Request Demo
What is Kebuzone used for?
15 June 2024
Kebuzone, a non-steroidal anti-inflammatory drug (NSAID), is widely recognized in the pharmaceutical world for its potent anti-inflammatory and analgesic properties. Known under various trade names, Kebuzone has been instrumental in managing pain and inflammation associated with a range of conditions, including arthritic disorders and musculoskeletal injuries. It primarily targets cyclooxygenase (COX) enzymes, which play a crucial role in the inflammatory process. Research on Kebuzone has been conducted by numerous institutions, and it continues to be a topic of interest due to its therapeutic potential and the ongoing search for effective pain management solutions.
As an NSAID, Kebuzone is used for its ability to reduce inflammation and alleviate pain. Its indications include the treatment of rheumatoid arthritis, osteoarthritis, and other inflammatory conditions. Clinical trials and research studies have demonstrated its efficacy in improving the quality of life for patients suffering from chronic pain and inflammation. The progress in Kebuzone research has been marked by a better understanding of its pharmacodynamics, pharmacokinetics, and the development of formulations that enhance its therapeutic effects while minimizing adverse reactions.
Kebuzone Mechanism of Action
The mechanism of action of Kebuzone involves the inhibition of cyclooxygenase (COX) enzymes, specifically COX-1 and COX-2. COX enzymes are responsible for the conversion of arachidonic acid to prostaglandins, which are lipid compounds that play a key role in the inflammatory response. By inhibiting the activity of these enzymes, Kebuzone effectively reduces the production of prostaglandins, leading to a decrease in inflammation, pain, and fever.
COX-1 is constitutively expressed in most tissues and is involved in maintaining physiological functions such as gastric mucosal protection and platelet aggregation. COX-2, on the other hand, is inducible and is primarily associated with inflammation and pain. Kebuzone's ability to inhibit both COX-1 and COX-2 makes it effective in managing inflammatory conditions, but it also increases the risk of gastrointestinal side effects, which is a common concern with NSAIDs.
The anti-inflammatory effects of Kebuzone are also attributed to its ability to modulate immune responses and reduce the activity of pro-inflammatory cytokines. This dual-action mechanism not only alleviates pain but also addresses the underlying inflammatory processes, making Kebuzone a valuable option for long-term management of chronic inflammatory diseases.
How to Use Kebuzone
Kebuzone is available in various forms, including oral tablets, capsules, and topical formulations. The route of administration and dosage depend on the condition being treated, the severity of symptoms, and the patient's overall health status.
For oral administration, Kebuzone tablets or capsules are usually taken with food to minimize gastrointestinal irritation. The typical dosage for adults ranges from 200 to 400 mg, administered two to three times daily, depending on the clinical response. It is essential to follow the prescribed dosage regimen and not to exceed the recommended dose to avoid potential adverse effects.
Topical formulations of Kebuzone, such as creams or gels, are applied directly to the affected area. This method is particularly useful for localized pain and inflammation, as it allows for targeted delivery of the drug with reduced systemic exposure. The onset of action for topical Kebuzone is generally faster than oral administration, providing quicker relief for acute symptoms.
The onset of action for oral Kebuzone typically occurs within 30 minutes to 1 hour after ingestion, with peak plasma concentrations reached within 2 to 3 hours. The duration of action can vary, but the therapeutic effects generally last for 6 to 8 hours. For sustained relief, it is crucial to adhere to the dosing schedule recommended by the healthcare provider.
What is Kebuzone Side Effects
Like all medications, Kebuzone can cause side effects, although not everyone experiences them. The most common side effects are related to the gastrointestinal system due to its COX-1 inhibitory activity. These include nausea, dyspepsia, abdominal pain, and, in more severe cases, gastrointestinal bleeding or ulcers. To mitigate these effects, it is advisable to take Kebuzone with food or use a gastroprotective agent as recommended by a healthcare provider.
