Request Demo
Last update 08 May 2025
Fortis Memorial Research Institute
Last update 08 May 2025
Overview
Related
4
Clinical Trials associated with Fortis Memorial Research InstituteCTRI/2020/04/024567
Assessment of optic nerve sheath diameter measured by bedside sonography as a predictor of raised intracranial pressure in adults.
Start Date16 Apr 2020 |
Sponsor / Collaborator |
CTRI/2020/03/024343
Comparison of ceftazidime-avibactam plus aztreonam with meropenem plus colistin in Intensive Care Unit patients with Extensively drug resistant (XDR) Gram-Negative Bacterial (GNB) infection- a Prospective Observational study
Start Date01 Apr 2020 |
Sponsor / Collaborator |
CTRI/2019/01/017371
COMPARATIVE EVALUATION OF CISATRACURIUM AND ATRACURIUM IN PATIENTS UNDERGOING ABDOMINAL LAPAROSCOPIC SURGERIES - cisatracurium
Start Date31 Jan 2019 |
Sponsor / Collaborator |
100 Clinical Results associated with Fortis Memorial Research Institute
Login to view more data
0 Patents (Medical) associated with Fortis Memorial Research Institute
Login to view more data
460
Literatures (Medical) associated with Fortis Memorial Research Institute01 May 2025·Magnetic Resonance Imaging
Large blood vessel segmentation in quantitative DCE-MRI of brain tumors: A Swin UNETR approach
Article
Author: Sheikh, Mohammad Tufail ; Kesari, Anshika ; Gupta, Rakesh Kumar ; Maurya, Satyajit ; Singh, Anup
01 Apr 2025·Gastrointestinal Endoscopy
BULLET IN CBD- A RARE CAUSE OF JAUNDICE
Article
Author: Khanna, Deepanshu ; Khurana, Arvind Kumar
10 Mar 2025·International Journal for Quality in Health Care
HemeTEAM India: together everyone achieves more
Article
Author: Arora, Sunisha ; Sharma, Kiran ; Singh, Shikha ; Verma, Kanika ; Shrinidhi, Nathany ; Rudrakumar, Karthika ; Paritosh, Garg ; Dorothy, Veronica ; Bhayana, Swati ; Dua, Vikas ; Saxena, Poonam ; Jaiswal, Akash ; Varma, Haristuti ; Garg, Ritu ; Singh, Surbhi ; Chakraborty, Sohini ; Kumar, Nikhil M ; Kothari, Aakriti ; Gupta, Aastha ; Danewa, Arun ; Arora, Madhur ; Bhargava, Rahul ; Mahajan, Prerna ; Singh, Sukhdeep ; Rastogi, Neha Panda ; Swaminathan, Anusha ; Saini, Manish ; Yadav, Chitresh ; Soni, Richa
2
News (Medical) associated with Fortis Memorial Research Institute21 Feb 2025
Phase 3 ASTRO study achieves primary and all secondary endpoints at Week 12 in ulcerative colitis patients
The only SC induction data for an IL-23 inhibitor show statistically significant and clinically meaningful improvements across clinical and endoscopic measures versus placebo, consistent with IV induction
SPRING HOUSE, Pa., Feb. 21, 2025 /PRNewswire/ -- Johnson & Johnson (NYSE: JNJ) today announced data from the Phase 3 ASTRO study of TREMFYA® (guselkumab) subcutaneous (SC) induction therapy in adults with moderately to severely active ulcerative colitis (UC) at the 20th Congress of the European Crohn's and Colitis Organization (ECCO). Study findings through Week 12 showed statistically significant and clinically meaningful improvements compared to placebo across all clinical and endoscopic measures consistent with the U.S. Food and Drug Administration (FDA)-approved intravenous (IV) induction regimen in this population.1
"The Week 12 results from the ASTRO study build on data from the QUASAR study demonstrating that both guselkumab SC and IV induction achieved clinically differentiated results in patients with moderately to severely active UC," said Laurent Peyrin-Biroulet, M.D., Ph.D., Head of the Inflammatory Bowel Disease (IBD) Unit at Nancy University Hospital in France and study investigator.a "The flexibility of a fully SC treatment regimen would be a welcome option for many patients, especially those with busy and active lifestyles."
