Request Demo
Last update 09 Sep 2025

Danbury Hospital
Last update 09 Sep 2025
Overview
Related
12
Clinical Trials associated with Danbury HospitalNCT04687449
Curcumin in Management of Chronic Obstructive Pulmonary Disease: A Randomized Controlled Trial (C-COPD Trial)
In this double-blind, placebo-controlled trial, 120 patients with a diagnosis of COPD will be randomized to receive either a daily curcumin preparation or placebo for 90 days, in addition to the standard of care treatment. The outcomes will be compared between the study arms. No dose escalation will be used.
Start Date01 Jan 2022 |
Sponsor / Collaborator |
NCT04540510
Oscillatory Positive Expiratory Pressure Devices in Acute Inpatient Treatment of Pneumonia
This is a randomized-controlled prospective study to be conducted at Danbury Hospital and Norwalk Hospital to evaluate oscillatory positive expiratory pressure (OPEP) devices for "airway clearance" (helping to clear out phlegm or mucous from your lungs and bronchial tubes) in the treatment of patients admitted to the hospital with pneumonia.
Approximately 200 subjects are expected to participate in this study.
Approximately 200 subjects are expected to participate in this study.
Start Date13 Aug 2019 |
Sponsor / Collaborator |
NCT03870685
Surgical Site Infiltration of Liposomal Bupivacaine Versus Transversus Plane Block With Liposomal Bupivacaine in Patients With Suspected or Known Gynecologic Cancer Undergoing Laparotomy Via Midline Incision
This is a randomized-controlled prospective study to be conducted at Danbury Hospital and Norwalk Hospital to compare postoperative opioid consumption and pain scores of patients with suspected or known gynecologic malignancies undergoing midline laparotomy who received TAP block with liposomal bupivacaine versus surgical site infiltration of liposomal bupivacaine.
Primary outcome: Total postoperative opioid consumption as measured by morphine equivalents over 48 hour period.
Secondary outcomes include: Pain scores (based on visual analog scale 1-10) at 2 hours, 6 hours, 12 hours, 24 hours and 48 hours postoperatively at rest and upon exertion (Valsalva maneuver), Severity of nausea, Episodes of vomiting, Total antiemetics consumption over 48 hour period.
Primary outcome: Total postoperative opioid consumption as measured by morphine equivalents over 48 hour period.
Secondary outcomes include: Pain scores (based on visual analog scale 1-10) at 2 hours, 6 hours, 12 hours, 24 hours and 48 hours postoperatively at rest and upon exertion (Valsalva maneuver), Severity of nausea, Episodes of vomiting, Total antiemetics consumption over 48 hour period.
Start Date05 Jul 2018 |
Sponsor / Collaborator |
100 Clinical Results associated with Danbury Hospital
Login to view more data
0 Patents (Medical) associated with Danbury Hospital
Login to view more data
582
Literatures (Medical) associated with Danbury Hospital01 Oct 2025·Case reports in women's health
Isthmic tubal ectopic pregnancy from a partial molar pregnancy: A case report and literature review
Article
Author: Hurd, Molly ; Vuong, Richard Q ; Brzozowski, Nicole ; Tek, Zeynep
While tubal ectopic pregnancies and molar pregnancies are relatively common, tubal molar pregnancies are exceptionally rare, with an estimated incidence of 1.5 per 1,000,000 pregnancies. Molar pregnancies are at risk for developing malignant gestational trophoblastic neoplasia (15-20 % for complete hydatidiform moles and 0.5-6 % for partial hydatidiform moles) and warrant robust diagnostic workup to determine appropriate management. Presented here is a case of an isthmic tubal ectopic pregnancy secondary to a partial hydatidiform mole; additionally, a literature review through PubMed discusses all tubal molar pregnancies reported within a 5-year period. A 41-year-old woman (gravida 2, para 0, aborta 1) at 6 weeks and 5 days of gestation presented to the emergency department from the outpatient clinic because prenatal ultrasound did not show an intrauterine pregnancy and her a __-mml:math xmlns:mml="http://www.w3.org/1998/Math/MathML"-__β -hCG level was 17,913 mIU/mL. Due to concern for ectopic pregnancy, she underwent diagnostic laparoscopy, which revealed an unruptured right isthmic tubal ectopic gestation. The specimen was removed and sent for histological evaluation, which confirmed a partial hydatidiform mole that stained positive for p57; the finding was supported by molecular studies. The patient was discharged the same day and follow-up __-mml:math xmlns:mml="http://www.w3.org/1998/Math/MathML"-__β -hCG levels were monitored weekly until undetectable. The literature review found that 13 tubal molar pregnancies had been reported between 2019 and 2024. Histopathologic examination of gestational trophoblastic disease should be supported by ancillary studies such as immunohistochemical, flow cytometry, and molecular analyses to ensure accurate diagnosis. Magnetic resonance imaging could offer a way to preoperatively diagnose molar ectopic pregnancy in select hemodynamically stable patients.
