Request Demo
Last update 08 May 2025
IL-6R x ERα
Last update 08 May 2025
Related
1
Drugs associated with IL-6R x ERαTarget |
Mechanism ERα modulators [+1] |
Active Org.- |
Originator Org. |
Active Indication- |
Inactive Indication |
Drug Highest PhaseDiscontinued |
First Approval Ctry. / Loc.- |
First Approval Date20 Jan 1800 |
100 Clinical Results associated with IL-6R x ERα
Login to view more data
100 Translational Medicine associated with IL-6R x ERα
Login to view more data
0 Patents (Medical) associated with IL-6R x ERα
Login to view more data
112
Literatures (Medical) associated with IL-6R x ERα01 Jan 2025·Journal of Cancer
Elucidating the Role of Estrogen Effects in Leukemia: Insights from Single-Cell RNA Sequencing and Mendelian Randomization
Article
Author: Wu, Qibiao ; Sun, Changgang ; Yu, Yang ; Liu, Cun ; Zhuang, Jing ; Zhao, Jiahan ; Sun, Mengxuan ; Liu, Ruijuan
01 Oct 2024·Circulation: Heart Failure
Sex Differences in Skeletal Muscle Pathology in Patients With Heart Failure and Reduced Ejection Fraction
Article
Author: Pereira, Marcelo G. ; Egginton, Stuart ; Roberts, Lee D. ; Wood, Nathanael ; Witte, Klaus K. ; Hendrickse, Paul W. ; Cheng, Chew W. ; Straw, Sam ; Bowen, T. Scott ; Critchlow, Annabel ; Wheatcroft, Stephen B.
02 Jan 2024·Autophagy
The presence of blastocyst within the uteri facilitates lumenal epithelium transformation for implantation via upregulating lysosome proteostasis activity
Article
Author: Wang, Haibin ; Bao, Haili ; Huang, Ziying ; Deng, Wenbo ; Wang, Peike ; Guo, Chuanhui ; Ni, Zhangli ; Deng, Na ; Du, Shuailin ; Kong, Shuangbo ; Lu, Jinhua ; Zhang, Hua
1
News (Medical) associated with IL-6R x ERα28 Mar 2024
On March 26th, the US FDA granted approval for Merck’s WINREVAIR™ (sotatercept-csrk), marking a significant milestone in pulmonary arterial hypertension (PAH) treatment. PAH, characterized by elevated blood pressure in the arteries connecting the heart and lungs, poses a grave risk of heart failure. While pulmonary vasodilators have improved patient prognosis, the challenge of disease progression persists, underscoring the importance of innovative treatments like Sotatercept.
Sotatercept’s Mechanism of Action
Sotatercept introduces a novel paradigm in PAH therapy. It functions as a fusion protein, incorporating the binding site of ACVR2A, thereby disrupting downstream signaling pathways, particularly the SMAD pathway. By sequestering activin, a member of the TGF-β superfamily, Sotatercept reinstates the equilibrium between growth-promoting and growth-inhibiting pathways within the pulmonary arteries.
ACVR2A: Implications Across Disease Spectrum
Beyond its role in PAH, ACVR2A emerges as a pivotal player in the pathogenesis of various ailments. This broad implication positions ACVR2A targeting as a promising strategy in arresting disease progression. Alongside Sotatercept, two other pharmaceutical pipelines are on the cusp of market approval, while six companies are advancing drugs targeting ACVR2A in preclinical phases, addressing conditions ranging from cancer to myelofibrosis.
Sino Biological's offering to support PAH Research
The pursuit of PAH therapeutics primarily revolves around targeting an array of molecular pathways, including ACVRs, BRD4, NF-kB, Nrf2, NFE2L1/Nrf1, mTOR, ASK-1, mineralocorticoid receptor, estrogen receptor, CD20, calcineurin, IL-6R, leukotriene A4 hydrolase, tryptophan hydrolase, and endothelial progenitor cells. Sino Biological plays a pivotal role in this endeavor by supplying recombinant proteins, antibodies, cytokines, and growth factors, catering to diverse research needs across various stages of PAH drug development.