At Week 12, significantly greater proportions of patients treated with TREMFYA® 400 mg SC induction compared with patients receiving placebo achieved all of the following multiplicity-controlled endpoints:
Clinical remission (27.6% vs 6.5%; P<0.001)b Clinical response (65.6% vs 34.5%; P<0.001)c Endoscopic improvement (37.3% vs 12.9%; P<0.001)d
In prespecified analyses of subpopulations defined by prior advanced therapy treatment status, TREMFYA® demonstrated statistically significant results across endpoints in both biologic and JAK inhibitor-naïve and biologic and JAK inhibitor-refractory patients.
Safety data from the ASTRO study were consistent with the well-established safety profile of TREMFYA®. The proportions of patients with ≥1 adverse event (AE), serious AE, or AE leading to treatment discontinuation were similar across the TREMFYA® and placebo treatment groups.
"We aim to offer treatment options for patients with IBD that allow them to effectively manage their disease while also meeting the daily demands of life. These results further underscore the potential of TREMFYA to transform the UC treatment paradigm," said Esi Lamousé-Smith, M.D., Ph.D., Vice President, Gastroenterology Disease Area Lead, Immunology, Johnson & Johnson Innovative Medicine. "Pending approval, TREMFYA would be the first IL-23 inhibitor with a fully SC induction and maintenance regimen, increasing options for both patients and healthcare providers."
TREMFYA® is the first and only approved fully-human, dual-acting monoclonal antibody that blocks IL-23 while also binding to CD64, a receptor on cells that produce IL-23. IL-23 is a cytokine secreted by activated monocyte/macrophages and dendritic cells that is known to be a driver of immune-mediated diseases including UC.1,2,3,4,5
Applications seeking approval of TREMFYA® for both UC and Crohn's disease (CD) have been submitted in Europe. TREMFYA® received FDA approval in September 2024 for the treatment of adult patients with moderately to severely active UC and is currently administered via an IV induction regimen, followed by a SC maintenance regimen. In November 2024, a supplemental Biologics License Application (sBLA) was submitted to the FDA seeking approval of a SC induction regimen of TREMFYA® for the treatment of adults with moderately to severely active UC. An application for the treatment of adults with moderately to severely active CD has also been submitted in the U.S.
For a full list of all data being presented at ECCO visit: https://innovativemedicine.jnj.com/our-innovation/focus-areas/immunology/gastroenterology/gastroenterology-newsroom
Editor's Notes:
a. Dr. Peyrin-Biroulet is a paid consultant for Johnson & Johnson. He has not been compensated for any media work.b. Clinical remission is defined as a Mayo stool frequency subscore of 0 or 1 and not increased from baseline, a Mayo rectal bleeding subscore of 0, and a Mayo endoscopic subscore of 0, or 1 with no friability present on the endoscopy.c. Clinical response was defined as a decrease from induction baseline in the modified Mayo score by ≥30 percent and ≥2 points, with either a ≥1-point decrease from baseline in the rectal bleeding subscore or a rectal bleeding subscore of 0 or 1.d. Endoscopic improvement was defined as an endoscopy subscore of 0 or 1 with no friability present on the endoscopy.
