic-related side effects; judicious antibiotic use and stewardship is of paramount importance.
Aim: To determine whether post-operative antibiotics are required at all, following surgery for mandible fractures, and, if so, what is the most clinically- and cost-effective regimen
Objectives:
Primary Objective To conduct a Randomized Controlled Trial (MANTRA) in order to establish the non-inferiority (or not) of not giving post-operative antibiotics versus 2 other post-operative antibiotic regimens. An internal pilot phase will optimise recruitment and retention.
Secondary Objectives
* Measure the cost-effectiveness of the proposed antibiotic pathways
* Assess patient and clinician acceptability to change clinical practice
* Process evaluation to inform dissemination and implementation Methods: The investigators designed and propose the MANTRA RCT to compare 3 post-operative antibiotic approaches to prevent Surgical Site Infections (SSIs) following surgery for mandible fractures. The MANTRA trial is a large open label, multicentre study in NHS OMFS units. The 3 study arms represent the most common clinical pathways in the UK based on previous work; the control group is the approach prescribed by most UK OMFS clinicians. All patients will receive 1 dose of IV antibiotics (co-amoxiclav 1.2g, if no penicillin allergy, which is the most commonly used prophylactic antibiotic currently) on induction of anaesthesia, prior to their surgery.
The participants will be randomised to the following (1:1:1):
Group A: No further antibiotics Group B: 2 further postoperative IV doses of co-amoxiclav 1.2g Group C: 2 further postoperative IV doses (as above), followed by a 5-day course of oral co-amoxiclav 625mg every 8 hours if no penicillin allergy (Control).
Trial processes will be optimised by an internal pilot phase ensuring we recruit, randomise, and retain participants with clear progression criteria. We will also conduct cost-effectiveness analyses and process evaluation for dissemination and implementation
Timeline:
Start of grant: 1st July 2023 Start of RCT / pilot: 1st January 2024 End of pilot: 30th June 2024 End of recruitment: 31st December 2026 End of follow-up: 30th June 2027 Completion: 31st December 2027
Impact and dissemination:
* Practice changing outputs that standardise the use of antibiotics in mandible fractures in the NHS and provide a framework for other surgical prophylaxis research
* A bespoke clinical dissemination plan via an engagement and training legacy
* Cost-effectiveness data to inform policy making
* A research legacy and change of culture in the specialty of OMFS
Start Date06 Dec 2024 |
Sponsor / Collaborator |
100 Clinical Results associated with East Lancashire Hospitals NHS
Login to view more data
0 Patents (Medical) associated with East Lancashire Hospitals NHS
Login to view more data
469
Literatures (Medical) associated with East Lancashire Hospitals NHS01 Jan 2026·ANNALS OF VASCULAR SURGERY
Evaluating the Clinical Profile of Thoracic Endovascular Aortic Repair in Blunt Thoracic Aortic Injury: A Systematic Review and Meta-Analysis
Review
Author: Bashir, Mohamad ; Jubouri, Yousif F ; Alaraj, Rami S N ; Abdelhaliem, Amr ; Qaisi, Aya F ; Surkhi, Abdelaziz O ; Moothathamby, Thurkga ; Rajput, Muhammad Nabil ; Al-Bunnia, Ahmed ; Jubouri, Matti ; Alsarayrah, Abdullah I ; Piffaretti, Gabriele ; Akasheh, Hani M
BACKGROUND:
Blunt thoracic aortic injury (BTAI) is a critical vascular emergency associated with high mortality rates. Thoracic endovascular aortic repair (TEVAR) is the gold-standard treatment for this condition. This meta-analysis seeks to comprehensively evaluate the clinical profile and outcomes associated with TEVAR in managing BTAI.
METHODS:
A systematic review was undertaken using a rigorous methodology. This involved conducting searches across multiple electronic databases using defined search terms while adhering to stringent preestablished inclusion and exclusion criteria in accordance with the Cochrane Handbook and the PRISMA 2020 guidelines. Proportional meta-analysis was executed using Comprehensive Meta-Analysis software (version 4).
RESULTS:
A total of 117 studies comprising 29,972 patients were analyzed. The mean age was 42.3 years, with 74.9% being male. The mean injury severity score was 35.9, and the distribution of BTAI Society for Vascular Surgery grades was as follows: Grade 1 at 8%, Grade 2 at 18.1%, Grade 3 at 62.3%, and Grade 4 at 14.9%. The in-hospital and 30-day mortality rate was reported at an aggregated rate of 6.2%. A meta-regression analysis investigating the relationship between mortality and delayed intervention (>24 h) demonstrated a significant inverse correlation. The incidence of postoperative stroke and endoleak was aggregated at 3.2% and 3%, respectively. Coverage of the left subclavian artery (LSA) was noted in 37.3% of the patients. A subanalysis was performed to examine the association between BTAI grade and 30-day mortality, which indicated a weak and nonsignificant correlation (regression coefficient: 0.455, P-value = 0.2588). In addition, a meta-regression assessing the relationship between LSA coverage and left arm symptoms did not yield a significant relationship. However, a significant inverse relationship was identified between LSA coverage and stroke incidence.
CONCLUSION:
The management of BTAI poses significant challenges because of its associated high morbidity and mortality rates. However, TEVAR has emerged as a safe and effective intervention, yielding favorable outcomes for patients. Early diagnosis and timely referral to trauma centers equipped with TEVAR capabilities are essential to enhance survival rates and overall patient prognosis.
01 Dec 2025·Radiology case reports
Acute Stanford type B aortic dissection in a male: A case report
Article
Author: Sulaiman, Rafeeq Ahmed ; Teeli, Mehdi Hassan ; Jameel, Mohammed ; Cooper, Hannah
Acute aortic dissection (AAD) is a fatal cardio-vascular emergency initiated by an intimal breach in the aorta, leading to the delamination of its wall layers and the development of true and false lumina. Typically, Stanford Type B dissections are amenable to medical management unless complications develop. This report describes a 45-year-old hypertensive male who presented with acute, severe, constricting chest pain. Physical assessment identified a notable inter-arm blood pressure discrepancy. Emergency Computed Tomography Angiography (CTA) confirmed an acute Stanford Type B AAD, originating post to left subclavian artery and extending into the abdominal aorta and right common iliac artery, accompanied by mediastinal and pericardial hemorrhage. The patient promptly received aggressive medical therapy to stabilize hemodynamics (blood pressure and heart rate reduction) and was urgently transferred to a specialized cardio-thoracic intensive care facility. This case highlights the paramount importance of swift diagnosis and effective hemodynamic stabilization in managing acute aortic dissections.
01 Nov 2025·ANNALS OF THE ROYAL COLLEGE OF SURGEONS OF ENGLAND
Management of persistent postoperative wound leakage after total hip and knee arthroplasty: a regional perspective in the north west of England
Article
Author: Topping, J ; Wheelton, A ; Wilkinson, H ; Warner, C. ; Rogers, S ; Sahl, AB ; Choi, M ; Hughes, L ; Coombe-Jones, M ; Usman, M ; Hoggett, L ; Fendius, S ; Cornish, E ; Naylor, T
Introduction:
There is a well-documented association between persistent wound drainage and the development of prosthetic joint infections in total hip (THA) and total knee arthroplasty (TKA). Despite this, there are no national clinical guidelines in the United Kingdom on the diagnosis or management of postoperative wound drainage. We aimed to evaluate what variability exists within clinical practice in the recognition and treatment of persistent wound leakage following THA and TKA.
Methods:
An anonymous online survey consisting of 12 multiple-choice questions was distributed among hip and knee arthroplasty consultants in the north west of England. Topics covered in the questionnaire included definition, diagnosis, classification, timing and treatment of persistent wound drainage.
Results:
Twelve orthopaedic centres across the region participated in data collection. A total of 65 consultants completed the questionnaire. Some 45% of respondents used a definition of persistent wound leakage after arthroplasty, which ranged from drainage beyond 48h to that lasting more than 2 weeks. Only 54% of consultants reported having a monitoring system in place for patients with persistent wound drainage after discharge from hospital. There was wide variation in the preferred timing of initiating both non-operative and surgical management of wound leakage, as well as different treatment modalities used. Most respondents rated C-reactive protein as the most useful serological marker in aiding decision making.
Conclusion:
The results demonstrate a lack of concurrence in the recognition and management of postoperative wound drainage. Formal national clinical guidelines are necessary to standardise practice.
100 Deals associated with East Lancashire Hospitals NHS
Login to view more data
100 Translational Medicine associated with East Lancashire Hospitals NHS
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 04 Mar 2026
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or

