Request Demo
What is Dibenzepin Hydrochloride used for?
15 June 2024
Dibenzepin Hydrochloride: An In-Depth Look
Introduction to Dibenzepin Hydrochloride:
Dibenzepin Hydrochloride, commonly known by its trade names Noveril and Anelax, is a tricyclic antidepressant (TCA) developed to address various depressive disorders. Initially discovered and synthesized in the mid-20th century, Dibenzepin Hydrochloride has been the focus of numerous studies, particularly in Europe, where it is more commonly prescribed. This antidepressant is primarily targeted at neurotransmitter systems within the brain, aiming to alleviate symptoms of major depressive disorder (MDD) and other related conditions.
Research institutions across Europe and parts of Asia have been actively involved in studying Dibenzepin Hydrochloride, with a significant amount of data supporting its efficacy in treating depression. While the drug is less frequently mentioned in American medical literature compared to other TCAs like amitriptyline or imipramine, it still holds a respected place within the psychiatric community for its unique properties and patient response profiles.
The drug is indicated for major depressive episodes, dysthymia, and in some cases, anxiety disorders. Studies have shown that Dibenzepin Hydrochloride can be particularly effective in patients who have not responded well to other antidepressant therapies. Current research is also exploring its potential use in chronic pain management and certain neurological disorders, although these indications are still under investigation.
Dibenzepin Hydrochloride Mechanism of Action:
The primary mechanism of action for Dibenzepin Hydrochloride involves the inhibition of the reuptake of norepinephrine and serotonin, two key neurotransmitters in the brain. By preventing the reabsorption of these neurotransmitters into the presynaptic neuron, Dibenzepin Hydrochloride increases their availability in the synaptic cleft, thereby enhancing neurotransmission and improving mood.
This action on norepinephrine and serotonin helps to correct the chemical imbalances that are often associated with depression. Additionally, Dibenzepin Hydrochloride has a secondary action on histamine and acetylcholine receptors, which can contribute to its sedative effects and other side effects. The modulation of these pathways helps provide a more comprehensive approach to managing depressive symptoms, but it also necessitates careful monitoring to manage potential adverse effects.
How to Use Dibenzepin Hydrochloride:
Dibenzepin Hydrochloride is typically administered orally in tablet form. The dosage and frequency of administration depend on the severity of the condition being treated and the patient's response to the medication. A common starting dose for adults is around 20-30 mg per day, which can be gradually increased under medical supervision to a typical maintenance dose ranging from 75 to 150 mg per day.
It is often recommended that the daily dosage be divided into two or three doses to minimize potential side effects. In some cases, a single dose may be administered at bedtime to take advantage of the drug's sedative properties and improve sleep patterns disturbed by depression.
The onset of action for Dibenzepin Hydrochloride can vary from patient to patient, but therapeutic effects are generally observed within 2 to 4 weeks of consistent use. It is crucial for patients to adhere to their prescribed regimen and not to discontinue the medication abruptly, as this can lead to withdrawal symptoms and a potential relapse of depressive symptoms.
What is Dibenzepin Hydrochloride Side Effects:
Like all medications, Dibenzepin Hydrochloride comes with potential side effects. Common side effects include dry mouth, blurred vision, constipation, urinary retention, and sedation. These effects are primarily due to the drug's anticholinergic properties. While these side effects can be bothersome, they often diminish over time as the patient's body adjusts to the medication.
More serious side effects, although rarer, can include cardiovascular issues such as tachycardia, arrhythmias, and orthostatic hypotension. Due to these potential risks, it is essential for patients with pre-existing heart conditions to use Dibenzepin Hydrochloride with caution and under strict medical supervision.
Contraindications for the use of Dibenzepin Hydrochloride include a known hypersensitivity to the drug or other tricyclic antidepressants, recent myocardial infarction, and severe liver impairment. Additionally, it should not be used in conjunction with monoamine oxidase inhibitors (MAOIs) due to the risk of severe hypertensive reactions.