ABOUT THE ASTRO STUDY (NCT05528510)
ASTRO is a randomized, double-blind, placebo-controlled, parallel-group, multicenter, treat-through Phase 3 study designed to evaluate the efficacy and safety of TREMFYA® SC induction therapy (400 mg at Weeks 0, 4, and 8) in adults with moderately to severely active ulcerative colitis who had an inadequate response or intolerance to conventional therapy (e.g., thiopurines or corticosteroids), prior biologics (TNF antagonists or vedolizumab) and/or ozanimod or approved JAK inhibitors. Patients (n = 418) were randomized 1:1:1 to receive TREMFYA® 400 mg SC induction at Weeks 0, 4 and 8 followed by TREMFYA® 200 mg SC every 4 weeks (q4w); or TREMFYA® 400 mg SC induction at Weeks 0, 4 and 8, followed by TREMFYA® 100 mg SC every 8 weeks (q8w); or placebo. The maintenance dose regimens in ASTRO (200 mg SC q4w and 100 mg SC q8w) are the same as those evaluated in the Phase 3 QUASAR program which established the efficacy and safety profile of IV induction followed by SC maintenance therapy in patients with moderate to severely active UC.6
ABOUT THE QUASAR PROGRAM (NCT04033445)
QUASAR is a randomized, double-blind, placebo-controlled, parallel group, multicenter, Phase 2b/3 program designed to evaluate the efficacy and safety of TREMFYA® in adults with moderately to severely active ulcerative colitis who had an inadequate response or intolerance to conventional therapy (e.g., thiopurines or corticosteroids), prior biologics (TNF antagonists or vedolizumab) and/or JAK inhibitors (tofacitinib). QUASAR included a Phase 2b dose-ranging induction study, a confirmatory Phase 3 induction study, and a Phase 3 randomized withdrawal maintenance study. In the Phase 3 induction study, patients received either TREMFYA® 200 mg or placebo by IV infusion at Weeks 0, 4, and 8. In the Phase 3 maintenance study, patients received a SC maintenance regimen of either TREMFYA® 200 mg q4w, TREMFYA® 100 mg q8w, or placebo.7
ABOUT ULCERATIVE COLITIS
Ulcerative colitis (UC) is a chronic disease of the large intestine, also known as the colon, in which the lining of the colon becomes inflamed and develops tiny open sores, or ulcers, that produce pus and mucus. It is the result of the immune system's overactive response. Symptoms vary but may typically include loose and more urgent bowel movements, rectal bleeding or bloody stool, persistent diarrhea, abdominal pain, loss of appetite, weight loss, and fatigue.8
ABOUT CROHN'S DISEASE
Crohn's disease is one of the two main forms of inflammatory bowel disease, which affects an estimated three million Americans.9 Crohn's disease is a chronic inflammatory condition of the gastrointestinal tract with no known cause, but the disease is associated with abnormalities of the immune system that could be triggered by a genetic predisposition, diet, or other environmental factors. Symptoms of Crohn's disease can vary, but often include abdominal pain and tenderness, frequent diarrhea, rectal bleeding, weight loss, and fever.10
ABOUT TREMFYA® (guselkumab)
Developed by Johnson & Johnson, TREMFYA® is the first approved fully-human, dual-acting monoclonal antibody designed to neutralize inflammation at the cellular source by blocking IL-23 and binding to CD64 (a receptor on cell that produce IL-23). Findings for dual-acting are limited to in vitro studies that demonstrate guselkumab binds to CD64, which is expressed on the surface of IL-23 producing cells in an inflammatory monocyte model. The clinical significance of this finding is not known.
TREMFYA® is a prescription medicine approved in the U.S. to treat:
adults with moderate to severe plaque psoriasis who may benefit from taking injections or pills (systemic therapy) or phototherapy (treatment using ultraviolet or UV light). adults with active psoriatic arthritis. adults with moderately to severely active ulcerative colitis.2
TREMFYA® is approved Europe, Canada, Japan, and a number of other countries for the treatment of adults with moderate-to-severe plaque psoriasis and for the treatment of adults with active psoriatic arthritis.
Johnson & Johnson maintains exclusive worldwide marketing rights to TREMFYA®. For more information, visit: www.tremfya.com.
IMPORTANT SAFETY INFORMATIONWhat is the most important information I should know about TREMFYA® (guselkumab)?
