Last update 19 Sep 2024

Senzime AB
Last update 19 Sep 2024
Overview
Related
8
Clinical Trials associated with Senzime ABComparison of Electromyography-based TetraGraph and Acceleromyography-based TOF-Watch SX Neuromuscular Monitors Under Clinical Conditions
Anesthesiologists are often required to give certain drugs, called muscle relaxants to the patients for surgery. These drugs make the people weak for the procedure to make the work of the surgeon easier and prevent unexpected movements. The effect of these drugs must be terminated by the end of the procedures to ensure that the patients can breathe normally. Over the years several monitors have been developed to monitor the effect of these drugs. The monitors use different principles to measure muscle function. Some monitors are integrated into anesthesia machines while others are battery-operated, portable devices. The aim of the present study is two compare monitors using different technologies. Both monitors stimulate a peripheral nerve at the wrist that makes the thumb twitch. The older device (TOF-Watch SX) measures the acceleration of thumb movement, the new device (TetraGraph) measures the electrical activity of the muscle that moves the thumb. The two devices will be connected so that with one simulation both types of signals can be recorded and analyzed. The monitors will be used during the surgeries as described by the manufacturer. The study will not influence the surgical procedure or the anesthetic of the patients. The aim of the study is to collect data on how the two monitors correlate, since they measure neuromuscular function by different technologies (acceleromyography and electromyography).
Start Date17 Jun 2019 |
Sponsor / Collaborator |
Randomized Double---Blinded, Controlled Trial to Compare the Effectiveness of Sugammadex vs. Placebo to Prevent Residual Neuromuscular Block in the Post---Anesthesia Care Unit as Evaluated With a Non---Invasive Respiratory Volume Monitor
The study is designed to determine whether patients who receive sugammadex immediately after tracheal extubation will exhibit a decrease in the incidence of postoperative residual paralysis and an associated decrease in the incidence of postoperative respiratory depression.
Start Date01 Jun 2016 |
Sponsor / Collaborator  Mayo Clinic Mayo Clinic [+2] |
Local Metabolism of the Gastric Tube Reconstruction After Esophagectomy
Postoperative surveillance of local metabolism of the surgical reconstruction after esophagectomy by means of Microdialysis. Dialysate is collected continuously for seven postoperative Days. Results analysed in a blinded fashion and related to the clinical outcome. Primary endpoint: anastomotic leakage
Start Date25 Apr 2016 |
Sponsor / Collaborator |
100 Clinical Results associated with Senzime AB
Login to view more data
0 Patents (Medical) associated with Senzime AB
Login to view more data
15
Literatures (Medical) associated with Senzime AB01 Jun 2020·Journal of Clinical Monitoring and ComputingQ3 · MEDICINE
Use of a novel non-invasive respiratory monitor to study changes in pulmonary ventilation during labor epidural analgesia
Q3 · MEDICINE
Article
Author: Choi, Lynn ; Chau, Anton ; Kodali, Bhavani Shankar ; Brayanov, Jordan ; Harvey, Brian C ; Palanisamy, Arvind ; Tsen, Lawrence C
01 Jan 2020·Critical Care Medicine
1153: PREDICTING LOW MINUTE VENTILATION AND OXYGEN DESATURATION FROM EARLY POSTOPERATIVE DATA
Author: Vitale, Joseph ; Saha, Partha ; Essber, Hani ; Chelnick, David ; Hovsepyan, Karen ; Turan, Alparslan ; Adegboye, Janet ; Imsirovic, Jasmin ; Rivas, Eva
01 Feb 2019·Journal of Clinical AnesthesiaQ2 · MEDICINE
Minute ventilation assessment in the PACU is useful to predict postoperative respiratory depression following discharge to the floor: A prospective cohort study
Q2 · MEDICINE
Article
Author: Zahedi, Farhad ; Schumann, Roman ; Bonney, Iwona ; Harvey, Brian
4
News (Medical) associated with Senzime AB21 May 2024
UPPSALA, SWEDEN / ACCESSWIRE / May 21, 2024 / Senzime (STO:SEZI)(OTCQX:SNZZF) In a new clinical study published in the high-impact Anesthesiology journal, a team of US-based researchers compared the accuracy and precision of commercially available neuromuscular block monitors. The study confirms the leading accuracy and precision of Senzime's TetraGraph system, which produced results similar to a gold-standard laboratory reference, while the conventional AMG-based monitors have substantial variability and imprecision that could be clinically significant.