As a leading provider of comprehensive solutions and innovative tools used to advance life science and improve human health, Sino Biological is proud to offer premium products to support researchers in their quest to unlock novel treatments and improve patient outcomes.
Drug ApprovalPatent Expiration
Analysis
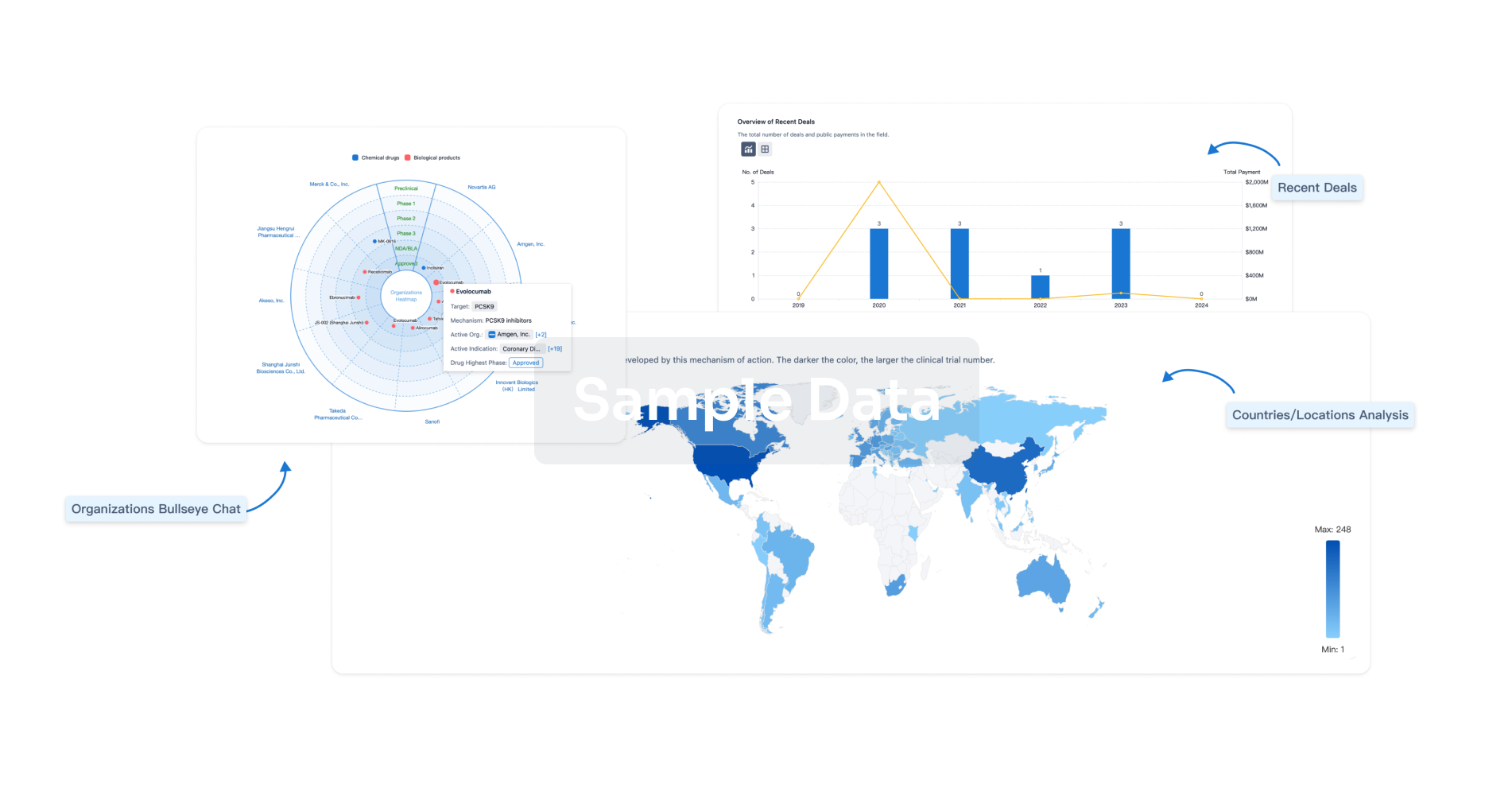
Perform a panoramic analysis of this field.
login
or
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free