Patients should also be monitored for signs of increased suicidal ideation, especially during the initial stages of treatment or when dosages are adjusted. This is particularly important in younger patients, as antidepressants have been associated with an increased risk of suicide in this demographic.
What Other Drugs Will Affect Dibenzepin Hydrochloride:
Dibenzepin Hydrochloride can interact with a variety of other medications, which can either potentiate its effects or increase the risk of adverse reactions. For instance, concurrent use with other central nervous system depressants, such as alcohol, benzodiazepines, or opioids, can enhance the sedative effects of Dibenzepin Hydrochloride, potentially leading to excessive drowsiness or respiratory depression.
The drug's metabolism can be affected by agents that inhibit or induce cytochrome P450 enzymes. For example, medications like cimetidine (a CYP450 inhibitor) can increase the plasma concentration of Dibenzepin Hydrochloride, heightening the risk of toxicity. Conversely, enzyme inducers like carbamazepine can reduce its effectiveness by increasing its clearance from the body.
Patients taking antihypertensive drugs should also be cautious, as Dibenzepin Hydrochloride can potentiate the hypotensive effects of these medications, leading to an increased risk of dizziness or fainting. Additionally, combining Dibenzepin Hydrochloride with other serotonergic drugs, such as selective serotonin reuptake inhibitors (SSRIs), can increase the risk of serotonin syndrome, a potentially life-threatening condition.
To avoid these interactions, it is crucial for patients to inform their healthcare providers of all medications they are currently taking, including over-the-counter drugs and herbal supplements. Close monitoring and possible dosage adjustments may be necessary to ensure safe and effective treatment with Dibenzepin Hydrochloride.
In conclusion, Dibenzepin Hydrochloride is a valuable option in the treatment of depressive disorders, offering a unique profile within the class of tricyclic antidepressants. While it requires careful management and monitoring due to its side effect profile and potential drug interactions, it remains a beneficial tool for many patients struggling with depression. As research continues to evolve, its applications may expand, providing hope for even more individuals in need of effective mental health treatment.
Introduction to Dibenzepin Hydrochloride:
Dibenzepin Hydrochloride, commonly known by its trade names Noveril and Anelax, is a tricyclic antidepressant (TCA) developed to address various depressive disorders. Initially discovered and synthesized in the mid-20th century, Dibenzepin Hydrochloride has been the focus of numerous studies, particularly in Europe, where it is more commonly prescribed. This antidepressant is primarily targeted at neurotransmitter systems within the brain, aiming to alleviate symptoms of major depressive disorder (MDD) and other related conditions.
Research institutions across Europe and parts of Asia have been actively involved in studying Dibenzepin Hydrochloride, with a significant amount of data supporting its efficacy in treating depression. While the drug is less frequently mentioned in American medical literature compared to other TCAs like amitriptyline or imipramine, it still holds a respected place within the psychiatric community for its unique properties and patient response profiles.
The drug is indicated for major depressive episodes, dysthymia, and in some cases, anxiety disorders. Studies have shown that Dibenzepin Hydrochloride can be particularly effective in patients who have not responded well to other antidepressant therapies. Current research is also exploring its potential use in chronic pain management and certain neurological disorders, although these indications are still under investigation.
Dibenzepin Hydrochloride Mechanism of Action:
The primary mechanism of action for Dibenzepin Hydrochloride involves the inhibition of the reuptake of norepinephrine and serotonin, two key neurotransmitters in the brain. By preventing the reabsorption of these neurotransmitters into the presynaptic neuron, Dibenzepin Hydrochloride increases their availability in the synaptic cleft, thereby enhancing neurotransmission and improving mood.
This action on norepinephrine and serotonin helps to correct the chemical imbalances that are often associated with depression. Additionally, Dibenzepin Hydrochloride has a secondary action on histamine and acetylcholine receptors, which can contribute to its sedative effects and other side effects. The modulation of these pathways helps provide a more comprehensive approach to managing depressive symptoms, but it also necessitates careful monitoring to manage potential adverse effects.