Recently published guidelines and recommendations by ASA (American Society of Anesthesiologists) and ESAIC (European Society of Anaesthesiology and Intensive Care) have called for routine use of quantitative neuromuscular monitoring to prevent residual neuromuscular block. There are currently two types of neuromuscular block monitors on the market that conform to these guidelines: acceleromyography (AMG)- and electromyography (EMG)-based monitors.
The study, "Accuracy and Precision of Three Acceleromyographs, Three Electromyographs and a Mechanomyograph Measuring the Train-of-Four Ratio in the Absence of Neuromuscular Blocking Drugs" by Wedemeyer Z et al. was designed to compare three commercially available AMG monitors and three EMG-based monitors, to a laboratory gold-standard mechanomyograph (MMG).
The study concluded that the AMG-based monitors produced overshoot of measurements and had substantial variability in the data that could be clinically significant. Senzime's EMG-based TetraGraph-system was shown to measure the responses with minimal overshoot and variability, in line with the gold-standard MMG reference technique
"This is an important, high-impact study that confirms the leading accuracy and precision of EMG as well as our TetraGraph system. This study may well solidify the role of the EMG-based TetraGraph as the new clinical standard, and certainly confirms what should be the preferred monitoring system for hospitals that are conforming to the new guidelines," comments Philip Siberg, CEO of Senzime.
AMG utilizes an accelerometer to measure the acceleration of muscle contraction in response to nerve stimulation. Important limitations of AMG include its time-consuming calibration procedure, reported variability and overshoot of data, and limitations of use in certain surgeries when free movement of the monitored muscle (thumb) cannot be assured. EMG differs as uses a disposable sensor and advanced algorithms that measure events at the neuromuscular junction - where the drugs work. The use of a disposable sensor to measure electrical activity is very precise and does not require the patient's thumb to move freely, hence eliminating many of the limitations of AMG technology.
Philip Siberg, CEO of Senzime AB
Phone: +46 (0) 707 90 67 34, e-mail: philip.siberg@senzime.com
About Senzime
Senzime, headquartered in Sweden, is a leading medical device company that develops, manufactures, and markets CE- and FDA-cleared patient monitoring systems. The company provides an innovative portfolio of solutions, including the TetraGraph® and ExSpiron® 2Xi for accurate monitoring of neuromuscular and respiratory functions, typically under and after surgery. The goal is to help eliminate in-hospital complications, and radically reduce health care costs related to surgical and high acuity procedures.
Senzime targets a market opportunity valued more than SEK 40 billion per year, and operates with sales teams in the world's leading markets. The company's shares are listed on Nasdaq Stockholm Main Market (Nasdaq: SEZI) and cross-traded in the US on the OTCQX market (OTCQX:SNZZF). More information is available at senzime.com .
Attachments
New clinical study published in Anesthesiology confirms the leading accuracy and precision of Senzime's TetraGraph system
SOURCE: Senzime
View the original press release on accesswire.com
26 Apr 2024
UPPSALA, SWEDEN / ACCESSWIRE / April 26, 2024 / Senzime (STO:SEZI)(OTCQX:SNZZF) has secured a three-year GPO contract with one of the largest hospital and managed care organizations in the US for the TetraGraph monitoring system. The sole source agreement includes TetraGraph as the only stand-alone EMG-based quantitative neuromuscular monitor available on contract, giving access to over 40 hospitals that serve over 12.5 million patients annually across 11 US states.
"Signing a GPO contract is certainly a key milestone for us as it validates the hospital market demand for our solutions. But being the sole source supplier to one the largest IDNs in the US market is really a landmark for Senzime as it validates our unique technology, our capabilities and our relentless strive for patient safety", comments Senzime's CEO Philip Siberg.
Every year, approximately 100 million patients, including children, receive neuromuscular blocking drugs as part of anesthesia to facilitate endotracheal intubation and optimize surgical conditions. These medications paralyze muscles required for breathing; hence, accurate monitoring during surgery to secure each patient's individual dose is paramount for a safe and timely recovery.
Senzime's TetraGraph is a state-of-the-art quantitative train-of-four (TOF) neuromuscular monitoring system used by anesthesiologists at hundreds of leading hospitals worldwide. Its proprietary technology helps anesthesiologists accurately select the right dose of neuromuscular blocking drugs and their antagonists allowing for patients to safely recover following surgery.