01 Aug 2025·AMERICAN JOURNAL OF SURGERY
Inclusive excellence in surgery: From recognition to transformation
Author: Moronta, Shaidy ; McMullin, Jessica Liu
19 Jul 2025·ANNALS OF SURGICAL ONCOLOGY
Is This the Right Link? How TikTok Views Oncoplastic Breast Surgery.
Article
Author: Aiello, Caterina ; Boolbol, Susan K ; Eum, Joyce L ; Anderson, Carinne W ; Smilen, Sydney H ; Pandya, Deep
BACKGROUND:
Patients are increasingly turning to online social media networks for healthcare information. This study evaluated content related to oncoplastic breast surgery found on TikTok.
METHODS:
The top 50 videos were retrieved from subsequent TikTok searches for 'oncoplastic breast surgery', 'oncoplastics', and 'oncoplastic surgery'. These videos were compiled and the 50 with the most views were selected. Video characteristics were abstracted, and the videos were analyzed for thematic content by three surgeons and graded for educational value by eight individuals of varying backgrounds.
RESULTS:
We focused our analysis on the two most common creator types: surgeons and patients. Both groups showed comparable audience engagement patterns, with no significant difference in the number of views, likes, or comments. However, subscribers, saves, and shares differed significantly, with surgeons showing higher numbers (p < 0.05). Analyzing thematic content by creator type highlights different priorities between the groups. Surgeon videos received significantly higher ratings on questions about providing accurate medical information (p < 0.01) and explaining surgery outcomes clearly (p < 0.05). Surgeons and trainees consistently noted these differences, with 70% of their ratings showing significance in favor of surgeon content. In contrast, non-healthcare raters showed fewer significant distinctions, with only 40% of their ratings identifying differences between creator groups.
CONCLUSION:
While patient creators focus heavily on personal experiences and survivorship, surgeon-created content emphasizes medical accuracy and detailed surgical information. Surgeons can use these findings to better understand the types of information their patients are accessing and to tailor their own educational efforts accordingly.
4
News (Medical) associated with Danbury Hospital30 May 2025
This year’s grantees represent a diverse and innovative group of researchers and institutions across the country, all working to change the trajectory of breast cancer”
— Karen Colella, BCA President.
GREENWICH, CT, CT, UNITED STATES, May 30, 2025 /
EINPresswire.com
/ --
Breast Cancer Alliance
(BCA), one of the nation’s leading and most impactful nonprofit breast cancer organizations, proudly announces the awarding of $1.3 million in 2025 grants supporting groundbreaking research, breast surgical oncology fellowships, and expanded access to screening and diagnostic services for underserved communities. Since its inception in 1996, BCA has invested over $37 million in grants supporting its mission to improve survival rates and quality of life for those impacted by breast cancer.