TREMFYA® is a prescription medicine that may cause serious side effects, including:
Serious Allergic Reactions. Stop using TREMFYA® and get emergency medical help right away if you develop any of the following symptoms of a serious allergic reaction:
fainting, dizziness, feeling lightheaded (low blood pressure)
swelling of your face, eyelids, lips, mouth, tongue, or throat
trouble breathing or throat tightness
chest tightness
skin rash, hives
itching
Infections. TREMFYA® may lower the ability of your immune system to fight infections and may increase your risk of infections. Your healthcare provider should check you for infections and tuberculosis (TB) before starting treatment with TREMFYA® and may treat you for TB before you begin treatment with TREMFYA® if you have a history of TB or have active TB. Your healthcare provider should watch you closely for signs and symptoms of TB during and after treatment with TREMFYA®.
Tell your healthcare provider right away if you have an infection or have symptoms of an infection, including:
fever, sweats, or chills
muscle aches
weight loss
cough
warm, red, or painful skin or sores on your body different from your psoriasis
diarrhea or stomach pain
shortness of breath
blood in your phlegm (mucus)
burning when you urinate or urinating more often than normal
Do not take TREMFYA® if you have had a serious allergic reaction to guselkumab or any of the ingredients in TREMFYA®.
Before using TREMFYA®, tell your healthcare provider about all of your medical conditions, including if you:
have any of the conditions or symptoms listed in the section "What is the most important information I should know about TREMFYA®?" have an infection that does not go away or that keeps coming back. have TB or have been in close contact with someone with TB. have recently received or are scheduled to receive an immunization (vaccine). You should avoid receiving live vaccines during treatment with TREMFYA®. are pregnant or plan to become pregnant. It is not known if TREMFYA® can harm your unborn baby.Pregnancy Registry: If you become pregnant during treatment with TREMFYA®, talk to your healthcare provider about registering in the pregnancy exposure registry for TREMFYA®. You can enroll by visiting www.mothertobaby.org/ongoing-study/tremfya-guselkumab, by calling 1-877-311-8972, or emailing MotherToBaby@health.ucsd.edu. The purpose of this registry is to collect information about the safety of TREMFYA® during pregnancy. are breastfeeding or plan to breastfeed. It is not known if TREMFYA® passes into your breast milk.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
What are the possible side effects of TREMFYA®?
TREMFYA® may cause serious side effects. See "What is the most important information I should know about TREMFYA®?"
The most common side effects of TREMFYA® include respiratory tract infections, headache, injection site reactions, joint pain (arthralgia), diarrhea, stomach flu (gastroenteritis), fungal skin infections, herpes simplex infections, and bronchitis.
These are not all the possible side effects of TREMFYA®. Call your doctor for medical advice about side effects.
Use TREMFYA® exactly as your healthcare provider tells you to use it.
Please read the full Prescribing Information, including Medication Guide, for TREMFYA® and discuss any questions that you have with your doctor.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch, or call 1-800-FDA-1088.
Dosage Forms and Strengths: TREMFYA® is available in a 100 mg/mL prefilled syringe and One-Press patient-controlled injector for subcutaneous injection, a 200 mg/2 mL prefilled syringe and prefilled pen (TREMFYA® PEN) for subcutaneous injection, and a 200 mg/20 mL (10 mg/mL) single dose vial for intravenous infusion.
ABOUT JOHNSON & JOHNSON
At Johnson & Johnson, we believe health is everything. Our strength in healthcare innovation empowers us to build a world where complex diseases are prevented, treated, and cured, where treatments are smarter and less invasive, and solutions are personal. Through our expertise in Innovative Medicine and MedTech, we are uniquely positioned to innovate across the full spectrum of healthcare solutions today to deliver the breakthroughs of tomorrow, and profoundly impact health for humanity.
Learn more at https://www.jnj.com/ or at www.innovativemedicine.jnj.com
Follow us at @JNJInnovMed.
Janssen Research & Development, LLC and Janssen Biotech, Inc. are Johnson & Johnson companies.