Philip Siberg, CEO of Senzime AB
Phone: +46 (0) 707 90 67 34, e-mail: philip.siberg@senzime.com
Slavoljub Grujicic, CFO
Phone: +46 (0) 76 306 60 11, e-mail: slavoljub.grujicic@senzime.com
About Senzime
Senzime, headquartered in Sweden, is a leading medical device company that develops, manufactures, and markets CE- and FDA-cleared patient monitoring systems. The company provides an innovative portfolio of solutions, including the TetraGraph® and ExSpiron® 2Xi for accurate monitoring of neuromuscular and respiratory functions, typically under and after surgery. The goal is to help eliminate in-hospital complications, and radically reduce health care costs related to surgical and high acuity procedures.
Senzime targets a market opportunity valued more than SEK 40 billion per year, and operates with sales teams in the world's leading markets. The company's shares are listed on Nasdaq Stockholm Main Market (Nasdaq: SEZI) and cross-traded in the US on the OTCQX market (OTCQX: SNZZF). More information is available at senzime.com.
Attachments
Senzime signs its first Group Purchasing Organization (GPO) contract with major US Hospital System as sole source supplier
SOURCE: Senzime
View the original press release on accesswire.com
07 Feb 2024
UPPSALA, SE / ACCESSWIRE / February 7, 2024 / Senzime (STO:SEZI)(OTCQX:SNZZF) Senzime, an industry leader in algorithm-based patient monitoring solutions, today announced that Fukuda Denshi CO, LTD., its licensee in the Japanese market, is launching the first integrated TetraGraph module. The new NH-100 module, powered by Senzime's TetraGraph technology, is now marketed by Fukuda Denshi as an integrated solution for their bedside patient monitors to facilitate EMG-based neuromuscular monitoring in the operating room.
"This is an important milestone for Senzime and the result of a joint co-development project over the last few years. This new, first of its kind, integrated EMG module for neuromuscular monitoring powered by our algorithms, is offered in Japan as an accessory to Fukuda's extensive installed base of patient monitors, and as an alternative solution to the existing portable, stand-alone TetraGraph. With a total of around 15,000 operating rooms in Japan, the new module offers excellent opportunities to increase the market penetration and increase sales of our TetraSens electrodes," commented Philip Siberg, CEO of Senzime.
The new Fukuda Denshi NH-100 module connects to Senzime's TetraSens disposable sensors. The module is sold initially as an accessory in Japan to the Dynascope 1000 series DS-1200 system used for bedside patient monitoring of vital signs.
Since 2016, Senzime has a license agreement with Fukuda Denshi, a leader in the patient monitoring market with annual sales exceeding US$ 1 billion. By the agreement, Fukuda Denshi is granted exclusive rights to license and commercialize Senzime's TetraGraph technology in the Japanese market under its own brand. Senzime generates revenues from Fukuda via manufacturing of certain products, product sales as well as royalty compensation based on actual sales in the Japanese market.
Philip Siberg, CEO of Senzime AB
Phone: +46 (0) 707 90 67 34, e-mail: philip.siberg@senzime.com
About Senzime
Senzime is a Swedish medical device company that develops, manufactures, and markets CE- and FDA-cleared patient monitoring systems. Senzime's employees worldwide are committed to the vision of a world without anesthesia- and respiratory-related complications. The company markets an innovative portfolio of solutions, including the TetraGraph® and ExSpiron® 2Xi for real-time monitoring of neuromuscular and respiratory functions, typically under and after surgery. The goal is to help eliminate in-hospital complications, and radically reduce health care costs related to surgical and high acuity procedures.
Senzime targets a market opportunity valued more than SEK 40 billion per year, and operates with sales teams in the world's leading markets. The company's shares are listed on Nasdaq Stockholm Main Market (Nasdaq: SEZI) and cross-traded in the US on the OTCQX market (OTCQX: SNZZF). More information is available at senzime.com.