Translational Medicine
Boost your research with our translational medicine data.
login
or

Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or

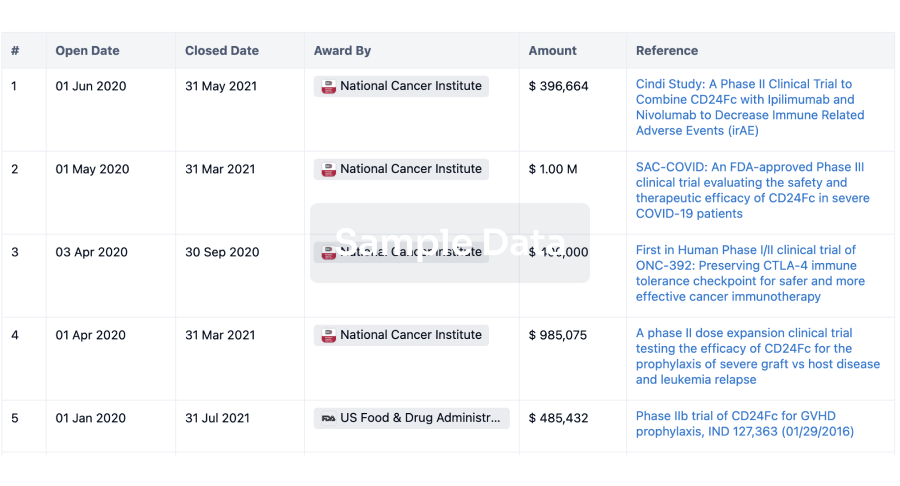
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or

Financing
Unearth financing trends to validate and advance investment opportunities.
login
or

AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free