Cautions Concerning Forward-Looking Statements
This press release contains "forward-looking statements" as defined in the Private Securities Litigation Reform Act of 1995 regarding TREMFYA®. The reader is cautioned not to rely on these forward-looking statements. These statements are based on current expectations of future events. If underlying assumptions prove inaccurate or known or unknown risks or uncertainties materialize, actual results could vary materially from the expectations and projections of Janssen Research & Development, LLC, Janssen Biotech, Inc., Janssen-Cilag International NV and/or Johnson & Johnson. Risks and uncertainties include, but are not limited to: challenges and uncertainties inherent in product research and development, including the uncertainty of clinical success and of obtaining regulatory approvals; uncertainty of commercial success; manufacturing difficulties and delays; competition, including technological advances, new products and patents attained by competitors; challenges to patents; product efficacy or safety concerns resulting in product recalls or regulatory action; changes in behavior and spending patterns of purchasers of health care products and services; changes to applicable laws and regulations, including global health care reforms; and trends toward health care cost containment. A further list and descriptions of these risks, uncertainties and other factors can be found in Johnson & Johnson's most recent Annual Report on Form 10-K, including in the sections captioned "Cautionary Note Regarding Forward-Looking Statements" and "Item 1A. Risk Factors," and in Johnson & Johnson's subsequent Quarterly Reports on Form 10-Q and other filings with the Securities and Exchange Commission. Copies of these filings are available online at www.sec.gov, www.jnj.com or on request from Johnson & Johnson. None of Janssen Research & Development, LLC, Janssen Biotech, Inc., Janssen-Cilag International NV nor Johnson & Johnson undertakes to update any forward-looking statement as a result of new information or future events or developments.
1 Peyrin-Biroulet, et al. Efficacy and safety of subcutaneous guselkumab induction therapy in patients with Ulcerative Colitis: Results through week 12 from the phase 3 ASTRO study. Results from the Phase 3 ASTRO study. Oral presentation (#OP10) at the 20th Congress of the European Crohn's and Colitis Organization (ECCO). February 2025.2 Kreuger JG, Eyerich K, Kuchroo VK. Il-23 past, present, and future: a roadmap to advancing IL-23 science and therapy. Front Immunol. 2024; 15:1331217. doi:10.3389/fimmu.2024.13312173 TREMFYA® Prescribing Information. Available at: https://www.janssenlabels.com/package-insert/product-monograph/prescribing-information/TREMFYA-pi.pdf Accessed October 2024.4 Skyrizi® [Prescribing Information]. North Chicago, IL: AbbVie, Inc.5 Omvoh™ [Prescribing Information]. Indianapolis, IN: Eli Lilly and Company.6 National Institutes of Health: Clinicaltrials.gov. A Study of Guselkumab Therapy in Participants With Moderately to Severely Active Ulcerative Colitis (ASTRO). Identifier: NCT05528510. https://clinicaltrials.gov/study/NCT05528510?term=astro&intr=guselkumab&rank=1. Accessed January 2025.7 National Institutes of Health: Clinicaltrials.gov. A Study of Guselkumab in Participants With Moderately to Severely Active Ulcerative Colitis (QUASAR). Identifier: NCT04033445. https://classic.clinicaltrials.gov/ct2/show/NCT04033445. Accessed January 2025.8 Crohn's & Colitis Foundation. What is ulcerative colitis? Available at: https://www.crohnscolitisfoundation.org/what-is-ulcerative-colitis. Accessed April 2024.9 Crohn's & Colitis Foundation. Overview of Crohn's disease. Available at: https://www.crohnscolitisfoundation.org/what-is-crohns-disease/overview. Accessed October 2024.10 Crohn's & Colitis Foundation. Signs and symptoms of Crohn's disease. Available at https://www.crohnscolitisfoundation.org/patientsandcaregivers/what-is-crohns-disease/symptoms. Accessed October 2024.
