Request Demo
What is Tucatinib used for?
14 June 2024
Tucatinib is a promising drug in the fight against certain types of advanced and metastatic cancers. Known by its trade name, Tukysa, this drug is a tyrosine kinase inhibitor specifically targeting HER2 (Human Epidermal growth factor Receptor 2). The development of Tucatinib has been spearheaded by Seattle Genetics, a biotechnology company specializing in the development and commercialization of innovative, empowered monoclonal antibody-based therapies for the treatment of cancer.
The primary indication for Tucatinib is in the treatment of HER2-positive breast cancer, particularly in cases where the disease is advanced or metastatic. This type of cancer overexpresses the HER2 protein, which promotes the growth of cancer cells. Tucatinib is also being researched for its potential benefits in treating other HER2-positive cancers, such as certain forms of colorectal cancer.
In clinical trials, particularly the pivotal HER2CLIMB trial, Tucatinib has shown significant promise. The trial demonstrated that when used in combination with trastuzumab and capecitabine, Tucatinib significantly improved progression-free survival and overall survival in patients with HER2-positive metastatic breast cancer, even in those with brain metastases, a particularly challenging aspect of cancer treatment.
Tucatinib works by inhibiting the activity of the HER2 protein. HER2 is a member of the epidermal growth factor receptor (EGFR) family, which plays a critical role in the regulation of cell growth and differentiation. Overexpression of HER2 is found in approximately 15-20% of breast cancers and is associated with a more aggressive disease course and poorer prognosis.
By specifically targeting HER2, Tucatinib interferes with the signaling pathways that promote tumor cell growth and survival. This selective inhibition helps to block the proliferation of cancer cells with minimal impact on normal, healthy cells, thereby reducing the likelihood of adverse effects commonly associated with chemotherapy and other more generalized cancer treatments.
One of the unique aspects of Tucatinib's mechanism is its ability to penetrate the blood-brain barrier, an essential feature given the tendency of HER2-positive breast cancer to metastasize to the brain. This ability allows Tucatinib to target and treat brain metastases effectively, offering hope to patients who previously had limited treatment options.
Tucatinib is administered orally in the form of tablets. The recommended dosage, as tested in clinical trials, is 300 mg taken twice daily, with or without food. The onset of action for Tucatinib can vary depending on individual patient factors and the specific regimen used, but patients typically begin to experience therapeutic effects within a few weeks of starting treatment.
It’s crucial to follow the prescribed regimen closely and attend all scheduled appointments with healthcare providers to monitor progress and manage any potential side effects. Regular blood tests and imaging studies may be conducted to assess the effectiveness of the treatment and make any necessary adjustments.
Like all medications, Tucatinib can cause side effects. The most common side effects observed in clinical trials include diarrhea, hand-foot syndrome, nausea, fatigue, and liver enzyme abnormalities. Diarrhea is the most frequently reported side effect and can be severe in some cases, requiring dose modification or discontinuation of the drug. Patients are often advised to take anti-diarrheal medications and maintain adequate hydration to manage this side effect effectively.
Other potential side effects include vomiting, decreased appetite, abdominal pain, headache, and anemia. Monitoring liver function is essential, as elevated liver enzymes can indicate liver toxicity. Patients should report any signs of jaundice, dark urine, or severe abdominal pain to their healthcare provider promptly.
Contraindications for Tucatinib include known hypersensitivity to the drug or any of its components. It’s also advised to exercise caution in patients with pre-existing liver conditions or those who are taking other medications known to affect liver function.
Drug interactions are an important consideration when taking Tucatinib. Certain medications can affect the metabolism and effectiveness of Tucatinib, potentially leading to adverse effects or reduced efficacy.
Strong CYP3A4 inhibitors, such as ketoconazole and itraconazole, can increase the plasma concentration of Tucatinib, raising the risk of toxicity. Conversely, strong CYP3A4 inducers, such as rifampin and phenytoin, can decrease Tucatinib levels, potentially reducing its therapeutic effectiveness.
Other drugs that may interact with Tucatinib include certain antidepressants, anticoagulants, and antiepileptics. It’s essential to inform your healthcare provider of all medications you are taking, including over-the-counter drugs and supplements, to avoid potential interactions.