How to Use Dibenzepin Hydrochloride:
Dibenzepin Hydrochloride is typically administered orally in tablet form. The dosage and frequency of administration depend on the severity of the condition being treated and the patient's response to the medication. A common starting dose for adults is around 20-30 mg per day, which can be gradually increased under medical supervision to a typical maintenance dose ranging from 75 to 150 mg per day.
It is often recommended that the daily dosage be divided into two or three doses to minimize potential side effects. In some cases, a single dose may be administered at bedtime to take advantage of the drug's sedative properties and improve sleep patterns disturbed by depression.
The onset of action for Dibenzepin Hydrochloride can vary from patient to patient, but therapeutic effects are generally observed within 2 to 4 weeks of consistent use. It is crucial for patients to adhere to their prescribed regimen and not to discontinue the medication abruptly, as this can lead to withdrawal symptoms and a potential relapse of depressive symptoms.
What is Dibenzepin Hydrochloride Side Effects:
Like all medications, Dibenzepin Hydrochloride comes with potential side effects. Common side effects include dry mouth, blurred vision, constipation, urinary retention, and sedation. These effects are primarily due to the drug's anticholinergic properties. While these side effects can be bothersome, they often diminish over time as the patient's body adjusts to the medication.
More serious side effects, although rarer, can include cardiovascular issues such as tachycardia, arrhythmias, and orthostatic hypotension. Due to these potential risks, it is essential for patients with pre-existing heart conditions to use Dibenzepin Hydrochloride with caution and under strict medical supervision.
Contraindications for the use of Dibenzepin Hydrochloride include a known hypersensitivity to the drug or other tricyclic antidepressants, recent myocardial infarction, and severe liver impairment. Additionally, it should not be used in conjunction with monoamine oxidase inhibitors (MAOIs) due to the risk of severe hypertensive reactions.
Patients should also be monitored for signs of increased suicidal ideation, especially during the initial stages of treatment or when dosages are adjusted. This is particularly important in younger patients, as antidepressants have been associated with an increased risk of suicide in this demographic.
What Other Drugs Will Affect Dibenzepin Hydrochloride:
Dibenzepin Hydrochloride can interact with a variety of other medications, which can either potentiate its effects or increase the risk of adverse reactions. For instance, concurrent use with other central nervous system depressants, such as alcohol, benzodiazepines, or opioids, can enhance the sedative effects of Dibenzepin Hydrochloride, potentially leading to excessive drowsiness or respiratory depression.
The drug's metabolism can be affected by agents that inhibit or induce cytochrome P450 enzymes. For example, medications like cimetidine (a CYP450 inhibitor) can increase the plasma concentration of Dibenzepin Hydrochloride, heightening the risk of toxicity. Conversely, enzyme inducers like carbamazepine can reduce its effectiveness by increasing its clearance from the body.
Patients taking antihypertensive drugs should also be cautious, as Dibenzepin Hydrochloride can potentiate the hypotensive effects of these medications, leading to an increased risk of dizziness or fainting. Additionally, combining Dibenzepin Hydrochloride with other serotonergic drugs, such as selective serotonin reuptake inhibitors (SSRIs), can increase the risk of serotonin syndrome, a potentially life-threatening condition.
To avoid these interactions, it is crucial for patients to inform their healthcare providers of all medications they are currently taking, including over-the-counter drugs and herbal supplements. Close monitoring and possible dosage adjustments may be necessary to ensure safe and effective treatment with Dibenzepin Hydrochloride.
In conclusion, Dibenzepin Hydrochloride is a valuable option in the treatment of depressive disorders, offering a unique profile within the class of tricyclic antidepressants. While it requires careful management and monitoring due to its side effect profile and potential drug interactions, it remains a beneficial tool for many patients struggling with depression. As research continues to evolve, its applications may expand, providing hope for even more individuals in need of effective mental health treatment.