Attachments
Senzime licensee Fukuda Denshi launches integrated TetraGraph module in Japanese market
SOURCE: Senzime
View the original press release on accesswire.com
License out/in
100 Deals associated with Senzime AB
Login to view more data
100 Translational Medicine associated with Senzime AB
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 06 Oct 2024
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or
Translational Medicine
Boost your research with our translational medicine data.
login
or
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
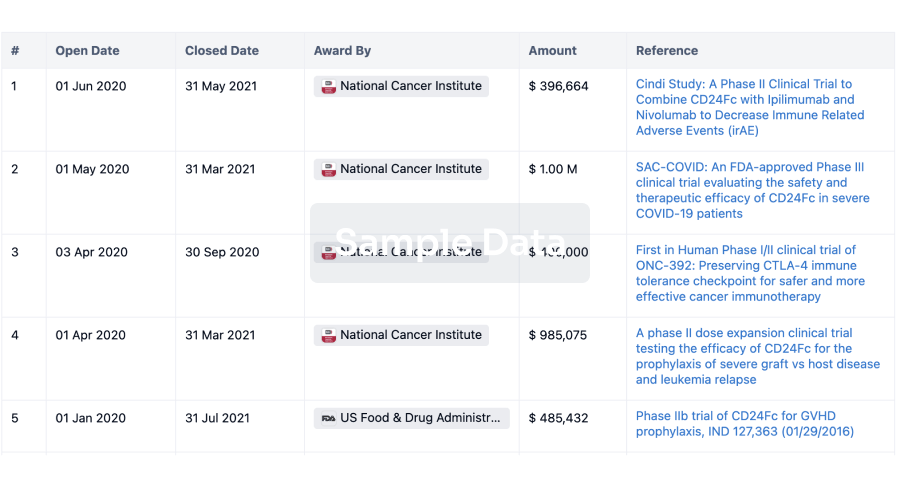
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
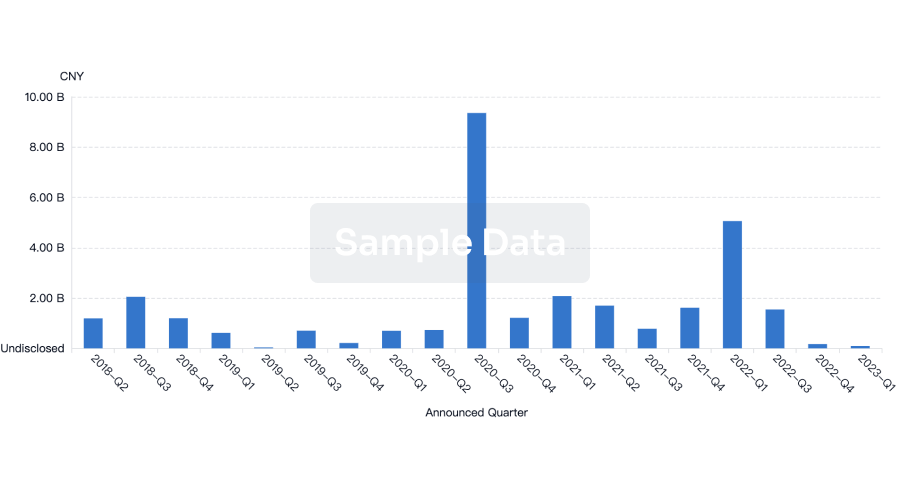
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
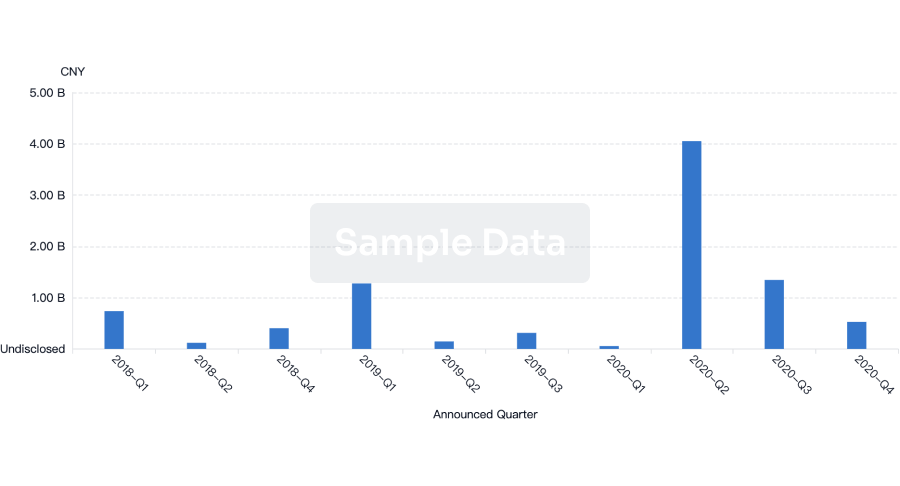
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free