In conclusion, Tucatinib represents a significant advancement in the treatment of HER2-positive cancers, offering hope to patients with advanced and metastatic disease. Its targeted mechanism of action, ability to penetrate the blood-brain barrier, and manageable side effect profile make it a valuable addition to the oncologist’s armamentarium. As with all cancer treatments, careful monitoring and open communication with healthcare providers are key to optimizing outcomes and managing any potential risks.
The primary indication for Tucatinib is in the treatment of HER2-positive breast cancer, particularly in cases where the disease is advanced or metastatic. This type of cancer overexpresses the HER2 protein, which promotes the growth of cancer cells. Tucatinib is also being researched for its potential benefits in treating other HER2-positive cancers, such as certain forms of colorectal cancer.
In clinical trials, particularly the pivotal HER2CLIMB trial, Tucatinib has shown significant promise. The trial demonstrated that when used in combination with trastuzumab and capecitabine, Tucatinib significantly improved progression-free survival and overall survival in patients with HER2-positive metastatic breast cancer, even in those with brain metastases, a particularly challenging aspect of cancer treatment.
Tucatinib works by inhibiting the activity of the HER2 protein. HER2 is a member of the epidermal growth factor receptor (EGFR) family, which plays a critical role in the regulation of cell growth and differentiation. Overexpression of HER2 is found in approximately 15-20% of breast cancers and is associated with a more aggressive disease course and poorer prognosis.
By specifically targeting HER2, Tucatinib interferes with the signaling pathways that promote tumor cell growth and survival. This selective inhibition helps to block the proliferation of cancer cells with minimal impact on normal, healthy cells, thereby reducing the likelihood of adverse effects commonly associated with chemotherapy and other more generalized cancer treatments.
One of the unique aspects of Tucatinib's mechanism is its ability to penetrate the blood-brain barrier, an essential feature given the tendency of HER2-positive breast cancer to metastasize to the brain. This ability allows Tucatinib to target and treat brain metastases effectively, offering hope to patients who previously had limited treatment options.
Tucatinib is administered orally in the form of tablets. The recommended dosage, as tested in clinical trials, is 300 mg taken twice daily, with or without food. The onset of action for Tucatinib can vary depending on individual patient factors and the specific regimen used, but patients typically begin to experience therapeutic effects within a few weeks of starting treatment.
It’s crucial to follow the prescribed regimen closely and attend all scheduled appointments with healthcare providers to monitor progress and manage any potential side effects. Regular blood tests and imaging studies may be conducted to assess the effectiveness of the treatment and make any necessary adjustments.
Like all medications, Tucatinib can cause side effects. The most common side effects observed in clinical trials include diarrhea, hand-foot syndrome, nausea, fatigue, and liver enzyme abnormalities. Diarrhea is the most frequently reported side effect and can be severe in some cases, requiring dose modification or discontinuation of the drug. Patients are often advised to take anti-diarrheal medications and maintain adequate hydration to manage this side effect effectively.
Other potential side effects include vomiting, decreased appetite, abdominal pain, headache, and anemia. Monitoring liver function is essential, as elevated liver enzymes can indicate liver toxicity. Patients should report any signs of jaundice, dark urine, or severe abdominal pain to their healthcare provider promptly.
Contraindications for Tucatinib include known hypersensitivity to the drug or any of its components. It’s also advised to exercise caution in patients with pre-existing liver conditions or those who are taking other medications known to affect liver function.
Drug interactions are an important consideration when taking Tucatinib. Certain medications can affect the metabolism and effectiveness of Tucatinib, potentially leading to adverse effects or reduced efficacy.
Strong CYP3A4 inhibitors, such as ketoconazole and itraconazole, can increase the plasma concentration of Tucatinib, raising the risk of toxicity. Conversely, strong CYP3A4 inducers, such as rifampin and phenytoin, can decrease Tucatinib levels, potentially reducing its therapeutic effectiveness.
Other drugs that may interact with Tucatinib include certain antidepressants, anticoagulants, and antiepileptics. It’s essential to inform your healthcare provider of all medications you are taking, including over-the-counter drugs and supplements, to avoid potential interactions.
In conclusion, Tucatinib represents a significant advancement in the treatment of HER2-positive cancers, offering hope to patients with advanced and metastatic disease. Its targeted mechanism of action, ability to penetrate the blood-brain barrier, and manageable side effect profile make it a valuable addition to the oncologist’s armamentarium. As with all cancer treatments, careful monitoring and open communication with healthcare providers are key to optimizing outcomes and managing any potential risks.
