Request Demo
What is Cloxazolam used for?
15 June 2024
Cloxazolam, a lesser-known but important member of the benzodiazepine class of medications, has carved a niche for itself in the treatment of anxiety and related disorders. Known by trade names such as Akton and Sepazon, Cloxazolam is primarily developed and researched in European countries and Japan. Its primary target is the central nervous system, where it exerts sedative, anxiolytic, and muscle-relaxant properties. As a benzodiazepine, Cloxazolam is similar to more commonly known drugs like diazepam (Valium) and lorazepam (Ativan), but with some unique pharmacological characteristics.
First synthesized in the 1970s, Cloxazolam has since been investigated for its efficacy in treating anxiety disorders, which include generalized anxiety disorder (GAD), social anxiety disorder, and panic disorder. The drug has also been explored for its potential use in conditions such as insomnia and muscle spasms, although its primary indication remains anxiety. Research into Cloxazolam is ongoing, with various studies examining its long-term efficacy and safety profile compared to other benzodiazepines and newer classes of anxiolytics.
The mechanism of action of Cloxazolam, like other benzodiazepines, involves modulation of the gamma-aminobutyric acid (GABA) neurotransmitter system. GABA is the primary inhibitory neurotransmitter in the brain, responsible for reducing neuronal excitability and promoting relaxation. Cloxazolam binds to specific sites on the GABA-A receptor, thereby enhancing the receptor's affinity for GABA. This action results in increased GABAergic activity, leading to a calming effect on the brain and reduced symptoms of anxiety. Additionally, the drug has muscle-relaxant properties due to its effects on the spinal cord and other central nervous system structures.
Cloxazolam is typically administered orally in tablet form, with dosages varying based on the severity of the condition being treated and the patient's response to the medication. The standard starting dose for adults is usually between 1 to 2 mg per day, which can be adjusted by the prescribing physician depending on the clinical response and tolerability. For elderly patients or those with compromised liver function, lower doses are often recommended to reduce the risk of adverse effects.
The onset of action of Cloxazolam is relatively rapid, with patients typically experiencing relief from anxiety symptoms within 30 minutes to an hour after ingestion. The drug's effects can last for several hours, making it suitable for both acute and chronic anxiety management. However, it is important to note that the use of Cloxazolam is generally recommended for short-term treatment due to the risk of tolerance, dependence, and withdrawal symptoms associated with long-term benzodiazepine use.
As with all medications, Cloxazolam is associated with a range of potential side effects. Common side effects include drowsiness, dizziness, and fatigue, which are generally mild and tend to diminish with continued use. Some patients may also experience headaches, confusion, and gastrointestinal disturbances such as nausea or constipation. More serious side effects, although rare, can include respiratory depression, especially when combined with other central nervous system depressants, as well as paradoxical reactions such as increased anxiety, agitation, or aggressive behavior, particularly in pediatric and geriatric populations.
Contraindications for the use of Cloxazolam include hypersensitivity to benzodiazepines, severe respiratory insufficiency, sleep apnea syndrome, and myasthenia gravis. It is also contraindicated in pregnant and breastfeeding women due to the potential risks to the fetus or infant. Caution is advised when prescribing Cloxazolam to individuals with a history of substance abuse, as benzodiazepines carry a risk of dependence and misuse.
The interaction of Cloxazolam with other drugs is an important consideration for clinicians. Substances that depress the central nervous system, such as alcohol, opioids, and other sedatives, can potentiate the effects of Cloxazolam, increasing the risk of severe sedation and respiratory depression. Concurrent use of these substances should be avoided or closely monitored. Additionally, certain medications that affect hepatic enzyme activity, such as cimetidine (a common H2 receptor antagonist used for treating gastrointestinal conditions) or certain antifungals, can alter the metabolism of Cloxazolam, potentially leading to increased plasma levels and enhanced effects or toxicity.
Conversely, drugs that induce hepatic enzymes, such as some anticonvulsants like phenytoin or carbamazepine, may reduce the efficacy of Cloxazolam by increasing its clearance from the body. It is essential for healthcare providers to review a patient's medication history thoroughly before prescribing Cloxazolam to avoid potential drug-drug interactions and ensure optimal therapeutic outcomes.