This year’s grantees represent a diverse and innovative group of researchers and institutions across the country, all working to change the trajectory of breast cancer,” said Karen Colella, BCA President. “From bold scientific research and targeted therapies to specialized breast surgical training and life-saving community screenings, these grants reflect the full spectrum of BCA’s mission. We are deeply grateful to our generous donors, sponsors, corporate partners, and collaborating institutions whose collective belief in our mission makes this impact possible.”
BCA’s 2025 GRANT RECIPIENTS:
Exceptional Project Research Grant Recipients
Awarded to established investigators pursuing innovative, high-impact research in breast cancer.
- Pietro Genovese, PhD, Boston Children’s Hospital, Boston, MA, Redirecting B cell specificity to improve immunotherapy of breast cancer, Deborah G. Black Memorial Research Grant
- Claudia Fischbach-Teschl, PhD, Cornell University, Ithaca, NY, Seizing control: Matrix regulation of breast cancer bone metastasis
- Agnel Sfeir, PhD, Memorial Sloan Kettering Cancer Center, New York, NY, Investigating the impact of mutagenic DNA repair by MMEJ on therapy resistance
- Melanie Rutkowski, PhD, University of Virginia, Charlottesville, VA, Defining how the gut microbiome promotes lung-associated metastasis of breast tumor cells
Young Investigator Research Grant Recipients
Seed funding awarded to early-career scientists to help advance novel hypotheses to secure larger long-term funding.
- Xiaojing Huang, MD, PhD, Rockefeller University, New York, NY, Functional consequences of obesity-dependent changes in adipose and tumor macrophage metabolism in breast cancer
- Petria Thompson, MD, PhD, University of California, San Francisco, CA, Targeting CDK2 to develop combinational strategies to target metastatic breast cancer
- Remco Bastiaannet, BSc, MSc, PhD, Washington University in St. Louis, St. Louis, MO, Paving the Way for Combination Therapies in HER2+ Metastatic Breast Cancer Treated with Alpha-Emitter Radiopharmaceutical Therapy
Breast Surgical Oncology Fellowship Recipients
Awarded to Society of Surgical Oncology accredited institutions in NY, NJ, and CT to train future leaders in breast surgery.
- Ichan School of Medicine at Mount Sinai, New York, NY, Andrew Seto, MD, BCA Breast Surgical Oncology Fellowship Grant
- Rutgers University, New Brunswick, NJ, Hannah Naughton, MD, Rodkin Family Breast Surgical Oncology Fellowship Grant
- Yale School of Medicine, New Haven, CT, Alanna Hickey, MD, Pierre Fabre USA Breast Surgical Oncology Fellowship Grant
- Memorial Sloan Kettering Cancer Center, New York, NY, Taylor Maramara, MD, Jane and Alan Batkin Breast Surgical Oncology Fellowship Grant
Screening and Diagnostic Support Grant Recipients
Supporting critical breast cancer screening, diagnostic imaging, and patient navigation services for underserved communities.
- Danbury Hospital & New Milford Hospital, New Milford, CT
- Greenwich Hospital, Greenwich, CT
- Hartford Hospital, Hartford, CT
- Hospital of Central Connecticut, New Britain, CT, Eisai USA Foundation Grant
- Norma F. Pfriem Breast Center / Bridgeport Hospital, Bridgeport, CT, Mitchell Family Grant
- Norwalk Hospital / Whittingham Cancer Center, Norwalk, CT
- St. Vincent’s Medical Center, Bridgeport, CT
- Stamford Hospital, Stamford, CT, Omnicom Group Grant
- White Plains Hospital, White Plains, NY
Claudia Marks
Breast Cancer Alliance
+1 203-861-0014
email us here
Visit us on social media:
LinkedIn
Instagram
TikTok
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability
for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this
article. If you have any complaints or copyright issues related to this article, kindly contact the author above.

