Request Demo
Last update 08 May 2025
MMAB
Last update 08 May 2025
Basic Info
Synonyms ATP:co(I)rrinoid adenosyltransferase MMAB, cblB, CFAP23 + [8] |
Introduction Converts cob(I)alamin to adenosylcobalamin (adenosylcob(III)alamin), a coenzyme for methylmalonyl-CoA mutase, therefore participates in the final step of the vitamin B12 conversion (PubMed:12514191). Generates adenosylcobalamin (AdoCbl) and directly delivers the cofactor to MUT in a transfer that is stimulated by ATP-binding to MMAB and gated by MMAA (Probable). |
Related
1
Drugs associated with MMABTarget |
Mechanism MMAB modulators |
Active Org. |
Originator Org. |
Active Indication |
Inactive Indication- |
Drug Highest PhasePreclinical |
First Approval Ctry. / Loc.- |
First Approval Date20 Jan 1800 |
100 Clinical Results associated with MMAB
Login to view more data
100 Translational Medicine associated with MMAB
Login to view more data
0 Patents (Medical) associated with MMAB
Login to view more data
81
Literatures (Medical) associated with MMAB01 Jul 2025·Journal of Affective Disorders
Genetic insights into the role of mitochondria-related genes in mental disorders: An integrative multi-omics analysis
Article
Author: Jia, Xinlei ; Wei, Ya Bin ; Sun, Yaoyao ; Que, Jianyu ; Yu, Lulu ; Cui, Naixue ; Feng, Zhendong ; Zheng, Yi-Ran ; Liu, Jia Jia ; Lu, Yan'e
01 Jan 2025·Progress in Neuro-Psychopharmacology and Biological Psychiatry
Multi-omics data integration reveals novel genes related to autoimmune hypothyroidism in the brain: A molecular basis for the brain–thyroid axis
Article
Author: Gao, Xiao ; Li, Ningjun ; Liu, Jun ; Cui, Weiwei ; Li, Can ; Yu, Hong ; Li, Zuoxi ; Liu, Xuehuan ; Lian, Xinying
01 Dec 2024·Molecular Genetics and Metabolism Reports
Isolated methylmalonic acidemia in Mexico: Genotypic spectrum, report of two novel MMUT variants and a possible synergistic heterozygosity effect
Article
Author: Ortega-Valdez, Enrique ; Fernández-Hernández, Liliana ; Carrillo-Nieto, Rosa Itzel ; Vela-Amieva, Marcela ; López-Mejía, Lizbeth ; Fernández-Lainez, Cynthia ; Alcántara-Ortigoza, Miguel Ángel ; Guillén-López, Sara ; Ridaura-Sanz, Cecilia ; Rojas-Maruri, Mauricio ; Reyna-Fabián, Miriam ; González-del Angel, Ariadna ; González-Del Angel, Ariadna
Analysis
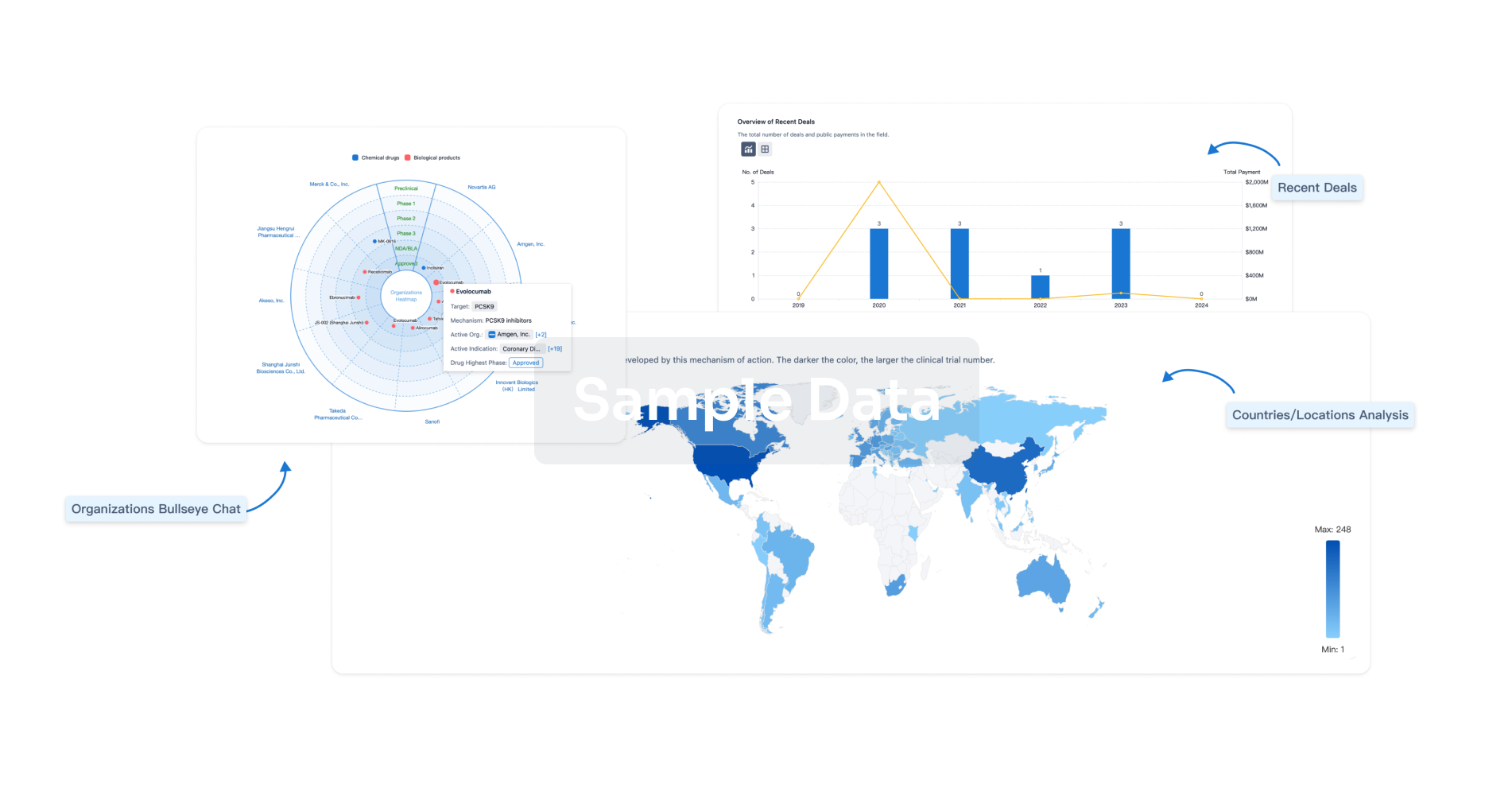
Perform a panoramic analysis of this field.
login
or
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free