In conclusion, Cloxazolam remains a valuable option within the benzodiazepine class for the treatment of anxiety and related disorders. Its rapid onset of action and effective anxiolytic properties make it suitable for both acute and chronic management of anxiety symptoms. However, due to its potential for dependence and other adverse effects, its use should be carefully monitored, particularly in populations at higher risk for complications. With ongoing research, the understanding of Cloxazolam's long-term safety and efficacy will continue to evolve, guiding its optimal use in clinical practice.
First synthesized in the 1970s, Cloxazolam has since been investigated for its efficacy in treating anxiety disorders, which include generalized anxiety disorder (GAD), social anxiety disorder, and panic disorder. The drug has also been explored for its potential use in conditions such as insomnia and muscle spasms, although its primary indication remains anxiety. Research into Cloxazolam is ongoing, with various studies examining its long-term efficacy and safety profile compared to other benzodiazepines and newer classes of anxiolytics.
The mechanism of action of Cloxazolam, like other benzodiazepines, involves modulation of the gamma-aminobutyric acid (GABA) neurotransmitter system. GABA is the primary inhibitory neurotransmitter in the brain, responsible for reducing neuronal excitability and promoting relaxation. Cloxazolam binds to specific sites on the GABA-A receptor, thereby enhancing the receptor's affinity for GABA. This action results in increased GABAergic activity, leading to a calming effect on the brain and reduced symptoms of anxiety. Additionally, the drug has muscle-relaxant properties due to its effects on the spinal cord and other central nervous system structures.
Cloxazolam is typically administered orally in tablet form, with dosages varying based on the severity of the condition being treated and the patient's response to the medication. The standard starting dose for adults is usually between 1 to 2 mg per day, which can be adjusted by the prescribing physician depending on the clinical response and tolerability. For elderly patients or those with compromised liver function, lower doses are often recommended to reduce the risk of adverse effects.
The onset of action of Cloxazolam is relatively rapid, with patients typically experiencing relief from anxiety symptoms within 30 minutes to an hour after ingestion. The drug's effects can last for several hours, making it suitable for both acute and chronic anxiety management. However, it is important to note that the use of Cloxazolam is generally recommended for short-term treatment due to the risk of tolerance, dependence, and withdrawal symptoms associated with long-term benzodiazepine use.
As with all medications, Cloxazolam is associated with a range of potential side effects. Common side effects include drowsiness, dizziness, and fatigue, which are generally mild and tend to diminish with continued use. Some patients may also experience headaches, confusion, and gastrointestinal disturbances such as nausea or constipation. More serious side effects, although rare, can include respiratory depression, especially when combined with other central nervous system depressants, as well as paradoxical reactions such as increased anxiety, agitation, or aggressive behavior, particularly in pediatric and geriatric populations.
Contraindications for the use of Cloxazolam include hypersensitivity to benzodiazepines, severe respiratory insufficiency, sleep apnea syndrome, and myasthenia gravis. It is also contraindicated in pregnant and breastfeeding women due to the potential risks to the fetus or infant. Caution is advised when prescribing Cloxazolam to individuals with a history of substance abuse, as benzodiazepines carry a risk of dependence and misuse.
The interaction of Cloxazolam with other drugs is an important consideration for clinicians. Substances that depress the central nervous system, such as alcohol, opioids, and other sedatives, can potentiate the effects of Cloxazolam, increasing the risk of severe sedation and respiratory depression. Concurrent use of these substances should be avoided or closely monitored. Additionally, certain medications that affect hepatic enzyme activity, such as cimetidine (a common H2 receptor antagonist used for treating gastrointestinal conditions) or certain antifungals, can alter the metabolism of Cloxazolam, potentially leading to increased plasma levels and enhanced effects or toxicity.
Conversely, drugs that induce hepatic enzymes, such as some anticonvulsants like phenytoin or carbamazepine, may reduce the efficacy of Cloxazolam by increasing its clearance from the body. It is essential for healthcare providers to review a patient's medication history thoroughly before prescribing Cloxazolam to avoid potential drug-drug interactions and ensure optimal therapeutic outcomes.
In conclusion, Cloxazolam remains a valuable option within the benzodiazepine class for the treatment of anxiety and related disorders. Its rapid onset of action and effective anxiolytic properties make it suitable for both acute and chronic management of anxiety symptoms. However, due to its potential for dependence and other adverse effects, its use should be carefully monitored, particularly in populations at higher risk for complications. With ongoing research, the understanding of Cloxazolam's long-term safety and efficacy will continue to evolve, guiding its optimal use in clinical practice.