Immunotherapy
31 Oct 2022
Neurologists are testing a remote monitoring program to support patients with mild cognitive impairment
POUGHKEEPSIE, N.Y. and DANBURY, Conn., Oct. 31, 2022 /PRNewswire/ -- Nuvance Health is one of the first health systems in the United States to pilot a new remote monitoring technology for patients with mild cognitive impairment (MCI). Neuroglee Connect™ is a virtual neurological specialty care program for clinical care teams to provide ongoing, personalized support for patients with MCI and caregivers from the comfort of their homes.
MCI is an early stage of memory loss or other cognition problems, such as difficulty with language and thinking. According to the Alzheimer's Association, 12% to 18% of people age 60 and older have MCI in the United States. While MCI is not a type of dementia, the Alzheimer's Association estimates 10% to 15% of people with MCI eventually develop dementia every year.
There are currently no approved medications to treat MCI. Current guidelines state that regularly stimulating the brain and adopting healthy lifestyle habits can be supportive to patients with MCI.
The remote monitoring program Nuvance Health has made available through its Neuroscience Institute includes brain-stimulating activities that can measure performance through timely assessments and identify signs of deterioration. A digital dashboard captures this information in real-time for neurologists who can provide ongoing therapy modifications based on real-world data while efficiently tracking each patient's adherence to the program.
"We care deeply about our patients with MCI and their caregivers, and understand how the diagnosis can be extremely worrisome," said Paul Wright, MD, senior vice president and system chair of the Neuroscience Institute at Nuvance Health. "We are passionate about bringing them the latest care options and support, and in particular, leveraging digital innovations that they can access from the comfort and convenience of home."
"Nuvance Health's neurologists will use a digital platform to remotely monitor patients and keep them mentally active with consistent and intense brain activities," said Dr. Wright. "Patients will use an iPad to participate in medically-tested activities to stimulate their brains."
The digital platform offers brain-stimulating activities such as playing games and learning new skills. It also offers memory compensation training, and reminiscing by uploading and viewing personal photographs and videos to trigger memories. In addition, the platform includes content about healthy lifestyle habits, such as eating well, exercising and getting enough sleep.
The remote monitoring program has a digital platform and resources for caregivers because they play a critical role in the management of neurodegenerative conditions. Care partners can monitor a patient's progress through the platform and access education, support, and informational tools for identifying and overcoming MCI-related anxiety and stress.
"The caregiver is also involved as they are a major contributing factor to a patient's well-being," said Dr. Wright. "Our neurologists will support their efforts at home because we now have an objective way to continuously track each patient's condition over time. We can then use the information to inform appropriate, individualized care."
A majority of Nuvance Health patients with MCI have adopted the remote monitoring program during the initial pilot phase. The new technology is currently available at Nuvance Health Neuroscience Institute neurology practices in New York and Connecticut.
Learn more about memory and dementia care at the Nuvance Health Neuroscience Institute.
CONTACT
Amy Forni, Director of External Communications
O: (203) 739-7478 | M: (475) 279-4673 | [email protected]
About Nuvance Health
Nuvance Health is a system of award-winning nonprofit hospitals and outpatient healthcare services throughout the Hudson Valley and western Connecticut, including: Danbury Hospital and its New Milford campus, Norwalk Hospital and Sharon Hospital in Connecticut; Northern Dutchess Hospital, Putnam Hospital and Vassar Brothers Medical Center in New York.
Nuvance Health offers the latest prevention, diagnostic, medical, surgical and rehabilitation services, including through the Cancer, Digestive Health, Heart & Vascular and Neuroscience Institutes; and primary and specialty care services through Nuvance Health Medical Practices. Nuvance Health also provides convenient healthcare through home care, urgent care and telehealth visits.
Visit nuvancehealth.org for more information. TTY: 1-800-421-1220
SOURCE Nuvance Health
14 Jul 2022
GIG HARBOR, Wash., July 14, 2022 /PRNewswire/ -- James D. Atkisson, MD, is being recognized by Continental Who's Who as a Top Physician for his distinguished career in Palliative Medicine and in acknowledgment of his work at Franciscan Hospice and Palliative Care.