Other potential side effects of Kebuzone include dizziness, headache, and hypersensitivity reactions such as rash or pruritus. In rare cases, more serious adverse effects may occur, such as renal impairment, hepatotoxicity, or cardiovascular events. Patients with pre-existing conditions such as renal or hepatic dysfunction, cardiovascular disease, or a history of gastrointestinal ulcers should use Kebuzone with caution and under strict medical supervision.
Contraindications for Kebuzone use include known hypersensitivity to the drug or other NSAIDs, active gastrointestinal bleeding or ulceration, severe renal or hepatic impairment, and during the third trimester of pregnancy due to the risk of fetal harm. It is also contraindicated in patients with a history of asthma or allergic reactions triggered by aspirin or other NSAIDs.
What Other Drugs Will Affect Kebuzone
Drug interactions can alter the effectiveness of Kebuzone and increase the risk of adverse effects. It is important to inform the healthcare provider of all medications being taken, including prescription, over-the-counter drugs, and supplements.
Concomitant use of Kebuzone with other NSAIDs or corticosteroids can increase the risk of gastrointestinal bleeding and ulceration. Anticoagulants, such as warfarin, can also interact with Kebuzone, enhancing the risk of bleeding. Monitoring coagulation parameters is essential when these drugs are used together.
Kebuzone can reduce the efficacy of antihypertensive medications, such as ACE inhibitors, angiotensin II receptor blockers (ARBs), and diuretics, potentially leading to elevated blood pressure. Additionally, co-administration with lithium or methotrexate may increase the levels of these drugs, raising the risk of toxicity.
Patients taking selective serotonin reuptake inhibitors (SSRIs) or serotonin-norepinephrine reuptake inhibitors (SNRIs) should be cautious, as combining these antidepressants with Kebuzone can further elevate the risk of gastrointestinal bleeding.
In summary, Kebuzone is a valuable NSAID with potent anti-inflammatory and analgesic properties. Its mechanism of action involves the inhibition of COX enzymes, leading to reduced prostaglandin production. While effective in managing pain and inflammation, careful consideration of its side effects and potential drug interactions is necessary to ensure safe and optimal use. Always consult a healthcare provider for personalized advice and recommendations when using Kebuzone.
As an NSAID, Kebuzone is used for its ability to reduce inflammation and alleviate pain. Its indications include the treatment of rheumatoid arthritis, osteoarthritis, and other inflammatory conditions. Clinical trials and research studies have demonstrated its efficacy in improving the quality of life for patients suffering from chronic pain and inflammation. The progress in Kebuzone research has been marked by a better understanding of its pharmacodynamics, pharmacokinetics, and the development of formulations that enhance its therapeutic effects while minimizing adverse reactions.
Kebuzone Mechanism of Action
The mechanism of action of Kebuzone involves the inhibition of cyclooxygenase (COX) enzymes, specifically COX-1 and COX-2. COX enzymes are responsible for the conversion of arachidonic acid to prostaglandins, which are lipid compounds that play a key role in the inflammatory response. By inhibiting the activity of these enzymes, Kebuzone effectively reduces the production of prostaglandins, leading to a decrease in inflammation, pain, and fever.
COX-1 is constitutively expressed in most tissues and is involved in maintaining physiological functions such as gastric mucosal protection and platelet aggregation. COX-2, on the other hand, is inducible and is primarily associated with inflammation and pain. Kebuzone's ability to inhibit both COX-1 and COX-2 makes it effective in managing inflammatory conditions, but it also increases the risk of gastrointestinal side effects, which is a common concern with NSAIDs.
The anti-inflammatory effects of Kebuzone are also attributed to its ability to modulate immune responses and reduce the activity of pro-inflammatory cytokines. This dual-action mechanism not only alleviates pain but also addresses the underlying inflammatory processes, making Kebuzone a valuable option for long-term management of chronic inflammatory diseases.
How to Use Kebuzone
Kebuzone is available in various forms, including oral tablets, capsules, and topical formulations. The route of administration and dosage depend on the condition being treated, the severity of symptoms, and the patient's overall health status.