Media contact:Craig Stoltz
cstoltz@its.jnj.com
Investor contact:Lauren Johnsoninvestor-relations@its.jnj.com
View original content to download multimedia:https://www.prnewswire.com/news-releases/tremfya-guselkumab-subcutaneous-sc-induction-data-support-potential-to-be-the-first-and-only-in-its-class-to-offer-the-option-of-both-intravenous-and-sc-induction-therapy-in-ulcerative-colitis-302381823.html
SOURCE Johnson & Johnson
Clinical ResultPhase 3Drug Approval
12 Oct 2023
GURUGRAM, India, Oct. 12, 2023 /PRNewswire/ -- Doctors at FMRI, India successfully conducted bone marrow transplants on 3 Iraqi thalassemia patients from the same family, aged 10, 13, and 19 years respectively. All three youngsters were detected at an early age with thalassemia major in Iraq. After being admitted to FMRI, under the expert care of
Dr Vikas Dua, Principal Director & Head, Paediatric Haematology, Paediatric Haemato Oncology & BMT, Fortis Memorial Research Institute, alongwith his team of expert doctors, the patients underwent matched sibling donor Hematopoietic stem cell transplant.
Continue Reading
Patients along with the team of doctors at Fortis Memorial Research Institute, Gurugram
Further explaining the complexity of the procedures,
Dr Dua said, "Since thalassemia patients require monthly blood transfusions from a very early age of about six months, they develop severe iron overload as the years pass by, increasing the complexity of the bone marrow transplant procedure."
The family of the 3 Iraqi patients was counseled and explained in detail about all the pros and cons pertaining to stem cell transplant. After getting informed consent, all three were admitted for a matched sibling donor stem cell transplant, which went off successfully. The donors had also come all the way from Iraq to help save their siblings. All three patients were discharged within 14 days of being admitted.
Thalassemia is an inherited blood disorder that is passed on through genes from the parents to their children and it causes the body to have less hemoglobin than normal. These 3 bone marrow transplants are a testimony to the availability of advanced medical infrastructure and affordable treatment options in India for thalassemia patients, though unfortunately, there is very little awareness of the same.
Speaking about the rare BMT procedure, Dr
Vikas Dua said, "The uniqueness about these 3 patients was their younger age. All the patients had severe iron overload due to blood transfusions from an early age after diagnosis. This can lead to heart and liver damage. What people need to understand is that the earlier the patients undergo BMT, the better is their chances of survival with minimal complexities."
Dr Rahul Bhargava, Principal Director & Chief BMT, Fortis Memorial Research Institute, Gurugram, India said, "India has the largest number of children with Thalassemia major in the world – about 1 to 1.5 lakh patients and almost 42 million thalassemia carriers. Given the alarming figures, there's little awareness of the treatments and facilities available to treat thalassemia. Fortis Gurugram has a dedicated team of Hematologists alongwith the best of medical infrastructure to treat the most complex cases. Timely treatment and diagnosis are the key to recovery in critically ill Thalassemic patients."
Contact
Ajey Maharaj
[email protected]
Photo:
Logo:
SOURCE Fortis Healthcare
100 Deals associated with Fortis Memorial Research Institute
Login to view more data
100 Translational Medicine associated with Fortis Memorial Research Institute
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 03 Aug 2025
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or
Translational Medicine
Boost your research with our translational medicine data.