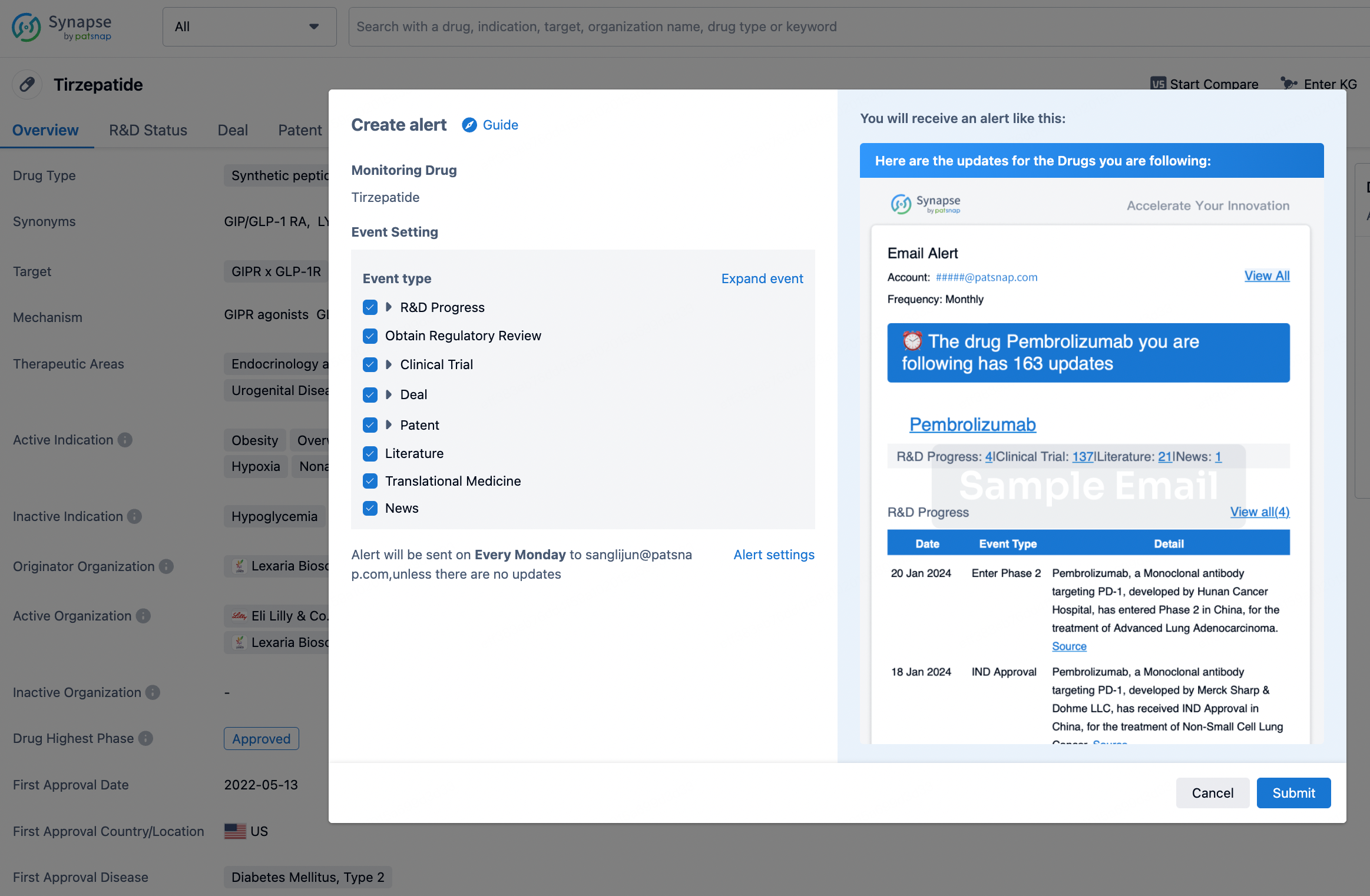
How to obtain the latest development progress of all drugs?
In the Synapse database, you can stay updated on the latest research and development advances of all drugs. This service is accessible anytime and anywhere, with updates available daily or weekly. Use the "Set Alert" function to stay informed. Click on the image below to embark on a brand new journey of drug discovery!
AI Agents Built for Biopharma Breakthroughs
Accelerate discovery. Empower decisions. Transform outcomes.
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.