For oral administration, Kebuzone tablets or capsules are usually taken with food to minimize gastrointestinal irritation. The typical dosage for adults ranges from 200 to 400 mg, administered two to three times daily, depending on the clinical response. It is essential to follow the prescribed dosage regimen and not to exceed the recommended dose to avoid potential adverse effects.
Topical formulations of Kebuzone, such as creams or gels, are applied directly to the affected area. This method is particularly useful for localized pain and inflammation, as it allows for targeted delivery of the drug with reduced systemic exposure. The onset of action for topical Kebuzone is generally faster than oral administration, providing quicker relief for acute symptoms.
The onset of action for oral Kebuzone typically occurs within 30 minutes to 1 hour after ingestion, with peak plasma concentrations reached within 2 to 3 hours. The duration of action can vary, but the therapeutic effects generally last for 6 to 8 hours. For sustained relief, it is crucial to adhere to the dosing schedule recommended by the healthcare provider.
What is Kebuzone Side Effects
Like all medications, Kebuzone can cause side effects, although not everyone experiences them. The most common side effects are related to the gastrointestinal system due to its COX-1 inhibitory activity. These include nausea, dyspepsia, abdominal pain, and, in more severe cases, gastrointestinal bleeding or ulcers. To mitigate these effects, it is advisable to take Kebuzone with food or use a gastroprotective agent as recommended by a healthcare provider.
Other potential side effects of Kebuzone include dizziness, headache, and hypersensitivity reactions such as rash or pruritus. In rare cases, more serious adverse effects may occur, such as renal impairment, hepatotoxicity, or cardiovascular events. Patients with pre-existing conditions such as renal or hepatic dysfunction, cardiovascular disease, or a history of gastrointestinal ulcers should use Kebuzone with caution and under strict medical supervision.
Contraindications for Kebuzone use include known hypersensitivity to the drug or other NSAIDs, active gastrointestinal bleeding or ulceration, severe renal or hepatic impairment, and during the third trimester of pregnancy due to the risk of fetal harm. It is also contraindicated in patients with a history of asthma or allergic reactions triggered by aspirin or other NSAIDs.
What Other Drugs Will Affect Kebuzone
Drug interactions can alter the effectiveness of Kebuzone and increase the risk of adverse effects. It is important to inform the healthcare provider of all medications being taken, including prescription, over-the-counter drugs, and supplements.
Concomitant use of Kebuzone with other NSAIDs or corticosteroids can increase the risk of gastrointestinal bleeding and ulceration. Anticoagulants, such as warfarin, can also interact with Kebuzone, enhancing the risk of bleeding. Monitoring coagulation parameters is essential when these drugs are used together.
Kebuzone can reduce the efficacy of antihypertensive medications, such as ACE inhibitors, angiotensin II receptor blockers (ARBs), and diuretics, potentially leading to elevated blood pressure. Additionally, co-administration with lithium or methotrexate may increase the levels of these drugs, raising the risk of toxicity.
Patients taking selective serotonin reuptake inhibitors (SSRIs) or serotonin-norepinephrine reuptake inhibitors (SNRIs) should be cautious, as combining these antidepressants with Kebuzone can further elevate the risk of gastrointestinal bleeding.
In summary, Kebuzone is a valuable NSAID with potent anti-inflammatory and analgesic properties. Its mechanism of action involves the inhibition of COX enzymes, leading to reduced prostaglandin production. While effective in managing pain and inflammation, careful consideration of its side effects and potential drug interactions is necessary to ensure safe and optimal use. Always consult a healthcare provider for personalized advice and recommendations when using Kebuzone.