Dr. James D. Atkisson has worked as a Palliative Medicine Specialist for over 38 years. He has practiced at Franciscan Hospice and Palliative Care for the past fifteen years, located at 2901 Bridgeport Way West in University Place, WA.
Continue Reading
James D. Atkisson
Dr. Atkisson has always wanted to be a doctor and help people. He was first inspired after witnessing a childhood friend who hurt his leg while playing. He constructed a splint for his friend to help him walk, and this was when he knew he would pursue a career as a physician when he grew up.
To attain his college education, Dr. Atkisson attended the University of Cincinnati College of Medicine in 1976. He then completed a General Surgery Residency at AMI Presbyterian Denver Hospital. Dr. Atkisson then did two Internal Medicine residencies at Danbury Hospital in 1980 and Greenwich Hospital in 1982. He is a Fellow of the American College of Physicians (FACP) and is board-certified in Internal Medicine by the American Board of Internal Medicine (ABIM). The ABIM is a group led by physicians to evaluate doctors who achieve high standards in Internal Medicine healthcare.
Dr. Atkisson currently works in Hospital and Palliative Medicine at Franciscan Hospice and Palliative Care in University Place, WA. He understands the family's emotional pain when their loved ones are diagnosed with a terminal illness or decide to remove themselves from medical treatment. He works to make the patient's final days comfortable, relieve pain, and support their family.
Dr. Atkisson mainly focuses on quality of life care, working closely with the Hospice Team to support patients and minimize their discomfort. He tries to reduce the patient's pain levels so they may spend time with their family in a relaxed environment after they stop receiving medical treatment. Dr. Atkisson enjoys working in this field to help his patients optimize their quality of life.