login
or
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
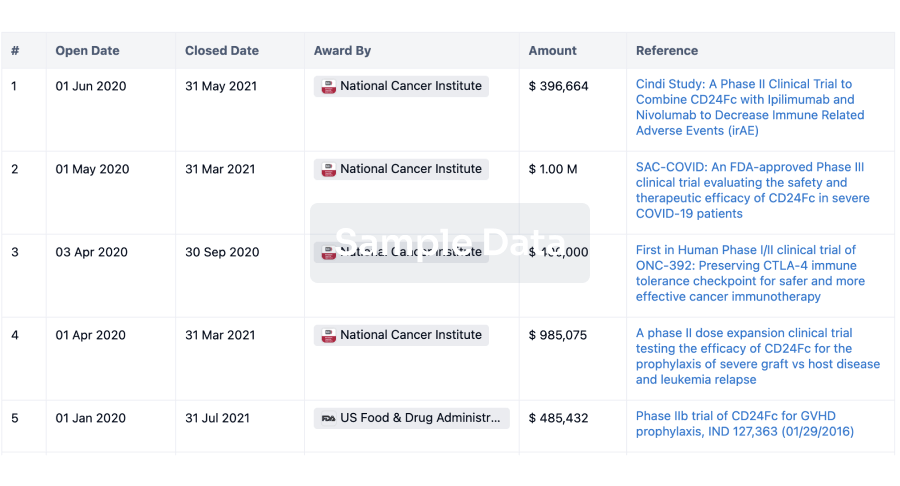
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
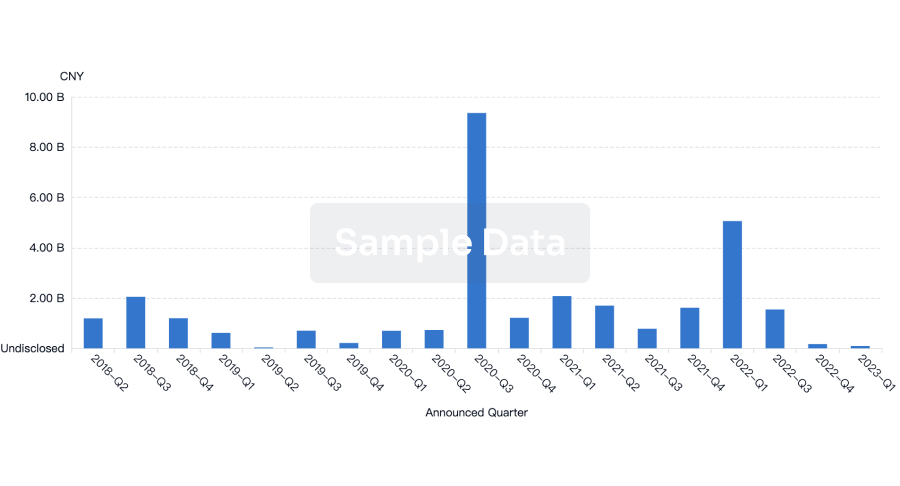
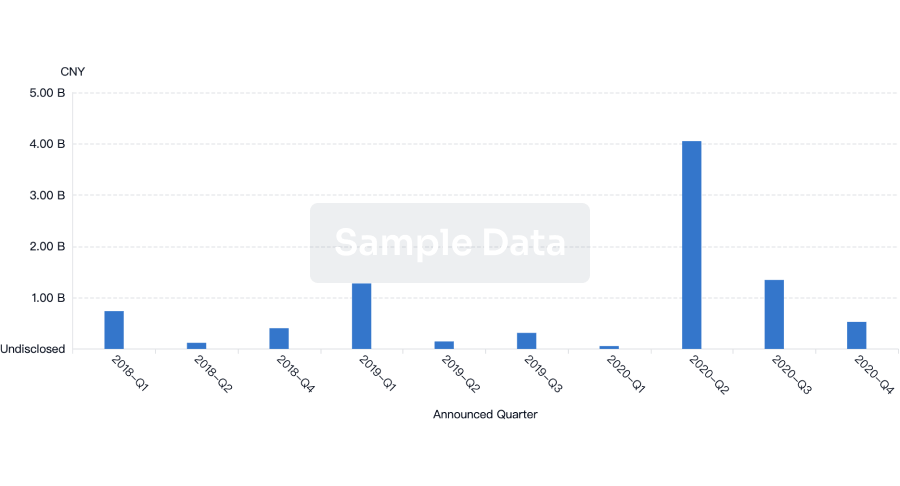
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free