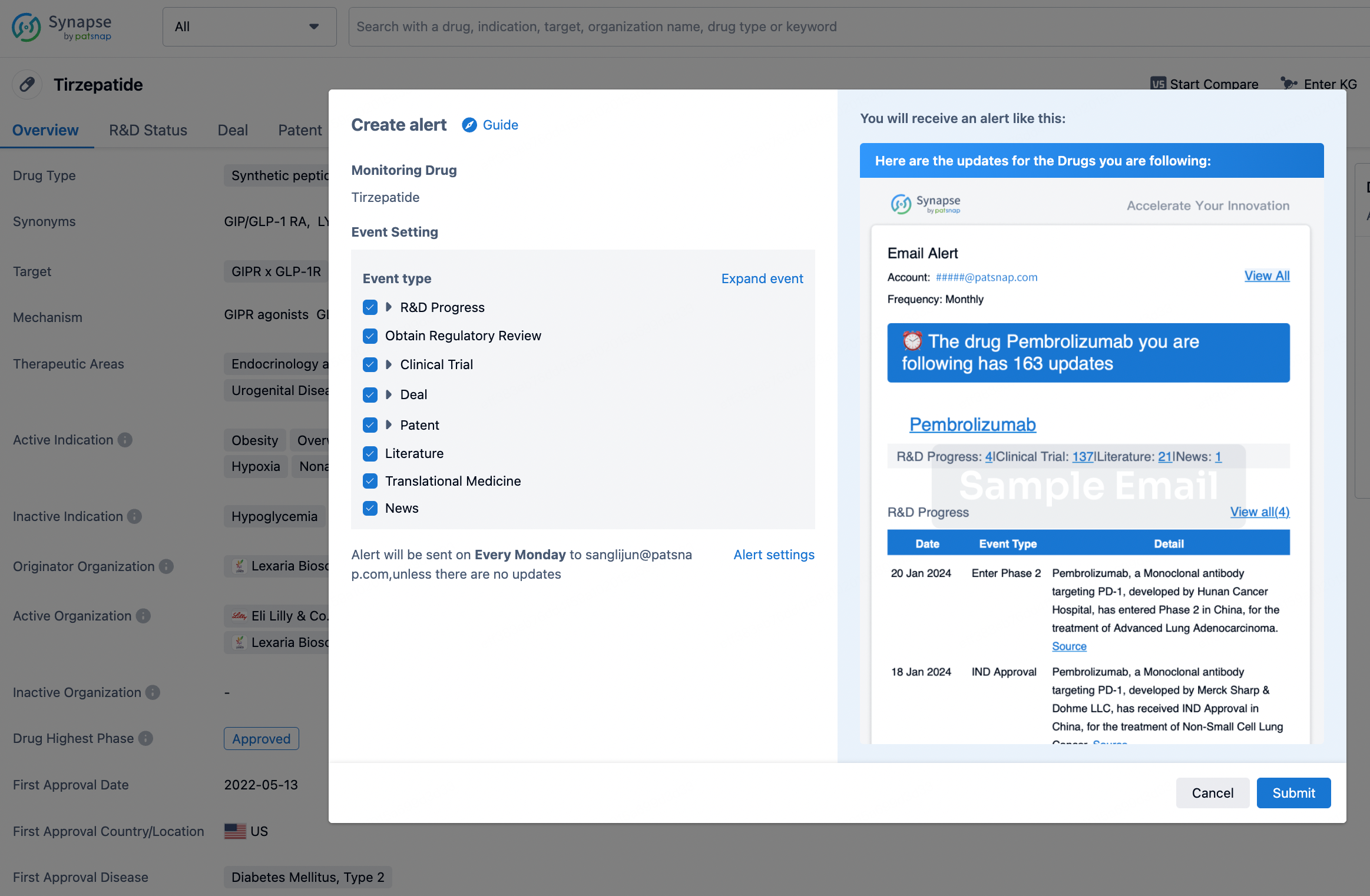
How to obtain the latest development progress of all drugs?
In the Synapse database, you can stay updated on the latest research and development advances of all drugs. This service is accessible anytime and anywhere, with updates available daily or weekly. Use the "Set Alert" function to stay informed. Click on the image below to embark on a brand new journey of drug discovery!
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.