How to obtain the latest development progress of all drugs?
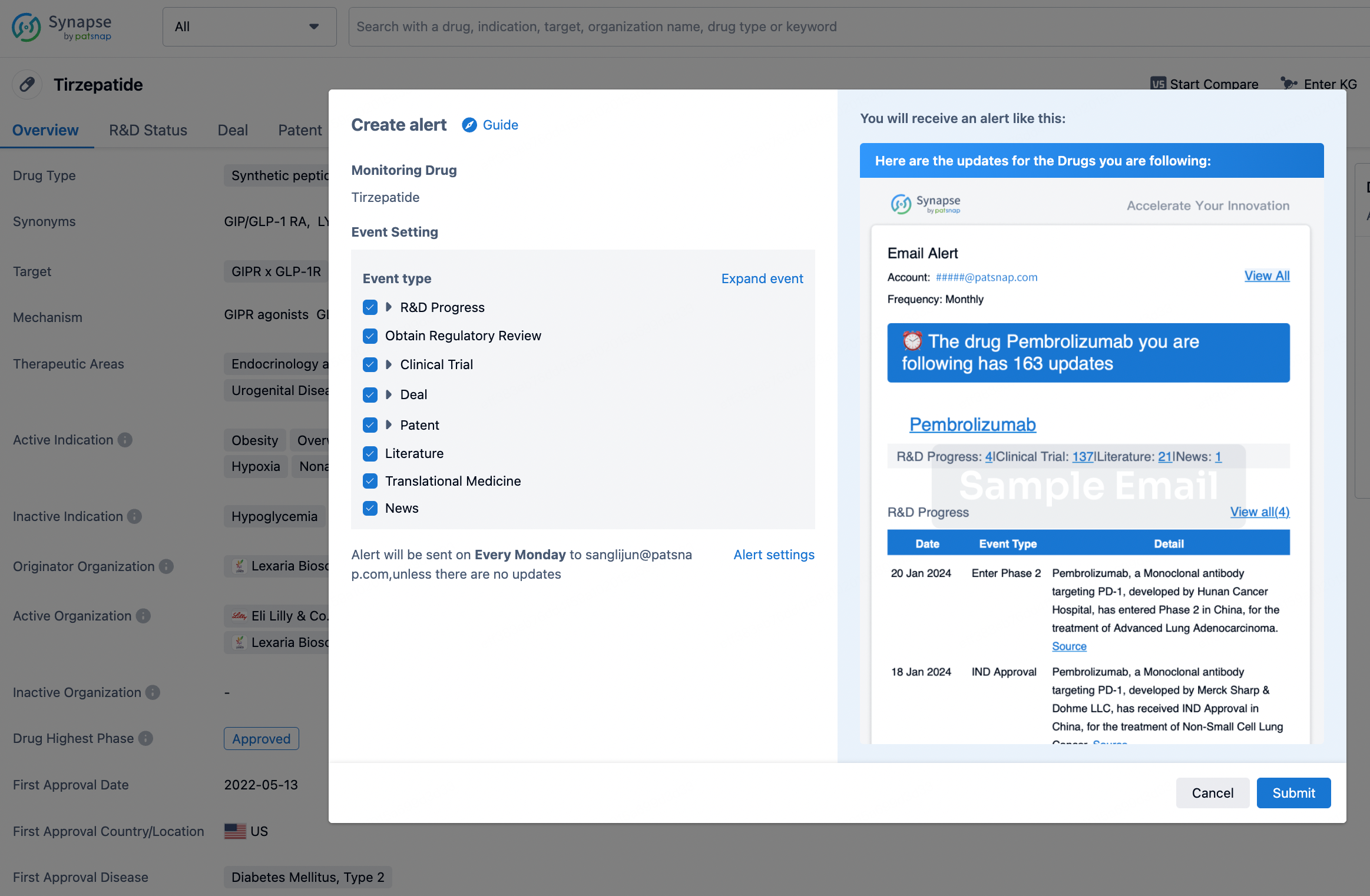
In the Synapse database, you can stay updated on the latest research and development advances of all drugs. This service is accessible anytime and anywhere, with updates available daily or weekly. Use the "Set Alert" function to stay informed. Click on the image below to embark on a brand new journey of drug discovery!
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.