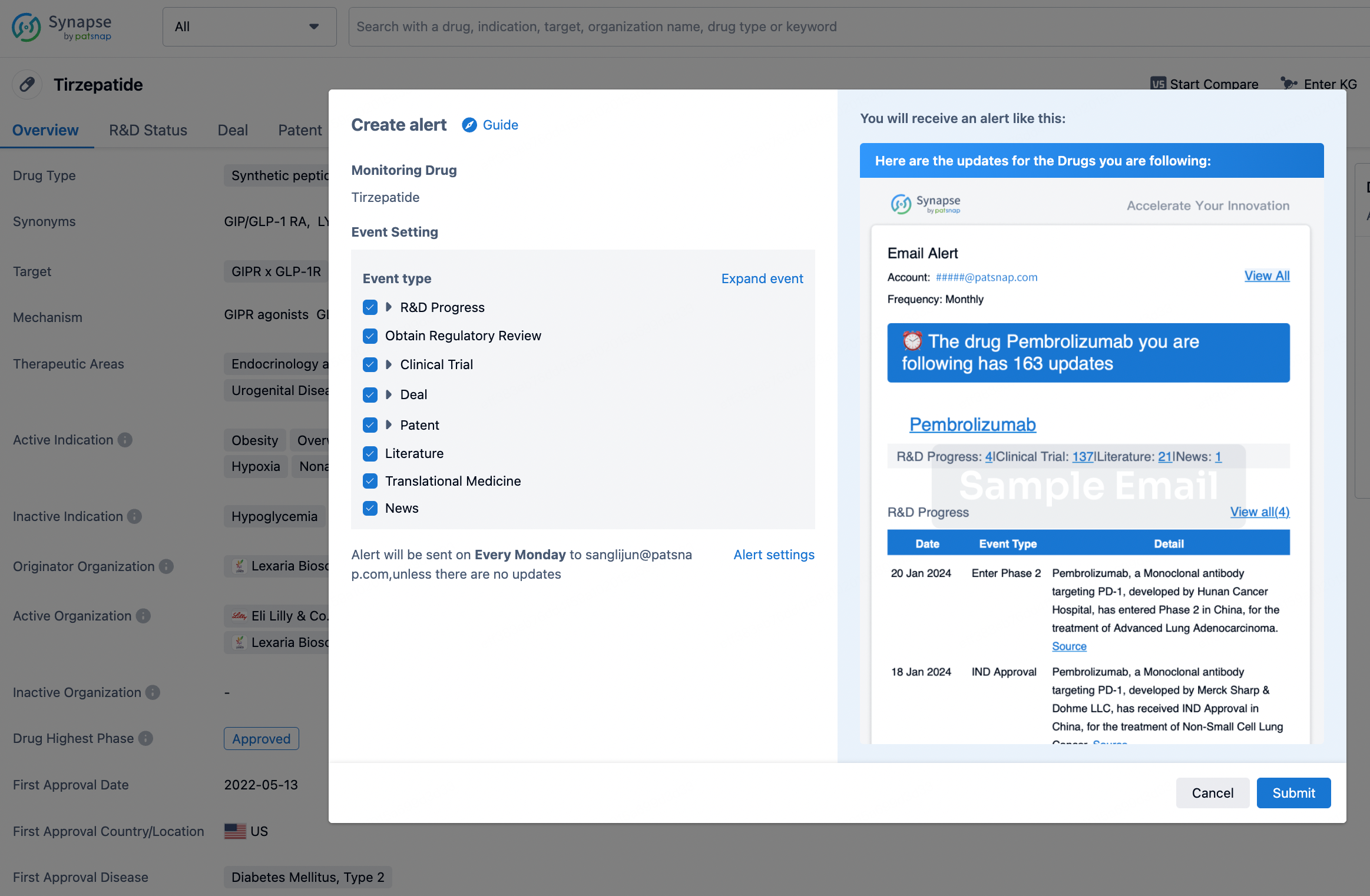
How to obtain the latest development progress of all drugs?
In the Synapse database, you can stay updated on the latest research and development advances of all drugs. This service is accessible anytime and anywhere, with updates available daily or weekly. Use the "Set Alert" function to stay informed. Click on the image below to embark on a brand new journey of drug discovery!
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.