On a personal note, Dr. Atkisson loves to travel the world and spend time in the great outdoors. He would like to dedicate this honorable recognition to his Chemistry Professor and great mentor at the University of Kansas, Earl Huyser.
For more information, visit .
Contact: Katherine Green, 516-825-5634, [email protected]
SOURCE Continental Who's Who
100 Deals associated with Danbury Hospital
Login to view more data
100 Translational Medicine associated with Danbury Hospital
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 14 Dec 2025
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or
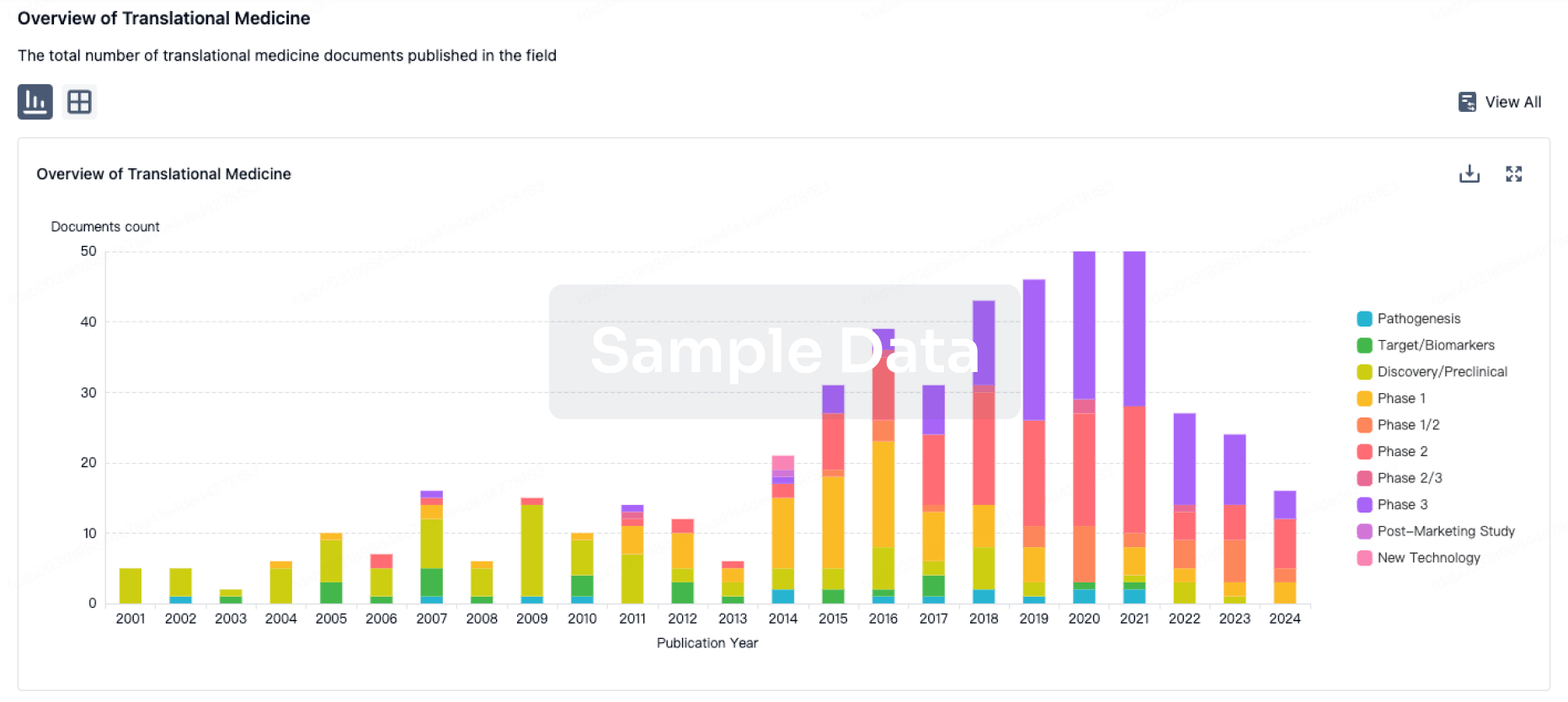
Translational Medicine
Boost your research with our translational medicine data.
login
or
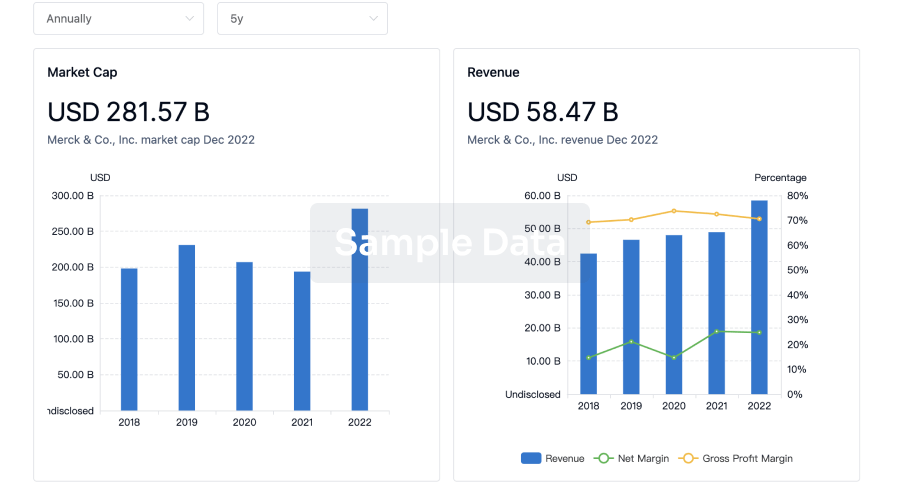
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
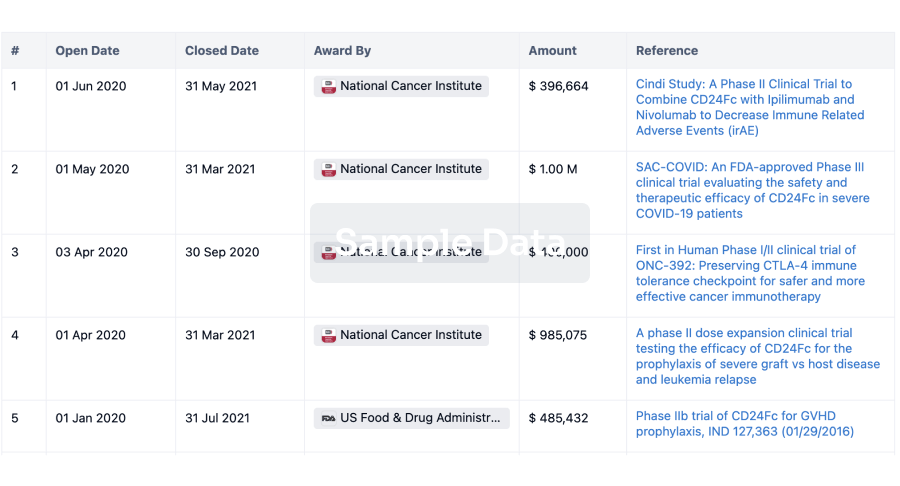
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
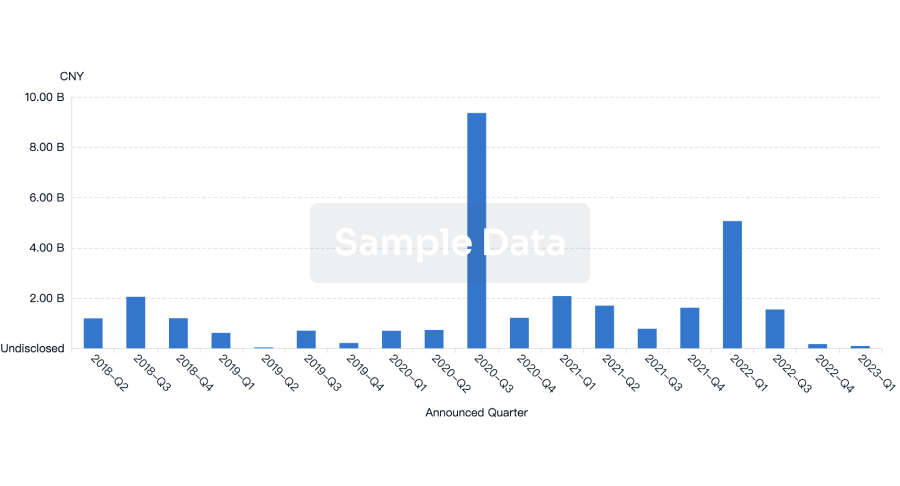
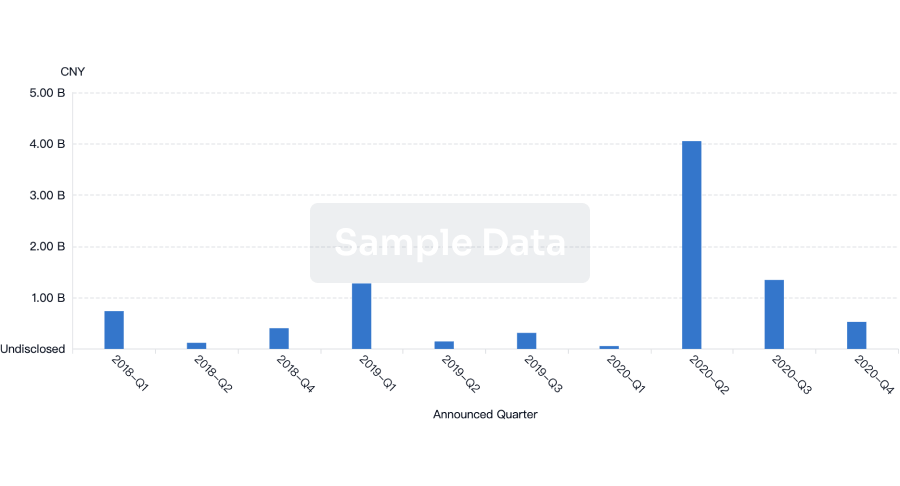
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free